Quick Summary: Waiting 6 weeks after birth allows the cervix to close, bleeding to stop, and tears or incisions to heal, reducing infection risk and complications. Resuming sex, exercise, or inserting tampons too early can cause hemorrhage, endometritis, or delayed healing. However, every recovery is different—some need longer, while low-impact activities may be safe earlier with medical clearance.
The six-week postpartum checkpoint isn’t arbitrary. It’s rooted in how the body heals after pregnancy and childbirth.
But what actually happens if you don’t wait? And is the rule the same for everyone?
Here’s what the research shows—and what medical professionals want new mothers to understand about postpartum recovery.
Why the 6-Week Waiting Period Exists
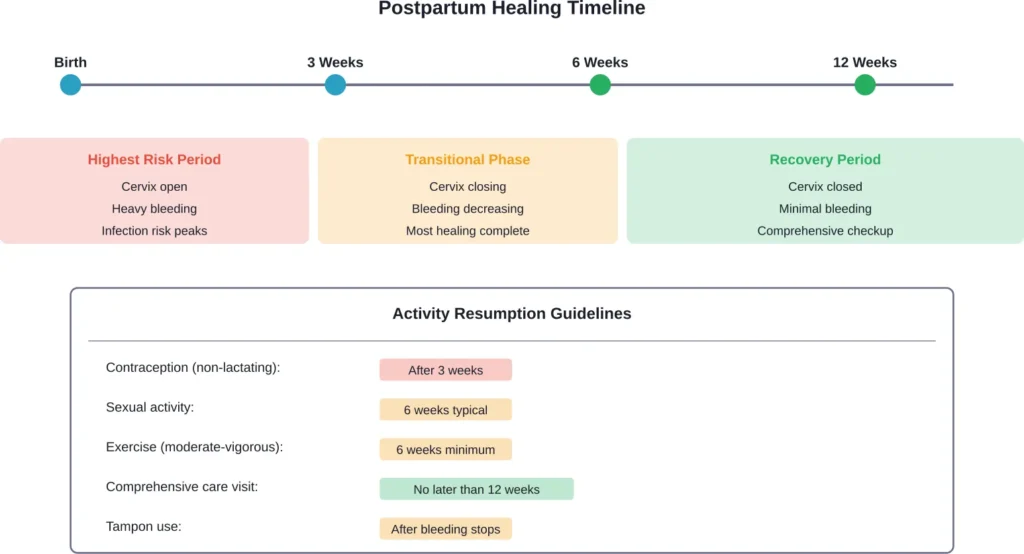
After delivery, the body undergoes significant physiological changes. The uterus shrinks back to its pre-pregnancy size. The cervix closes. Vaginal bleeding gradually stops. Tears or surgical incisions heal.
These processes don’t happen overnight.
According to the American College of Obstetricians and Gynecologists (ACOG), the traditional six-week postpartum visit serves as a checkpoint to ensure these healing processes are progressing normally. ACOG recommends ongoing postpartum care concluding with a comprehensive well-woman visit no later than 12 weeks after birth.
The six-week mark represents when most—but not all—women have healed enough to safely resume certain activities.
What’s Actually Healing During Those 6 Weeks
The postpartum period involves multiple healing processes happening simultaneously:
- Uterine involution: The uterus contracts back from watermelon-size to its normal pear-like dimensions
- Cervical closure: The open cervix gradually closes, creating a protective barrier against infection
- Lochia resolution: Vaginal bleeding and discharge decrease as the uterine lining sheds and heals
- Perineal healing: Tears, episiotomies, or C-section incisions close and tissue regenerates
- Hormonal adjustment: In the first 24 hours after childbirth, hormone levels quickly drop back to normal, pre-pregnancy levels, according to Women’s Health.gov
Each of these processes has its own timeline. And complications during delivery can extend healing time significantly.
Risks of Not Waiting: What the Research Shows
Studies examining early postpartum activity resumption reveal specific risks that increase when the six-week guideline isn’t followed.
Infection Risk
The most immediate concern is infection. With an open cervix and healing uterine lining, the risk of bacteria entering the reproductive tract is substantially higher.
Postpartum endometritis—infection of the uterine lining—can develop when bacteria enter through the cervix before it fully closes. According to ACOG, this condition can occur up to 12 weeks after delivery and requires prompt treatment to prevent serious complications.
Symptoms include fever, foul-smelling discharge, and pelvic pain. Without treatment, endometritis can lead to sepsis or other life-threatening conditions.
Hemorrhage
Postpartum hemorrhage typically occurs within 24 hours of delivery, but it can happen up to 12 weeks later, according to ACOG.
Activities that increase blood flow to the pelvic region—including sexual intercourse or vigorous exercise—can trigger bleeding in women whose bodies haven’t fully healed. The risk is particularly elevated for women who experienced complications during delivery.
According to ACOG, postpartum hemorrhage means soaking through two pads an hour for more than one to two hours. This constitutes a medical emergency.
Delayed Healing and Tissue Damage
Perineal tears and surgical incisions need time to develop tensile strength. Early disruption of healing tissue can cause:
- Wound dehiscence (reopening of stitches)
- Increased scar tissue formation
- Chronic pain
- Pelvic floor dysfunction
Research in the American Journal of Obstetrics and Gynecology examined early postpartum physical activity and pelvic floor outcomes, finding mean moderate-to-vigorous physical activity was 57.3 minutes per day at 2-3 weeks postpartum and 68.1 minutes per day at 5-6 weeks. One year postpartum, 54.2% met criteria for pelvic floor symptom burden.
Unintended Pregnancy
Here’s something many don’t realize: ovulation can resume before menstruation returns.
According to medical guidelines, non-lactating mothers should use contraceptive measures after 3 weeks, and lactating mothers after 3 months of delivery. Breastfeeding isn’t reliable contraception—the lactational amenorrhea method has a 2% failure rate even when specific criteria are met.
Women who resume sexual activity before discussing contraception with their healthcare provider risk closely spaced pregnancies, which carry their own health risks.
Sexual Activity: The Most Common Question
The six-week guideline for resuming sexual activity gets the most attention—and generates the most questions.
Why Wait for Sex Specifically?
Sexual intercourse poses unique risks during early postpartum recovery:
- Bacteria introduction through an open cervix
- Mechanical stress on healing perineal tissue
- Increased pelvic blood flow potentially triggering bleeding
- Risk of pregnancy before contraception is established
A cross-sectional study in China published in BMJ Open examined postpartum sexual resumption patterns. The research found significant variation in when women resumed sexual activity and emphasized the importance of contraceptive counseling, as many women resumed intercourse before establishing birth control.
What Studies Show About Early Resumption
Research from Ethiopia published in PLoS One examined early postpartum sexual resumption and associated risk factors. The study documented that resuming sexual activity before six weeks occurred among a notable percentage of postpartum women, with various factors influencing timing.
Another study in Frontiers in Medicine found that women who returned to sexual activity within six weeks postpartum often did so without adequate contraceptive counseling, increasing the risk of unintended pregnancy.
The research consistently emphasizes that early resumption without medical guidance and contraception poses risks.
When Some Women Resume Earlier
Despite medical guidelines, some women do resume sexual activity before six weeks. Community discussions on platforms like Reddit reveal varied experiences.
Some report no complications. Others describe pain, bleeding, or emotional discomfort. The difference often comes down to individual healing rates, delivery complications, and whether proper precautions were taken.
But here’s the thing: the absence of immediate complications doesn’t mean the activity was medically safe. Some consequences—like increased infection risk or tissue damage—may not be immediately apparent.
Exercise and Physical Activity
Physical activity recommendations are more nuanced than the blanket “wait six weeks” advice suggests.
Low-Impact vs. High-Impact Activities
Not all exercise carries the same risk. Walking, for example, can typically begin soon after delivery if there are no complications. The CDC emphasizes the importance of physical activity for postpartum health, but timing and intensity matter.
Research in the American Journal of Obstetrics and Gynecology examined early postpartum physical activity and pelvic floor outcomes. The study found that mean moderate-to-vigorous physical activity was 57.3 minutes per day at 2-3 weeks postpartum and 68.1 minutes per day at 5-6 weeks.
One year postpartum, 9.4% of participants showed worse vaginal support, and 54.2% met criteria for pelvic floor symptom burden. However, the relationship between early activity and later symptoms was complex, with multiple contributing factors.
Activities to Avoid Early Postpartum
Certain activities pose higher risks during early recovery:
- High-impact aerobics or running
- Heavy weightlifting
- Core exercises that increase intra-abdominal pressure
- Swimming (while still bleeding, due to infection risk)
- Contact sports
These activities can strain healing tissues, increase bleeding risk, or compromise pelvic floor recovery.
Other Activities Requiring Caution
Tampon Use
Tampons or menstrual cups shouldn’t be used while lochia continues. Inserting anything into the vagina while the cervix is open and the uterus is healing increases infection risk.
Most healthcare providers recommend waiting until bleeding has completely stopped—typically four to six weeks postpartum—before using internal menstrual products.
Bathing
Submerging in bathtubs, hot tubs, or pools carries infection risk during active bleeding. Showers are generally safe immediately after delivery, but full immersion should wait until bleeding stops and any incisions are healed.
Lifting and Carrying
Particularly after cesarean delivery, lifting restrictions protect healing abdominal muscles and incisions. Most providers recommend nothing heavier than the baby for several weeks.
| Activity | Typical Waiting Period | Primary Concern |
|---|---|---|
| Sexual intercourse | 6 weeks (minimum) | Infection, hemorrhage, pregnancy |
| Tampon use | Until bleeding stops | Infection risk |
| Swimming/bathing | Until bleeding stops | Infection risk |
| Vigorous exercise | 6 weeks (minimum) | Pelvic floor damage, bleeding |
| Heavy lifting (C-section) | 6-8 weeks | Incision dehiscence |
| Driving (C-section) | 1-2 weeks or when off pain meds | Reaction time, incision protection |
Individual Variation: Why Some Need More Time
The six-week guideline represents an average. Many women need substantially longer to heal completely.
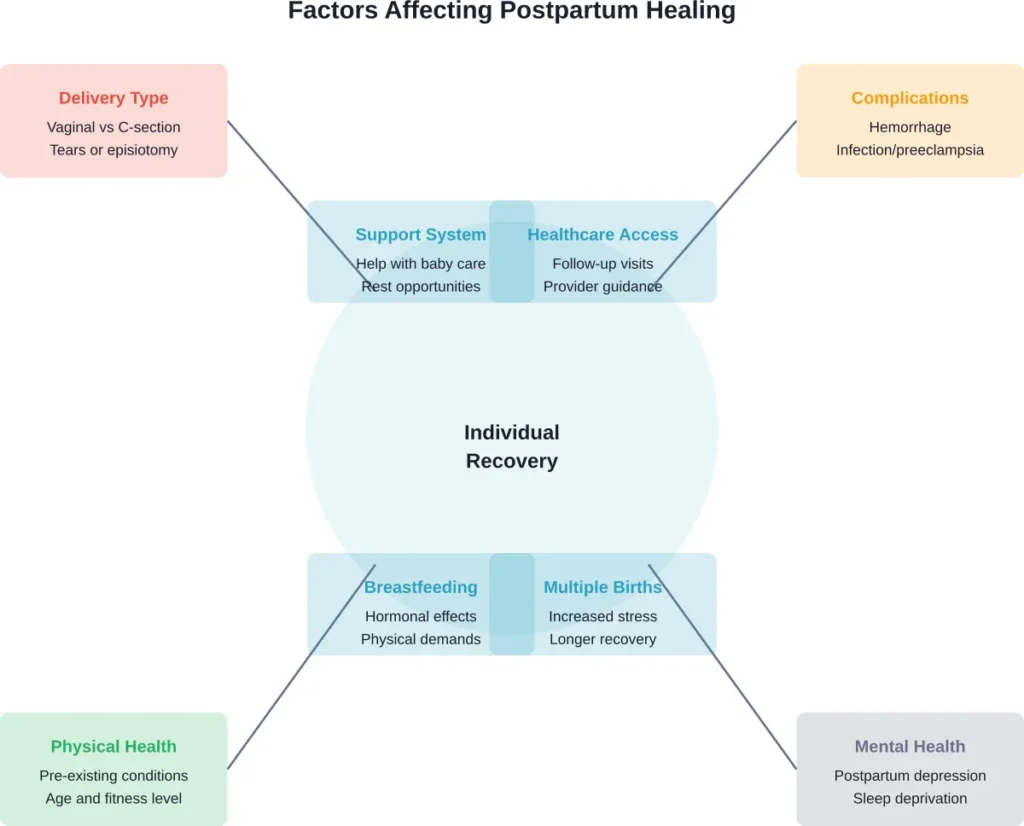
Factors That Extend Healing Time
Several conditions can delay postpartum recovery:
- Complicated vaginal delivery: Third or fourth-degree tears require extended healing
- Cesarean section: Major abdominal surgery necessitates longer recovery
- Postpartum complications: Hemorrhage, infection, or preeclampsia delay healing
- Multiple births: Twins or triplets increase physical stress
- Pre-existing conditions: Diabetes, hypertension, or obesity can slow healing
According to a systematic review in the European Journal of Midwifery, the percentage of women experiencing one or more postpartum health problems varies significantly, with many issues persisting beyond six weeks.
Mental Health Considerations
Physical healing isn’t the only consideration. Mental and emotional readiness matter too.
Research shows that less than half of pregnant women with depression receive the treatment they need, and 30% of women are not asked about symptoms of depression during a prenatal or postpartum checkup.
Postpartum depression is a serious mental health condition that affects many women. Sexual desire, relationship dynamics, and emotional well-being all influence when—and whether—resuming certain activities feels right.
Research indicates that a sexual function score of <26.55 is considered as a risk factor for postpartum depression.
Signs You’re Not Ready—Regardless of Timeline
Certain symptoms indicate the body needs more healing time, even if six weeks have passed:
- Ongoing vaginal bleeding heavier than light spotting
- Severe pain during attempted activity
- Foul-smelling discharge
- Fever or chills
- Redness, swelling, or discharge from incisions
- Persistent pelvic pain or pressure
Any of these warrant immediate consultation with a healthcare provider before resuming normal activities.
When Early Activity Might Be Okay
In some cases, certain activities may be safe earlier than six weeks—but only with explicit medical clearance.
Women with uncomplicated vaginal deliveries, minimal tearing, and no complications may receive approval for some activities earlier. This is particularly true for low-impact exercise like walking.
But “may be okay” and “is definitely safe” are different things. Individual assessment by a healthcare provider who knows your specific delivery and recovery is essential.
The Importance of Communication
Rather than following internet timelines or community anecdotes, direct communication with healthcare providers offers personalized guidance based on actual healing progress.
ACOG’s updated postpartum care guidelines emphasize ongoing contact rather than a single six-week visit. This approach allows providers to assess healing and give activity-specific guidance as recovery progresses.
What to Expect at Postpartum Checkups
The comprehensive postpartum visit assesses multiple aspects of recovery:
- Physical examination of healing tissues
- Blood pressure and other vital signs
- Emotional well-being screening
- Contraception discussion
- Breastfeeding support
- Sleep and fatigue assessment
- Activity resumption guidance
This visit provides the opportunity to ask specific questions about when particular activities are safe based on individual healing.
Long-Term Considerations
The postpartum period doesn’t end at six weeks. The postpartum period is divided into 3 arbitrary phases: the acute phase (the first 24 hours after delivery of the placenta), early (up to 7 days), and late (up to 6 weeks to 6 months).
Long-term postpartum health issues can persist or develop months after delivery. These include:
- Pelvic floor dysfunction
- Persistent perineal pain
- Sexual dysfunction
- Postpartum depression (which can develop up to one year after birth)
- Cardiovascular changes
Gestational diabetes increases risk for type 2 diabetes. Gestational diabetes may also increase risk for postpartum depression, according to the CDC.
Frequently Asked Questions
Feeling physically comfortable doesn’t necessarily mean internal healing is complete. The cervix may still be open, and the uterine lining may still be healing even without pain or visible symptoms. Early resumption increases infection and hemorrhage risk. Medical clearance is essential.
A single incident may not cause problems, but it increases the risk of incision dehiscence (reopening), hernia formation, or increased pain. If you experience sudden pain, swelling, discharge, or visible changes to the incision after lifting, contact your healthcare provider immediately.
Short walks are generally encouraged soon after delivery to promote circulation and prevent blood clots. However, “walking” means gentle, brief movement—not vigorous exercise. Listen to your body, and stop if you experience increased bleeding, pain, or dizziness.
Yes. Ovulation can occur before menstruation returns, making pregnancy possible even without a period. Non-lactating women should use contraception after 3 weeks, while lactating women should begin after 3 months, according to StatPearls.
Warning signs include fever over 100.4°F, foul-smelling vaginal discharge, severe abdominal pain, redness or swelling around incisions, and flu-like symptoms. Postpartum infections require prompt medical treatment and can become life-threatening if ignored.
Breastfeeding influences hormones, which can affect vaginal dryness, libido, and tissue healing. It doesn’t necessarily change the six-week guideline, but it may affect comfort levels. Breastfeeding isn’t reliable contraception despite common myths.
Light spotting can be normal at six weeks, but anything heavier warrants evaluation. Persistent heavy bleeding may indicate retained placental tissue, infection, or other complications requiring treatment. Don’t resume sexual activity or use tampons if bleeding continues.
The Bottom Line
The six-week postpartum guideline exists because it represents the minimum time most women need for essential healing processes to occur. Not waiting increases measurable risks: infection, hemorrhage, tissue damage, and unintended pregnancy.
But six weeks isn’t universal. Some women need longer. Some activities carry different risk profiles than others. And individual factors—delivery type, complications, pre-existing conditions, mental health—all influence appropriate timing.
The best approach? Open communication with healthcare providers who can assess individual healing and provide personalized guidance. Generic timelines provide a starting point, but medical evaluation determines when activities are actually safe for each woman.
Postpartum recovery isn’t a race. There’s no prize for resuming activities earliest. Prioritizing complete healing sets the foundation for long-term health—for both mother and baby.
Schedule that comprehensive postpartum visit. Ask specific questions. And give your body the time it actually needs to heal, regardless of arbitrary timelines or social pressure.
