Quick Summary: Missing a single dose of atorvastatin typically causes no immediate harm because the medication and its active metabolites remain in your system for 20-30 hours. If you remember within 12 hours, take the missed dose; otherwise, skip it and resume your regular schedule. Never double up on doses, and don’t stop taking atorvastatin without consulting your doctor, as poor adherence significantly increases cardiovascular risk.
Atorvastatin is one of the most commonly prescribed medications worldwide. It’s a statin used to lower cholesterol and reduce the risk of heart attack, stroke, and other cardiovascular events.
But life gets busy. Alarms get missed. Routines get disrupted.
So what actually happens when you miss a dose of atorvastatin? Should you panic? Take two pills the next day? Just skip it?
Here’s everything you need to know about missed doses, how your body responds, and what to do next.
Understanding How Atorvastatin Works in Your Body
Before diving into what happens when you miss a dose, it helps to understand how atorvastatin functions.
Atorvastatin belongs to a class of drugs called HMG-CoA reductase inhibitors. These medications work by blocking an enzyme in your liver that produces cholesterol. Less enzyme activity means less cholesterol production, which helps lower your LDL cholesterol levels over time.
The drug has a half-life of about 14 hours, but here’s what matters more: its active metabolites stick around for 20 to 30 hours. These metabolites do roughly 70% of the cholesterol-lowering work. So even 24 hours after your last dose, significant enzyme inhibition continues happening in your liver.
This extended activity is why atorvastatin doesn’t need to be taken at a specific time of day, unlike some older statins. Your body maintains a relatively steady level of the drug between doses.
What Happens to Your Cholesterol When You Miss One Dose
The short answer? Not much.
Missing a single dose won’t cause your cholesterol to spike overnight. Cholesterol levels change gradually, not dramatically, over days and weeks.
Think of atorvastatin like a thermostat for your cholesterol production. Missing one dose is like briefly adjusting the thermostat for a few hours—the overall temperature in your house doesn’t change immediately.
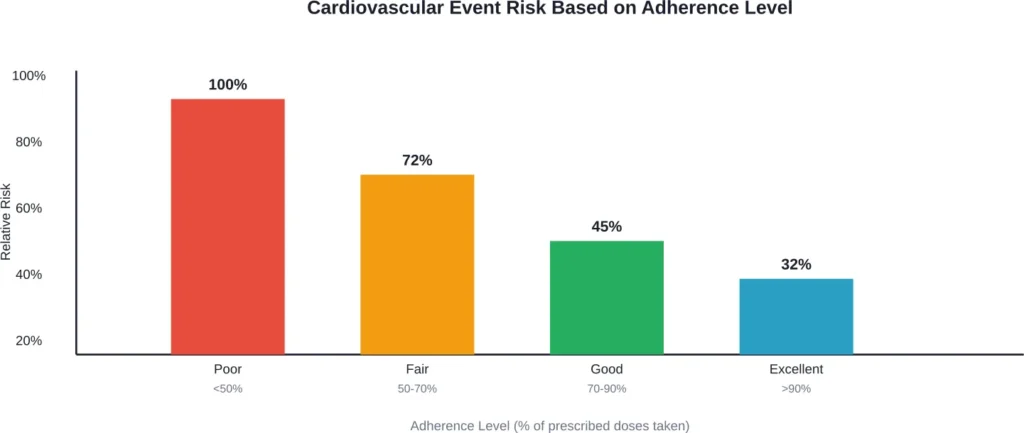
Research on statin adherence shows that the real problems emerge from patterns of missed doses, not isolated incidents. According to medical research published in the National Institutes of Health archives, poor adherence to statin therapy is linked to significantly increased risk of cardiovascular events and death—but this refers to chronic non-adherence, not the occasional forgotten pill.
Your liver will produce slightly more cholesterol during the gap, but the metabolites still circulating in your system continue providing some protective effect.
Immediate Physical Effects: What You Might (or Won’t) Notice
Will you feel anything different if you skip a dose?
Probably not.
Atorvastatin doesn’t work like blood pressure medication or insulin, where missing a dose can cause noticeable symptoms within hours. Cholesterol reduction is a long-term process. The drug doesn’t produce immediate, felt effects—neither when you take it nor when you miss it.
Most people won’t experience any symptoms from missing a single dose. You won’t feel your cholesterol rising, and you won’t suddenly feel different.
The concern with missed doses isn’t about immediate symptoms. It’s about long-term cardiovascular protection. Clinical trials involving more than 80,000 patients across 11 cardiovascular clinical outcomes trials have demonstrated that consistent atorvastatin therapy reduces cardiovascular risk for both primary and secondary prevention patients.
When that protection gets interrupted repeatedly, the cumulative effect becomes significant.
The 12-Hour Rule: When to Take a Missed Dose
So you realized you forgot your atorvastatin. What now?
According to guidance from Mayo Clinic and NHS resources, follow this simple rule:
| When You Remember | What to Do |
|---|---|
| Within 12 hours of your usual time | Take the missed dose immediately, then continue your regular schedule |
| More than 12 hours later | Skip the missed dose entirely and take your next dose at the regular time |
| Almost time for the next dose | Skip the missed dose; never double up |
The 12-hour window exists because of how the drug processes in your body. Taking it within this timeframe keeps your medication levels relatively consistent without risking an overlap with your next scheduled dose.
But here’s what you should never do: take two doses at once to “catch up.” Doubling doses increases the risk of side effects without providing additional cardiovascular benefit.

Missing Multiple Doses: When It Becomes a Problem
One missed dose is manageable. But what about missing several doses over time?
This is where the cardiovascular risk starts climbing.
Research from multiple studies shows that statin non-adherence dramatically increases the risk of major cardiovascular events. A study examining discontinuation patterns found that among 431,023 patients prescribed statins, those who stopped treatment had significantly worse cardiovascular outcomes compared to those who maintained therapy.
The problem compounds because cholesterol management is cumulative. Think of it like compound interest—but in reverse. Each missed dose slightly reduces your protection, and those small reductions add up over weeks and months.
Here’s what happens with chronic missed doses:
- Your cholesterol levels gradually rise back toward pre-treatment levels
- The protective effects on your blood vessel walls diminish
- Your risk of plaque buildup and cardiovascular events increases
- Any existing cardiovascular disease may progress faster
Real-world evidence examining adherence patterns shows that many patients struggle to maintain consistent statin therapy. The research indicates that long-term adherence rates are often suboptimal, with serious implications for cardiovascular health.
Special Timing Scenarios: Travel and Schedule Disruptions
Real life doesn’t always cooperate with medication schedules.
What about situations like international travel, shift work, or major schedule changes?
When traveling across time zones, take atorvastatin once every 24 hours at a time that fits your new schedule. The drug’s long half-life and active metabolites give you flexibility. The critical factor isn’t the exact time of day—it’s maintaining that once-daily pattern without skipping entire days.
For shift workers or people with irregular schedules, pick a consistent anchor point. Some patients find success tying their dose to a specific daily activity rather than a clock time: with breakfast, before bed, or when brushing teeth in the evening.
The NHS guidance confirms that atorvastatin can be taken at any time of day, as long as you take it consistently around the same time each day.
Side Effects and Missed Doses: Is There a Connection?
Some patients wonder whether missing doses affects their side effect profile.
Generally speaking, missing a dose won’t cause new side effects. The most common side effects of atorvastatin—muscle aches, digestive issues, and headaches—are related to taking the medication, not missing it.
But there’s an interesting pattern worth noting. Patients who frequently start and stop their statin therapy may experience what feels like recurring side effects. This on-again, off-again pattern can make side effects more noticeable compared to steady, consistent use.
According to a comprehensive meta-analysis published in The Lancet examining adverse effects in statin trials, only a small number of undesirable effects showed statistically significant increases with statin therapy versus placebo. The study found abnormal liver transaminases and other liver function test abnormalities were related to statin intensity, but found no evidence that statins cause the majority of adverse effects listed in product labels.
The takeaway? If you’re experiencing side effects, missing doses won’t solve the problem. Talk to your doctor about adjusting your dose or trying a different statin instead.
Can You Stop Atorvastatin Suddenly?
Here’s where things get more serious.
Intentionally stopping atorvastatin—or letting missed doses turn into discontinued treatment—carries significant risks.
Research on statin discontinuation shows that patients who stop their statin therapy after a myocardial infarction face worse long-term outcomes. Real-life statin dosing studies indicate that early treatment patterns strongly influence long-term cardiovascular health.
Stopping atorvastatin doesn’t cause immediate withdrawal symptoms like some medications. But it does mean:
- Your cholesterol protection ends within days
- Cholesterol levels begin rising within 2-4 weeks
- Cardiovascular risk increases gradually over months
- Any benefits gained from previous treatment start eroding
A study examining discontinuation patterns found that many patients who stop statins don’t restart them, even when they remain at high cardiovascular risk. The research tracked hundreds of thousands of patients and documented the gap between treatment guidelines and real-world adherence.
If you’re considering stopping atorvastatin due to side effects, cost concerns, or skepticism about necessity, talk to your doctor first. There may be alternatives: different statins, lower doses, or combination approaches with other lipid-lowering therapies.
Why People Miss Doses: The Adherence Challenge
Understanding why doses get missed helps prevent future problems.
Research identifies several common patterns:
| Reason for Non-Adherence | Impact |
|---|---|
| Simply forgetting | Most common reason; usually sporadic missed doses |
| Complex medication schedules | Patients on multiple medications struggle more |
| Side effects or perceived side effects | Leads to intentional dose-skipping or discontinuation |
| Cost concerns | Some patients ration pills or stop refilling prescriptions |
| Lack of noticeable benefit | Unlike blood pressure meds, patients don’t “feel” statins working |
| Skepticism about necessity | Patients question whether they really need the medication |
Studies on statin adherence consistently show that patients struggle more with medications that don’t produce felt effects. Blood pressure medication lowers your pressure immediately—you might feel dizzy if you skip it. Insulin affects your blood sugar within hours.
But atorvastatin? It quietly works in your liver, producing no sensations. This “invisible” benefit makes adherence psychologically harder.
Research examining patient perception and knowledge about statin therapy found that understanding of why the medication matters significantly impacts adherence rates. Patients who grasp the cardiovascular protection atorvastatin provides tend to maintain better adherence.
Practical Strategies to Avoid Missing Doses
Prevention beats damage control.
Here are evidence-based strategies that help maintain consistent adherence:
Use technology: Smartphone alarms, medication reminder apps, or smart pill bottles can prompt you at the same time daily. Set your alarm for a time when you’re typically home and following a routine.
Link to an existing habit: Pair your atorvastatin with something you do every day without fail. Brushing teeth, morning coffee, or plugging in your phone before bed all work as anchors.
Weekly pill organizers: These aren’t just for older adults. They provide a visual check—you can instantly see if you’ve taken today’s dose or if you forgot yesterday’s.
Keep medication visible: Store your atorvastatin where you’ll see it during your routine. Near the coffee maker, on your nightstand, next to your toothbrush.
Simplify your regimen: If you take multiple medications, ask your doctor whether any can be combined or taken at the same time. Fewer medication times means fewer opportunities to forget.
Refill before running out: Set a reminder to refill when you have a week’s supply left. Running out guarantees missed doses.
Research on nonadherence to statins suggests that individualized intervention strategies work better than one-size-fits-all approaches. What works for one person might not work for another. Experiment to find your reliable system.

Does a Missed Dose Affect Cholesterol Test Results?
Planning to get your cholesterol checked soon? Wondering if that missed dose last week will affect your results?
Generally speaking, a single missed dose won’t significantly skew your cholesterol test results. Lipid panels measure your average cholesterol levels, which reflect weeks of treatment patterns, not yesterday’s dose.
However, if you’ve missed multiple doses in the weeks leading up to your test, your results may be higher than they would be with consistent adherence. This could lead your doctor to adjust your dose unnecessarily, thinking the current dose isn’t working well enough.
For the most accurate test results, maintain your usual medication schedule in the weeks before testing. If you’ve had several missed doses recently, mention this to your doctor when discussing test results.
Some patients ask whether they should take atorvastatin before their blood test. Since atorvastatin works over the long term to reduce cholesterol production, taking it the morning of your test won’t affect the results. What matters is your pattern of use over the previous weeks.
Special Considerations for High-Risk Patients
Not everyone faces the same risk from missed doses.
Patients in certain categories should be especially vigilant about adherence:
Post-heart attack or stroke patients: If you’re taking atorvastatin for secondary prevention (meaning you’ve already had a cardiovascular event), consistent adherence is absolutely critical. Research on initial statin dosing after myocardial infarction shows that both dose intensity and consistency dramatically affect long-term outcomes.
Very high cholesterol: Patients with familial hypercholesterolemia or extremely elevated cholesterol levels have less margin for error. Every dose matters more when baseline risk is higher.
Multiple risk factors: If you have diabetes, high blood pressure, smoking history, or family history of early heart disease alongside high cholesterol, the cumulative risk makes adherence more important.
Older adults: Age itself is a cardiovascular risk factor. While older adults sometimes struggle more with adherence due to complex medication regimens, the cardiovascular protection statins provide becomes even more valuable.
For high-risk patients, even sporadic missed doses can incrementally increase cardiovascular event risk. The protective effect of statins is dose-dependent and consistency-dependent.
When to Contact Your Doctor
Most missed doses don’t require a call to your doctor. But certain situations warrant a conversation:
- You’ve missed multiple doses over several weeks
- You’re considering stopping atorvastatin due to side effects
- You’re having trouble affording your medication
- You’ve developed a pattern of forgetting despite trying reminder strategies
- You’re experiencing muscle pain or weakness (rare but important side effect)
- You have questions about whether you still need the medication
Your doctor can help troubleshoot adherence problems. Options might include switching to a different statin, adjusting your dose, adding combination therapy, or using alternative lipid-lowering medications if atorvastatin isn’t working for you.
According to the National Lipid Association’s guidance on statin intolerance, doctors now have multiple strategies for patients who struggle with standard statin therapy. Complete statin intolerance is rare—most adherence issues can be solved with the right approach.
The Bigger Picture: Adherence and Cardiovascular Health
Here’s the real message behind the “missed dose” question.
Atorvastatin works when taken consistently over time. It’s not a short-term fix or an emergency medication. It’s a long-term investment in cardiovascular health.
Clinical trials demonstrate that atorvastatin reduces cardiovascular events by approximately 23% in major coronary events and 22% in vascular events who take it consistently. That protection accumulates over months and years of regular use.
But that same protection erodes when adherence falters.
Research examining real-world adherence patterns shows that patients who maintain consistent therapy see dramatically better cardiovascular outcomes than those with spotty adherence—even when the inconsistent group takes the medication “most of the time.”
One missed dose won’t undo months of treatment. But a pattern of missed doses—whether from forgetfulness, side effects, or intentional discontinuation—substantially reduces the medication’s protective benefit.
Think of atorvastatin adherence like compound interest in a retirement account. Missing one monthly deposit won’t ruin your retirement, but skipping deposits regularly will leave you short of your goal.
Frequently Asked Questions
Missing two consecutive days won’t cause immediate harm, but your cholesterol protection decreases more significantly than with a single missed dose. Resume your regular schedule as soon as you remember—don’t take extra doses to compensate. If you frequently miss multiple days, talk to your doctor about adherence strategies or alternative treatments.
Some research suggests that alternate-day atorvastatin dosing can provide cholesterol-lowering effects, though studies show daily dosing is more effective for reaching treatment goals. Never switch to every-other-day dosing without consulting your doctor first. The standard recommendation remains once-daily dosing for optimal cardiovascular protection.
No. Cholesterol levels change gradually over days and weeks, not hours. A single missed dose won’t cause a measurable spike in your cholesterol. However, patterns of missed doses over weeks will allow your cholesterol to gradually rise back toward pre-treatment levels.
No. Never double up on atorvastatin doses. Taking two pills at once increases your risk of side effects without providing additional cardiovascular benefit. If you missed yesterday’s dose, simply skip it and take today’s dose at your regular time.
There’s no specific number because cholesterol changes happen gradually. Even one missed dose slightly reduces your protection, though the effect is minimal. Missing 20-30% of your doses over several weeks will noticeably reduce the medication’s effectiveness. The goal should be to take atorvastatin as consistently as possible—aim for over 90% adherence.
Usually not. If you’ve been off atorvastatin for a few weeks, you can typically restart at your previous dose. However, if you stopped due to side effects or if it’s been several months, consult your doctor before restarting. They may want to reassess your cholesterol levels and determine the appropriate dose.
Your doctor can’t directly detect missed doses, but inconsistent adherence often shows up in cholesterol test results. If your cholesterol isn’t improving as expected despite being prescribed an adequate dose, it may indicate adherence issues. Be honest with your doctor about adherence challenges—they can help troubleshoot rather than simply increasing your dose.
Conclusion: Building Consistency for Long-Term Health
Missing a single dose of atorvastatin isn’t a catastrophe. The medication’s long half-life and active metabolites provide a buffer that protects you from immediate harm.
But cardiovascular health is a marathon, not a sprint.
The real value of atorvastatin comes from taking it consistently over months and years. That consistent use gradually reduces your cholesterol, stabilizes arterial plaques, and lowers your risk of heart attack and stroke.
If you’ve missed a dose, follow the 12-hour rule: take it if you remember within 12 hours, skip it if you’re beyond that window. Never double up. And if missed doses are becoming a pattern, implement some of the adherence strategies discussed here—or talk to your doctor about alternatives.
The protection atorvastatin provides is powerful, but only when you take it. Make adherence a priority, and your cardiovascular system will thank you for decades to come.
