Quick Summary: Popping a blister typically leads to infection risk, delayed healing, and pain. The protective skin roof prevents bacteria entry, and removing it exposes raw tissue. Most blisters heal faster when left intact, though large painful blisters may sometimes require sterile drainage by a healthcare provider.
That fluid-filled bubble on your foot or hand might be tempting to puncture. But popping a blister creates an open wound that significantly increases infection risk.
Understanding what actually happens when blister skin breaks—accidentally or intentionally—helps prevent complications that can turn a minor annoyance into a medical problem.
What Actually Happens When You Pop a Blister
The moment blister skin ruptures, several immediate changes occur. The protective barrier that kept bacteria out disappears, exposing the raw dermis underneath to environmental contaminants.
According to CDC clinical guidance for wound management, any break in the skin creates potential entry points for pathogens. Tetanus vaccination and wound assessment are key preventive measures. The blister fluid—which contains proteins and growth factors that support healing—drains away, removing these beneficial components.
The exposed tissue lacks the protective outer layer of skin cells. This makes the area vulnerable to:
- Bacterial colonization within hours of exposure
- Increased pain from nerve endings now directly exposed to air
- Greater risk of further tissue damage from friction or pressure
- Slower healing compared to intact blisters
Research on burn blister fluid indicates that blister fluid contains beneficial factors for wound healing, including proteins and growth factors that aid tissue repair. When this fluid drains prematurely, those advantages vanish.

Infection Risk: The Primary Danger
The biggest consequence of popping a blister is infection. Once the skin barrier breaks, bacteria like Staphylococcus aureus and Streptococcus can colonize the wound.
According to Mayo Clinic data on staph infections, these bacteria live harmlessly on many people’s skin surfaces. But they become dangerous when introduced through breaks in the skin—exactly what happens with a popped blister.
Surgical site infection research published by the National Institutes of Health shows that even small skin openings can develop serious complications. Research on calcaneal fractures found a 7.9% infection rate after plate internal fixation procedures; fracture blisters complicate treatment and can alter surgical planning.
Warning Signs of an Infected Blister
Recognizing infection early prevents serious complications. Watch for these symptoms:
| Symptom | What It Indicates | Action Required |
|---|---|---|
| Increasing redness spreading beyond blister | Cellulitis developing | Seek care within 24 hours |
| Pus or cloudy fluid drainage | Bacterial infection present | Medical evaluation needed |
| Fever or chills | Systemic infection spreading | Immediate medical attention |
| Warmth extending from site | Inflammation progressing | Professional assessment |
| Red streaks from blister | Lymphangitis (serious) | Emergency care |
The American Academy of Dermatology emphasizes that blisters leaking fluid and opening up require medical care within 24 hours to prevent life-threatening infections.
Pain and Prolonged Healing
Beyond infection, popping blisters causes immediate increased pain. The nerve endings in the dermis aren’t designed for direct environmental exposure.
Intact blisters often heal on their own within a week. Popped blisters typically require longer healing periods because:
- The body must regenerate the entire outer skin layer from scratch
- Continued friction damages forming tissue repeatedly
- Scab formation becomes necessary, adding healing stages
- Risk of re-injury increases without the fluid cushion
That protective roof of blister skin—even though it looks dead—serves critical functions during healing.
When Blisters Pop Accidentally
Sometimes blisters burst without intentional popping. This happens frequently with friction blisters on feet during continued activity.
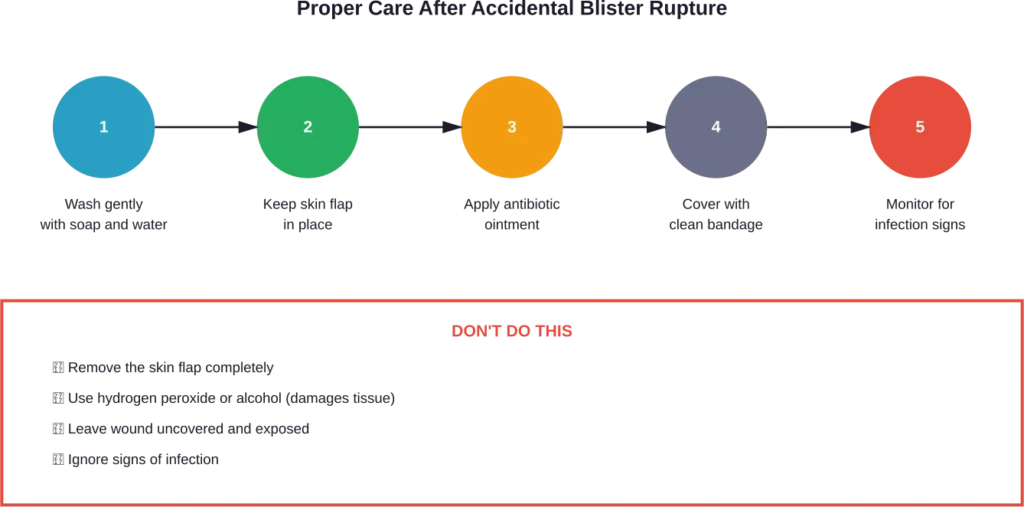
If a blister pops on its own, proper wound care becomes essential:
- Gently wash the area with mild soap and clean water
- Do not remove the overlying skin—it still provides some protection
- Apply antibiotic ointment to prevent bacterial growth
- Cover with a clean, non-stick bandage
- Change dressing daily and monitor for infection signs
According to the American Academy of Dermatology, keeping the skin flap intact—even after the fluid drains—helps minimize scarring and speeds recovery.
Special Cases Requiring Medical Attention
Certain types of blisters should never be popped at home. Medical evaluation becomes necessary when blisters result from:
- Burns (second-degree or deeper)
- Chemical exposure
- Medical conditions like bullous pemphigoid
- Blood-filled blisters indicating deeper damage
- Locations near surgical sites or fractures
Research on fracture blisters indicates these can complicate treatment, making it difficult to splint or cast and often overlying ideal surgical incision sites. Medical literature shows no consensus on managing these specialized blisters—healthcare providers typically recommend either early treatment before blister formation or delay until complete resolution.
Burns present another special concern. The fluid in burn blisters contains factors that aid healing, and premature removal can worsen outcomes.
Frequently Asked Questions
Popped blisters take longer to heal than intact blisters. Intact blisters often heal within a week or less. Healing time extends further if infection develops or the protective skin flap is removed entirely.
Generally speaking, small friction blisters heal without permanent effects. However, infection from improper popping can lead to complications including cellulitis. Severe skin infections such as necrotizing fasciitis are documented in medical case reports as potential surgical site complications.
Large, extremely painful blisters that interfere with walking or daily activities may benefit from sterile drainage by a healthcare provider. Attempting this at home significantly increases infection risk. Medical professionals use proper sterilization techniques and often preserve the blister roof.
Blisters may refill after drainage as the body continues producing protective fluid. This is normal during the first 24 hours. Persistent refilling beyond this period may indicate ongoing tissue damage or improper healing conditions.
Infection signs include increasing redness spreading beyond the original blister, pus or cloudy discharge, warmth, red streaks extending from the area, swelling, fever, or worsening pain after the first day. Any of these symptoms require medical evaluation.
Use non-stick bandages or gauze pads on popped blisters. Standard adhesive bandages can stick to the wound and tear newly forming tissue when removed. Apply antibiotic ointment first to create a barrier between the wound and dressing.
Protect intact blisters with padded dressings that cushion the area without putting direct pressure on the fluid bubble. Donut-shaped pads work well by distributing pressure around the blister rather than on it.
The Bottom Line on Popping Blisters
Popping a blister removes the natural protective barrier, exposes vulnerable tissue, drains beneficial healing fluid, and creates significant infection risk. The consequences—pain, delayed healing, and potential complications—far outweigh any temporary relief.
When blisters pop accidentally, proper wound care minimizes these risks. But intentional popping should be avoided except in specific circumstances under medical supervision.
If dealing with a problematic blister, consult a healthcare provider rather than attempting home drainage. Professional care ensures proper sterilization and technique while reducing complication risks.
