Quick Summary: Having sex with a yeast infection is technically possible but not recommended. Sexual activity can worsen symptoms, prolong healing time, and potentially cause discomfort or pain. According to the CDC, approximately 75% of women will experience at least one yeast infection episode in their lifetime, making this a common concern.
Yeast infections aren’t fun. The itching, burning, and thick discharge make you miserable enough without wondering whether intimacy is off the table completely.
But here’s the thing—people often want to know if sex is actually harmful during a yeast infection or just uncomfortable. The answer isn’t as simple as yes or no.
Understanding what happens to your body when you have sex during a yeast infection can help you make informed decisions about your sexual health and recovery.
Understanding Vaginal Yeast Infections
Vulvovaginal candidiasis (VVC) is caused primarily by Candida albicans, though other Candida species can occasionally be responsible. According to the CDC, this fungal infection affects an estimated 75% of women at least once in their lifetime, with 40%–45% experiencing two or more episodes.
The infection develops when the natural balance of yeast and bacteria in the vagina gets disrupted. Candida normally lives in the body harmlessly, but certain conditions trigger overgrowth.
Common symptoms include vaginal and vulvar itching, burning sensations, thick white discharge resembling cottage cheese, redness and swelling, and pain during urination or intercourse. Not everyone experiences all these symptoms, and they can vary in intensity.
What Actually Happens During Sex With a Yeast Infection
Technically, you can have sex with a yeast infection. But should you? That’s where things get complicated.
Sexual activity during an active infection creates several immediate effects on your body. The friction from intercourse irritates already inflamed vaginal tissues, intensifying burning and discomfort. Many women report that sex becomes genuinely painful rather than just uncomfortable.
The physical act can also spread the infection to different areas. What started as a vaginal infection might extend to the vulva or surrounding skin, expanding the affected area and complicating treatment.
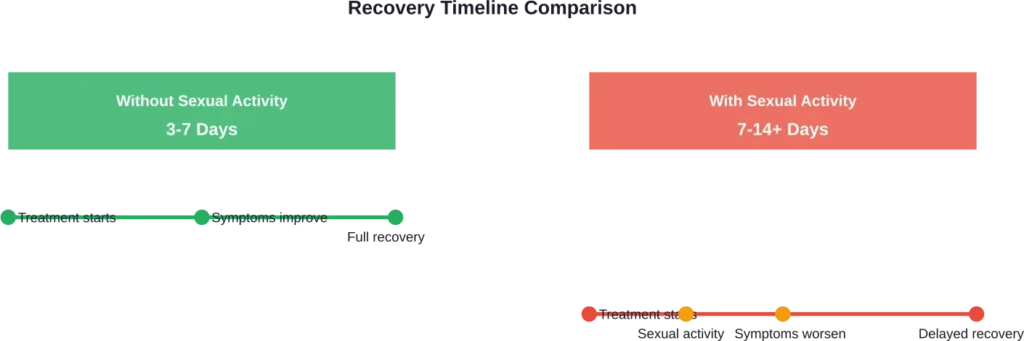
How Sex Affects Recovery Time
Here’s what many don’t realize—sex can significantly extend how long you’re dealing with symptoms. The irritation from intercourse disrupts the healing process, essentially setting back your recovery.
The vaginal environment needs time to restore its natural balance. Sexual activity during treatment interferes with this delicate process, potentially requiring additional treatment courses.
Can Your Partner Get Infected?
Yeast infections aren’t classified as sexually transmitted infections. The CDC notes that VVC develops due to internal imbalances rather than external transmission.
That said, transmission to partners can occur in certain situations. Male partners might develop symptoms like redness, itching, or a rash on the penis, though this is relatively uncommon. The risk increases with uncircumcised males.
Female partners in same-sex relationships can also potentially transmit yeast infections through sexual contact, though research on transmission rates in these partnerships remains limited.
Risks and Complications of Sexual Activity
Beyond discomfort and delayed healing, having sex with a yeast infection creates additional concerns.
The inflamed vaginal tissue becomes more susceptible to micro-tears during intercourse. These small injuries create entry points for other infections, potentially introducing bacteria and increasing the risk of secondary infections.
| Risk Factor | Impact Level | Description |
|---|---|---|
| Increased Pain | High | Friction irritates inflamed tissues |
| Delayed Healing | High | Disrupts natural recovery process |
| Symptom Worsening | Medium-High | Spreads infection to new areas |
| Partner Transmission | Low-Medium | Possible but not common |
| Secondary Infection | Medium | Tissue damage creates vulnerability |
Condoms and dental dams won’t prevent yeast transmission, though they do protect against actual STIs. Some antifungal treatments can also weaken latex barriers, reducing their effectiveness.
When It’s Safe to Resume Sexual Activity
So how long should you actually wait? The answer depends on your treatment and symptoms.
Most over-the-counter antifungal treatments are designed to work within three to seven days, though individual results vary. But symptom relief doesn’t automatically mean you’re ready for sex. The infection needs to fully clear, not just feel better.
Wait until all symptoms have completely resolved—no itching, no abnormal discharge, no burning. Then wait an additional 24-48 hours after your last symptom disappears. This ensures the treatment has fully worked and your vaginal environment has stabilized.
If you used prescription medication, follow your healthcare provider’s specific guidance on when sexual activity is safe.
Signs You’re Ready
Complete absence of itching or irritation, normal vaginal discharge (clear or white, thin consistency), no burning during urination, and no discomfort when inserting a tampon all indicate healing has completed.
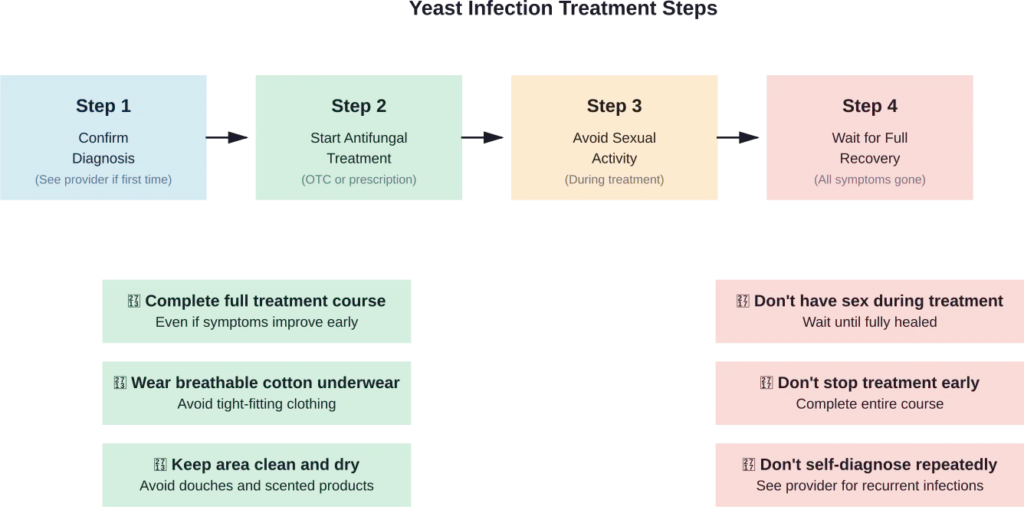
Treatment Options and Best Practices
According to the CDC, most healthy women with uncomplicated VVC can use over-the-counter antifungal medications. These come as creams, ointments, or suppositories applied for one, three, or seven days depending on the formulation.
Common active ingredients include miconazole, clotrimazole, and tioconazole. The treatment duration varies by product strength, not effectiveness—single-dose treatments aren’t necessarily better than seven-day courses.
For recurrent infections (defined as more than three episodes per year), prescription treatments become necessary. Healthcare providers typically recommend longer treatment courses for recurrent VVC.
Frequently Asked Questions
Yeast infections aren’t sexually transmitted infections. They develop from an overgrowth of Candida that already lives in your body. However, sexual activity can sometimes trigger an infection by disrupting vaginal pH balance or introducing bacteria.
Wait until all symptoms have completely disappeared, then an additional 24-48 hours. Most treatments work within three to seven days, but individual healing times vary. Complete symptom resolution is essential before resuming sexual activity.
Yes. Sexual activity during an active infection worsens symptoms, spreads the infection to new areas, delays healing, and can cause significant pain or discomfort. The friction from intercourse irritates already inflamed tissues.
Men can develop yeast infections, though it’s less common. Symptoms include redness, itching, and rash on the penis. Uncircumcised men face higher risk. While transmission can occur, most male yeast infections develop from other causes.
Generally, partner treatment isn’t necessary unless they develop symptoms. Unlike bacterial vaginosis where the American College of Obstetricians and Gynecologists recommends considering concurrent sexual partner therapy for recurrent cases, standard yeast infection protocol doesn’t require treating asymptomatic partners.
If symptoms persist after completing over-the-counter treatment, contact a healthcare provider. You might have a different type of infection, a resistant Candida strain, or recurrent VVC requiring prescription medication. Never self-diagnose repeatedly.
Tampons are generally safe but might increase discomfort. Many women prefer pads during treatment. If you’re menstruating while treating a yeast infection, change tampons frequently and consider switching to pads if irritation worsens.
The Bottom Line on Sex and Yeast Infections
While technically possible, having sex with a yeast infection creates more problems than it solves. The discomfort isn’t worth it, and you’re actively working against your recovery.
Give your body the time it needs to heal completely. Most treatments resolve infections within a week, and waiting those few extra days prevents weeks of prolonged symptoms.
If you’re experiencing frequent yeast infections or symptoms that don’t respond to over-the-counter treatment, consult a healthcare provider. Recurrent infections might indicate underlying health issues that need addressing.
Your sexual health matters. Making informed decisions about when to abstain and when it’s safe to resume intimacy protects both you and your partner.
