Quick Summary: Drinking blood carries severe health risks including bloodborne infections (HIV, hepatitis B and C), iron toxicity, and digestive complications. Medical professionals strongly advise against consuming human or animal blood due to the high risk of contracting dangerous pathogens and potential organ damage.
The concept of drinking blood has fascinated humans for centuries, appearing throughout folklore and modern vampire fiction. But what actually happens when someone consumes blood in real life? The answer is far less romantic than pop culture suggests.
Medical professionals universally discourage this practice. Despite its presence in certain subcultures and cultural traditions, blood consumption poses serious health threats that far outweigh any perceived benefits.
The Immediate Biological Response
When blood enters the digestive system, the body treats it like any other protein-rich substance. However, blood is fundamentally different from typical foods.
The stomach begins breaking down blood proteins through gastric acids. This process releases iron in significant quantities—far more than the body typically processes from a standard meal. Blood contains concentrated levels of proteins and pathogens that can overwhelm normal digestive processes.
Here’s the thing though—the human digestive system isn’t designed to handle blood as a primary food source. While some cultures consume small amounts of cooked animal blood in traditional dishes, raw consumption presents entirely different risks.
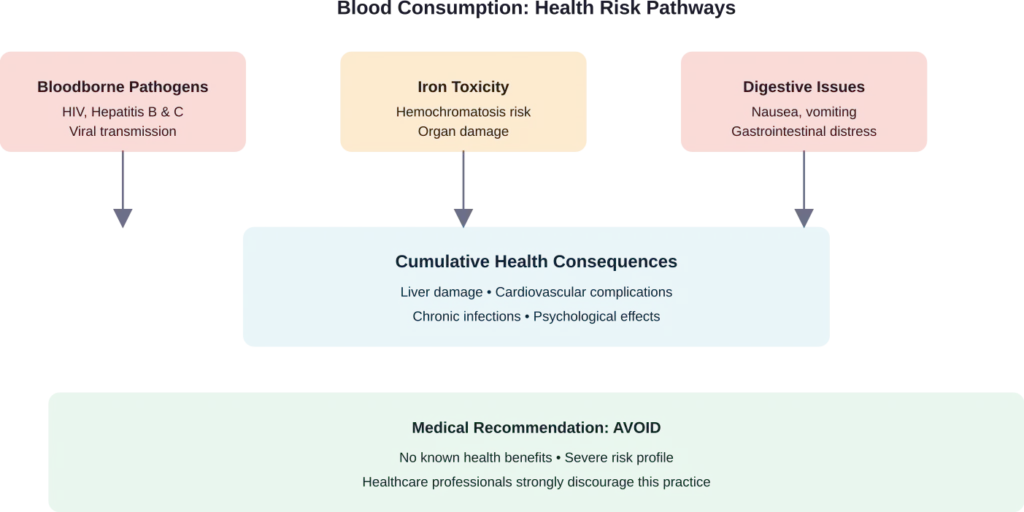
Bloodborne Disease Transmission
The most serious risk comes from bloodborne pathogens. The primary bloodborne pathogens of concern include human immunodeficiency virus (HIV), hepatitis B virus (HBV), and hepatitis C virus (HCV). According to the CDC, healthcare workers face exposure risks from these pathogens.
These same risks apply—often magnified—when someone intentionally consumes blood. Viral particles present in infected blood remain active and infectious when ingested. Even small quantities can transmit disease.
The CDC emphasizes that knowing how to prevent exposure to bloodborne diseases is vital for healthcare workers. That prevention advice? Avoid direct blood contact. This guidance becomes even more critical when discussing deliberate consumption.
Specific Disease Risks
HIV transmission through blood is well-documented. While transmission requires specific conditions, consuming infected blood creates multiple exposure points through the mouth, throat, and digestive tract. Any small cut or abrasion becomes a potential entry point.
Hepatitis B and C pose even greater transmission risks. These viruses are more resilient outside the body and more infectious per viral particle than HIV. Hepatitis infections can lead to chronic liver disease, cirrhosis, and liver cancer.
Iron Overload and Hemochromatosis
Blood contains extraordinarily high iron concentrations. A single cup of blood delivers approximately 120mg of iron—more than six times the recommended daily intake for adults.
Regular blood consumption can trigger iron toxicity, clinically known as hemochromatosis. This condition causes iron to accumulate in organs, particularly the liver, heart, and pancreas. Over time, this buildup damages tissue and impairs organ function.
Symptoms of iron overload include:
- Chronic fatigue and weakness
- Joint pain and stiffness
- Abdominal pain
- Heart arrhythmias
- Skin discoloration (bronze or gray tinge)
- Liver enlargement and dysfunction
Real talk: the body has limited mechanisms to eliminate excess iron. Once absorbed, iron stays in the system. Unlike water-soluble vitamins that flush out through urine, iron accumulates. This makes repeated blood consumption particularly dangerous.
| Health Risk | Onset Time | Severity | Reversibility |
|---|---|---|---|
| Bloodborne infections (HIV, Hepatitis) | Days to weeks | Critical | Manageable with treatment, not curable |
| Iron toxicity | Weeks to months | Severe | Partially reversible with chelation |
| Gastrointestinal distress | Hours | Moderate | Fully reversible |
| Organ damage (liver, heart) | Months to years | Critical | Often permanent |
Digestive System Complications
The digestive tract rebels against blood consumption. Nausea and vomiting frequently occur as the body attempts to expel the foreign substance. This isn’t just discomfort—it’s a protective response.
Blood’s high protein and iron content can irritate the stomach lining. This irritation may lead to gastritis or ulcer formation with repeated exposure. The digestive system simply wasn’t designed to process blood as nutrition.
But wait. What about cultures that consume blood in traditional dishes? The key difference: cooking. Heat treatment kills most pathogens and alters blood proteins, making them safer to digest. Raw blood consumption carries exponentially higher risks.
Psychological and Behavioral Aspects
Clinical literature documents rare cases of blood-drinking behaviors, often classified under autovampirism (drinking one’s own blood) or clinical vampirism (drinking others’ blood). These behaviors typically emerge from psychological conditions requiring professional treatment.
Research published in medical case studies describes these behaviors as psychiatric concerns rather than lifestyle choices. They often develop following traumatic incidents and require comprehensive mental health intervention.
The Vampire Subculture Reality
Some individuals identify with vampire subcultures and report consuming small amounts of blood. Medical professionals emphasize that this practice offers no health benefits and carries the risks outlined above.
No scientific evidence supports claims of enhanced energy, vitality, or other benefits from blood consumption. Any perceived effects likely stem from placebo responses or psychological factors rather than nutritional value.
Legal and Ethical Considerations
Laws regarding blood consumption vary globally. Many jurisdictions have no specific prohibitions, as lawmakers never anticipated needing such regulations. However, related laws around assault, bodily harm, and disease transmission may apply.
Consent doesn’t eliminate health risks. Even with willing donors, disease transmission remains a serious concern. Blood banks and medical facilities follow strict screening protocols precisely because blood carries such significant infection risks.
What Medical Professionals Recommend
The medical consensus is clear and unanimous: don’t drink blood. No legitimate medical organization or healthcare professional recommends this practice for any reason.
For individuals experiencing urges to consume blood, mental health support is the appropriate intervention. These impulses may indicate underlying psychological conditions that respond well to therapy and treatment.
Anyone who has consumed blood and experiences symptoms—fever, fatigue, jaundice, nausea, or other concerning signs—should seek immediate medical attention. Early intervention significantly improves outcomes for bloodborne infections.
Frequently Asked Questions
Yes, animal blood carries many of the same risks as human blood, including bacterial contamination, parasites, and iron toxicity. While some cultures consume cooked animal blood safely, raw consumption poses serious health risks including foodborne illnesses and digestive complications.
No. No legitimate medical condition requires blood consumption. Patients needing blood receive it through controlled transfusions directly into the bloodstream, where it serves its intended function. Drinking blood provides no medical benefit and can cause harm.
Small amounts of your own blood from minor bleeding (nosebleeds, dental work) typically cause no serious harm beyond possible nausea or stomach upset. However, swallowing large quantities may cause vomiting or diarrhea as the digestive system reacts to the iron and protein overload.
Absolutely. According to the CDC, bloodborne pathogens including HIV, hepatitis B, and hepatitis C can be transmitted through blood consumption, especially if there are any cuts, sores, or abrasions in the mouth, throat, or digestive tract that allow viral entry into the bloodstream.
Human blood contains approximately 0.5 grams of iron per liter. Consuming just one cup (240ml) of blood delivers roughly 120mg of iron—more than six times the recommended daily intake for adults. This excessive amount can quickly lead to iron toxicity with repeated consumption.
Some traditional cultures consume animal blood as part of their diet, but safety comes from preparation methods—primarily cooking or fermenting the blood, which kills pathogens. These practices differ significantly from consuming raw human or animal blood, which carries severe health risks.
Monitor for symptoms including fever, nausea, fatigue, or jaundice, and seek medical attention if any appear. Be honest with healthcare providers about the exposure—they need complete information to assess risks for bloodborne infections and provide appropriate testing or preventive treatment if necessary.
The Bottom Line
Despite its portrayal in fiction and its presence in certain subcultures, drinking blood is medically dangerous. The risks include life-threatening infections, iron toxicity, organ damage, and serious digestive complications.
No health benefits justify these dangers. Medical professionals universally advise against this practice, regardless of the source or circumstances.
If you’re experiencing urges to consume blood or have engaged in this behavior, reach out to a mental health professional. Treatment options exist that address underlying causes while protecting your physical health. Your wellbeing matters more than any fictional narrative or subcultural identity.
