Quick Summary: If you accidentally ate an edible while pregnant, don’t panic. According to the CDC, cannabis use during pregnancy may affect fetal development, but a single accidental exposure is unlikely to cause immediate harm. Contact your healthcare provider right away to discuss monitoring and avoid any further cannabis use throughout pregnancy and breastfeeding.
Picture this: You’re at a family gathering or a friend’s place, and you grab what looks like a regular brownie or gummy from the counter. An hour later, you realize with horror that it wasn’t just any snack—it was a cannabis edible. And you’re pregnant.
This scenario happens more often than you might think. With cannabis legalization spreading across many states and edibles looking increasingly like everyday treats, accidental consumption is a real concern for pregnant women.
The good news? A single accidental exposure is different from regular use. But understanding what happens next, what risks exist, and when to seek help can make all the difference in managing this stressful situation.
Understanding Cannabis Edibles and Pregnancy
Cannabis edibles are food products infused with THC (delta-9-tetrahydrocannabinol), the main psychoactive compound in marijuana. Unlike smoking or vaping, edibles are metabolized through the digestive system, which creates different effects and timing.
According to the CDC, cannabis may be harmful during pregnancy no matter how it’s consumed—smoking, vaping, dabbing, eating, drinking, or even applying cannabis-infused creams to the skin. The agency emphasizes that THC readily crosses the placenta, potentially affecting fetal development.
Research from the NIH indicates that marijuana is the most commonly used dependent substance in pregnancy, with up to half of users continuing their use while pregnant. This results in up to 34% of pregnancies impacted. Prevalence rates among pregnant individuals range from 3.9% to 16.0% according to ACOG data.
How THC Affects Pregnancy
The main active chemical in marijuana, THC, doesn’t just stay in your system—it crosses the placenta and reaches your developing baby. Cannabinoid receptors have been identified in fetal brain tissue, which means THC can interact directly with your baby’s developing nervous system.
That said, there’s a significant difference between a single accidental exposure and ongoing cannabis use throughout pregnancy.
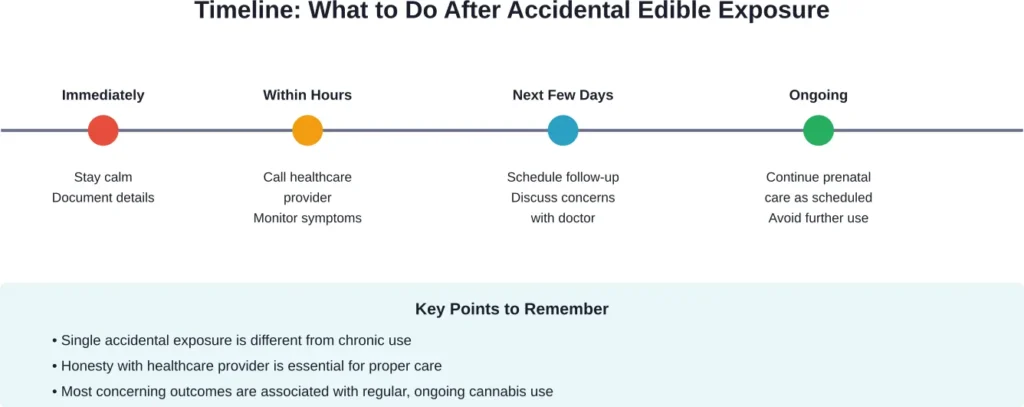
Immediate Steps After Accidental Edible Consumption
Real talk: If you’ve just realized you accidentally consumed an edible while pregnant, here’s what to do right now.
Stay calm. Panicking won’t help the situation, and stress itself can affect pregnancy. A single exposure is not the same as chronic use.
Contact your healthcare provider immediately. Call your OB-GYN, midwife, or primary care doctor. They can assess your specific situation, including how far along you are in pregnancy and the estimated dose consumed.
Monitor yourself for effects. Edibles can take 30 minutes to 2 hours to produce noticeable effects. The delayed onset is one reason edibles can be particularly unpredictable—effects may not manifest immediately, making it harder to connect symptoms with consumption.
Stay hydrated and rest. If you begin feeling the psychoactive effects, find a safe, comfortable place to rest. Have someone stay with you if possible.
Document what happened. Note the time of consumption, the type of edible (gummy, brownie, chocolate, etc.), and the estimated THC content if known. This information helps your healthcare provider assess potential exposure levels.
Potential Risks of Cannabis Exposure During Pregnancy
Understanding the risks helps put accidental exposure into context. According to authoritative health organizations, regular cannabis use during pregnancy has been associated with several concerning outcomes.
Effects on Fetal Development
The CDC reports that using cannabis during pregnancy may affect your baby’s development and put you at risk of pregnancy complications. Research published in medical journals has identified several potential concerns:
Low birth weight. Some studies have found associations between prenatal cannabis exposure and reduced birth weight, though results vary across research.
Preterm birth. ACOG notes that cannabis use in pregnancy has been associated with spontaneous preterm birth, though the exact mechanisms aren’t fully understood.
Neurodevelopmental concerns. Animal studies have shown that chronic prenatal THC exposure can affect offspring neurodevelopment, alter metabolic and cardiovascular function, and cause long-term behavioral changes. However, translating animal research to human outcomes requires caution.
Placental function. Research from Oregon Health & Science University found that chronic prenatal delta-9-tetrahydrocannabinol exposure adversely impacts placental function and development in animal models.
Birth Defects and Developmental Outcomes
According to MotherToBaby data from the NIH, birth defects can happen in any pregnancy for different reasons. Out of all babies born each year, about 3 out of 100 (3%) will have a birth defect. Some studies have examined whether marijuana exposure might increase this baseline risk, though results have been mixed and many studies don’t adequately control for other factors like tobacco use or other substances.
The challenge with interpreting this research? Many studies can’t distinguish between effects from marijuana alone versus combined exposures to multiple substances, making definitive conclusions difficult.
Why Edibles Present Unique Concerns
Edibles aren’t just another way to consume cannabis—they come with specific risks that make them particularly concerning during pregnancy.
Unpredictable Dosing
Here’s the thing: Edibles are metabolized differently by different individuals and can deliver large, unpredictable doses regardless of the amount ingested. The effects can take anywhere from 30 minutes to 2 hours to fully manifest, depending on factors like metabolism, what else was eaten, and individual body chemistry.
This delay means someone might consume more thinking the first dose didn’t work, leading to unexpectedly intense effects hours later.
Higher THC Concentrations
Modern cannabis products often contain significantly higher THC concentrations than marijuana from previous decades. Some edibles can contain 10-100 mg of THC per serving, and homemade edibles may have even more variable potency.
For context, smoking cannabis typically delivers effects almost immediately, allowing users to titrate their dose. Edibles remove this control mechanism entirely.
Longer Duration of Effects
When cannabis is ingested, the liver converts THC into a more potent form called 11-hydroxy-THC. This metabolite is more psychoactive and has a longer half-life, meaning edible effects can last 6-8 hours or even longer—much longer than smoked cannabis.
What Medical Professionals Recommend
The American College of Obstetricians and Gynecologists now recommends universal screening for cannabis use during the prepregnancy, pregnancy, and postpartum periods. This guidance reflects growing concern about cannabis exposure during critical developmental windows.
ACOG’s position is clear: Women who are pregnant, planning to get pregnant, or breastfeeding should not use marijuana in any form. This recommendation is based on the principle that no amount of cannabis has been proven safe during pregnancy.
The CDC echoes this guidance, stating that cannabis may be harmful to your baby no matter how it’s used. If you’re using cannabis and are pregnant, planning to become pregnant, or breastfeeding, they recommend talking to your doctor about cessation strategies and support.
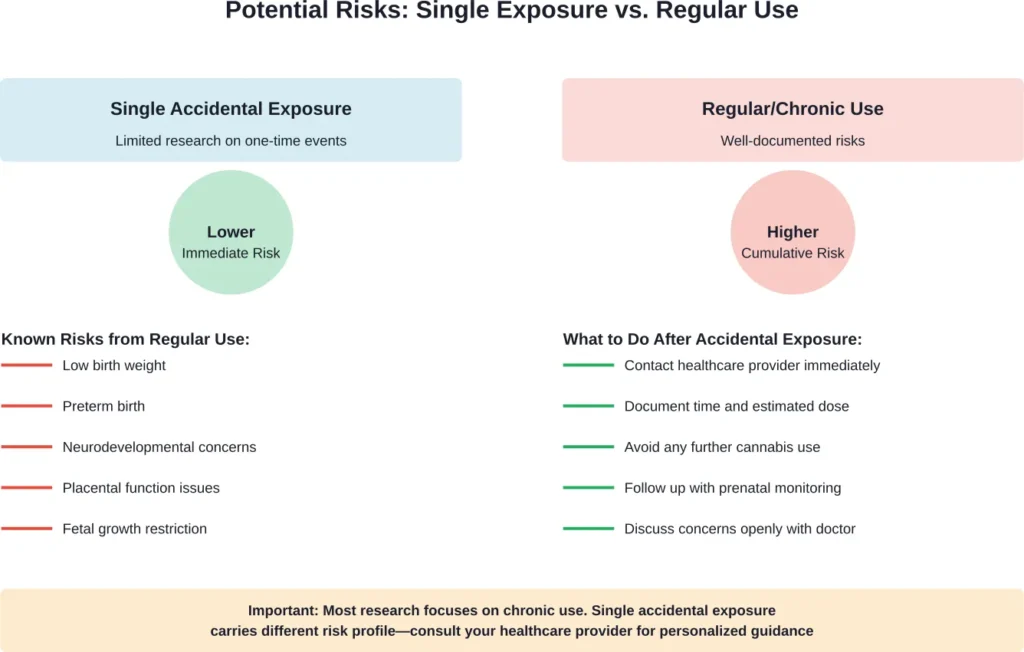
Single Exposure vs. Chronic Use: An Important Distinction
Now, this is where context matters. Most research on cannabis and pregnancy focuses on regular, ongoing use—not single accidental exposures.
Women who use marijuana regularly during pregnancy face cumulative exposure that builds over time. The research showing developmental concerns, low birth weight, and preterm birth primarily involves chronic use patterns, not isolated incidents.
Does this mean a single exposure is completely risk-free? No healthcare provider can guarantee that. But the risk profile is fundamentally different from regular consumption throughout pregnancy.
What matters most after accidental exposure is what happens next: stopping all cannabis use, being honest with your healthcare provider, and ensuring appropriate prenatal monitoring going forward.
Monitoring and Follow-Up Care
After accidental edible consumption during pregnancy, your healthcare provider may recommend additional monitoring or assessments. This might include:
Standard prenatal checkups. In many cases, continuing with your regular prenatal care schedule is sufficient, especially if the exposure occurred early and was truly isolated.
Ultrasound monitoring. Depending on timing and circumstances, your provider might order additional ultrasounds to monitor fetal growth and development.
Honest communication. This is critical. Your doctor needs to know about the exposure to provide appropriate care, and this information is protected by medical confidentiality laws.
Substance use screening. Your provider may offer resources for substance use support, not as judgment but as standard care for anyone with potential exposure.
Safe Alternatives for Common Pregnancy Symptoms
Many pregnant women turn to cannabis edibles hoping to manage legitimate pregnancy symptoms like nausea, anxiety, or sleep problems. But safer alternatives exist for these common complaints.
| Symptom | Cannabis Alternative | Safe Pregnancy Options |
|---|---|---|
| Morning sickness and nausea | THC edibles or gummies | Vitamin B6, ginger tea, small frequent meals, prescription antiemetics if needed |
| Anxiety and stress | CBD or THC products | Prenatal yoga, meditation, therapy, approved medications under doctor supervision |
| Sleep problems | Cannabis edibles | Sleep hygiene practices, pregnancy pillow, relaxation techniques, approved sleep aids |
| Pain management | THC for chronic pain | Acetaminophen (Tylenol), physical therapy, prenatal massage, warm baths |
| Appetite issues | Marijuana for appetite stimulation | Small frequent meals, nutrient-dense smoothies, working with nutritionist |
Nausea and Morning Sickness
According to CDC data from eight states, 4.2% of women reported marijuana use during pregnancy, with the most frequently reported reasons being to relieve stress or anxiety, nausea or vomiting, and pain. But effective alternatives exist that don’t carry the same risks.
Vitamin B6 supplements, ginger in various forms (tea, capsules, candies), eating small frequent meals, and staying hydrated can all help manage morning sickness. For severe cases, prescription medications like ondansetron or doxylamine-pyridoxine combinations are proven safe and effective.
Anxiety and Stress Management
Pregnancy anxiety is real and can be overwhelming. Instead of cannabis, consider prenatal-safe options like cognitive behavioral therapy, mindfulness meditation, prenatal yoga, or talking with a therapist specializing in perinatal mental health.
Some pregnant women may need medication for anxiety or depression, and several options exist that are safer than cannabis. Your healthcare provider can discuss risks and benefits based on your specific situation.
The Legal and Social Context
Cannabis legalization has created a perception that marijuana is safe, including during pregnancy. This perception doesn’t align with medical evidence.
As cannabis has been legalized in Canada and increasingly across U.S. states, researchers note that the lack of information regarding its safety in the pregnant and lactating population has become more apparent. Legalization changes access and social attitudes but doesn’t change biological effects on fetal development.
Some states have laws that complicate cannabis use during pregnancy. Testing positive for THC during pregnancy or at delivery can trigger child protective services involvement in certain jurisdictions, though laws vary widely by state.
Breastfeeding Considerations
The guidance against cannabis doesn’t end at delivery. THC passes into breast milk and can be detected in nursing infants.
According to the CDC, if you are breastfeeding and using cannabis, you should talk to your doctor. The American Academy of Pediatrics discourages cannabis use during breastfeeding due to concerns about infant exposure during a critical period of brain development.
THC can remain in breast milk for up to six days after use, meaning even occasional use results in ongoing infant exposure.
Community Experiences and Support
Community discussions reveal that accidental edible consumption during pregnancy is more common than many realize. Many women share experiences of grabbing the wrong brownie at a party or eating food that wasn’t properly labeled.
The overwhelming advice from both healthcare providers and women who’ve been through this? Contact your doctor immediately, be honest about what happened, and don’t continue using cannabis during pregnancy.
Support matters. If you’re struggling with cannabis dependence during pregnancy, resources exist. Your healthcare provider can connect you with substance use counselors, support groups, and treatment programs that specialize in pregnancy-related care.
Preventing Accidental Exposure
The best approach is prevention. If you’re pregnant or planning to become pregnant, consider these strategies:
Communicate clearly with household members. If others in your home use cannabis products, ask them to store edibles separately from regular food and clearly label everything.
Be cautious at social gatherings. Before eating homemade baked goods or candies at parties, ask whether they contain cannabis. Don’t assume something is cannabis-free just because it looks normal.
Check packaging carefully. Many commercial edibles are packaged to look like regular candy or snacks. Read labels before consuming anything you didn’t personally purchase or prepare.
Store your food separately. If you live with cannabis users, designate separate storage areas for your food to eliminate mix-up risks.
Frequently Asked Questions
A single accidental exposure is unlikely to cause birth defects on its own. Most research showing increased risks involves regular, chronic cannabis use throughout pregnancy rather than isolated incidents. However, no amount of cannabis has been proven completely safe during pregnancy, which is why contacting your healthcare provider after any exposure is important for appropriate monitoring.
THC can be detected in urine for 3-30 days after use, depending on factors like frequency of use, metabolism, and body composition. For someone who accidentally consumed a single edible, THC would typically clear faster than for regular users. However, THC is fat-soluble and can be stored in fatty tissues, potentially extending detection windows.
Yes, absolutely. Honest communication with your healthcare provider is essential for receiving appropriate prenatal care. Medical confidentiality protects this information, and your doctor needs to know about any potential exposures to monitor your pregnancy properly. Healthcare providers are there to help, not judge.
Research on cannabis and miscarriage shows mixed results, and most studies focus on regular use rather than single exposures. While some research has suggested possible associations between cannabis use and pregnancy loss, establishing direct causation is difficult because many studies don’t adequately control for other factors like tobacco use, alcohol, or other substances. A single accidental exposure is unlikely to directly cause miscarriage.
No. The CDC and ACOG recommend avoiding all cannabis products during pregnancy, including CBD. CBD products are poorly regulated, often contain varying amounts of THC, and haven’t been adequately studied for safety during pregnancy. Additionally, CBD itself crosses the placenta and could potentially affect fetal development.
All trimesters involve critical developmental processes that could potentially be affected by cannabis exposure. The first trimester involves organ formation, the second trimester includes rapid brain development, and the third trimester is crucial for brain maturation and growth. Rather than focusing on which trimester is “most” dangerous, the medical consensus is to avoid cannabis throughout the entire pregnancy.
No. The CDC, ACOG, and American Academy of Pediatrics all recommend against cannabis use while breastfeeding. THC passes into breast milk and can be detected in nursing infants. THC can remain in breast milk for up to six days after use, exposing your baby during a critical period of brain development.
Moving Forward After Accidental Exposure
If you’ve accidentally consumed an edible during pregnancy, the path forward is clear: contact your healthcare provider, be honest about what happened, avoid any further cannabis use, and continue with appropriate prenatal care.
Most women who experience a single accidental exposure go on to have healthy pregnancies and healthy babies. What matters most is taking the right steps after exposure and ensuring the rest of your pregnancy is as healthy as possible.
Don’t let guilt or fear prevent you from seeking appropriate medical care. Healthcare providers understand that accidents happen, and their priority is supporting you and your baby’s health throughout pregnancy.
Conclusion: Knowledge and Action Make the Difference
Accidentally eating an edible while pregnant is understandably frightening, but it’s important to put the situation in perspective. Single accidental exposures carry different risks than regular, chronic cannabis use throughout pregnancy.
The research is clear that ongoing cannabis use during pregnancy poses real risks to fetal development, including potential effects on birth weight, gestational age, neurodevelopment, and placental function. These concerns are why every major medical organization recommends against marijuana use during pregnancy and breastfeeding.
But research on single accidental exposures is limited, and most concerning outcomes are associated with repeated use rather than isolated incidents. This doesn’t mean accidental exposure carries zero risk—it means the risk profile is fundamentally different.
What you do next matters far more than the single exposure itself. Contact your healthcare provider immediately, document what happened, be completely honest about the circumstances, and commit to avoiding all cannabis use for the remainder of your pregnancy and while breastfeeding.
Take action today: If you’ve accidentally consumed an edible while pregnant, call your healthcare provider now. If you’re using cannabis regularly during pregnancy, talk to your doctor about safe cessation strategies and alternative treatments for whatever symptoms you’re trying to manage. Your baby’s health depends on the choices you make from this point forward.
