Quick Summary: Stopping eye injections for macular degeneration typically leads to worsening vision, though some patients with stable wet AMD may safely discontinue treatment under close monitoring. Research shows up to 30% of wet AMD patients can safely stop injections under specific circumstances with close monitoring, but most require ongoing treatment every 4-6 weeks to prevent disease progression and permanent damage to the macula.
Age-related macular degeneration affects millions of people, making it one of the leading causes of blindness in western countries. For those with the wet form of the disease, regular eye injections have become the standard treatment.
But here’s the thing—these injections are inconvenient, uncomfortable, and costly. So it’s no surprise that many patients wonder whether they can safely stop treatment.
The answer isn’t straightforward. What happens when you stop depends on multiple factors, including disease stability, treatment response, and individual patient characteristics.
Understanding Macular Degeneration and Why Injections Matter
Macular degeneration comes in two forms: dry and wet. While only 10% of people with macular degeneration develop the wet form, these patients face much worse outcomes—in the past, wAMD has caused 90 percent of the blindness associated with macular degeneration.
Wet AMD occurs when abnormal blood vessels grow beneath the retina. These vessels leak fluid and blood, causing damage to the macula—the central part of your retina responsible for sharp, detailed vision.
Eye injections deliver anti-VEGF medications directly into the eye. These drugs target vascular endothelial growth factor, the protein that promotes abnormal blood vessel growth. By blocking VEGF, the injections reduce vessel formation and leakage.
The treatment works. Research demonstrates that treating wet AMD generates substantial patient benefit, with economic models showing treatment value between $5.1 and $8.2 billion in patient benefit according to USC researchers.
What Typically Happens When You Stop Treatment
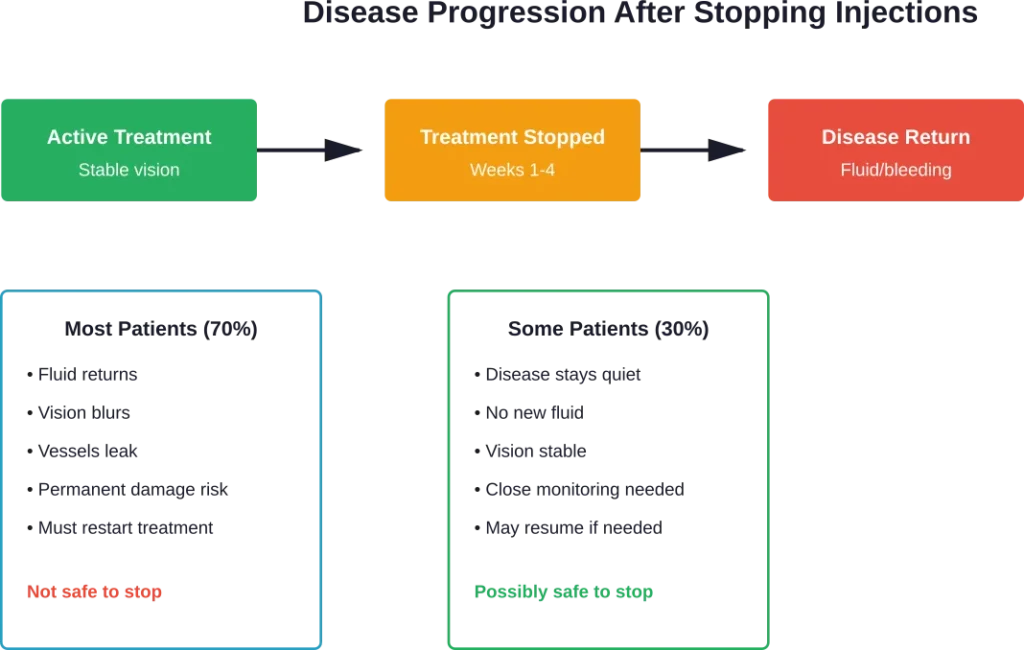
For most patients, stopping injections without medical guidance leads to disease progression. The abnormal blood vessels don’t disappear—they’re only controlled while medication remains active in the eye.
Vision deterioration can happen rapidly or more gradually. Some patients experience sudden bleeding or fluid accumulation. Others see slower decline over weeks or months.
Real talk: the macula doesn’t heal from this type of damage. Once cells are lost or scarring occurs, that vision loss becomes permanent. This makes timely treatment critical.
Research on Safely Stopping Eye Injections
Now, this is where it gets interesting. Recent research from the National Eye Institute shows that up to 30% of patients with wet macular degeneration can safely stop eye injections under specific circumstances.
The key word here? “Specific.”
These patients typically have stable disease after extended treatment. They’ve shown no active leakage or fluid accumulation for a significant period, and they continue regular monitoring even after stopping injections.
According to experts from the American Academy of Ophthalmology, after 3 injections of aflibercept, approximately 20% of patients will have persistent leakage. With 3 injections of ranibizumab, about 30% of patients will have persistent leakage.
One study showed that of patients who elected to discontinue injections, only 2.4% restarted treatment within 24 months. However, this low percentage came from a select group—patients who had reached end-stage disease where further treatment offered minimal benefit.
Treatment Schedules and Monitoring
Standard treatment typically involves injections every 4-6 weeks initially. Over time, doctors may extend the interval using a “treat-and-extend” protocol.
This approach gradually increases time between injections for patients showing stable response. If the disease remains quiet at longer intervals, some patients eventually discontinue treatment while maintaining vigilant monitoring.
The American Academy of Ophthalmology notes that financial and practice burdens of anti-VEGF agents influence treatment schedules. Drug costs vary dramatically—averaging about $50 per injection for Avastin, $2,000 for Lucentis, and $1,850 for Eylea.
Risks of Stopping Without Medical Supervision
Stopping injections without doctor approval carries serious risks. The most significant? Rapid vision loss that can’t be reversed.
When abnormal blood vessels reactivate, they can cause:
- Sudden bleeding into the retina
- Fluid accumulation beneath the macula
- Scarring and permanent tissue damage
- Expansion of blind spots in central vision
- Progressive loss of reading and driving ability
Here’s the thing though—even if vision seems stable, underlying disease activity may continue. Without regular monitoring, patients won’t detect problems until significant damage occurs.
| Risk Factor | Impact if Injections Stopped | Monitoring Requirement |
|---|---|---|
| Active fluid leakage | Rapid vision deterioration | Monthly eye exams |
| Recent bleeding | Recurrent hemorrhage likely | Every 2-4 weeks |
| Unstable disease course | Unpredictable progression | Monthly initially |
| Stable for 12+ months | Lower risk of recurrence | Every 2-3 months |
When Doctors May Recommend Stopping Treatment
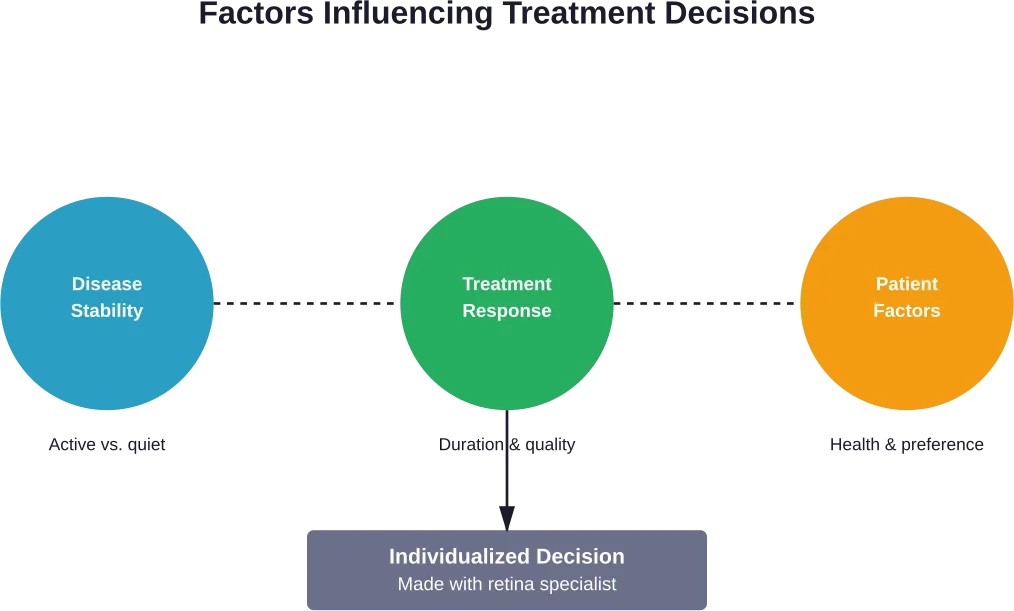
Retina specialists consider several factors when discussing treatment discontinuation. Disease stability tops the list—patients need extended periods without active leakage or new vessel growth.
Some patients reach end-stage disease where the macula has developed permanent scarring. In these cases, continued injections offer minimal vision benefit. The decision becomes about quality of life versus treatment burden.
Other situations where stopping might be considered:
- Severe systemic health issues making injections risky
- Patient preference after informed discussion of risks
- Geographic atrophy development without active neovascularization
- Extended disease quiescence on treat-and-extend protocol
But wait. Even in these scenarios, stopping doesn’t mean abandoning care. Regular monitoring remains essential to catch any disease reactivation early.
Alternative Approaches and Future Treatments
For patients struggling with the injection burden, some alternatives exist. Longer-acting anti-VEGF medications can extend time between treatments for responsive patients.
Research continues into sustained-release delivery systems that could reduce injection frequency. Some investigational approaches involve implantable devices that release medication over months.
Photodynamic therapy and laser treatments represent older options, though anti-VEGF injections have largely replaced these due to superior outcomes.
The treatment landscape continues evolving. Clinical trials registered on ClinicalTrials.gov explore new approaches to reducing treatment burden while maintaining vision protection.
Making the Decision: Talking With Your Eye Specialist
The decision to continue or stop injections shouldn’t happen in isolation. Open communication with your retina specialist is critical.
Come prepared to discuss:
- Current vision quality and any recent changes
- Treatment burden and how it affects daily life
- Financial concerns related to ongoing therapy
- Ability to maintain regular monitoring appointments
- Any health changes that might affect treatment decisions
Your doctor will review imaging studies showing disease activity, discuss your treatment response history, and assess risk factors for disease progression. This comprehensive evaluation guides personalized recommendations.
Many patients feel caught between wanting to stop uncomfortable treatments and fearing vision loss. That tension is normal. The goal is finding the right balance for each specific situation.
Frequently Asked Questions
Some patients experience extended quiet periods without active disease, but true permanent remission is uncommon. Research shows about 30% of patients can safely stop injections with close monitoring, but most eventually require resumed treatment if they live long enough. The abnormal blood vessels typically remain present even when inactive.
The timeline varies considerably between patients. Some experience rapid fluid accumulation within weeks, while others maintain stability for months. Disease activity before stopping treatment is the best predictor—patients with recently active disease tend to worsen faster than those with prolonged stability.
Watch for blurred or distorted central vision, new dark spots, difficulty reading, and straight lines appearing wavy. However, early reactivation often occurs without noticeable symptoms, making regular eye examinations essential even after stopping injections. Imaging tests can detect fluid before vision changes occur.
Yes, treatment can typically resume if disease reactivates. However, vision lost during the treatment gap may not fully recover. The macula can develop irreversible damage during periods without treatment, which is why close monitoring remains critical even after stopping injections.
Optical coherence tomography imaging showing prolonged absence of fluid provides the best indication of disease stability. Doctors also consider treatment history, initial disease severity, and duration of disease quiescence. No single test perfectly predicts outcomes, making individualized assessment essential.
Most specialists recommend monthly or every-other-month examinations initially after stopping treatment. If the disease remains quiet, the interval may gradually extend to every three months. The schedule depends on individual risk factors and how long the disease has been inactive.
Medicare and most insurance plans cover medically necessary eye examinations and imaging for patients with diagnosed macular degeneration, regardless of current treatment status. However, coverage specifics vary by plan, so confirming benefits with your insurance provider is recommended.
The Bottom Line on Stopping Eye Injections
Macular degeneration injections represent a significant burden—nobody denies that. The treatments are uncomfortable, expensive, and time-consuming.
But for most patients with wet AMD, they’re also necessary to preserve vision. The evidence is clear: untreated wet macular degeneration typically progresses to severe vision loss.
That said, selected patients with prolonged disease stability may safely discontinue treatment under careful medical supervision. Approximately 30% fall into this category according to research from the National Eye Institute.
The critical factor? Never stop injections without discussing it with your retina specialist first. The decision requires thorough evaluation of your specific disease characteristics, treatment response, and risk factors.
If the treatment burden feels overwhelming, have an honest conversation with your doctor. Together, you can explore options like extended treatment intervals, medication switches, or in select cases, supervised treatment discontinuation with intensive monitoring.
Your vision is worth protecting. Make informed decisions based on your individual circumstances, current research, and expert medical guidance. Schedule regular appointments, communicate openly about challenges, and don’t let fear of injections prevent you from preserving the sight you have.