Quick Summary: An untreated yeast infection rarely clears on its own and typically worsens over days to weeks, causing severe itching, inflammation, skin cracking, and potential secondary infections. According to the CDC, leaving candidiasis untreated can lead to invasive complications in vulnerable populations, though this is rare in healthy individuals. Most vaginal yeast infections require antifungal treatment to resolve completely, and delaying care risks misdiagnosing more serious conditions like bacterial vaginosis or STIs.
Vaginal itching, burning, unusual discharge—these symptoms make a yeast infection hard to ignore. But life gets busy, and the temptation to wait it out is real. Maybe it’ll just disappear on its own, right?
Not exactly. While some mild cases might improve without intervention, most untreated yeast infections don’t simply vanish. They escalate. And sometimes, what feels like a straightforward yeast infection turns out to be something entirely different that needs immediate attention.
Here’s what actually happens when candidiasis goes untreated, backed by medical research and authoritative health data.
Why Yeast Infections Happen
Candidiasis occurs when Candida, a yeast naturally present in the body, grows out of control. According to the CDC, many types of Candida live on skin and in various body parts without causing problems. Symptoms only emerge when overgrowth happens.
Several factors trigger this imbalance. The CDC identifies weakened immune systems and antibiotic use as primary risk factors. Pregnancy and hormonal changes significantly increase vaginal candidiasis risk. Antibiotics disrupt the vaginal microbiome, eliminating beneficial bacteria that normally keep Candida in check.
The result? Itching, burning, redness, swelling, and thick white discharge that resembles cottage cheese. These symptoms range from mildly annoying to genuinely debilitating.
What Happens When You Skip Treatment
Ignoring a yeast infection sets off a predictable progression. Without intervention, the infection doesn’t maintain a steady state—it intensifies.
Symptoms Worsen Progressively
The initial mild itching transforms into severe, constant discomfort. Inflammation spreads throughout the vaginal area, extending to the vulva and surrounding skin. Burning sensations intensify, making urination painful.
Discharge increases in volume and thickness. The affected tissue becomes increasingly inflamed and discolored. What started as minor irritation becomes impossible to ignore during daily activities.
Skin Damage and Secondary Infections
Persistent scratching—an almost irresistible response to severe itching—damages the skin barrier. Cracked, broken skin creates entry points for bacterial infections.
This secondary complication transforms a fungal problem into a mixed infection requiring multiple treatment approaches. The damaged tissue heals slowly, prolonging discomfort even after treatment begins.
Extended Duration of Discomfort
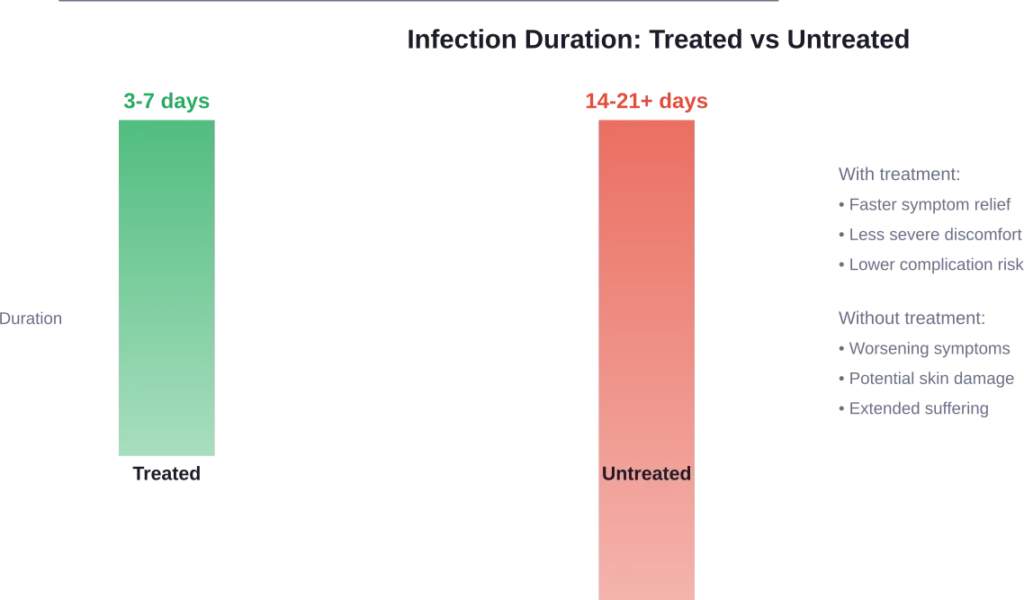
How long does an untreated yeast infection last? The timeline varies, but moderate to severe symptoms can persist for two to three weeks or longer without treatment. Some mild cases might improve within days, but this is the exception rather than the rule.
Compare this to treated infections, which typically clear within three to seven days with proper antifungal therapy. The math is straightforward: treatment shortens suffering dramatically.
Serious Complications Are Rare But Real
For most healthy individuals, an untreated yeast infection remains localized to the vaginal area. It’s miserable, but not medically dangerous. However, certain populations face genuinely serious risks.
Invasive Candidiasis in Vulnerable Groups
According to CDC data, invasive candidiasis occurs when Candida enters the bloodstream and spreads to organs or bones. This severe complication primarily affects hospitalized patients, those with severely weakened immune systems, and people with HIV/AIDS.
The NIH’s StatPearls database notes that invasive candidiasis is the most common fungal infection worldwide. While vaginal yeast infections rarely progress to this stage in healthy people, the risk increases dramatically for immunocompromised individuals.
According to CDC guidance, invasive candidiasis carries high mortality rates in hospitalized and immunocompromised populations. While invasive candidiasis is serious, it primarily affects hospitalized patients, those with severe immunosuppression, and people with HIV/AIDS rather than healthy individuals with vaginal yeast infections.
Pregnancy Complications
The CDC emphasizes that pregnancy significantly increases yeast infection risk due to hormonal changes. Pregnant individuals can transmit the infection to newborns during labor and delivery.
Transmission of infections from mother to baby during labor occurs in 1% to 2% when the mother does not receive treatment, as noted in research on maternal infections. Treating maternal yeast infections before delivery protects both mother and baby.
Recurrent Infections
Leaving a yeast infection untreated often leads to recurrence. The initial infection might eventually subside on its own, but without addressing the underlying cause or completely eliminating the overgrowth, Candida returns.
Some individuals develop chronic or recurrent vulvovaginal candidiasis, defined as four or more infections within 12 months. This pattern significantly impacts quality of life and becomes progressively harder to treat.
The Misdiagnosis Problem
Here’s the thing that makes skipping treatment particularly risky: what feels like a yeast infection might be something else entirely.
One study found that 69% of those who thought they had a yeast infection had something else, as noted in competitor content from Evvy.
Conditions That Mimic Yeast Infections
Several infections produce similar symptoms to vaginal candidiasis:
- Bacterial vaginosis: The most common vaginal infection, caused by bacterial imbalance rather than yeast overgrowth
- Trichomoniasis: A sexually transmitted infection requiring different treatment
- Chlamydia: Often asymptomatic but can cause discharge and discomfort
- Atrophic vaginitis: Inflammation from hormonal changes, particularly during menopause
According to the American College of Obstetricians and Gynecologists (ACOG), proper diagnosis requires healthcare provider evaluation. Symptoms alone don’t distinguish between these conditions reliably.
The treatment for bacterial vaginosis is antibiotics, not antifungals. Trichomoniasis requires specific antimicrobial therapy. Using the wrong treatment delays proper care and allows the actual condition to worsen.
| Condition | Primary Symptom | Discharge Characteristics | Treatment Type |
|---|---|---|---|
| Yeast Infection | Intense itching | Thick, white, odorless | Antifungal |
| Bacterial Vaginosis | Fishy odor | Thin, grayish, strong odor | Antibiotics |
| Trichomoniasis | Greenish discharge | Frothy, yellow-green | Antiprotozoal |
| Atrophic Vaginitis | Vaginal dryness | Watery, minimal | Hormone therapy |
When Yeast Infections Require Medical Attention
Certain situations demand professional evaluation rather than home treatment attempts.
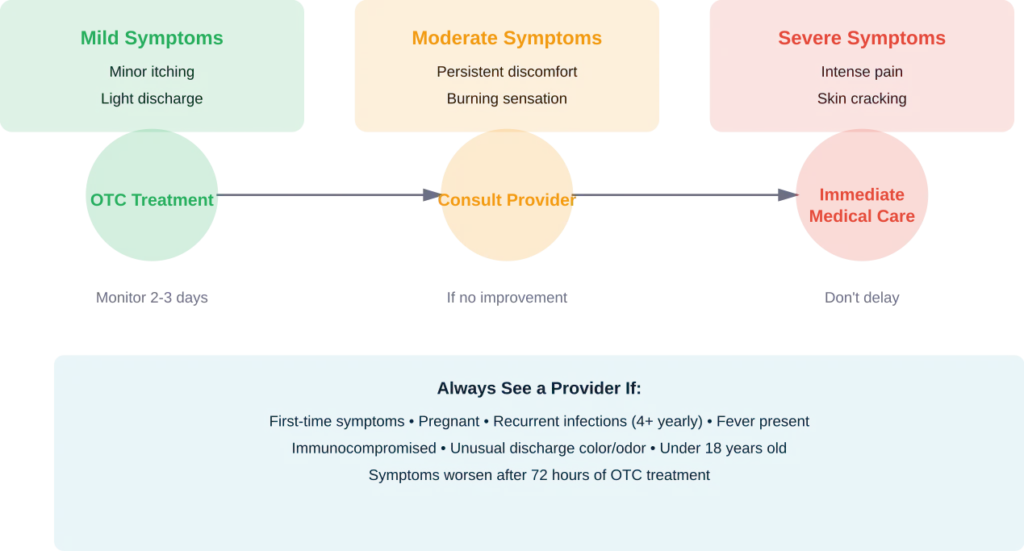
Seek medical care if:
- This is the first time experiencing these symptoms
- Symptoms don’t improve after 72 hours of over-the-counter treatment
- Symptoms are severe (extensive redness, swelling, or cracking)
- Infections recur four or more times yearly
- Pregnancy is current or possible
- Fever develops alongside vaginal symptoms
- Unusual discharge appears (greenish, grayish, or foul-smelling)
- Immune system is compromised due to diabetes, HIV, chemotherapy, or immunosuppressive medications
Healthcare providers can perform accurate diagnostic testing, including microscopic examination and cultures. This confirms whether Candida is actually the culprit and identifies the specific species, which matters for treatment selection.
Treatment Options Work Quickly
The good news? Yeast infections respond well to treatment when properly diagnosed.
Over-the-counter antifungal medications come as creams, ointments, and suppositories. Common active ingredients include miconazole, clotrimazole, and tioconazole. Treatment courses range from one to seven days depending on the product strength.
Prescription options include oral fluconazole, a single-dose pill that treats the infection systemically. For recurrent infections, healthcare providers may prescribe extended treatment protocols or maintenance therapy.
Symptoms should improve within 72 hours of starting treatment, according to ACOG guidance. Most treated infections clear within a few days to one week with proper antifungal therapy.
The contrast with untreated infections is stark. Why endure two to three weeks of escalating misery when effective treatment brings relief within days?
Prevention Strategies
While not all yeast infections are preventable, certain habits reduce risk:
- Wear breathable cotton underwear and avoid tight-fitting synthetic fabrics
- Change out of wet swimsuits and workout clothes promptly
- Avoid douches, scented feminine products, and harsh soaps in the vaginal area
- Maintain blood sugar control if diabetic
- Consider probiotic supplements during antibiotic courses
- Limit unnecessary antibiotic use
These measures help maintain the vaginal microbiome balance that keeps Candida in check.
Frequently Asked Questions
Some very mild yeast infections might resolve without intervention, but this is uncommon. Most untreated infections worsen over time, with symptoms intensifying and duration extending to two to three weeks or longer. Treatment typically resolves symptoms within three to seven days, making it the more reliable approach.
Worsening signs include increasing intensity of itching and burning, spreading redness and swelling beyond the initial area, skin cracking or fissures, pain during urination or intercourse, and increasing discharge volume. If symptoms intensify rather than improve after 48-72 hours, medical evaluation is necessary.
In healthy individuals, untreated vaginal yeast infections rarely cause permanent damage, though they can lead to skin breakdown and secondary bacterial infections. However, in immunocompromised individuals, untreated infections can potentially progress to invasive candidiasis, which carries serious health risks including organ damage.
Chronic yeast infections lasting months indicate either incomplete treatment, misdiagnosis of a different condition, or an underlying health issue like diabetes or immune system dysfunction. Long-term infections cause persistent inflammation, skin changes, and significantly impaired quality of life. Medical evaluation is essential to identify the root cause and establish effective treatment.
Over-the-counter antifungal treatments are safe and effective for straightforward yeast infections in healthy adults who have had confirmed yeast infections previously. However, first-time symptoms, pregnancy, recurrent infections, or symptoms that don’t improve within 72 hours of OTC treatment all require professional medical evaluation.
In healthy individuals with normal immune function, vaginal yeast infections typically remain localized. However, Candida can affect other areas like the mouth (oral thrush), skin folds, or nails. According to the CDC, invasive candidiasis where infection spreads to the bloodstream and organs primarily occurs in hospitalized patients or severely immunocompromised individuals.
Recurrent yeast infections stem from various causes: incomplete treatment of the initial infection, antibiotic use disrupting vaginal flora, uncontrolled diabetes, hormonal changes, immune system issues, or resistant Candida strains. ACOG recommends medical evaluation for anyone experiencing four or more infections within 12 months to identify underlying causes and establish appropriate treatment strategies.
The Bottom Line
Skipping treatment for a yeast infection is a gamble that rarely pays off. While the infection might not pose life-threatening danger for most healthy individuals, the prolonged discomfort, risk of complications, and possibility of misdiagnosis make treatment the sensible choice.
Effective therapies exist that work quickly and reliably. The difference between days of relief and weeks of suffering comes down to one decision: seeking appropriate treatment.
If symptoms suggest a yeast infection—especially if this is the first occurrence or symptoms are severe—professional evaluation provides accurate diagnosis and effective treatment. The minor inconvenience of a healthcare visit beats weeks of escalating misery every time.
Take vaginal health seriously. The body deserves proper care, and effective solutions are readily available.
