Quick Summary: If you don’t burp a baby, they will likely be fine. Research shows that burping may be unnecessary, as babies naturally release air through an immature lower esophageal sphincter. While trapped air can occasionally cause temporary discomfort or fussiness, it typically resolves on its own without intervention.
New parents often feel intense pressure to burp their babies after every feeding. The familiar scene plays out countless times daily: a parent gently pats their infant’s back over their shoulder, waiting for that telltale burp.
But what actually happens if you skip this ritual? Will your baby suffer from painful gas? Experience more colic? Develop stomach problems?
The answer might surprise you. Recent research challenges decades of conventional wisdom about burping babies.
The Truth About Burping Babies
Here’s the thing though—burping babies might be one of those parenting practices that continues more from tradition than medical necessity.
According to pediatrician Dr. Cindy Gellner not to worry: the air in babies will find a way out on its own. Babies have natural mechanisms that allow them to release swallowed air without assistance.
The theory behind burping seems logical enough. Babies swallow air during feeding, whether breastfeeding or bottle-feeding. That air needs to come out. Patting their backs helps them expel it. Simple, right?
Not quite. Research reveals a more complex picture.
How Babies Naturally Release Air
Newborns possess an immature lower esophageal sphincter—the muscle between the esophagus and stomach. While this sounds like a problem, it actually serves as a natural venting system.
This sphincter relaxes and opens frequently in young infants. Air escapes naturally without requiring intervention. Babies can burp independently, just like older children and adults.
According to guidance from pediatric health authorities, breastfed infants typically nurse 8 to 12 times in 24 hours. Not all these feeding sessions require deliberate burping attempts.
What Actually Happens When You Skip Burping
So what occurs when you put a baby down without burping them? The outcomes vary depending on the individual infant.
Most Babies Show No Negative Effects
The majority of babies experience no problems whatsoever. They sleep comfortably, digest their milk normally, and wake for their next feeding on schedule.
Research including a study of 71 mother-baby pairs found that burping did not reduce colic rates. The air simply exits through other means—either as a burp that happens spontaneously or by passing through the digestive system.
Some Babies May Experience Temporary Discomfort
A smaller percentage of babies might wake after 20 minutes if they have trapped air that needs release. As pediatricians note, if a baby wakes shortly after being put down and seems fussy, attempting to burp may provide relief.
Signs that trapped air might be causing discomfort include:
- Fussiness or crying shortly after feeding
- Pulling legs up toward the belly
- Arching the back
- Difficulty settling to sleep
- Squirming or appearing uncomfortable
Even when these symptoms appear, they typically resolve quickly as the baby naturally releases the air.
The Surprising Connection to Spit-Up
Real talk: burping might actually increase one problem parents hope to prevent.
A study of 71 mother-baby pairs found that burping babies did not reduce colic rates but did increase regurgitation or spit-up compared to not burping babies.
The explanation makes intuitive sense. Patting a baby with a full stomach on the back can trigger vomiting or spit-up. The mechanical pressure combined with the relaxed esophageal sphincter creates perfect conditions for milk to come back up.
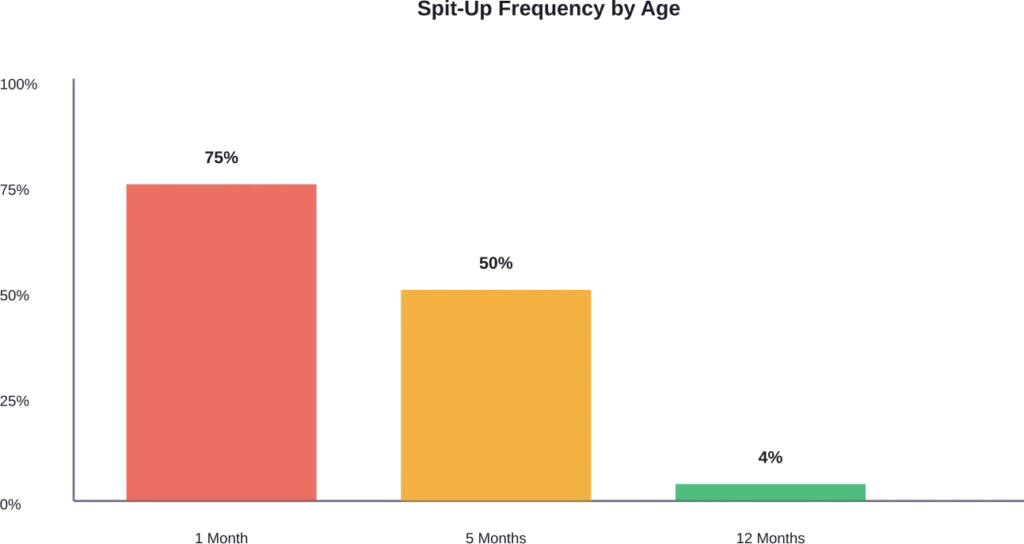
According to research findings, three-quarters of babies one month old spit up after feeding at least once a day. Only half of babies still spit up at five months and almost all (96%) stop by their first birthdays.
Understanding Gas and Colic in Babies
Many parents worry that not burping will cause gas problems or colic. The relationship between these conditions and burping is more nuanced than commonly believed.
What Causes Gas in Newborns
According to Children’s Hospital of Philadelphia pediatricians Julie Kardos, MD, and Naline Lai, MD, all babies are gassy in their first two months of life.
After spending nine months developing in fluid, newborns have zero experience with air until their first breath. Learning to manage air in their digestive systems takes time.
Babies swallow air when they cry, feed, or even just breathe with their mouths open. This air moves through their digestive tract naturally. Some exits as burps, some passes through as gas.
The Colic Connection
Colic is usually defined as crying that lasts more than 3 hours per day for more than 3 days out of the week in an otherwise healthy infant under 3 months of age. Healthcare providers are not certain what causes colic.
Many theories exist, but research hasn’t established that gas in the stomach causes fussiness or reflux. Even if gas contributes to discomfort, there’s no physiological reason babies would need help burping to release it.
Research indicates that approximately 50% of all infants are estimated to suffer from at least one functional gastrointestinal disorder during their first months of life. These conditions occur despite normal feeding and burping practices.
When Burping Might Actually Help
While burping isn’t medically necessary for most babies, certain situations exist where it provides genuine benefit.
Babies Who Gulp Air During Feeding
Some infants swallow more air than others. Bottle-fed babies sometimes gulp air if the bottle nipple flow is too fast. Breastfed babies with a poor latch may take in excess air.
For these babies, attempting to burp during and after feeding may reduce discomfort. The key word is “may”—individual results vary significantly.
Babies With Reflux Issues
Infants diagnosed with gastroesophageal reflux may benefit from more frequent burping. These babies have additional challenges with stomach contents coming back up.
That said, aggressive burping can worsen reflux by putting pressure on a full stomach. Gentle techniques work better than vigorous patting.
When Baby Shows Clear Discomfort
If a baby demonstrates obvious signs of discomfort—arching, crying, pulling legs up—attempting to help them burp makes sense. The baby’s cues provide the best guidance.
Try burping for 5-10 minutes maximum. If no burp emerges and the baby seems comfortable, stop trying. Continuing beyond this point typically stresses both parent and child without additional benefit.
Different Approaches to Burping
Parents who choose to burp their babies have several position options. No single method works best for all infants.
| Position | How It Works | Best For |
|---|---|---|
| Over the shoulder | Baby’s chin rests on shoulder while parent pats or rubs back | Most babies, traditional method |
| Sitting upright | Baby sits on lap, parent supports chest and chin while patting back | Babies with reflux, reduces pressure on stomach |
| Face-down on lap | Baby lies across parent’s lap, parent rubs or pats back | Older infants with good head control |
| Walking and swaying | Hold baby upright against chest while walking | Fussy babies who need movement |
The motion matters less than giving the baby time in an upright position for air to naturally rise.
What About Sleeping Babies?
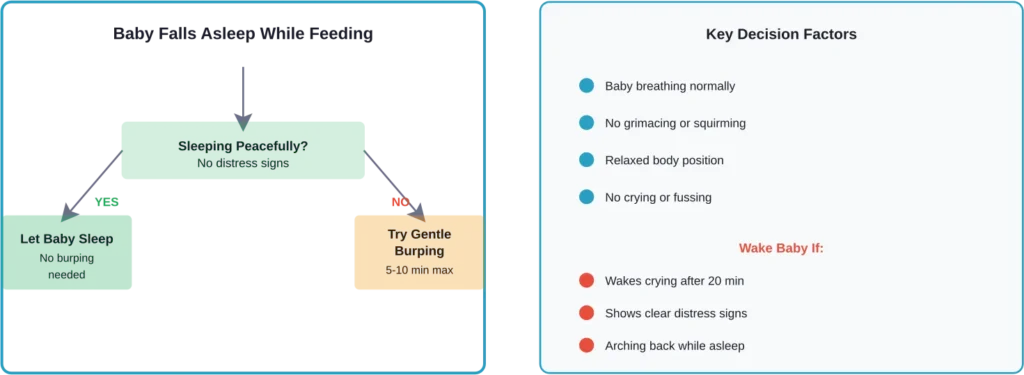
One common dilemma: the baby falls asleep during feeding. Should parents wake them to burp?
Generally speaking, if a baby falls asleep comfortably after feeding, there’s no need to wake them for burping. Sleep is valuable for infant development, and interrupting it to force a burp creates more problems than it solves.
If the baby wakes 20 minutes later crying and uncomfortable, then attempting to burp makes sense. But many babies sleep soundly through their sleep cycle without any intervention.
The decision ultimately depends on knowing the individual baby’s patterns and needs.
Cultural and Historical Perspectives
Burping babies is primarily a Western parenting practice. Many cultures around the world don’t emphasize burping, yet babies in those cultures develop normally without increased digestive problems.
The practice gained popularity in Western countries during the mid-20th century as infant feeding became more medicalized. Formula feeding increased, and with it came various feeding rituals—including mandatory burping.
Now, as research catches up with practice, the medical community increasingly recognizes that burping falls into the category of “probably harmless but possibly unnecessary” interventions.
Making the Decision for Your Baby
So should parents burp their babies or not? The honest answer: it depends on the individual situation.
If burping feels helpful and the baby seems more comfortable afterward, continue the practice. If attempting to burp creates stress for parent or baby without obvious benefit, it’s perfectly fine to stop.
| Consider Burping If… | Skip Burping If… |
|---|---|
| Baby shows discomfort after feeds | Baby falls asleep peacefully |
| Baby gulps air during feeding | Baby seems comfortable without it |
| Baby has diagnosed reflux | Burping attempts cause distress |
| Baby fusses until burped | Baby never burps despite trying |
| It helps parents feel confident | It creates parental anxiety |
Trust the baby’s cues. Infants communicate their needs through behavior. A comfortable baby who feeds well, sleeps adequately, and has normal bowel movements doesn’t need intervention—even if they never burp audibly.
What Medical Professionals Say
The pediatric community has evolved its stance on burping over recent years. While older guidelines emphasized routine burping, newer perspectives acknowledge the lack of evidence supporting its necessity.
As one pediatrician noted, there’s no physiological reason babies would need help burping. The immature lower esophageal sphincter naturally allows air to escape. Babies are protected from gas buildup by this normal developmental feature.
Medical professionals now generally advise parents to do what works for their individual baby rather than following rigid rules about burping after every feeding.
Frequently Asked Questions
No, babies will not choke from not being burped. The concern about choking relates to spit-up or reflux, but research actually shows burping can increase spit-up frequency. Babies positioned on their backs to sleep are safe even if they spit up, as their natural reflexes protect their airways.
Try burping for 5-10 minutes maximum. If no burp emerges and the baby appears comfortable, stop trying. Continuing beyond this timeframe typically provides no additional benefit and may stress both parent and baby unnecessarily.
Many babies never produce audible burps, and that’s completely normal. The air they swallow exits their digestive system through other means. If the baby seems comfortable, feeds well, and has normal bowel movements, the absence of burps indicates nothing wrong.
Research has not established a connection between skipping burping and colic. A study of 71 mother-baby pairs found that burping did not reduce colic rates. Colic has multiple potential causes, and gas buildup from not burping is not considered a primary factor.
Generally, no. If a baby falls asleep comfortably during or after feeding, let them sleep. Waking a peacefully sleeping baby to force a burp disrupts valuable rest. If the baby wakes 20 minutes later showing discomfort, then attempting to burp may help.
Breastfed babies often swallow less air than bottle-fed babies because they control the flow of milk better. However, individual variation matters more than feeding method. Some breastfed babies gulp air, while some bottle-fed babies don’t. Watch the individual baby’s cues rather than following blanket rules based on feeding type.
Most parents naturally phase out deliberate burping attempts between 4-6 months as babies develop better control over their digestive systems. By this age, infants can burp independently, change positions on their own, and communicate discomfort more clearly. Stop whenever it no longer seems necessary for the individual baby’s comfort.
The Bottom Line on Burping Babies
What happens if you don’t burp a baby? In most cases, absolutely nothing negative.
Babies possess natural mechanisms for releasing swallowed air. Research shows that burping doesn’t reduce colic and may actually increase spit-up. The practice continues largely from tradition rather than medical necessity.
That said, some babies do seem more comfortable with burping, particularly those who swallow excessive air during feeding. The key is responding to individual baby’s needs rather than following rigid rules.
Trust the baby. Watch for signs of discomfort. Try gentle burping if it seems helpful. But don’t stress if burping doesn’t happen or if the baby peacefully falls asleep without it.
Parenting involves enough genuine challenges without adding unnecessary worry about optional practices. If skipping burping works for your family, the evidence suggests your baby will be just fine.
