Quick Summary: Picking at a basal cell carcinoma can cause bleeding, infection, and scarring without removing the cancer itself. Manipulating the lesion may disrupt the tissue but won’t eliminate malignant cells, potentially complicating diagnosis and treatment. Professional medical removal through surgery, Mohs surgery, or other dermatologist-supervised methods remains the only effective way to treat BCC safely.
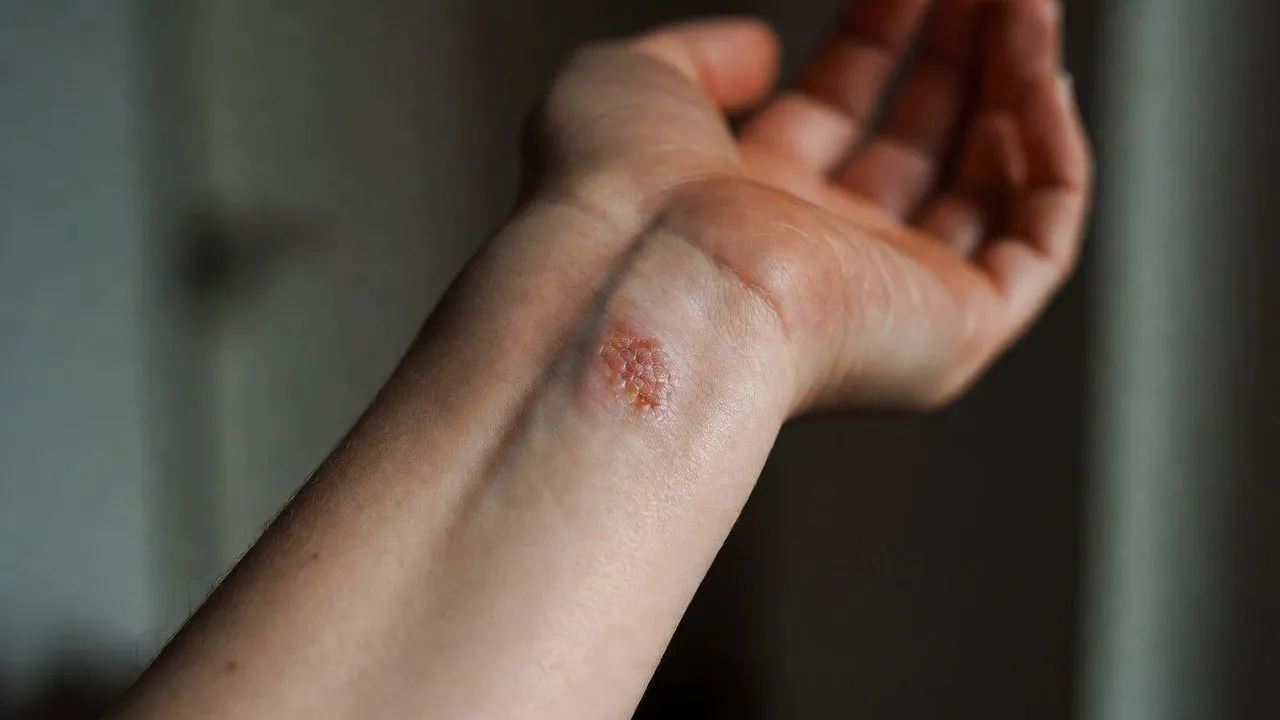
Spotting a strange growth on your skin can trigger immediate anxiety. That pearly bump on your nose or scaly patch on your shoulder begs to be scratched, picked, or somehow removed.
But here’s the thing—basal cell carcinoma isn’t like a scab or pimple. It’s a type of skin cancer that requires proper medical intervention.
Picking at it won’t make it go away. In fact, it can create a cascade of complications that make treatment more difficult and outcomes worse.
Understanding Basal Cell Carcinoma
Basal cell carcinoma represents the most common type of skin cancer diagnosed worldwide. According to the American Cancer Society, BCC develops in the basal cells that make new skin cells as old ones die off.
These cancers typically appear on sun-exposed areas like the face, neck, and arms. They often present as slightly transparent bumps, though they can take various forms including flat, scaly patches or sores that don’t heal.
Most basal cell carcinomas grow slowly and rarely spread to other parts of the body. That said, ignoring them creates serious problems.
The cancer can invade nearby skin and deeper tissues over time. Untreated BCC can damage cartilage, bone, and other structures beneath the skin surface.
Why BCC Looks Tempting to Pick
Basal cell carcinomas frequently develop characteristics that make them feel like something you should remove yourself:
- Pearly or waxy texture that feels raised
- Central depression or ulceration that resembles a sore
- Crusting or scabbing that never quite heals
- Bleeding with minimal trauma
- Texture different from surrounding normal skin
These features trigger natural grooming behaviors. The human impulse to remove irregularities from skin runs deep.
Real talk: that impulse can lead to significant harm when dealing with malignant tissue.
What Actually Happens When You Pick at BCC
Manipulating a basal cell carcinoma produces several immediate effects, none of them beneficial for treatment or outcome.
Bleeding and Tissue Disruption
Basal cell carcinomas often bleed easily because the abnormal cell growth creates fragile tissue with irregular blood vessel formation. Picking disrupts this tissue structure.
The lesion will bleed, sometimes profusely for such a small area. It may scab over temporarily, giving the false impression that you’ve removed something harmful.
But the malignant cells extend deeper than the superficial tissue you’ve disturbed. The cancer remains beneath the surface, continuing to grow and invade.
Infection Risk
Breaking the skin barrier on a BCC opens the door for bacterial infection. Your hands and fingernails carry bacteria that can colonize the open wound.
An infected basal cell carcinoma becomes harder to diagnose and treat. The inflammation from infection can mask the cancer’s true margins and characteristics.
Dermatologists need clear tissue to make accurate assessments. Infection complicates that process significantly.
Scarring Without Cancer Removal
Repeated picking creates scar tissue in and around the carcinoma. This scar tissue doesn’t replace the cancer—it forms alongside and over it.
When treatment eventually becomes necessary (and it will), the surgeon must work through this scarring. That can complicate surgical margins and make complete removal more challenging.
Sound familiar? The scar you created trying to remove the lesion actually makes professional removal harder.

Diagnostic Confusion
Dermatologists diagnose basal cell carcinoma through visual examination and biopsy. When you’ve been picking at a lesion, the tissue characteristics change.
The doctor sees inflamed, traumatized tissue rather than the cancer’s natural presentation. This can delay accurate diagnosis or require multiple biopsies to get clean tissue samples.
Early detection of basal cell carcinoma provides the best chance of removal with minimal scarring. Picking interferes with that early detection window.
Why Professional Removal Matters
Basal cell carcinoma requires complete removal of all malignant cells to prevent recurrence and local tissue damage. Self-manipulation can’t achieve this goal.
Mohs Surgery: The Gold Standard
For many basal cell carcinomas, Mohs surgery represents the most effective treatment option. This specialized technique allows surgeons to remove tissue layer by layer.
The surgeon examines each layer under a microscope in an adjacent lab, identifying exactly where cancerous cells remain. The process continues until no microscopic cancer cells are found.
This precision maximizes cancer removal while minimizing damage to healthy tissue. It’s particularly valuable for BCCs on the face, where tissue preservation matters for cosmetic outcomes.
Standard Surgical Excision
For lower-risk basal cell carcinomas, standard surgical excision works well. The surgeon removes the visible cancer plus a margin of normal-appearing tissue around it.
The removed tissue goes to a pathology lab for examination. If the margins show cancer cells, additional surgery may be necessary.
This approach offers high cure rates for appropriately selected cases.
Other Treatment Options
Depending on the BCC’s size, location, and characteristics, dermatologists may recommend:
- Electrodesiccation and curettage (scraping and burning)
- Cryotherapy (freezing)
- Topical medications for superficial lesions
- Radiation therapy in specific circumstances
Each method requires professional administration and follow-up. None can be replicated through picking or self-treatment.
| Treatment Method | Best For | Cure Rate Range |
|---|---|---|
| Mohs Surgery | High-risk areas, recurrent BCC | 97-99% for primary BCC |
| Surgical Excision | Low-risk, well-defined lesions | 90-95% for primary BCC |
| Electrodesiccation | Small, low-risk BCCs | 85-90% cure rate |
| Topical Therapy | Superficial BCC only | 70-90% depending on lesion |
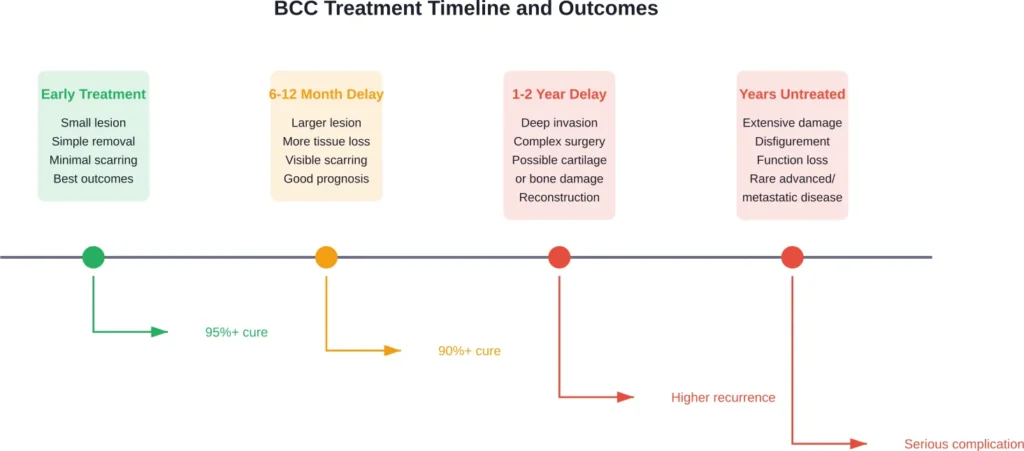
Consequences of Delaying Treatment
While basal cell carcinoma grows slowly and rarely metastasizes, delaying professional treatment creates progressively worse outcomes.
Local Tissue Invasion
Untreated BCC continues invading deeper into surrounding tissue. It can destroy skin, fat, muscle, cartilage, and even bone over time.
On the nose or ear, this invasion can cause significant disfigurement. On the scalp, it can penetrate to the skull. Near the eye, it can threaten vision.
The longer treatment waits, the more extensive the required surgery becomes.
Functional Impairment
Advanced basal cell carcinomas can interfere with normal function. A BCC on the eyelid may prevent proper eye closure. One near the mouth might affect eating or speaking.
Lesions on the nose can erode through cartilage, creating breathing difficulties and severe cosmetic deformity.
These complications become permanent if the cancer advances far enough before treatment.
Rare But Serious Progression
In rare cases, basal cell carcinoma can become locally advanced or even metastasize to other body parts. This happens infrequently but represents a life-threatening development.
Advanced BCC may require systemic therapies including targeted medications or immunotherapy in addition to surgery.
Early treatment prevents these rare but serious outcomes.
When to See a Dermatologist
Don’t ignore suspicious-looking changes to skin and moles. Make an appointment with a doctor or dermatologist if any spot on the skin:
- Changes in size, shape, or color
- Bleeds easily with minimal contact
- Develops a pearly or waxy appearance
- Forms a persistent sore that doesn’t heal
- Creates a raised border with central depression
- Grows steadily over weeks or months
Basal cell carcinoma often appears on sun-exposed areas but can develop anywhere on the body. People with fair skin, significant sun exposure history, or previous skin cancers face higher risk.
That said, BCC can affect anyone regardless of skin tone or background.
What to Expect at Your Appointment
Dermatologists examine suspicious lesions visually, often using magnification. If they suspect basal cell carcinoma, they’ll perform a biopsy.
The biopsy involves removing a small tissue sample under local anesthesia. The sample goes to a lab where a pathologist examines it under a microscope.
Results typically return within several days to a week. If the biopsy confirms BCC, the dermatologist discusses treatment options based on the cancer’s characteristics and location.
Preventing Basal Cell Carcinoma
While some risk factors for BCC can’t be controlled, limiting UV exposure significantly reduces risk. According to the American Cancer Society, indoor tanning can increase the risk of basal and squamous cell skin cancers by 40% and the risk of melanoma by 27%.
Protection strategies include:
- Using broad-spectrum sunscreen with SPF 30 or higher
- Seeking shade during peak sun hours (10 AM to 4 PM)
- Wearing protective clothing including wide-brimmed hats
- Avoiding indoor tanning beds completely
- Performing regular skin self-examinations
- Getting annual skin checks from a dermatologist if at higher risk
No amount of tanning is safe for skin. A tan won’t prevent skin cancer or skin aging—it represents skin damage at the cellular level.
Living With a BCC Diagnosis
Receiving a basal cell carcinoma diagnosis understandably causes concern. But this represents one of the most treatable forms of cancer when caught early.
Most people who develop BCC undergo treatment and return to normal activities quickly. Modern surgical techniques minimize scarring, especially when treatment happens promptly.
After successful BCC treatment, follow-up care matters. People who’ve had one basal cell carcinoma face increased risk of developing others.
Regular dermatology appointments allow early detection of any new lesions. This ongoing surveillance provides peace of mind and catches potential problems early.
Frequently Asked Questions
Basal cell carcinoma rarely spreads (metastasizes) to distant body parts, and picking won’t cause metastasis. However, picking can cause local spreading through tissue disruption, infection, and delayed proper treatment. The cancer continues growing deeper into surrounding tissue regardless of surface manipulation.
No. Basal cell carcinomas don’t spontaneously resolve without treatment. They continue growing slowly but persistently, invading deeper tissue over time. Only professional medical removal can eliminate the cancer completely.
While BCCs grow slowly, delaying treatment allows deeper invasion and more extensive damage. Schedule treatment as soon as possible after diagnosis. Waiting months or years increases the complexity of required surgery and worsens cosmetic outcomes. Early treatment provides the best results with minimal tissue loss.
Mohs surgery removes tissue layer by layer with immediate microscopic examination, ensuring complete cancer removal while preserving maximum healthy tissue. Regular excision removes the visible cancer plus a safety margin in one procedure, with lab results available days later. Mohs surgery offers higher cure rates and better tissue conservation for high-risk or cosmetically sensitive areas.
No over-the-counter products or natural remedies can effectively treat basal cell carcinoma. These cancers require professional medical intervention to ensure complete removal of all malignant cells. Attempting self-treatment delays proper care and allows the cancer to advance.
Inform the dermatologist about the picking behavior during your appointment. While this complicates diagnosis and treatment somewhat, doctors encounter this situation regularly. They can still perform biopsy and treatment, though healing may take longer due to the previous trauma. Stop picking immediately and seek professional evaluation.
Scar size and visibility depend on the lesion’s size, location, and chosen treatment method. Small BCCs caught early often leave minimal scarring. Mohs surgery maximizes tissue preservation, reducing scar size. Advanced techniques including plastic surgery reconstruction can minimize scarring for larger lesions. Early treatment generally produces better cosmetic outcomes than waiting until the cancer grows larger.
Taking Action on Suspicious Skin Lesions
That strange spot on your skin deserves professional evaluation, not amateur removal attempts. Basal cell carcinoma represents a manageable diagnosis when addressed appropriately.
Picking creates complications without providing any benefit. It can’t remove the cancer, and it makes eventual treatment more difficult.
The smart approach? Schedule an appointment with a dermatologist for any suspicious skin changes. Early detection and professional treatment provide excellent outcomes with minimal impact on your life.
Modern medicine offers multiple effective treatment options for BCC. Take advantage of them rather than gambling with self-treatment that can’t succeed.
Contact a board-certified dermatologist today if you’ve noticed concerning skin changes. Professional care makes all the difference in outcomes, scarring, and peace of mind.