Quick Summary: Having sex with a UTI is generally not recommended as it can worsen symptoms, prolong recovery, and potentially spread bacteria to your partner. Medical professionals typically advise waiting until the infection has completely cleared—usually 1-2 weeks after completing antibiotics—before resuming sexual activity to avoid complications and ensure proper healing.
Urinary tract infections affect millions of people every year, with women experiencing these uncomfortable infections at significantly higher rates than men. According to the CDC, UTIs are among the most common bacterial infections, leading to millions of healthcare visits annually.
When dealing with the burning, urgency, and discomfort of a UTI, questions about sexual activity naturally arise. The short answer? Most healthcare providers recommend against it.
But the reality is more nuanced than a simple yes or no. Understanding what happens when you have sex during a UTI—and why waiting matters—can help you make informed decisions about your health and recovery.
What Happens When You Have Sex With a UTI
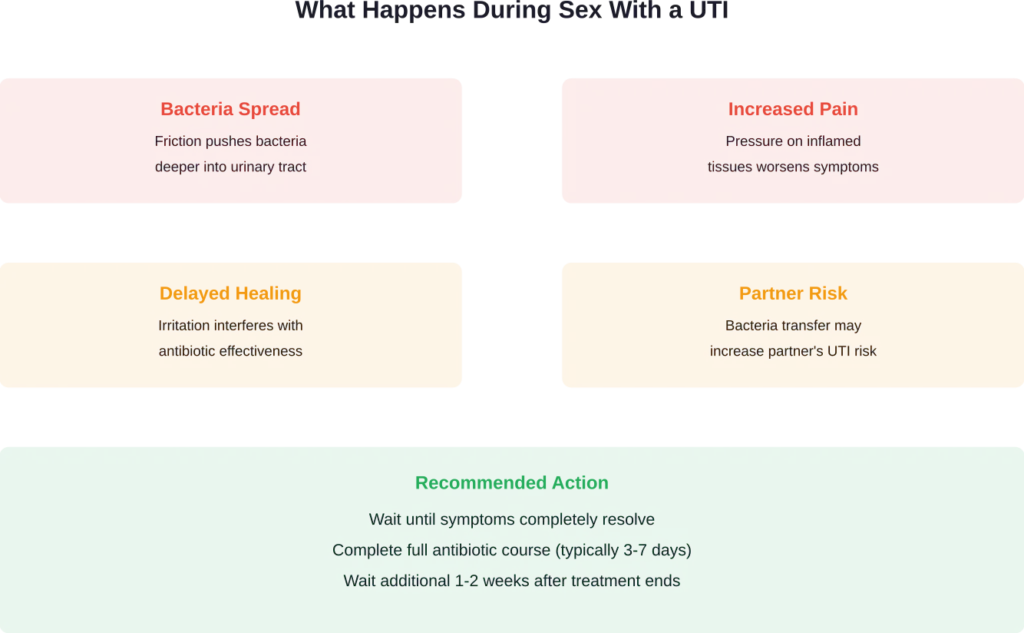
Sexual activity during an active urinary tract infection creates several problems that can interfere with healing. The mechanical friction involved in intercourse can irritate already inflamed urinary tissues, making painful symptoms significantly worse.
Here’s what actually occurs. The urethra—the tube that carries urine from your bladder—sits very close to the vaginal opening. During sex, this area experiences pressure and movement that can push bacteria deeper into the urinary tract.
When you already have an infection, this bacterial movement can spread the infection further or introduce additional bacteria into an already compromised system. Research published in the Journal of General Internal Medicine found that sexual intercourse increases the risk of symptomatic UTIs, with an adjusted hazard ratio of 3.42 (95% CI 1.49–7.80) appearing 2 calendar days after sexual activity in post-menopausal women.
Physical Discomfort and Pain
Beyond spreading bacteria, sex with a UTI typically hurts. The inflammation in your urinary tract makes the entire pelvic region more sensitive. Pressure on the bladder and urethra during intercourse can trigger sharp pain, burning sensations, or an urgent need to urinate.
Many people report that attempting sex during a UTI transforms what should be pleasurable into an uncomfortable or downright painful experience. This discomfort isn’t just unpleasant—it’s your body signaling that something is wrong.
Can You Pass a UTI to Your Partner?
UTIs aren’t classified as sexually transmitted infections. The bacteria that cause most UTIs—primarily E. coli from the digestive tract—don’t spread from person to person through sexual contact the way STIs do.
That said, sexual activity can still affect your partner’s health. While you won’t directly transmit the UTI, the bacteria present during an infection can potentially be transferred to your partner’s genital area during intercourse.
For female partners, this bacterial transfer can increase their own risk of developing a UTI. The CDC notes that bacteria from the skin or rectum can enter the urethra during sexual activity, which is why sexual intercourse is a well-established risk factor for UTIs in women.
Male partners face lower risk but aren’t completely protected. In some cases, bacteria can cause urethral irritation or, less commonly, lead to infections like urethritis (inflammation of the urethra). According to CDC guidelines on urethritis, while this condition often results from STIs, noninfectious causes and bacterial transfer can also play a role.
How Long Should You Wait After a UTI to Have Sex?
Timing matters when it comes to resuming sexual activity after a urinary tract infection. Most healthcare providers recommend waiting until you’ve completed your full course of antibiotics and symptoms have completely disappeared.
For typical UTIs treated with antibiotics, symptoms often improve within 1-3 days of starting medication. But feeling better doesn’t mean the infection is gone. The CDC emphasizes that antibiotics treat UTIs, but the full course must be completed to ensure all bacteria are eliminated.
A safe timeline looks like this:
- Complete the entire antibiotic prescription (usually 3-7 days)
- Wait until all symptoms have resolved for at least 24-48 hours
- Some providers recommend waiting an additional week after symptoms clear to ensure the infection is fully gone
This conservative approach reduces the risk of recurring infection. Research on recurrent UTIs indicates that incomplete healing can contribute to repeat infections, which affect a significant portion of women who experience UTIs.
Signs Your UTI Has Cleared
Before resuming sexual activity, confirm that these symptoms have completely disappeared:
- Burning or pain during urination
- Frequent urge to urinate
- Cloudy, dark, or strong-smelling urine
- Pelvic pain or pressure
- Blood in urine
If any symptoms persist after completing antibiotics, contact your healthcare provider. Lingering symptoms might indicate that the infection hasn’t fully cleared or that a different treatment approach is needed.
The Connection Between Sex and UTI Risk
Sexual activity is one of the most well-documented risk factors for UTIs, particularly in women. The anatomical proximity of the urethra to the vaginal opening means that intercourse can introduce bacteria into the urinary tract.
According to research published in the Journal of General Internal Medicine, sexual intercourse increases the risk of symptomatic UTIs, with an adjusted hazard ratio of 3.42 (95% CI 1.49–7.80) appearing 2 calendar days after sexual activity in post-menopausal women. While this study focused on older women, the mechanism applies across age groups.
This doesn’t mean sex inevitably causes UTIs. Rather, certain behaviors and biological factors influence risk levels. Women face higher UTI rates than men due to having a shorter urethra, which gives bacteria a shorter distance to travel to reach the bladder.
Why Some People Get UTIs After Sex
Several factors explain the sex-UTI connection. During intercourse, bacteria from the genital area, perineum, or anus can be mechanically pushed toward and into the urethra. Once inside, these bacteria can multiply and cause infection.
Certain sexual practices increase risk more than others. Activities that involve anal contact followed by vaginal contact can transfer intestinal bacteria like E. coli—the culprit behind most UTIs—directly to the urinary tract opening.
Hormonal factors also play a role. Research from the National Institute of Diabetes and Digestive and Kidney Diseases notes that decreased estrogen after menopause can change the vaginal bacterial environment, potentially increasing UTI susceptibility.
| Risk Factor | Impact Level | Prevention Strategy |
|---|---|---|
| Frequent sexual activity | High | Urinate before and after sex |
| New sexual partner | Moderate-High | Maintain hygiene practices |
| Spermicide use | Moderate | Consider alternative contraception |
| Diaphragm use | Moderate | Ensure proper fit or switch methods |
| Inadequate lubrication | Low-Moderate | Use water-based lubricants |
Preventing UTIs Related to Sexual Activity
While you can’t eliminate UTI risk entirely, several evidence-based strategies significantly reduce the likelihood of developing an infection after sex.
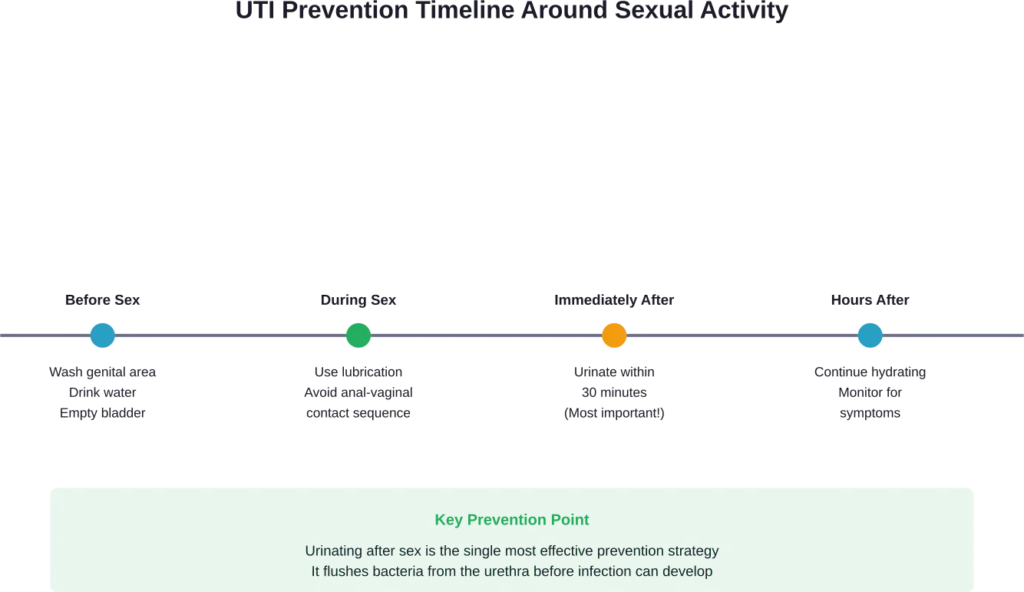
The single most effective preventive measure is urinating shortly after sexual activity. This simple act flushes out bacteria that may have entered the urethra during intercourse, preventing them from traveling to the bladder and multiplying.
Hydration supports this process. Drinking water before and after sex ensures you’ll be able to urinate and helps dilute any bacteria present in the urinary tract. Well-hydrated individuals produce more urine, creating more opportunities to flush out potential pathogens.
Hygiene Practices That Help
Proper hygiene before sex reduces the bacterial load in the genital area. Both partners should wash their hands and genital areas before intimacy. This doesn’t need to be clinical—a quick wash with mild soap and water is sufficient.
The direction of genital cleaning matters too. Always wipe from front to back after using the bathroom to avoid transferring intestinal bacteria toward the urethra. This principle applies during sexual activity as well—avoid contact that moves bacteria from the anal area toward the vaginal opening.
For women prone to recurrent UTIs, some healthcare providers recommend avoiding certain contraceptive methods. According to the American College of Obstetricians and Gynecologists, spermicides and diaphragms have been associated with increased UTI risk. If you experience frequent UTIs, discuss contraceptive alternatives with your provider.
When to Consider Preventive Antibiotics
For people who experience recurrent UTIs—defined as 2 or more infections within 6 months or 3 or more within a year—preventive strategies may include low-dose antibiotics. The cost of treating UTIs in the United States is about 3.5 billion dollars annually.
Some providers prescribe a single dose of antibiotics to be taken after sexual activity for patients with a clear pattern of post-coital UTIs. The American College of Obstetricians and Gynecologists notes that preventive antibiotics can reduce UTI risk by more than 75 percent over time (estimated based on vaginal estrogen data; preventive antibiotics vary by duration and individual factors), though this approach is reserved for specific situations due to antibiotic resistance concerns.
When to See a Healthcare Provider
Not all UTIs require immediate medical attention, but certain symptoms indicate a need for prompt evaluation. If you experience fever, chills, back pain (especially in the kidney area), nausea, or vomiting alongside urinary symptoms, seek medical care quickly.
These warning signs may indicate that the infection has spread to the kidneys—a more serious condition called pyelonephritis that requires aggressive treatment. According to the CDC, untreated UTIs can lead to complications including kidney damage.
You should also contact your healthcare provider if:
- Symptoms don’t improve within 2-3 days of starting antibiotics
- Symptoms return shortly after completing treatment
- You experience 2 or more UTIs within 6 months
- You see blood in your urine
- You’re pregnant and develop UTI symptoms
Pregnancy requires special attention. UTIs during pregnancy carry higher risks of complications and can potentially lead to premature labor or low birth weight. The American College of Obstetricians and Gynecologists recommends that pregnant women with UTI symptoms receive prompt evaluation and treatment.
Understanding the Difference Between UTIs and STIs
Because both UTIs and certain sexually transmitted infections can cause urinary symptoms, distinguishing between them matters for proper treatment. UTIs result from bacteria (usually E. coli) entering the urinary tract, while STIs involve different pathogens transmitted through sexual contact.
Some STIs like chlamydia and gonorrhea can cause symptoms that mimic UTIs, including burning during urination and increased urinary frequency. According to CDC data on STIs, millions of new sexually transmitted infections occur each year in the United States, making them quite common.
The CDC’s guidelines on urethritis note that inflammation of the urethra can result from both infectious and noninfectious conditions. Nongonococcal urethritis (NGU) is caused by C. trachomatis in 15%–40% of cases; however, prevalence varies by age group.
If you have UTI-like symptoms along with unusual discharge, genital sores, or pelvic pain, your provider may test for both UTIs and STIs. This dual testing is particularly important if you have a new sexual partner or multiple partners.
Alternative Intimacy During UTI Recovery
Waiting for a UTI to clear doesn’t mean eliminating all physical intimacy. Many forms of non-penetrative sexual activity carry little to no risk of worsening a UTI or spreading bacteria.
Communication with your partner matters most. Explain that you’re dealing with an infection that makes penetrative sex uncomfortable and potentially harmful to your recovery. Most understanding partners will support whatever timeline you need.
Low-risk alternatives include kissing, massage, manual stimulation that doesn’t involve the urethra or bladder area, and other forms of touch that don’t create pressure or friction on the pelvic region. The key is avoiding activities that could irritate inflamed urinary tissues or introduce bacteria.
This recovery period is temporary. Once the infection clears completely, you can return to your normal sexual routine—ideally with prevention strategies in place to reduce future UTI risk.
Frequently Asked Questions
Yes, sexual activity during an active UTI typically worsens symptoms and can prolong the infection. The friction and pressure involved in intercourse irritate already inflamed urinary tissues, intensify pain and burning, and can push bacteria deeper into the urinary tract. This mechanical action interferes with healing and may reduce antibiotic effectiveness.
Most healthcare providers recommend waiting until you’ve completed the full antibiotic course and symptoms have been gone for at least 24-48 hours. For a typical 3-7 day antibiotic treatment, this means waiting approximately 1-2 weeks total before resuming sexual activity. This conservative timeline ensures the infection is completely cleared and reduces recurrence risk.
UTIs aren’t contagious in the traditional sense—you can’t directly transmit the infection to your partner. However, sexual activity during a UTI can transfer bacteria to your partner’s genital area, potentially increasing their risk of developing their own UTI. Female partners face higher risk due to anatomical factors, though male partners can also experience urethral irritation from bacterial transfer.
Recurrent post-coital UTIs typically result from bacteria being pushed into the urethra during intercourse. Women are particularly susceptible due to the short distance between the urethra and vaginal opening. Contributing factors include inadequate lubrication, certain contraceptive methods (especially spermicides and diaphragms), dehydration, and not urinating after sex. Some people are also genetically more prone to UTIs.
The evidence on cranberry juice for UTI prevention is mixed. While cranberries contain compounds that may prevent bacteria from adhering to urinary tract walls, most studies show only modest benefits at best. Cranberry juice is not a substitute for proven prevention strategies like urinating after sex, staying hydrated with water, and maintaining proper hygiene. If you experience recurrent UTIs, discuss evidence-based prevention options with your healthcare provider rather than relying solely on cranberry products.
Oral sex can potentially introduce bacteria to the urinary tract, particularly if it involves the genital area near the urethra. The mouth naturally contains various bacteria that, when transferred to the urethral opening, could cause infection in susceptible individuals. The risk is generally lower than with penetrative vaginal intercourse, but people prone to UTIs should still practice good hygiene and urinate after oral sexual contact.
A bladder infection (cystitis) is actually a type of UTI. The urinary tract includes the kidneys, ureters, bladder, and urethra. When an infection affects the bladder specifically, it’s called cystitis or a bladder infection. Most UTIs are bladder infections, characterized by frequent urination, burning, and pelvic discomfort. When infection spreads to the kidneys, it becomes pyelonephritis—a more serious condition requiring immediate medical attention.
Making the Right Decision for Your Health
The question of whether to have sex with a UTI ultimately comes down to weighing short-term desires against longer-term health outcomes. The medical consensus is clear: waiting until the infection completely clears produces better results.
Sexual activity during an active UTI creates a trifecta of problems—it hurts, it can worsen and prolong the infection, and it may affect your partner’s health. None of these outcomes are worth the temporary intimacy.
Real talk: UTIs are incredibly common, and most sexually active people will deal with at least one. Having a UTI doesn’t reflect poorly on your hygiene or habits. It’s simply a reality of human anatomy and bacterial biology.
What matters is how you respond. Completing your antibiotic course, allowing adequate healing time, and implementing prevention strategies sets you up for better sexual health long-term. The 1-2 week waiting period might feel frustrating, but it’s a small investment in avoiding recurrent infections and chronic urinary issues.
If you’re experiencing UTI symptoms, contact your healthcare provider for proper diagnosis and treatment. If you notice a pattern of infections related to sexual activity, discuss preventive strategies including timing of urination, contraceptive methods, and in some cases, prophylactic antibiotics.
Your urinary health affects your quality of life, sexual satisfaction, and overall wellbeing. Taking UTIs seriously—and giving your body the time it needs to fully recover—protects all of these important aspects of health.
