Quick Summary: Drinking alcohol while taking Accutane (isotretinoin) is strongly discouraged because both substances are metabolized by the liver, significantly increasing the risk of liver damage, elevated liver enzymes, and hepatotoxicity. Combining them can also worsen side effects like mood changes, pancreatitis, and lipid abnormalities. Medical guidance consistently advises avoiding alcohol during treatment and for at least one month after stopping the medication.
Accutane, the brand name for isotretinoin, stands as one of the most powerful treatments for severe nodular acne that doesn’t respond to conventional therapies. According to the National Institutes of Health, isotretinoin works by shrinking sebaceous glands, reducing sebum production, normalizing skin cell turnover, and delivering anti-inflammatory effects.
But here’s where things get serious.
This medication comes with strict monitoring requirements, contraindications, and a list of potential interactions that can’t be ignored. One of the most common questions dermatology patients ask involves alcohol consumption during treatment.
The short answer? Mixing these two substances creates significant health risks that go far beyond a simple hangover.
Why Accutane and Alcohol Don’t Mix
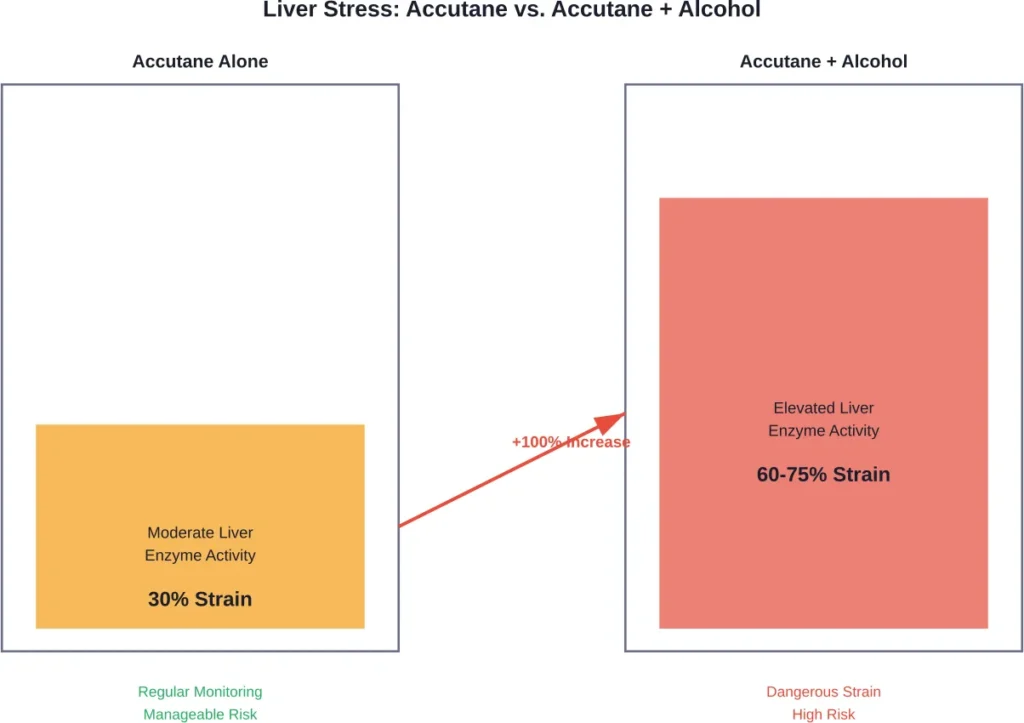
Both isotretinoin and alcohol are processed through the liver, and that’s where the fundamental problem begins. When someone takes Accutane, the liver metabolizes the medication along with its primary metabolites. According to StatPearls research published by the National Library of Medicine, liver enzyme elevations represent a known side effect of isotretinoin therapy.
Add alcohol into this equation, and the liver faces a double metabolic burden.
Ethanol metabolism produces acetaldehyde, a toxic compound that the liver must break down. Meanwhile, isotretinoin undergoes hepatic metabolism through the same pathways. This simultaneous processing forces the organ to work overtime, substantially increasing the strain on liver function.
Research documented in LiverTox, the NIH’s clinical resource on drug-induced liver injury, confirms that isotretinoin can cause serum aminotransferase elevations. While the medication hasn’t been definitively linked to acute liver injury with jaundice as frequently as other retinoids, the hepatotoxic potential remains a documented concern.
The Liver Enzyme Connection
Clinical monitoring during Accutane treatment requires regular blood work precisely because liver function changes can occur. The FDA-approved prescribing information mandates baseline liver function tests before starting isotretinoin therapy.
When alcohol enters the picture, enzyme levels can spike even higher. One academic case report documented acute liver failure induced by isotretinoin, demonstrating that severe hepatotoxicity, though rare, represents a real possibility. The severity of drug-induced liver injury ranges from mild enzyme elevations to acute liver failure requiring transplantation.
Alcohol consumption amplifies this risk profile considerably.
What the Medical Research Actually Says
Research on isotretinoin metabolism and pharmacokinetics has examined drug processing patterns. Does that mean drinking is safe? Absolutely not.
Studies focused narrowly on drug metabolism rates do not address the cumulative liver stress or clinical safety of combining these substances. Researchers have noted that after ceasing isotretinoin therapy, the recommended one-month period for contraceptive measures in fertile women appears adequate—a timeline that also applies to alcohol avoidance.
Here’s what science doesn’t show: large-scale clinical trials proving moderate alcohol consumption is safe during isotretinoin treatment. The absence of this evidence matters tremendously in clinical decision-making.
Individual Variability in Response
Medical literature emphasizes that patient responses to isotretinoin vary significantly. Factors that influence how someone tolerates the medication include:
- Baseline liver health and pre-existing hepatic conditions
- Dosage and duration of isotretinoin therapy
- Age and metabolic rate
- Concurrent medications and supplements
- Genetic variations in drug metabolism enzymes
Someone with existing liver compromise faces exponentially higher risks when mixing alcohol with Accutane. According to one PubMed study, hepatic disease or alcohol use history serves as a superior predictor of treatment abnormalities compared to baseline lab values alone.
Beyond Liver Damage: Other Serious Risks
Hepatotoxicity represents just one piece of the danger profile. Combining Accutane and alcohol creates additional health concerns that patients need to understand.
Psychiatric and Mental Health Effects
Isotretinoin has been associated with psychiatric side effects including depression, suicidality, and psychotic symptoms. According to research published in Annals of General Psychiatry, the first report of psychiatric effects came in 1982 when approximately 25% of cancer patients receiving isotretinoin developed depressive symptoms and suicidality.
Alcohol itself functions as a central nervous system depressant.
When someone dealing with acne—a condition already linked to mental health challenges—takes a medication with known psychiatric risks and adds alcohol, the combination can worsen mood instability, depressive episodes, and emotional volatility.
Pancreatitis Risk Elevation
The NIH’s LiverTox database notes that isotretinoin use has been linked to pancreatitis. Alcohol represents one of the leading causes of acute and chronic pancreatitis globally. Combining two substances that independently stress the pancreas creates a compounding risk that medical professionals take seriously.
Lipid Abnormalities and Triglyceride Spikes
Isotretinoin commonly causes elevations in serum lipids and triglycerides. The FDA prescribing information requires fasting lipid profiles before treatment begins. Alcohol consumption—particularly binge drinking or regular heavy use—also raises triglyceride levels.
When triglycerides reach severely elevated levels, the risk of pancreatitis increases dramatically. This represents another mechanism through which the Accutane-alcohol combination becomes medically dangerous.
| Risk Category | Accutane Alone | Alcohol Alone | Combined Effect |
|---|---|---|---|
| Liver Enzyme Elevation | Moderate risk | Dose-dependent risk | Significantly increased |
| Triglyceride Levels | Common increase | Moderate increase | Potentially dangerous elevation |
| Pancreatitis | Rare but documented | Well-established risk | Compounded risk |
| Mental Health Effects | Depression, mood changes | CNS depression | Amplified psychiatric symptoms |
| Dehydration | Dry skin, mucous membranes | Diuretic effect | Severe dehydration possible |
How Much Alcohol Creates Problems?
Community discussions and patient forums frequently debate whether occasional drinking or moderate consumption carries the same risks as heavy alcohol use. The medical reality is nuanced but cautious.
No established safe threshold exists for alcohol consumption during isotretinoin treatment. Research hasn’t identified a specific quantity—whether one drink per week or one drink per month—that medical professionals can confidently endorse as risk-free.
That said, dermatologists recognize that clinical scenarios vary.
Some healthcare providers may discuss the difference between someone having a single glass of wine at a wedding versus regular weekend drinking. However, these conversations happen on an individual basis, factoring in the patient’s specific health profile, lab results, dosage, and risk factors.
Why Blanket Recommendations Exist
Medical guidelines tend toward conservative recommendations for liability reasons, but also because predicting individual responses proves nearly impossible. Someone might have undiagnosed liver issues, genetic variations affecting drug metabolism, or other risk factors they’re unaware of.
Rather than establishing complex tiered guidance that might be misinterpreted, healthcare providers typically recommend complete alcohol avoidance during treatment. This approach eliminates ambiguity and maximizes safety.
Critical Conversations with Healthcare Providers
Before making any decisions about alcohol consumption during Accutane therapy, several factors require discussion with the prescribing dermatologist or physician:
- Current liver function test results and trends over time
- Baseline lipid panel values and monitoring schedule
- Personal or family history of liver disease or alcoholism
- Mental health status and psychiatric medication use
- Current isotretinoin dosage and treatment duration
- Any symptoms suggesting liver stress (fatigue, abdominal pain, jaundice)
Honest disclosure matters tremendously. Some patients fear judgment about drinking and withhold information from their doctors. This creates dangerous situations where providers can’t make fully informed treatment decisions or adjust monitoring protocols appropriately.
What Blood Work Reveals
Regular laboratory monitoring during Accutane treatment tracks several key markers:
- Alanine aminotransferase (ALT) and aspartate aminotransferase (AST) for liver function
- Triglycerides and cholesterol levels
- Complete blood count
- Pregnancy tests for those who can become pregnant
If someone drinks alcohol and lab values show concerning changes, the provider might reduce the isotretinoin dose, increase monitoring frequency, or discontinue treatment altogether. Early detection through blood work can prevent progression to serious liver injury.
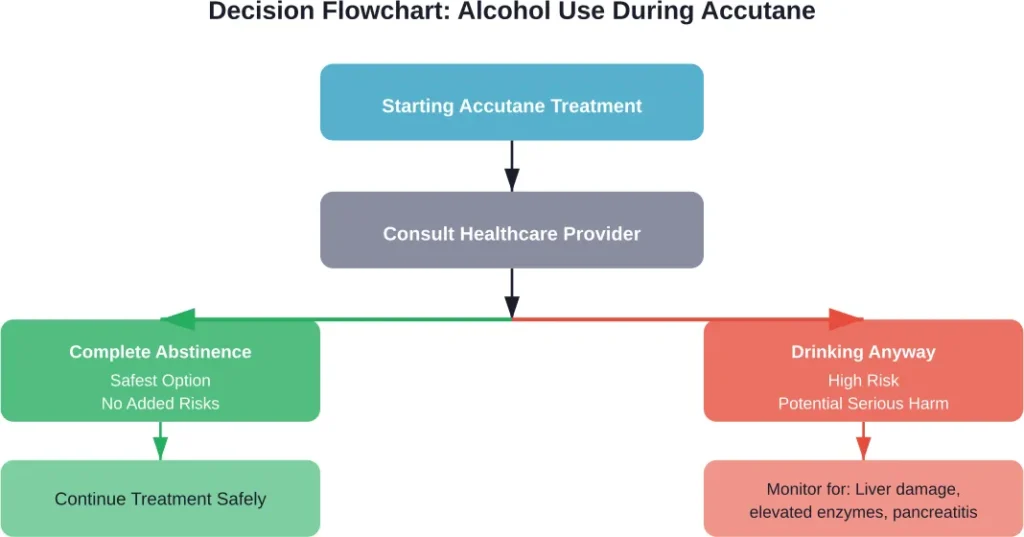
Warning Signs That Require Immediate Medical Attention
Anyone who consumes alcohol while taking Accutane should watch for symptoms indicating liver stress or other complications:
- Yellowing of skin or eyes (jaundice)
- Dark-colored urine or pale stools
- Severe abdominal pain, especially upper right quadrant
- Persistent nausea, vomiting, or loss of appetite
- Unusual fatigue or weakness
- Severe headaches or vision changes
- Worsening depression, suicidal thoughts, or psychiatric symptoms
These symptoms warrant immediate contact with a healthcare provider. Acute liver injury, pancreatitis, and other serious complications require prompt medical evaluation and intervention.
How Long After Stopping Accutane Can Drinking Resume?
Medical research examining isotretinoin pharmacokinetics suggests that one month represents an adequate waiting period after treatment completion. This timeline allows the medication and its metabolites to clear from the system.
The one-month recommendation appears consistently in medical literature and prescribing guidance. During this washout period, liver function can begin returning to baseline, and the interactive risks between isotretinoin and alcohol diminish.
Some dermatologists recommend waiting until follow-up blood work confirms normalized liver enzymes and lipid levels before resuming alcohol consumption. This personalized approach provides additional safety assurance based on individual response to treatment.
Practical Tips for Patients Who Choose to Drink
Despite medical recommendations, some patients decide to consume alcohol during treatment. For those individuals, harm reduction strategies become relevant:
- Inform the healthcare provider honestly about any drinking
- Request more frequent laboratory monitoring
- Limit consumption to minimal amounts (one drink on rare occasions)
- Avoid binge drinking or heavy alcohol use entirely
- Stay well-hydrated before, during, and after any alcohol consumption
- Watch carefully for warning symptoms
- Never drink if lab values show any concerning trends
These strategies don’t eliminate risk—they attempt to reduce it. The safest approach remains complete abstinence during treatment and for one month afterward.
The Dehydration Factor
Accutane causes significant drying effects throughout the body. According to NIH data, common side effects include dry skin, nosebleeds, conjunctivitis, and dry mucous membranes. Patients frequently experience chapped lips, dry eyes, and skin sensitivity.
Alcohol acts as a diuretic, promoting fluid loss through increased urination.
Combining these two dehydrating influences can lead to severe discomfort and potentially dangerous dehydration. Adequate hydration already requires conscious effort during isotretinoin therapy. Adding alcohol makes maintaining proper fluid balance even more challenging.
Real-World Patient Experiences
Community discussions reveal that many patients have consumed alcohol during Accutane treatment without immediate catastrophic consequences. This anecdotal reality sometimes creates confusion about whether medical warnings are overstated.
Here’s the thing though—the absence of immediate symptoms doesn’t mean no harm occurred.
Liver damage can develop gradually and silently. Enzyme elevations might not produce noticeable symptoms initially. Someone might drink occasionally throughout treatment, complete their course, and only discover elevated liver enzymes on post-treatment blood work.
Additionally, individual variation means one person’s experience doesn’t predict another’s outcome. Someone with robust liver function and low genetic risk might tolerate occasional drinking better than someone with undiagnosed liver compromise or specific enzyme deficiencies.
Relying on anecdotal experiences rather than medical guidance represents a gamble with long-term health.
Alternative Social Strategies
Many patients worry about social situations during treatment. College students, young adults, and others in environments where drinking represents common social activity face pressure and awkwardness around abstinence.
Strategies for navigating these situations include:
- Using non-alcoholic alternatives that look like cocktails
- Being upfront about medical treatment requirements
- Focusing on activities that don’t center on drinking
- Finding supportive friends who respect health decisions
- Remembering the temporary nature of treatment (most courses last 4-6 months)
The treatment period represents a relatively short window in the context of a full lifetime. Prioritizing skin health and overall wellbeing during this time creates better long-term outcomes than risking serious complications for temporary social comfort.
When Treatment Modifications Become Necessary
If laboratory monitoring reveals concerning changes during Accutane therapy—whether related to alcohol consumption or not—dermatologists have several options:
- Reducing the daily isotretinoin dose
- Implementing a treatment pause to allow values to normalize
- Increasing monitoring frequency
- Discontinuing treatment if abnormalities become severe
Early intervention based on lab trends prevents progression to serious injury. This monitoring system exists specifically to catch problems before they become irreversible.
Patients who drink alcohol during treatment and develop abnormal lab values face difficult decisions. Continuing both substances isn’t medically advisable. The choice becomes either eliminating alcohol or potentially stopping Accutane treatment altogether.
The Bigger Picture: Medication Compliance and Treatment Success
Research on treatment compliance in acne shows that various disease-related and social factors influence whether patients follow medical recommendations. The psychological burden of severe acne creates complex decision-making around treatments that carry significant restrictions.
However, isotretinoin offers the possibility of long-term remission or cure for severe acne that has resisted other therapies. Many patients achieve clear skin that remains stable for years or permanently after completing treatment.
Compromising treatment safety or effectiveness for alcohol consumption during this relatively brief treatment window risks undermining the entire therapeutic goal. The cost-benefit analysis heavily favors temporary abstinence to maximize treatment success and safety.
Frequently Asked Questions
Medical guidance recommends avoiding all alcohol during isotretinoin treatment because both substances stress the liver. While one drink likely won’t cause immediate catastrophic harm in most people, no safe threshold has been established through research. The risk increases with frequency and quantity. Discuss any planned alcohol consumption with the prescribing healthcare provider rather than making this decision independently.
Blood tests during Accutane treatment measure liver enzymes, lipids, and other markers—not alcohol directly. However, drinking can cause elevations in liver enzymes (ALT, AST) and triglycerides that will appear on lab results. These abnormal values might prompt questions about alcohol use and could lead to dose adjustments or treatment discontinuation.
Isotretinoin and its metabolites typically clear from the body within approximately one month after stopping treatment. This is why medical guidelines recommend waiting at least one month before pregnancy becomes safe and why this same timeline applies to resuming alcohol consumption. Some providers recommend waiting until follow-up blood work confirms normalized values before drinking.
If alcohol consumption occurs once accidentally, monitor carefully for warning symptoms like abdominal pain, jaundice, severe fatigue, or nausea. Contact the healthcare provider to report the incident and discuss whether additional lab monitoring is needed. One isolated incident typically doesn’t cause permanent damage, but honesty with medical providers ensures appropriate monitoring and safety precautions going forward.
Isotretinoin doesn’t significantly alter how alcohol is metabolized or change intoxication levels directly. However, the combined effects on the liver, the dehydrating properties of both substances, and potential interactions affecting mental state can make the overall experience more unpredictable and potentially dangerous. The concern isn’t about getting more intoxicated but about compounding health risks.
Medical guidance suggests waiting at least one month after completing isotretinoin treatment before resuming alcohol consumption. This allows the medication to clear from the system and liver function to return to baseline. Some dermatologists recommend confirming normalized lab values through follow-up blood work before drinking. Once treatment is complete and appropriate time has passed, previous drinking patterns can typically resume safely.
No type of alcoholic beverage is considered safer than others during Accutane treatment. Whether beer, wine, or liquor, all alcoholic drinks are metabolized by the liver and create the same interactive risks with isotretinoin. The concern relates to alcohol content and liver processing burden, not the specific type of drink. Complete abstinence from all forms of alcohol represents the safest approach during treatment.
Making Informed Decisions About Your Health
Accutane represents a powerful tool for treating severe acne that has failed to respond to other therapies. Research, including Cochrane Database systematic reviews, indicates isotretinoin is highly effective for severe acne, offering many patients the possibility of long-term clear skin.
But this effectiveness comes with requirements and risks that demand respect.
The interaction between isotretinoin and alcohol isn’t a minor consideration or an overly cautious medical recommendation. Both substances independently stress the liver, and combining them creates genuinely dangerous potential for hepatotoxicity, elevated triglycerides, pancreatitis, and worsening psychiatric effects.
Medical professionals don’t issue these warnings to restrict social activities or exert control. The guidance stems from documented risks, case reports of serious complications, and the fundamental pharmacology of how these substances affect the body.
Treatment typically lasts four to six months—a relatively short period that offers the potential for transformative results. Prioritizing safety during this window maximizes the likelihood of achieving clear skin without complications or long-term health consequences.
The decision ultimately belongs to each individual patient, but it should be an informed decision made in consultation with healthcare providers, based on accurate medical information rather than anecdotal experiences or social pressure.
Your health is worth protecting. Your liver is worth preserving. And the clear skin you’re working toward deserves the best possible chance of success through safe, compliant treatment practices.
If acne has led to considering Accutane treatment, work closely with a dermatologist who can provide personalized guidance based on individual health factors, monitor progress carefully through regular blood work, and help navigate the requirements of this powerful but demanding medication.
