Quick Summary: Not getting enough protein can lead to muscle loss, weakened immunity, brittle hair and nails, persistent hunger, and slower wound healing. According to WHO, protein deficiency contributes to severe malnutrition conditions affecting millions worldwide. Most sedentary adults require approximately 0.36 grams of protein per pound of body weight daily as a minimum to prevent deficiency.
Protein gets plenty of attention these days, and for good reason. It’s not just about building muscle or following the latest wellness trend. This macronutrient plays critical roles in nearly every function inside the body—from maintaining immune defenses to keeping hair strong and skin healthy.
But what actually happens when protein intake falls short?
The consequences range from subtle signs like constant hunger to serious conditions that affect millions globally. According to NIH research, severe acute malnutrition manifests in two primary forms: marasmus (extreme wasting from overall calorie deficiency) and kwashiorkor (nutritional edema from severe protein deficiency). Both conditions present life-threatening complications, particularly in vulnerable populations.
Understanding these effects isn’t about creating fear. It’s about recognizing the real signs that the body might need more protein—and knowing how to address them before minor issues become major problems.
Why Protein Matters for Every Body Function
Protein isn’t just one thing. It’s composed of amino acids—often called the building blocks of life. These compounds form the structural foundation for muscles, bones, skin, and hair. They also create enzymes that drive chemical reactions, hormones that regulate processes, and antibodies that defend against infection.
Without adequate protein, the body can’t perform these essential functions properly.
According to WHO guidelines on healthy diets, protein represents one of the critical macronutrients required for adequate nutrition. The organization emphasizes that protein adequacy meets micronutrient and macronutrient needs without exceeding them—a balance that’s easier to disrupt than many realize.
Here’s the thing though—the body doesn’t store protein the way it stores fat or carbohydrates. When protein intake drops, the body starts breaking down muscle tissue to access the amino acids it needs for more critical functions. This process happens gradually, making the early signs easy to miss.
The Visible Signs: Hair, Skin, and Nails
Some of the earliest and most noticeable effects show up in appearance. Hair, skin, and nails all depend heavily on protein structures—particularly keratin and collagen.
Hair Changes
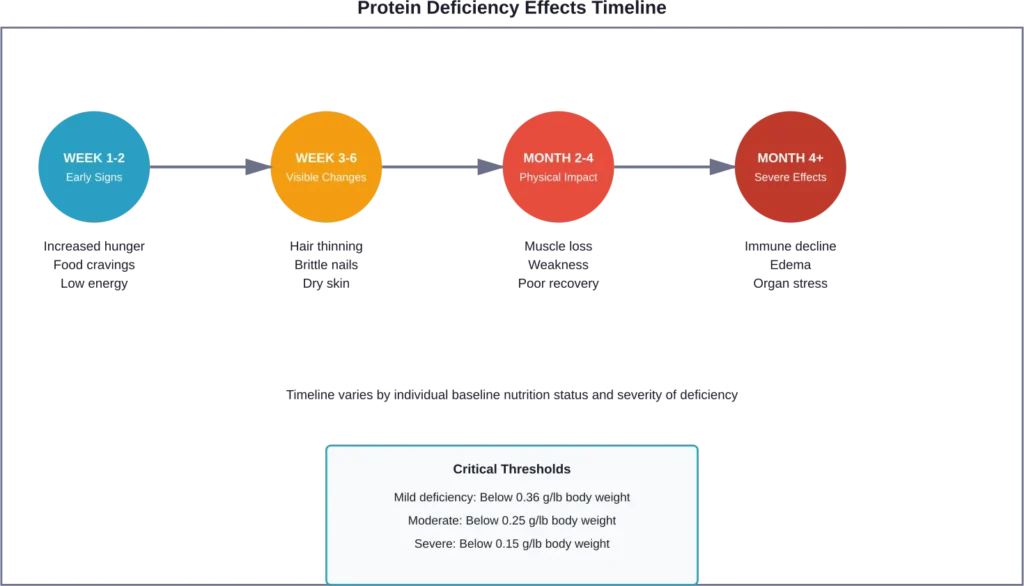
Hair that’s thinning, brittle, or losing its shine often signals insufficient protein intake. Hair follicles require constant protein supplies to produce new strands. When that supply dwindles, growth slows and existing hair becomes fragile.
Some people notice their hair breaking more easily during brushing or washing. Others see increased shedding in the shower. These changes don’t happen overnight—they develop gradually as protein stores deplete.
Skin Problems
Skin might appear dry, flaky, or lose its elasticity. In severe cases documented by NIH researchers, protein deficiency can cause skin lesions and changes in pigmentation. The skin relies on collagen—a protein—to maintain structure and resilience.
Wounds also heal more slowly when protein levels are low. The body needs amino acids to repair damaged tissue and generate new cells at injury sites.
Brittle Nails
Nails that crack, peel, or develop ridges frequently point to nutritional deficiencies, with protein deficiency being a common culprit. Nail beds require consistent protein to produce the keratin that makes nails strong.
These cosmetic changes might seem minor, but they’re actually the body’s way of rationing limited resources. When protein is scarce, the body prioritizes vital organs over hair and nails.
Muscle Loss and Physical Weakness
Muscle tissue represents the body’s largest protein reservoir. When dietary protein falls short, the body cannibalizes muscle to maintain more critical functions.
This process—called muscle wasting or sarcopenia when chronic—affects strength, mobility, and overall physical performance. According to recent NIH research on protein intake and muscle mass, preserving muscle during stress or illness requires not just protein, but adequate energy balance and minimal muscle disuse.
The effects include:
- Difficulty building muscle despite exercise
- Loss of muscle mass and definition
- Decreased strength for everyday tasks
- Slower recovery after workouts
- Increased fatigue during physical activity
For older adults, this becomes particularly concerning. NIH studies on elderly females show that protein intake levels significantly impact muscle mass composition. The research compared 0.8 grams per kilogram of body weight versus 1.2 grams per kilogram, finding notable differences in muscle preservation at higher intakes.
Real talk: losing muscle doesn’t just affect appearance or athletic performance. It impacts metabolic rate, glucose regulation, and long-term mobility. Less muscle means fewer calories burned at rest, which can create a cascade of metabolic changes.
Constant Hunger and Food Cravings
Ever feel hungry an hour after eating? Insufficient protein might be the culprit.
Protein is the most satiating macronutrient—it keeps people feeling full longer than carbohydrates or fats. When meals lack adequate protein, hunger returns quickly, often accompanied by cravings for quick energy from sugary or starchy foods.
This creates a frustrating cycle. Low protein intake triggers hunger, leading to snacking on carbohydrate-heavy foods that provide temporary satisfaction but don’t address the underlying protein deficit. The hunger returns, and the pattern repeats.
According to nutrition research, at least 10% of daily calories should come from protein. For someone eating 2,000 calories daily, that’s roughly 50 grams minimum. To calculate individual needs more precisely, multiply body weight in pounds by 0.36—that’s the baseline protein requirement in grams.
But here’s where it gets interesting: many experts suggest these baseline recommendations are too low for optimal health. Active individuals, older adults, and people recovering from illness often need significantly more.
Weakened Immune System and Frequent Illness
Getting sick more often than usual? Low protein might be undermining immune defenses.
Antibodies—proteins that identify and neutralize pathogens—require amino acids for production. When protein intake drops, the immune system can’t generate adequate antibodies or maintain sufficient levels of infection-fighting cells.
This manifests as:
- More frequent colds and infections
- Longer recovery times from illness
- Wounds that heal slowly
- Increased susceptibility to seasonal illnesses
According to WHO data on nutrition, malnutrition in all forms weakens immune systems and increases disease susceptibility. The organization notes that proper nutrition—including adequate protein—helps protect against both infectious diseases and noncommunicable conditions.
Children face particularly high risks. NIH research shows that young children with severe acute malnutrition typically have concomitant micronutrient deficiencies affecting immune function, cognitive development, and growth.
Severe Protein Deficiency: Kwashiorkor and Marasmus
In extreme cases, prolonged protein deficiency leads to life-threatening conditions that affect millions worldwide.
Kwashiorkor develops primarily from severe protein deficiency despite adequate or near-adequate calorie intake. The condition typically affects young children after early weaning to low-protein, high-carbohydrate diets. Kwashiorkor typically affects young children after early weaning to low-protein, high-carbohydrate diets, and the condition is characterized by bilateral edema and other distinctive features documented in NIH medical literature.
Characteristic features include:
- Bilateral edema (fluid retention and swelling)
- Enlarged, fatty liver
- Skin lesions and pigmentation changes
- Thinning, discolored hair
- Muscle wasting despite edema
Marasmus, by contrast, results from overall calorie deficiency including protein. Children with marasmus show severe wasting with minimal edema—essentially starvation affecting all macronutrients.
While these severe forms primarily affect populations experiencing food insecurity, they illustrate the critical nature of protein for human health. Even in developed countries, milder forms of protein-energy malnutrition occur among hospitalized patients, elderly individuals with poor appetite, and people with restrictive eating patterns.
How Much Protein Do You Actually Need?
The question everyone asks: what’s the right amount?
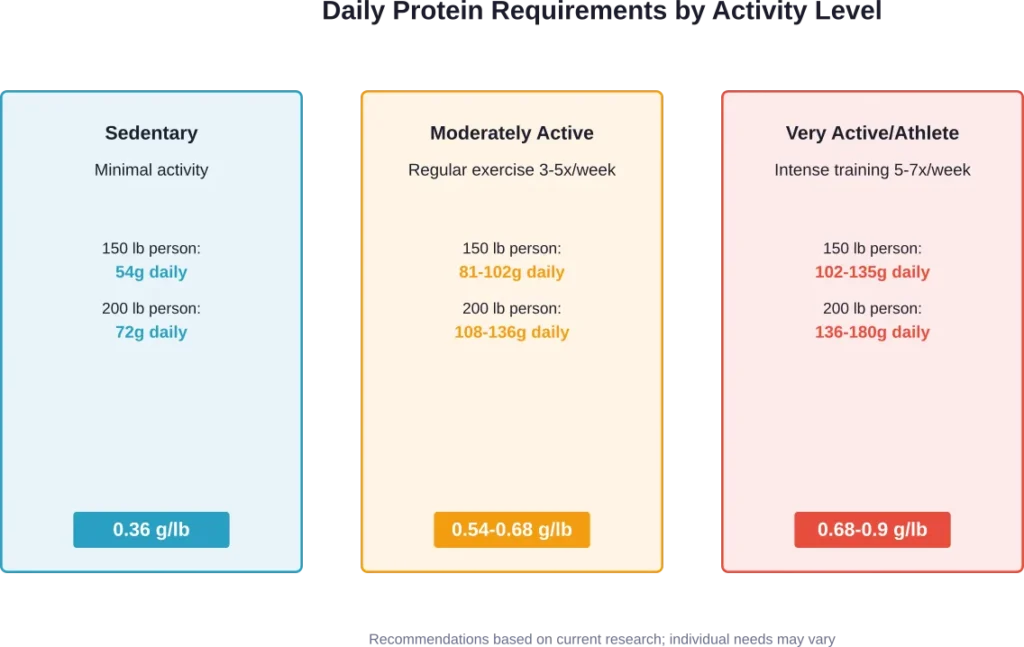
The baseline recommendation—0.36 grams per pound of body weight—represents the minimum to prevent deficiency in sedentary adults. For a 150-pound person, that’s approximately 54 grams daily. For someone weighing 200 pounds, approximately 72 grams.
But optimal intake often exceeds these minimums, particularly for:
- Active individuals and athletes (0.54-0.9 g/lb)
- Older adults maintaining muscle mass (0.54-0.68 g/lb)
- People recovering from illness or injury (0.68-0.9 g/lb)
- Pregnant and breastfeeding women (additional 25-30g daily)
WHO expert consultations on protein and amino acid requirements acknowledge that needs vary based on age, gender, physical activity level, and physiological state. The organization emphasizes adequate protein as part of diversified, balanced diets.
Spreading protein throughout the day also matters. Protein intake distributed across meals may support optimal utilization, with recommendations often suggesting 20-30 grams per meal.
Best Protein Sources: Animal vs. Plant
Not all protein sources are created equal. The body uses some more efficiently than others based on amino acid profiles and digestibility.
Complete vs. Incomplete Proteins
Complete proteins contain all nine essential amino acids the body can’t produce on its own. Most animal sources qualify as complete proteins:
- Meat (beef, pork, lamb)
- Poultry (chicken, turkey)
- Fish and seafood
- Eggs
- Dairy products (milk, yogurt, cheese)
Plant proteins are typically incomplete, lacking one or more essential amino acids. Exceptions include quinoa, soy, buckwheat, and hemp seeds. However, combining different plant proteins throughout the day provides all essential amino acids—think beans with rice, or hummus with whole grain bread.
Digestibility Matters
The body absorbs animal proteins more readily than most plant proteins. This doesn’t mean plant proteins are inferior—it just means plant-based eaters may need slightly higher total intake to meet amino acid requirements.
Protein powders offer convenience for people struggling to meet needs through whole foods. Whey protein (dairy-based) digests quickly and contains all essential amino acids. Plant-based powders from pea, rice, or hemp provide alternatives for those avoiding animal products.
| Protein Source | Serving Size | Protein Content | Complete Protein? |
|---|---|---|---|
| Chicken breast | 3 oz cooked | 26g | Yes |
| Ground beef (90% lean) | 3 oz cooked | 22g | Yes |
| Salmon | 3 oz cooked | 22g | Yes |
| Eggs | 2 large | 12g | Yes |
| Greek yogurt | 6 oz | 17g | Yes |
| Lentils | 1 cup cooked | 18g | No |
| Black beans | 1 cup cooked | 15g | No |
| Tofu | 4 oz | 10g | Yes |
| Quinoa | 1 cup cooked | 8g | Yes |
| Almonds | 1 oz (23 nuts) | 6g | No |
Special Populations at Risk
Certain groups face higher risks of protein deficiency and may need closer monitoring.
Older Adults
Aging reduces appetite and changes taste perception, often leading to decreased food intake overall. Simultaneously, older bodies become less efficient at using dietary protein for muscle maintenance. This combination puts elderly individuals at elevated risk for sarcopenia and frailty.
Research on protein intake in aging populations indicates that adequate dietary protein supports muscle mass and bone health. Studies comparing different protein intake levels show variations in outcomes among older adults.
Hospitalized Patients
Illness and hospitalization increase protein needs while often decreasing appetite. Patients recovering from surgery, fighting infections, or managing chronic conditions require extra protein for tissue repair and immune function.
Research on nutritional support in critically ill patients indicates that adequate protein intake may support muscle preservation and nutritional outcomes.
Plant-Based Eaters
Vegetarians and vegans can absolutely meet protein needs—it just requires more intentional planning. The lower digestibility of most plant proteins means total intake may need to increase by 10-20% compared to omnivorous diets.
Variety becomes essential. Relying on a single plant protein source increases the risk of amino acid gaps. Rotating between legumes, whole grains, nuts, seeds, and soy products ensures comprehensive amino acid coverage.
Disease-Related Malnutrition and Protein
Protein deficiency doesn’t only stem from inadequate intake. Disease-related malnutrition (DRM) affects millions who consume seemingly adequate diets but can’t properly absorb or utilize nutrients.
Conditions affecting protein status include:
- Digestive disorders (Crohn’s disease, celiac disease, IBS)
- Kidney disease (requiring careful protein balance)
- Liver disease (affecting protein synthesis)
- Cancer and cancer treatments (increasing needs while reducing appetite)
- Chronic infections (elevating protein requirements)
Disease-related malnutrition affecting protein status remains an important clinical concern, particularly in patients with digestive disorders, kidney disease, liver disease, and chronic infections. They independently and synergistically contribute to increased risk of adverse health outcomes.
Targeted nutritional interventions—including appropriate protein intake adjusted for specific conditions—can significantly improve outcomes for these populations.
Recognizing the Warning Signs
Now that the consequences are clear, what should people actually watch for?
Early warning signs include:
- Persistent hunger shortly after meals
- Cravings for carbohydrate-heavy snacks
- Fatigue that doesn’t improve with rest
- Difficulty concentrating or brain fog
- More frequent minor infections
Physical changes that develop over weeks to months:
- Hair thinning or increased shedding
- Brittle, splitting nails
- Dry, flaky skin
- Muscle definition decreasing despite exercise
- Strength declining for routine activities
- Longer recovery times after workouts
Severe deficiency signs requiring medical attention:
- Significant unintended weight loss
- Swelling in legs, feet, or abdomen (edema)
- Severe fatigue affecting daily function
- Frequent infections or wounds not healing
- Cognitive changes or confusion
Anyone experiencing severe symptoms should consult healthcare providers. Blood tests can assess protein status, albumin levels, and overall nutritional markers to guide appropriate interventions.
Fixing Protein Deficiency: Practical Steps
Addressing low protein intake doesn’t require complicated meal plans or expensive supplements. Small, strategic changes often make significant differences.
Start With Breakfast
Many breakfast foods are carbohydrate-heavy but protein-poor. Cereal, toast, pastries, and fruit alone won’t cut it. Adding eggs, Greek yogurt, cottage cheese, or protein powder to morning smoothies establishes a strong foundation for the day.
Prioritize Protein at Every Meal
Build meals around protein sources rather than treating them as afterthoughts. Choose the protein first—whether chicken, fish, beans, or tofu—then add vegetables, grains, and healthy fats around it.
Aim for these per-meal targets:
- Breakfast: 20-25g
- Lunch: 25-30g
- Dinner: 25-30g
- Snacks: 10-15g total
Keep Convenient Protein Options Available
Preparation barriers often derail good intentions. Stock easy protein sources:
- Hard-boiled eggs (prepare several at once)
- Greek yogurt cups
- String cheese or cheese cubes
- Cooked chicken strips
- Canned tuna or salmon
- Protein bars (check labels—aim for 15g+ per bar)
- Nuts and nut butter
- Protein powder for quick shakes
Track Intake Temporarily
Most people significantly underestimate protein consumption. Tracking intake for just a few days using a food diary or app reveals actual patterns and highlights gaps. This awareness alone often drives meaningful changes.
When to See a Doctor
Most cases of insufficient protein intake respond well to dietary adjustments. But certain situations warrant professional evaluation:
- Unexplained weight loss exceeding 5% of body weight
- Persistent swelling in extremities
- Severe fatigue unresponsive to diet changes
- Recurrent infections or poor wound healing
- Underlying conditions affecting digestion or metabolism
- Pregnancy, breastfeeding, or advanced age with concerning symptoms
Healthcare providers can order blood tests assessing albumin, prealbumin, and total protein levels. They can also evaluate for underlying conditions contributing to protein malnutrition and recommend appropriate interventions, which might include dietary counseling, oral supplements, or in severe cases, medical nutrition therapy.
Frequently Asked Questions
Recovery timelines vary based on severity and individual circumstances. Mild deficiency often shows improvement within 2-3 weeks of increased intake, with visible changes to hair, skin, and energy levels. Muscle mass recovery takes longer—typically 8-12 weeks of adequate protein combined with resistance exercise. Severe deficiency requires medical supervision and may take several months of targeted nutritional intervention.
Yes, absolutely. While meat eaters generally have easier access to complete proteins, total intake still matters. Someone eating small portions infrequently, skipping meals, or relying heavily on processed foods might still fall short of requirements despite consuming some meat. Portion sizes and meal frequency both factor into adequacy.
Protein powder offers a convenient, efficient way to increase intake, particularly for people with poor appetite, high requirements, or limited time for food preparation. However, whole food sources provide additional nutrients—vitamins, minerals, healthy fats—that powders lack. Ideally, powders supplement a varied diet rather than replacing whole foods entirely.
Most people tolerate gradual increases well. Sudden dramatic increases might cause temporary digestive discomfort—bloating, gas, or changes in bowel habits—as the body adjusts. Increasing intake gradually over 7-10 days minimizes these effects. Adequate hydration also helps, as protein metabolism produces nitrogen waste that kidneys must filter.
While severe forms like kwashiorkor are rare in developed nations, milder deficiency can occur in children with very restrictive diets, food allergies limiting options, or extremely picky eating patterns. Growth delays, frequent illness, or low energy might signal inadequate protein. Pediatricians can assess nutritional status and recommend appropriate interventions.
Both can prevent deficiency when consumed in adequate amounts with attention to amino acid completeness. Animal proteins provide all essential amino acids in single sources with high digestibility. Plant proteins require combining various sources throughout the day to ensure complete amino acid profiles. Neither approach is inherently superior—both work when properly planned.
Typically, severe protein deficiency causes weight loss due to muscle wasting. However, the fluid retention seen in kwashiorkor can mask this loss and even increase scale weight despite tissue wasting. Mild deficiency sometimes contributes to weight gain indirectly—constant hunger from low protein leads to overconsumption of high-calorie carbohydrates, creating calorie surpluses despite protein deficits.
The Bottom Line
Protein isn’t just another wellness trend or bodybuilding obsession. It’s an absolute requirement for maintaining the body’s most fundamental functions—from building and preserving muscle to supporting immune defenses and keeping hair, skin, and nails healthy.
The consequences of inadequate intake range from annoying but minor issues like brittle nails and constant hunger to serious medical conditions affecting millions globally. According to WHO and NIH data, protein deficiency contributes significantly to malnutrition burdens, particularly in vulnerable populations including children, elderly individuals, and those with chronic illness.
But here’s the good news: for most people, preventing or correcting protein deficiency is entirely achievable through straightforward dietary adjustments. Understanding individual requirements, choosing quality protein sources, and distributing intake across meals creates a strong foundation for optimal health.
Calculate personal protein needs using body weight and activity level. Track intake for a few days to establish current patterns. Make incremental changes prioritizing protein at each meal. Monitor how the body responds—energy levels, recovery, hunger patterns, and physical changes all provide feedback about adequacy.
The body communicates its needs clearly. Those signals—whether persistent hunger, thinning hair, or declining strength—deserve attention. Addressing them doesn’t require perfection, just consistent effort toward meeting this fundamental nutritional requirement.
Start today. Check current intake, identify gaps, and take one concrete step toward adequate protein consumption. The benefits—sustained energy, maintained muscle, strong immunity, and overall vitality—are worth the effort.
