Quick Summary: Swallowing a battery, especially a button or coin battery, is a life-threatening emergency that can burn through the esophagus in as little as two hours. According to the National Capital Poison Center, immediate medical attention is critical—parents should take the child to the emergency room without delay and call the National Battery Ingestion Hotline at 800-498-8666.
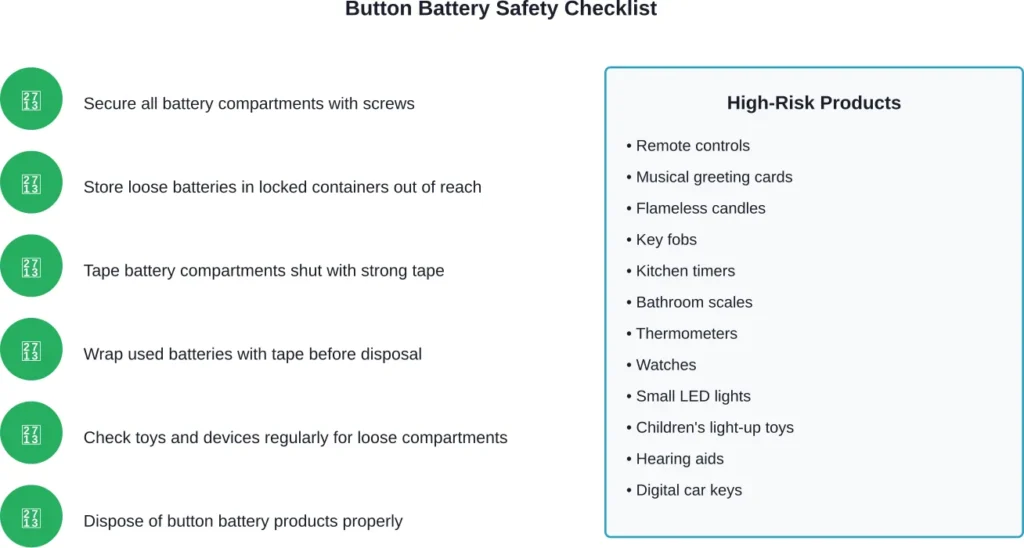
Button batteries hide everywhere. Remote controls, musical greeting cards, key fobs, flameless candles, and children’s toys all contain these shiny, coin-sized power sources. They look harmless enough sitting on your kitchen counter.
But here’s the thing—when swallowed, these small batteries become medical emergencies that unfold with terrifying speed.
From 1997 to 2010, an estimated 40,400 children aged under 13 years were treated in hospital emergency departments for battery-related injuries, according to CDC data. Nearly three quarters of these injuries involved children aged ≤4 years, with 10% requiring hospitalization.
The numbers haven’t improved. The danger remains present in thousands of homes, and most serious battery ingestions aren’t even witnessed by parents.
Why Button Batteries Are So Dangerous
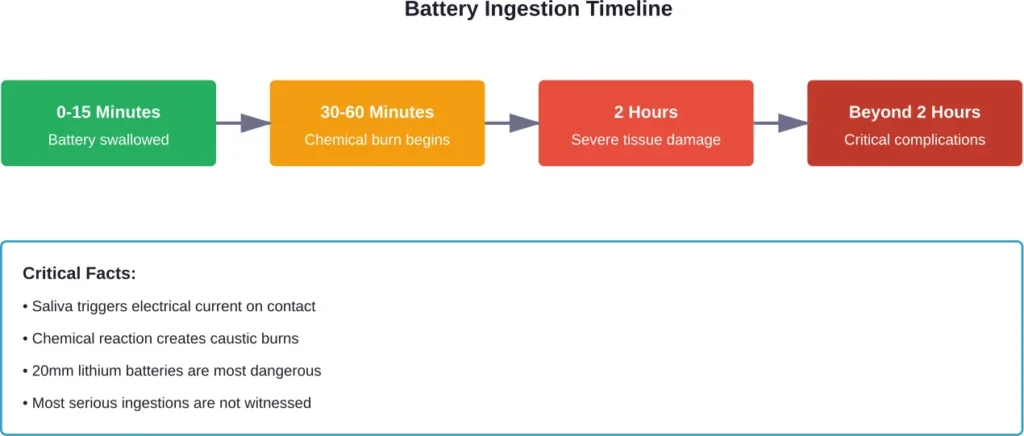
When a battery gets stuck in the esophagus, saliva triggers an electrical current. This current causes a chemical reaction that severely burns the esophageal tissue.
The damage happens fast. According to the National Capital Poison Center, swallowed batteries burn through a child’s esophagus in just 2 hours, leading to surgery, months with feeding and breathing tubes, and even death.
The 20 mm, 3-volt lithium coin cells—about the size of a nickel—are the most hazardous. They’re big enough to get stuck in the esophagus and burn faster than other battery types.
National Battery Ingestion Hotline data reveals where swallowed 20 mm lithium coin cells were mainly used over recent years: 25% were intended for remote controls, 15% for lights, and 14% for flameless candles.
What Happens Inside the Body
The mechanism of injury goes beyond simple chemical burns. When stuck in the esophagus, the battery creates an electrical circuit with the moist tissue. This generates hydroxide ions at the negative pole, creating a highly alkaline solution with a pH above 13.
Research on esophageal injury shows the tissue pH value drops dramatically within 20 minutes of battery exposure. The alkaline burn liquefies tissue, penetrating deeper into the esophageal wall as time passes.
The damage doesn’t stop at burns. Complications include:
- Esophageal perforation
- Tracheoesophageal fistula (abnormal connection between esophagus and airway)
- Vocal cord paralysis
- Stricture formation requiring repeated dilations
- Massive bleeding from erosion into major blood vessels
- Death from catastrophic hemorrhage or sepsis
The National Capital Poison Center has documented 280 cases of nonfatal button battery ingestions with severe esophageal or airway injury. These children faced months of recovery, multiple surgeries, and permanent complications.
Signs That Someone Has Swallowed a Battery
Most serious battery ingestions aren’t witnessed. That’s what makes them so dangerous.
Parents should consider the possibility of battery ingestion in every patient with these symptoms:
- Acute airway obstruction
- Wheezing or noisy breathing
- Drooling
- Vomiting
- Chest pain or discomfort
- Refusal to eat
- Coughing or choking
- Fever
But here’s the problem—early symptoms can be vague or absent. A child might seem fine for hours while catastrophic damage develops internally.
Sound familiar to other childhood illnesses? Exactly. That’s why a high index of suspicion matters when button batteries are present in the home.
Emergency Steps If Battery Ingestion Occurs
This is an emergency. Not a “wait and see” situation. Not a “call the pediatrician in the morning” scenario.
Take the child to an emergency department immediately.
While En Route to the Hospital
According to the U.S. Consumer Product Safety Commission and National Capital Poison Center guidelines, parents can take one protective measure during transport:
If the child is over 12 months old and the battery was swallowed within the past 12 hours, give honey. The dose is 10 mL every 10 minutes, up to six doses maximum. (Note: Some sources reference this as 2 tablespoons rather than 2 teaspoons)
The honey coats the esophagus and battery, potentially reducing the severity of burns. Research suggests it may slow the chemical reaction.
Critical limitations apply:
- Do NOT give honey to children under 12 months (botulism risk)
- Do NOT delay going to the emergency room to obtain honey
- Do NOT exceed six doses
- This is NOT treatment—only a potential harm reduction measure
Call the National Battery Ingestion Hotline at 800-498-8666 or Poison Help at 1-800-222-1222 while traveling to the hospital.
What NOT to Do
Never induce vomiting. This may cause more damage or force the battery into the lungs, creating an even more dangerous situation.
Don’t give food or drink (other than the honey protocol described above). Don’t wait for symptoms to develop.
Medical Treatment and Diagnosis
Emergency departments use X-rays to locate the battery and determine its size. The location determines urgency and treatment approach.
| Battery Location | Timeframe for Removal | Risk Level |
|---|---|---|
| Esophagus | Immediate (within 2 hours) | Critical—highest risk of severe injury |
| Stomach (large battery) | Within 12-24 hours | High—can cause gastric perforation |
| Stomach (small battery, asymptomatic) | Monitor; may pass naturally | Moderate—requires close observation |
| Beyond stomach | Monitor unless symptomatic | Variable—depends on battery size and symptoms |
According to National Capital Poison Center triage guidelines, if the patient is > 12 years and the ingested battery is ≤ 12 mm, no x-ray to locate the battery is required if the patient is entirely asymptomatic and has been asymptomatic since the battery was ingested, only one battery was ingested, and no magnet was also ingested.
For batteries stuck in the esophagus, endoscopic removal happens as quickly as possible. Gastroenterologists use specialized tools to extract the battery without causing additional trauma.
Recent research on electric insulating irrigations shows that flushing the esophagus with certain solutions during endoscopy may help mitigate injury. This approach aims to neutralize the alkaline environment and wash away caustic material.
Prevention Strategies for Families
The U.S. Consumer Product Safety Commission approved a mandatory standard in September 2023 to reduce button cell and coin battery ingestion hazards for children six years and younger. This regulation, resulting from Reese’s Law, requires secure battery compartments in consumer products.
Real talk: regulations help, but prevention at home remains critical.
A recent study found that 29.8% of button battery ingestions involved batteries that were being stored or had been removed from devices. Proper disposal matters.
Before throwing away button batteries, tape the positive and negative poles. This prevents the battery from creating a circuit if a child retrieves it from the trash.
What About Adults and Older Children?
While young children face the highest risk, battery ingestion can affect anyone. Adults with cognitive impairments, dementia, or psychiatric conditions may accidentally or intentionally swallow batteries.
Cylindrical batteries (like AAA or AA) pose different risks. They’re larger, so they typically don’t lodge in the esophagus as easily. However, they can still cause obstruction or perforation, particularly if they fragment.
According to medical literature, cases of battery ingestion including cylindrical cells have been documented, with varying outcomes based on battery size and location.
For patients over 12 years who swallow small batteries (12 mm or less) and remain completely asymptomatic, observation may be appropriate if only one battery was swallowed and no magnet was also ingested.
But any symptoms—vomiting, abdominal pain, fever, difficulty swallowing—require immediate medical evaluation and imaging.
Long-Term Outcomes and Recovery
Children who survive serious button battery ingestions face challenging recoveries. Months with feeding tubes. Repeated surgeries to repair fistulas or dilate strictures. Speech therapy for vocal cord damage.
Some require lifelong monitoring for late complications like esophageal strictures that develop months or years after the initial injury.
The emotional toll on families is immeasurable. Preventable injuries carry unique grief and guilt.
Frequently Asked Questions
According to the National Capital Poison Center, batteries can burn through a child’s esophagus in just 2 hours. Damage begins within minutes when saliva creates an electrical current. The 20 mm lithium coin cells cause the fastest and most severe injuries because they’re large enough to lodge in the esophagus and generate more electrical current.
Go to the emergency room immediately—this is a life-threatening emergency. Call the National Battery Ingestion Hotline at 800-498-8666 while traveling. If your child is over 12 months old and the battery was swallowed within the past 12 hours, give 10 mL of honey every 10 minutes, up to six doses, while going to the ER. Never induce vomiting.
Small batteries that pass beyond the esophagus and stomach may transit through the intestines without causing harm, particularly in older children and adults. However, this requires medical monitoring with repeat X-rays to confirm the battery is moving through the system. Large batteries or those that become stuck anywhere in the digestive tract require removal.
No. The 20 mm, 3-volt lithium coin cells are the most hazardous because they’re big enough to lodge in the esophagus and generate strong electrical current. Button batteries are far more dangerous than cylindrical batteries (AA, AAA, C, D) because they’re more likely to get stuck. Larger cylindrical batteries typically don’t lodge in the esophagus but can cause obstruction or perforation elsewhere.
Symptoms include drooling, vomiting, chest pain, difficulty swallowing, refusal to eat, coughing, wheezing, or noisy breathing. However, many children show no symptoms initially even while severe damage develops. Most serious battery ingestions aren’t witnessed, so maintain high suspicion if batteries are accessible in your home and your child shows any unusual symptoms.
For batteries lodged in the esophagus, gastroenterologists perform emergency endoscopy—inserting a flexible tube with a camera and tools through the mouth to visualize and extract the battery. This procedure happens as quickly as possible, ideally within 2 hours of ingestion. Batteries in the stomach may be removed endoscopically or monitored depending on size, type, and symptoms.
Severe cases result in esophageal strictures requiring repeated dilations, tracheoesophageal fistulas needing surgical repair, vocal cord paralysis affecting speech and breathing, chronic feeding difficulties requiring long-term feeding tubes, and increased risk of esophageal cancer later in life. The National Capital Poison Center has documented 280 nonfatal cases with severe esophageal or airway injury, many requiring months of recovery and multiple surgeries.
The Bottom Line
Battery ingestion represents one of the most time-critical pediatric emergencies. The window for preventing catastrophic injury is measured in hours, not days.
Secure battery compartments. Store loose batteries out of reach. Tape battery poles before disposal. Check devices regularly for damaged compartment covers.
If ingestion occurs or is suspected, get to an emergency room immediately. Call the National Battery Ingestion Hotline at 800-498-8666 for expert guidance during transport.
These small, shiny objects that power our convenient modern devices carry devastating potential. Awareness and vigilance protect the children in our care.
