Quick Summary: Yes, two women can have a baby together using assisted reproductive technology. The most common method is reciprocal IVF (also called ROPA), where one partner provides the eggs while the other carries the pregnancy. Both partners need donor sperm for fertilization, but this approach allows both women to participate biologically in creating their child.
For lesbian couples wanting to build a family, modern reproductive technology offers multiple pathways to parenthood. The answer is absolutely yes—two women can have a baby together, though it requires assisted reproductive techniques and donor sperm.
What makes today’s options particularly meaningful is that both partners can participate biologically in the pregnancy journey. One woman can provide the genetic material while the other carries and gives birth to the child.
This wasn’t always possible. But advances in fertility treatment have created opportunities for shared motherhood that go far beyond traditional adoption or single-partner conception.
Current Reproductive Options for Lesbian Couples
Same-sex female couples have several established fertility treatment paths available. Each method offers different levels of biological participation for both partners.
The primary options break down into a few distinct categories based on how involved each partner wants to be in the conception and pregnancy process.
Intrauterine Insemination (IUI) with Donor Sperm
IUI represents the most straightforward approach. One partner undergoes insemination with donor sperm during her ovulation window. This method works similarly to natural conception, just with medical assistance for the sperm delivery.
According to research from Stanford School of Medicine analyzing 11,870 IUI cycles, lesbian women using donor sperm achieved pregnancy success rates comparable to heterosexual couples undergoing similar treatments.
The process is less invasive than IVF and typically costs less. However, only one partner participates biologically—the one who carries the pregnancy and provides the egg.
Reciprocal IVF (The ROPA Method)
Here’s where it gets interesting. Reciprocal IVF allows both women to participate in creating their child.
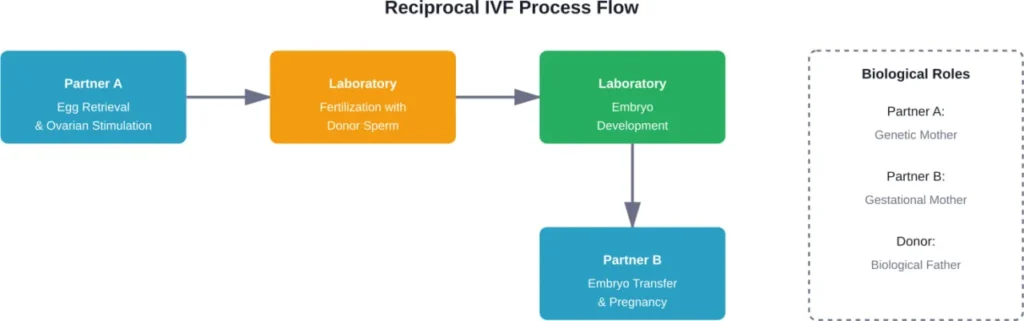
One partner undergoes ovarian stimulation and egg retrieval. Those eggs are then fertilized with donor sperm through in vitro fertilization. The resulting embryos are transferred to the other partner’s uterus for pregnancy.
This method is also called ROPA—Reception of Oocytes from PArtner. It’s become increasingly popular among lesbian couples specifically because it creates a shared biological connection.
One woman is the genetic mother. The other is the gestational mother. Both play essential biological roles.
Traditional IVF (Single Partner)
Some couples choose standard IVF where one partner provides both the eggs and carries the pregnancy. This works identically to IVF for heterosexual couples dealing with male infertility—donor sperm replaces partner sperm.
This option makes sense when one partner has fertility concerns or when the couple has a clear preference about which partner will be pregnant.
Success Rates and Clinical Outcomes
Research shows that sexual orientation doesn’t impact fertility treatment outcomes. According to studies analyzing assisted reproductive technology data, lesbian couples achieve pregnancy rates comparable to heterosexual couples using similar methods.
However, fertility disorders are discovered during medical workup in approximately 40% of lesbian couples seeking treatment, according to research published in medical journals. This matches patterns seen in the broader population.
Research shows that more than half of lesbian couples require IVF instead of IUI, as a fertility disorder is discovered during medical work-up in approximately 40% of couples.
| Method | Both Partners Involved | Relative Cost | Invasiveness |
|---|---|---|---|
| IUI with Donor Sperm | No (one partner only) | Lower | Minimal |
| Reciprocal IVF (ROPA) | Yes (both biologically) | Higher | Moderate to High |
| Traditional IVF | No (one partner only) | Higher | Moderate to High |
| Intravaginal Culture (IVC) | Yes (experimental) | Moderate | Moderate |
Understanding Reciprocal IVF in Detail
The ROPA method has gained significant traction in fertility clinics worldwide. Six out of the eight studies on this technique were conducted in Spain, with one in the United Kingdom and one in the United States.
Real talk: this method creates unique emotional and legal dynamics. Both women can claim biological motherhood, which many couples find deeply meaningful.
The process requires careful coordination. The partner providing eggs undergoes hormone injections to stimulate multiple egg production. After retrieval, those eggs are fertilized in the laboratory with carefully selected donor sperm.
Meanwhile, the partner who will carry the pregnancy receives hormones to prepare her uterine lining for embryo implantation. Timing is everything.
Choosing Roles in Reciprocal IVF
How do couples decide who provides eggs versus who carries the pregnancy? The decision factors vary widely.
Age plays a significant role—egg quality declines with age, so the younger partner often provides eggs while the older partner may prefer to carry the pregnancy. Medical history matters too, as certain conditions affect fertility or pregnancy safety differently.
But plenty of couples base the decision on personal preference. Some women feel strongly about experiencing pregnancy. Others prioritize the genetic connection.
The Donor Sperm Component
All current methods for two women to have a baby together require donor sperm. There’s no way around this biological reality with existing technology.
Most lesbian couples go to a fertility clinic in search of a sperm donor, according to research on reproductive planning in same-sex female couples.
Donor selection involves detailed profiles including physical characteristics, medical history, education, and sometimes even personality assessments. Some sperm banks offer adult photos or childhood pictures.
Anonymous versus known donors represents another choice. Anonymous donors provide sperm through regulated sperm banks. Known donors might be friends or acquaintances, though this route requires careful legal documentation.
Future Possibilities: Creating Eggs from Skin Cells
Now, this is where it gets really interesting. Scientists are exploring whether two women could someday have a biological baby without any donor sperm.
The theoretical approach involves taking regular cells—maybe skin or blood cells—from one partner and using gene-editing to convert them into stem cells. These stem cells could potentially be coaxed into developing into sperm cells.
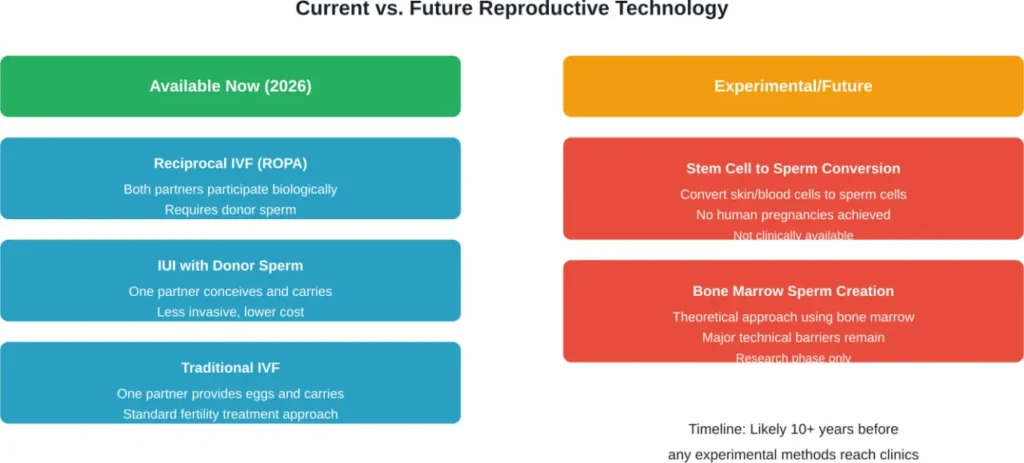
But here’s the thing: this technology remains firmly in the research phase. No human pregnancies have resulted from this approach. The scientific and ethical complexities are substantial.
Creating functional sperm from female cells would require overcoming the fundamental issue that women have two X chromosomes, while sperm needs either an X or Y chromosome. The technical barriers are significant.
So while fascinating from a scientific perspective, this isn’t a practical option for couples wanting to have a baby in 2026.
Legal and Practical Considerations
Beyond the medical procedures, lesbian couples face important legal questions. Parental rights vary significantly by country and even by state within the United States.
In reciprocal IVF, the gestational mother typically has automatic legal parental rights. The genetic mother may need to complete second-parent adoption or establish legal parentage through other means, depending on local laws.
Some jurisdictions have streamlined this process for married same-sex couples. Others still require additional legal steps even when both partners are clearly invested in parenting.
Working with fertility clinics experienced in treating same-sex couples helps navigate these complexities. Many clinics now have specialized programs for LGBTQ families.
Costs and Insurance Coverage
Fertility treatment represents a significant financial investment. IUI with donor sperm typically costs less than IVF-based approaches, but multiple cycles are often necessary.
Reciprocal IVF involves costs for both partners—ovarian stimulation and egg retrieval for one, embryo transfer and pregnancy monitoring for the other. Add in donor sperm costs and multiple treatment cycles if needed.
Insurance coverage varies dramatically. Some plans cover fertility treatment for same-sex couples. Others exclude coverage based on the couple’s ability to conceive without medical assistance, even though donor sperm is obviously required.
Check your specific insurance policy and state regulations, as fertility coverage mandates differ by location.
Frequently Asked Questions
No, not with current technology. While reciprocal IVF allows both women to participate biologically (one provides the egg, the other carries the pregnancy), the baby only receives DNA from the egg provider and the sperm donor. The gestational mother doesn’t contribute genetic material, though she influences fetal development through the pregnancy environment.
Reciprocal IVF often costs more because it involves medical procedures for both partners—egg retrieval for one and embryo transfer for the other. Both partners require monitoring, medications, and clinical care throughout the process. However, pricing varies by clinic and geographic location.
No. Research from Stanford and other institutions shows that sexual orientation doesn’t impact fertility treatment outcomes. Lesbian couples using donor sperm achieve pregnancy rates comparable to heterosexual couples undergoing similar treatments. Success depends on age, egg quality, and general health factors, not sexual orientation.
Absolutely. Couples decide together based on factors like age, fertility status, medical history, and personal preference about pregnancy versus genetic connection. Some couples even switch roles for subsequent children, allowing each partner to experience both aspects of motherhood.
With current medical technology, yes. Scientists are researching methods to create sperm cells from female cells, but this remains experimental with no successful human pregnancies. For couples wanting to have a baby in 2026, donor sperm is necessary for fertilization.
From initial consultation to embryo transfer typically takes 2-4 months, depending on cycle timing and clinic protocols. Both partners undergo medical screening and preparation. The actual egg retrieval and embryo transfer happen within days of each other, but preparation requires coordinating both partners’ cycles.
They’re the same thing. ROPA stands for Reception of Oocytes from PArtner, which is the technical term for reciprocal IVF. Different clinics and countries use different terminology, but the process is identical—one partner provides eggs, the other carries the pregnancy.
Making the Decision
Choosing how to build your family is deeply personal. The medical options available to lesbian couples in 2026 offer meaningful ways for both partners to participate in bringing a child into the world.
Reciprocal IVF creates a unique shared biological connection. One woman contributes genetics, the other contributes gestation and birth. Both are mothers in the fullest biological sense, just through different mechanisms.
Other couples prefer simpler approaches like IUI, especially if one partner feels strongly about being both the genetic and gestational mother.
The right answer depends on your specific situation—your health, your preferences, your finances, and what feels meaningful to you as a couple.
Start by consulting with fertility clinics that have experience working with same-sex female couples. They can assess both partners’ fertility, explain options in detail, and help you understand what to expect medically, financially, and legally.
The technology exists. The success rates are solid. And thousands of lesbian couples have successfully had babies using these methods. Parenthood through fertility treatment is absolutely achievable.
