Quick Summary: Eating feces can cause serious bacterial, viral, and parasitic infections due to harmful pathogens like E. coli, Salmonella, hepatitis A, and parasites. While accidental ingestion (especially in children) rarely causes emergencies, symptoms include nausea, vomiting, diarrhea, and fever. Immediate steps include rinsing the mouth, monitoring for symptoms, and contacting a poison center if severe reactions occur.
The idea of eating poop sounds disgusting. And for good reason.
But accidental ingestion happens more than most people realize. Contaminated food, children exploring their environment, or contact with animals can all lead to fecal exposure. While the thought alone makes most people queasy, understanding what actually happens when someone ingests feces can help manage these situations effectively.
Here’s what the science says about eating poop and the health risks involved.
What Are Feces and Why Are They Dangerous?
Feces are waste matter eliminated from the bowels. They consist of undigested food, bacteria, cells from the digestive tract lining, and metabolic byproducts.
But here’s the thing: feces also harbor potentially harmful microorganisms. The human digestive system contains trillions of bacteria, and while many are beneficial, fecal matter concentrates pathogens that can cause serious illness.
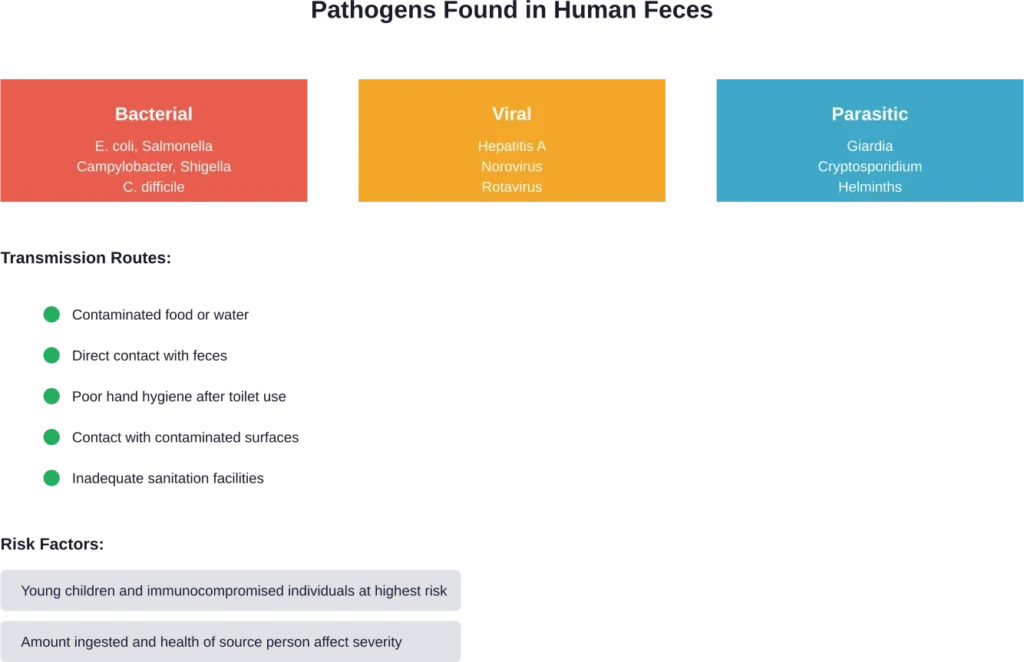
According to the CDC, faecal-oral transmission is a major route for disease spread globally. Bacterial, viral, and parasitic infections commonly transmit this way, particularly in areas with inadequate sanitation.
The danger level depends on several factors: the health status of the person whose feces were ingested, the amount consumed, and the recipient’s immune system strength.
Common Infections From Eating Feces
When someone eats poop, they expose themselves to numerous pathogens. The Illinois Poison Center notes that while accidental fecal ingestion doesn’t always result in medical emergencies, the potential for infection remains real.
Bacterial Infections
Bacteria commonly found in feces include E. coli, Salmonella, Campylobacter, and Shigella. These organisms cause foodborne illnesses with symptoms ranging from mild discomfort to life-threatening complications.
The CDC reports that about 5% of Shigella infections in 2022 were caused by extensively drug-resistant strains. These XDR strains increased from zero in 2015, highlighting evolving resistance patterns.
Campylobacter and Salmonella rank among the leading causes of bacterial gastroenteritis. In 2014, Maryland, Ohio, and Virginia reported 2,977 campylobacteriosis cases and 2,259 salmonellosis cases combined.
C. difficile presents another concern. Around half a million people in the United States get sick from this bacterium annually, often after antibiotic use disrupts normal gut flora.
Viral Infections
Hepatitis A spreads primarily through the fecal-oral route. The virus can survive outside the body for months and causes liver inflammation with symptoms like jaundice, fatigue, and abdominal pain.
Norovirus and rotavirus also transmit through fecal contamination. These viruses cause severe gastroenteritis, particularly dangerous for young children and immunocompromised individuals.
Recent research suggests fecal-oral transmission may play a role in COVID-19 spread, though respiratory transmission remains primary. Approximately 48% of COVID-19 patients in Hong Kong had detectable SARS-CoV-2 RNA in stool samples, even after negative tests of respiratory samples.
Parasitic Infections
Parasites like Giardia, Cryptosporidium, and various helminths can transmit through fecal matter. These organisms cause persistent diarrhea, malabsorption, and in severe cases, long-term developmental issues in children.
Baylisascaris procyonis, a roundworm found in raccoon feces, poses particular danger. While infection in humans is rare (about 7% of wildlife rehabilitators show exposure), it can affect the brain, spinal cord, and eyes with serious consequences.
Symptoms of Fecal Ingestion
Symptoms after eating poop typically appear within hours to days, depending on the pathogen involved.
Common symptoms include:
- Nausea and vomiting
- Diarrhea (sometimes bloody)
- Abdominal cramps and pain
- Fever and chills
- Dehydration
- Loss of appetite
- Weakness and fatigue
Severe cases may involve high fever, severe dehydration requiring intravenous fluids, or signs of systemic infection. According to the CDC’s guidance on foodborne illnesses, concerning symptoms include persistent vomiting, bloody diarrhea, fever above 101.5°F, and signs of dehydration like decreased urination or dizziness.
The WHO notes that diarrheal diseases remain a leading cause of death globally among children under five. Severe diarrhea leads to fluid loss that can be life-threatening, particularly in young children and those with compromised immunity.
What to Do If Someone Eats Poop
Immediate action can reduce infection risk and complications.
Immediate Steps
First, rinse the mouth thoroughly with water. This helps remove remaining fecal matter and bacteria. Do not induce vomiting unless specifically instructed by a medical professional.
Offer small sips of water to help rinse away bacteria from the mouth and throat. For children, monitor closely for any immediate distress.
Contact a poison control center for guidance. The National Poison Control hotline (1-800-222-1222) provides free, confidential, 24-hour expert advice. Online resources like webPOISONCONTROL also offer immediate assistance.
Monitoring and Medical Care
Watch for symptoms over the next 24-48 hours. Most infections manifest within this timeframe, though some parasites have longer incubation periods.
Seek medical attention if severe symptoms develop, including persistent vomiting, bloody diarrhea, high fever, severe abdominal pain, or signs of dehydration. Infants, elderly individuals, and those with weakened immune systems should receive medical evaluation even with mild symptoms.
Medical treatment depends on the pathogen identified. Bacterial infections may require antibiotics, though antibiotic resistance complicates treatment for some strains. The CDC notes that ampicillin or TMP-SMX can treat susceptible Shigella strains, but XDR strains require alternative approaches.
Viral infections typically receive supportive care focused on hydration and symptom management. According to WHO guidelines, oral rehydration solution (ORS) replaces water and electrolytes lost through diarrhea. Zinc supplements can reduce diarrhea duration by 25% and stool volume by 30%.
Special Considerations for Children and Babies
Babies and toddlers explore the world through their mouths, making accidental fecal ingestion more common in this age group.
If a baby eats poop, parents should remain calm but vigilant. While concerning, most cases don’t result in serious complications. Rinse the baby’s mouth gently with water and monitor for symptoms like unusual fussiness, vomiting, diarrhea, or fever.
Contact a pediatrician or poison center for specific guidance. Medical professionals can assess risk based on the amount ingested, the child’s health status, and the feces source (human, pet, or wildlife).
Prevention matters more than treatment. Flush toilets immediately after use, wash hands thoroughly after diaper changes, keep diaper pails secured, and supervise young children around pets and their waste.
Animal Feces: A Different Risk Profile
Pet feces carry different pathogens than human waste. Dogs and cats can harbor bacteria like Salmonella and Campylobacter, parasites like Toxoplasma and Giardia, and various worms.
Interestingly, about 16% of dogs engage in coprophagy (eating feces), according to research published in Veterinary Medicine and Science. This behavior, while paradoxical given dogs’ typical aversion to conspecific feces, appears linked to ancestral scavenging behaviors.
Wildlife feces present additional risks. Raccoon feces may contain Baylisascaris, while bird droppings can carry histoplasmosis spores. Research on raw meat feeding (BARF diet) in pets shows these animals can shed parasites that pose risks to other household members.
| Feces Source | Common Pathogens | Primary Risks |
|---|---|---|
| Human | E. coli, Salmonella, Hepatitis A, Norovirus | Gastroenteritis, liver infection, severe dehydration |
| Dog/Cat | Toxoplasma, Giardia, Roundworms, Campylobacter | Parasitic infections, gastroenteritis, especially risky for pregnant women |
| Wildlife (Raccoon) | Baylisascaris, Leptospira | Neurological damage, organ failure |
| Bird | Histoplasma, Salmonella, Cryptococcus | Respiratory infections, systemic illness |
When Feces Becomes Medicine: Fecal Transplants
Not all fecal exposure is harmful. Fecal microbiota transplantation (FMT) represents a legitimate medical treatment for recurrent C. difficile infections.
The procedure involves transferring stool from a healthy donor to a patient’s gastrointestinal tract, restoring beneficial bacteria that antibiotics destroyed. Some research indicates that fecal transplantation can resolve up to 90% of C. difficile cases.
But here’s the critical distinction: medical fecal transplants use extensively screened donors and processed material administered under controlled conditions. This differs entirely from accidental or intentional consumption of unscreened feces.
Research continues into FMT applications for inflammatory bowel disease, obesity, and other conditions linked to gut microbiome disruption.
Prevention: The Best Defense
Preventing fecal-oral transmission requires multiple strategies. The WHO identifies water, sanitation, and hygiene interventions as primary prevention methods for diarrheal diseases.
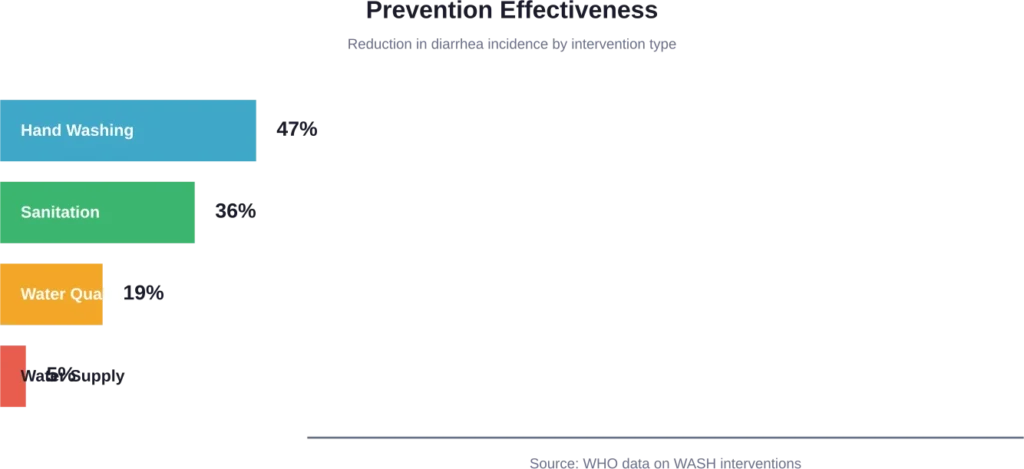
Hand washing with soap after toilet use and before food preparation reduces diarrhea incidence by up to 47%, according to pooled analyses. Access to improved sanitation facilities reduces incidence by 36%, while water quality interventions achieve 19% reduction.
Key prevention strategies include:
- Thorough hand washing with soap after bathroom use and before handling food
- Proper food handling and storage practices
- Safe drinking water from improved sources
- Adequate sanitation facilities with proper waste disposal
- Supervising young children around potential fecal contamination sources
- Keeping pet areas clean and washing hands after animal contact
In 2022, at least 1.7 billion people globally used drinking water sources contaminated with feces, according to WHO data. Addressing this requires infrastructure improvements alongside behavior change.
Frequently Asked Questions
While rare, eating feces can be fatal in severe cases, particularly for vulnerable populations like infants, elderly individuals, or those with compromised immune systems. Severe dehydration from diarrhea and systemic infections from pathogens like E. coli or hepatitis A can become life-threatening without prompt treatment. Most cases result in temporary illness rather than death, but medical attention is essential for severe symptoms.
Symptom onset varies by pathogen. Bacterial infections like Salmonella typically cause symptoms within 6-72 hours. Norovirus acts faster, often within 12-48 hours. Hepatitis A has a longer incubation period of 15-50 days. Parasites may take weeks to manifest symptoms. Most acute gastroenteritis symptoms appear within 24-48 hours of exposure.
No. While the pathogen profile differs slightly, eating one’s own feces still poses significant health risks. The digestive system concentrates harmful bacteria and metabolic waste products meant for elimination. These substances can cause infection when reintroduced to the mouth and upper digestive tract. Additionally, individuals with undiagnosed infections pose risks to themselves through fecal-oral re-exposure.
Rinse the child’s mouth with water immediately. Contact a poison control center or pediatrician for guidance. Dog feces can contain Toxoplasma, Giardia, roundworms, and various bacteria. Monitor the child for vomiting, diarrhea, fever, or unusual behavior over the next 48 hours. Most cases require only observation, but medical evaluation may be necessary depending on the amount consumed and the child’s symptoms.
Research indicates SARS-CoV-2 can be detected in feces, and gastrointestinal infection occurs in some patients. Approximately 48% of COVID-19 patients experience GI symptoms. While respiratory transmission remains the primary route, some evidence suggests fecal-oral transmission is possible, particularly in settings with inadequate sanitation. Proper hand hygiene and sanitation practices help minimize this risk.
Coprophagy serves different purposes across species. Rabbits and rodents practice it to extract additional nutrients from partially digested plant material. Research shows the growth of rats is stunted by 20% when coprophagia is prevented, and coprophagia appears to aid bacterial synthesis of nutrients, particularly B group vitamins and vitamin K. Dogs may engage in coprophagy due to ancestral scavenging behaviors, though about 16% of dogs do this frequently. Birds sometimes practice parental coprophagy, which may relate to microbiome transmission to offspring.
Yes. Fecal microbiota transplantation treats recurrent C. difficile infections with high success rates. Some research indicates that fecal transplantation can resolve up to 90% of C. difficile cases. The procedure uses extensively screened donor stool to restore healthy gut bacteria. Research continues into FMT applications for inflammatory bowel disease, metabolic disorders, and other conditions. However, this medical procedure differs entirely from consuming unprocessed, unscreened feces.
The Bottom Line
Eating poop poses real health risks due to bacterial, viral, and parasitic pathogens concentrated in fecal matter. While accidental ingestion happens, particularly among young children, prompt action and monitoring can prevent serious complications.
If fecal ingestion occurs, rinse the mouth, monitor for symptoms, and contact medical professionals or poison control for guidance. Prevention through proper hygiene, sanitation, and supervision remains the most effective strategy.
Understanding these risks empowers better decision-making in both everyday situations and emergencies. When in doubt, seek professional medical advice rather than waiting for symptoms to worsen.
