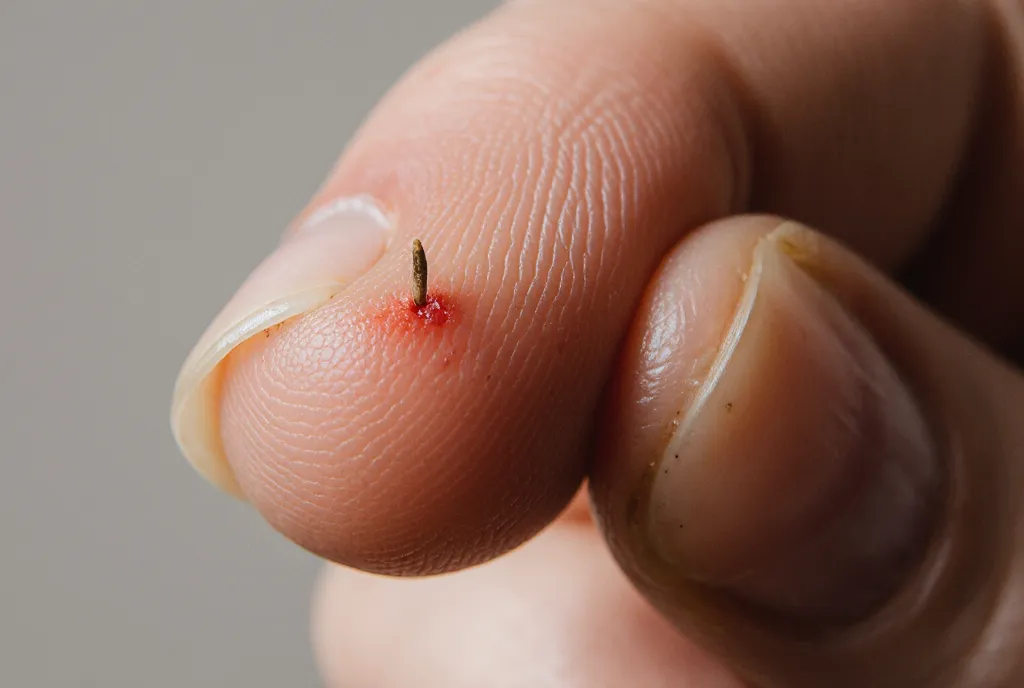
Quick Summary: If you leave a splinter in your skin, your body may naturally push it out or encapsulate it, but there’s also a significant risk of infection, particularly with wooden or plant-based splinters. While tiny surface splinters often work themselves out, deeper splinters can introduce bacteria like Staphylococcus aureus, potentially causing cellulitis, abscesses, or even serious complications like osteomyelitis if left untreated.
Getting a splinter is one of those universal experiences that’s easy to ignore. Maybe it’s a tiny wood fragment from a deck railing, a plant thorn from gardening, or a small glass sliver. The temptation to leave it alone and hope it disappears is strong.
But what actually happens if you don’t remove a splinter?
The answer depends on several factors: what the splinter is made of, where it’s located, how deep it penetrated, and your body’s response. Sometimes your immune system handles it just fine. Other times? Things can get complicated fast.
Can Splinters Work Their Own Way Out?
Here’s the thing—sometimes they can. Your skin constantly regenerates, with new cells forming beneath the surface and pushing older cells outward. For very shallow splinters sitting in the top layer of skin, this natural turnover process can gradually push the foreign object toward the surface.
Many superficial splinters can be eventually expelled by the body’s natural healing processes through skin cell turnover. But this doesn’t work for all splinters.
Deeper objects that penetrate beyond the epidermis into the dermis or subcutaneous tissue won’t easily surface. These require active removal or can become permanently embedded.
Your Body’s Defense Response
When a foreign object breaches your skin, your immune system immediately kicks into action. The body recognizes the splinter as an invader and triggers an inflammatory response.
White blood cells rush to the area, attempting to isolate and eliminate the threat. You’ll notice this as redness, swelling, warmth, and tenderness around the entry site.
In ideal circumstances, this inflammatory process creates enough pressure to push the splinter outward while simultaneously breaking it down. But this defense mechanism isn’t foolproof—and it comes with risks.
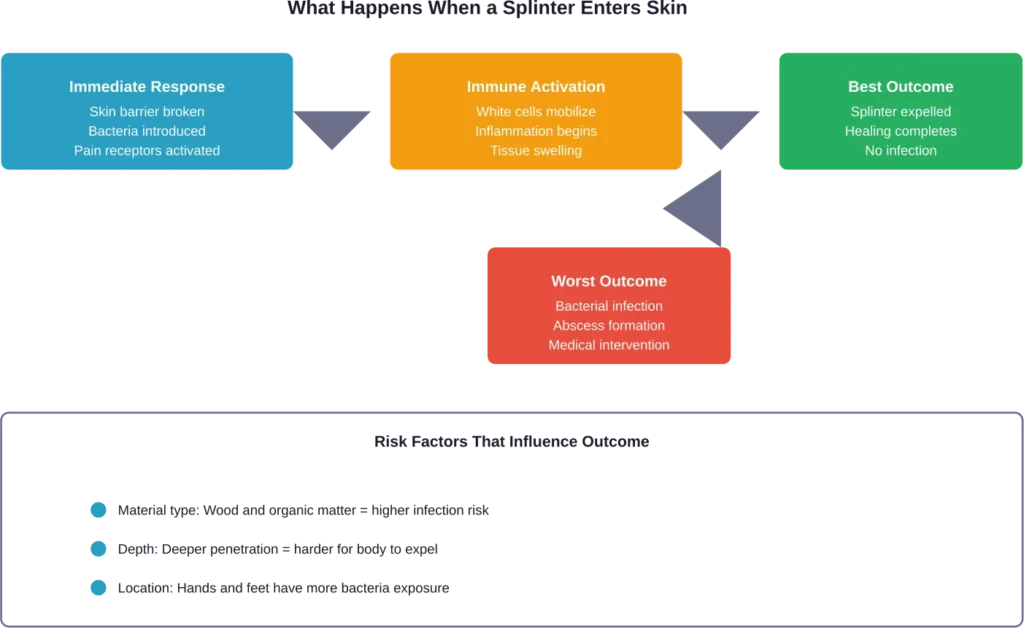
The Infection Risk: Not All Splinters Are Equal
This is where material matters enormously. Not all splinters pose the same infection risk.
Splinters from plants are more likely to carry bacteria like Staphylococcus aureus—commonly known as golden staph, according to medical research and dermatological sources. Wooden splinters can introduce bacteria deep into tissue, where warm, oxygen-poor conditions allow infections to flourish.
Medical case reports have documented retained wooden splinters that migrated within digital flexor tendon sheaths, requiring surgical intervention.
Glass and metal splinters, while still problematic, are generally inert and don’t harbor bacteria the same way organic materials do. However, they can still cause chronic inflammation and pain if left embedded.
| Splinter Material | Infection Risk | Body’s Ability to Expel | Visibility on X-ray |
|---|---|---|---|
| Wood | High | Poor | No |
| Plant thorns | Very High | Moderate | No |
| Glass | Low to Moderate | Poor | Yes |
| Metal | Low | Poor | Yes |
| Plastic | Low to Moderate | Poor | Sometimes |
Warning Signs of Infection
So you’ve decided to leave that splinter alone. What should you watch for?
Signs that a splinter has become infected include:
- Red or hardened skin around the entry site
- White or yellow discharge
- Increasing pain rather than gradual improvement
- Warmth radiating from the area
- Red streaks extending from the wound
- Swelling that spreads beyond the immediate area
That red streak deserves special attention. It indicates inflammation in the lymph vessels—a condition called lymphangitis—and typically appears around 24 hours after infection sets in. This requires immediate medical attention.
Serious Complications: When Splinters Turn Dangerous
While most splinter situations resolve without drama, retained foreign bodies can lead to serious complications.
Medical case reports have documented osteomyelitis (bone infection) caused by neglected wooden splinters in pediatric patients. The infection required aggressive treatment including foreign body removal, bone curettage, and antibiotics.
Other documented complications include:
- Abscess formation requiring surgical drainage
- Cellulitis spreading to surrounding tissue
- Tenosynovitis (tendon sheath infection)
- Foreign body granuloma (inflammatory nodule)
- Chronic pain and neurovascular impairment
Foreign bodies may remain undetected despite wound examination. Studies have found that foreign bodies can be missed on initial evaluation in a significant percentage of cases.
When to Remove a Splinter Yourself
The American Academy of Family Physicians notes that most superficial splinters can be safely removed at home if certain conditions are met.
Good candidates for home removal:
- The splinter is visible and accessible
- It’s located in the top layer of skin
- The entry site shows no signs of infection
- You have proper tools (clean tweezers, good lighting)
- The area can be properly cleaned before and after
But here’s the reality: if you’ve tried unsuccessfully for 10 to 15 minutes, it’s time to stop and seek professional help. Prolonged digging increases tissue damage and infection risk.
When to See a Doctor
Cleveland Clinic experts suggest leaving splinter removal to medical professionals if:
- The splinter has entered near the eye or under a fingernail
- You notice signs of infection
- The splinter entered the skin vertically and is deeply embedded
- It’s in a sensitive area like the foot or hand where nerves and tendons are vulnerable
- You haven’t had a tetanus shot within 10 years
Medical professionals have tools and techniques unavailable to home practitioners. Ultrasound imaging, for instance, can locate radiolucent foreign bodies like wood that don’t show up on X-rays.
Ultrasound evaluation before surgery for wooden foreign body removal has been associated with efficient surgical outcomes, with many procedures completed rapidly with minimal complications.

The Bottom Line on Leaving Splinters In
Real talk: leaving a splinter in your skin is a gamble. Sometimes your body wins and pushes it out naturally. Other times, you’re looking at infection, chronic inflammation, or worse.
The material matters enormously. That tiny wooden splinter carries bacteria that a metal fragment doesn’t. Location matters too—hands and feet have higher exposure to additional contaminants.
Some individuals report leaving small splinters alone with no apparent negative consequences. But medical literature documents enough serious complications that dismissing the risk entirely isn’t wise.
If a splinter is easily accessible and you catch it early, removal is straightforward and eliminates all risk. But if you’re going to dig around blindly causing more tissue damage than the original injury, that’s not helping anyone.
The smart approach? Assess each situation individually. Tiny surface splinters that cause minimal discomfort might resolve on their own. Deeper penetrating injuries, especially from organic materials, deserve prompt attention—either from you with proper technique or from a medical professional.
And watch for those warning signs. Your body is usually pretty good at telling you when something’s wrong.
Frequently Asked Questions
For very shallow splinters in the top layer of skin, the natural skin cell turnover process can push them out in 1-2 weeks. However, deeper splinters that penetrate beyond the epidermis are unlikely to surface on their own and may become permanently embedded or cause infection before natural expulsion occurs.
While rare, untreated splinter infections can potentially lead to sepsis if bacteria enter the bloodstream. This is more likely with deep splinters from contaminated organic materials like wood or plant thorns, especially in individuals with compromised immune systems or diabetes. Seek immediate medical attention if you develop fever, rapid heartbeat, or confusion after a splinter injury.
When your body can’t expel a foreign object, it may encapsulate the splinter with fibrous tissue in a process called granuloma formation. This isolates the foreign material from surrounding tissue. While this prevents spread of infection, it doesn’t eliminate the splinter—the encapsulated foreign body remains embedded and can cause chronic inflammation or pain.
Epsom salt soaks may help with very shallow splinters by softening the skin and reducing inflammation, potentially making removal easier. However, there’s limited scientific evidence that soaking actually “draws out” splinters. For deeper splinters, soaking alone is ineffective and may delay proper removal, increasing infection risk.
Glass splinters are inert and don’t carry bacteria like wooden splinters, but they won’t dissolve or be absorbed by your body. A glass fragment left in your foot can cause chronic pain, inflammation, and difficulty walking. It may also migrate deeper into tissue over time. Glass is visible on X-rays, making medical removal relatively straightforward.
According to medical guidelines, you need tetanus prophylaxis if your last tetanus vaccination was more than 10 years ago for clean minor wounds, or more than 5 years ago for contaminated wounds. Splinters from dirty outdoor sources like rusty metal, soil-contaminated wood, or animal environments are considered higher risk. Consult a healthcare provider if uncertain about your vaccination status.
Yes. Wooden splinters can cause delayed infections because bacteria embedded in the wood fibers may take time to multiply and trigger an immune response. Infections can develop anywhere from 24 hours to several weeks after the initial injury. Medical research has documented cases where retained wooden splinters caused serious complications weeks after the initial penetration, particularly when the foreign body migrated deeper into tissue.