Quick Summary: Plan B works primarily by delaying or preventing ovulation. If ovulation has already occurred when Plan B is taken, it cannot prevent pregnancy because it doesn’t stop fertilization or implantation. Timing matters critically—the pill is most effective when taken before the egg is released, but offers little to no protection once ovulation has already happened.
There’s a lot of confusion about emergency contraception. Most people know Plan B as the “morning-after pill” that prevents pregnancy after unprotected sex. But here’s the thing—timing isn’t just about how quickly you take it after sex. It’s also about where you are in your menstrual cycle.
If you’ve already ovulated before taking Plan B, the pill won’t be effective. This is a critical piece of information that doesn’t always get communicated clearly, leaving many people wondering why emergency contraception might fail.
Let’s break down exactly what happens when Plan B is taken after ovulation, why it won’t work, and what alternatives exist.
How Plan B Actually Works
Plan B contains levonorgestrel, a synthetic hormone that prevents pregnancy through a specific mechanism. According to the NIH, levonorgestrel is FDA-approved to be used within 72 hours of unprotected sexual intercourse or when a presumed contraceptive failure has occurred.
But what does it actually do?
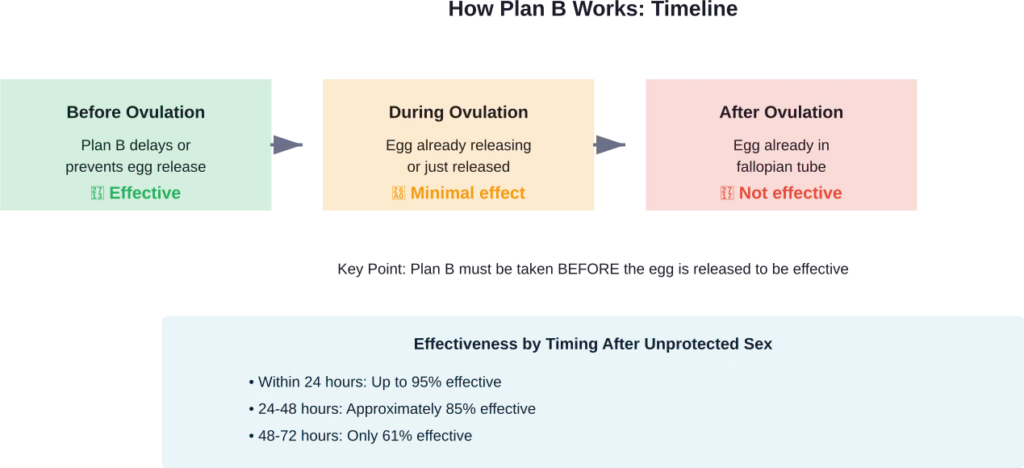
The primary mechanism is delaying or preventing ovulation. When the medication enters the system before ovulation occurs, it temporarily stops the ovaries from releasing an egg. No egg means sperm has nothing to fertilize, and pregnancy can’t happen.
Plan B may also thicken cervical mucus, making it harder for sperm to reach an egg. Some sources suggest it might affect the uterine lining, though research on this mechanism remains debated within the medical community.
Here’s what Plan B does NOT do: it doesn’t prevent fertilization if the egg has already been released. It doesn’t stop implantation of a fertilized egg. And it definitely won’t terminate an existing pregnancy.
The Ovulation Problem
Ovulation typically happens around day 14 of a 28-day cycle, though this varies significantly between individuals. When ovulation occurs, an egg is released from the ovary into the fallopian tube, where it can survive for 12-24 hours.
Sperm, on the other hand, can live inside the female reproductive tract for up to five days.
This creates a fertility window—the days when pregnancy can occur. If unprotected sex happens during this window and ovulation has already occurred or is about to occur, Plan B faces a serious limitation.
The pill can’t pull back an egg that’s already been released. Once ovulation happens, that egg is available for fertilization. Plan B doesn’t prevent sperm from reaching the egg, and it doesn’t prevent fertilization from occurring.
Discussions on community platforms frequently highlight this misunderstanding, with some users reporting taking Plan B during their fertile window without realizing that if ovulation had already occurred, the medication would not prevent pregnancy.
So what happens if ovulation has already occurred?
Simply put: Plan B won’t work. The egg is already there, waiting. If sperm reaches it within that 12-24 hour window, fertilization can occur, and pregnancy becomes possible.
Effectiveness Rates and What They Really Mean
The numbers often cited for Plan B can be misleading without context. Plan B is often said to be 87% effective at preventing pregnancy when taken as directed, though effectiveness varies significantly by timing. But that effectiveness drops dramatically based on timing.
According to medical sources, effectiveness within the first 24 hours following unprotected sex can reach up to 95%. But this assumes ovulation hasn’t occurred yet. Between 48 and 72 hours later, effectiveness plummets to only 61%.
Why the drop?
Partly because of natural delays in taking the medication. But also because the longer the time between intercourse and taking Plan B, the higher the chance that ovulation has already happened or will happen before the medication can work.
| Timing After Sex | Effectiveness Rate | Key Factor |
|---|---|---|
| 0-24 hours | Up to 95% | Highest chance of preventing ovulation |
| 24-48 hours | ~85% | Still effective if ovulation hasn’t occurred |
| 48-72 hours | ~61% | Significantly reduced effectiveness |
| After ovulation | Minimal to 0% | Cannot prevent pregnancy once egg is released |
Another factor: body weight. Research suggests Plan B may be less effective for individuals weighing over 165-175 lbs (the threshold cited varies slightly in literature). The medication’s concentration in the body may not be sufficient at higher body weights to effectively delay ovulation.
Signs You Might Have Already Ovulated
Recognizing ovulation can help determine whether Plan B will be effective. While ovulation itself happens quickly, there are signs that indicate it’s occurring or has just occurred.
Common ovulation symptoms include:
- Changes in cervical mucus (clear, stretchy, similar to egg whites)
- Mild cramping or pain on one side of the lower abdomen
- Slight increase in basal body temperature
- Increased sex drive
- Breast tenderness
- Bloating
If unprotected sex occurred and these signs were present at the time, there’s a higher likelihood that ovulation was happening or had just happened. In that scenario, Plan B’s effectiveness is severely limited.
Ovulation predictor kits can identify the luteinizing hormone (LH) surge that occurs 24-36 hours before ovulation. But by the time someone is considering emergency contraception, that information is retrospective.
Real talk: most people don’t track their cycles closely enough to know exactly when they ovulate. That’s completely normal. But it does mean that taking Plan B always carries some uncertainty about whether the timing will work in its favor.
Alternative Emergency Contraception Options
If ovulation has likely occurred or is occurring, other emergency contraception methods may be more effective than Plan B.
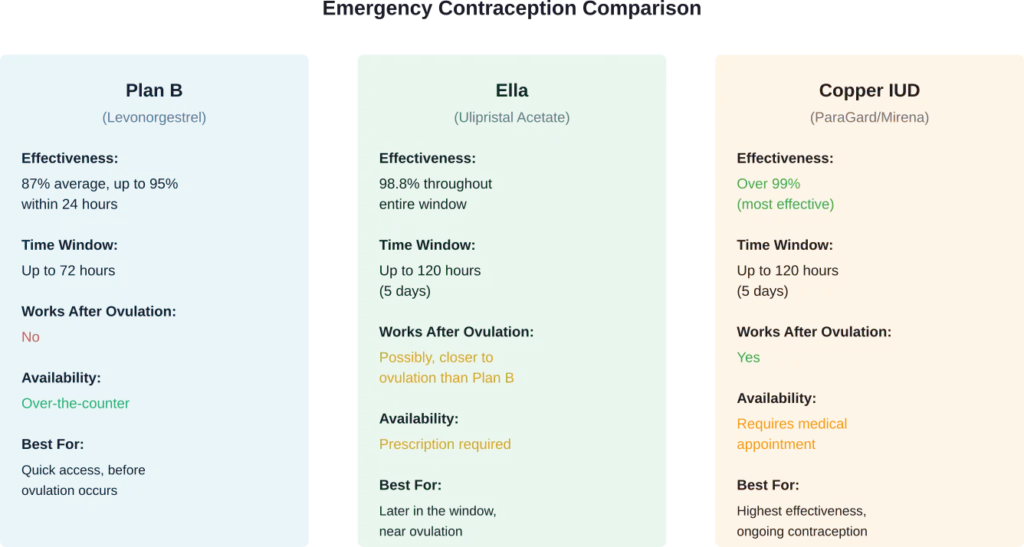
Ella (Ulipristal Acetate)
Ella is another emergency contraceptive pill, but it works differently than levonorgestrel-based options. Ulipristal acetate can delay ovulation even when LH levels are beginning to rise—meaning it works closer to the actual moment of ovulation.
According to medical sources, ella is reported to maintain 98.8% effectiveness and can be taken up to 120 hours (five days) after unprotected sex. It’s more effective than Plan B, particularly in the 72-120 hour window.
However, ella requires a prescription. It’s not available over-the-counter like Plan B.
Copper IUD
The copper intrauterine device is the most effective form of emergency contraception. A copper IUD inserted within 120 hours (5 days) after unprotected sex is more than 99% effective at preventing pregnancy, according to the World Health Organization.
Unlike oral emergency contraception, the copper IUD works even after ovulation has occurred. The copper creates an environment that’s toxic to sperm and eggs, preventing fertilization. If fertilization has already occurred, it prevents implantation.
The copper IUD also provides ongoing contraception for up to 10-12 years, depending on the product, making it a dual-purpose option.
The drawback? It requires a medical appointment and insertion procedure, which may not be immediately accessible.
What To Do If You Think Plan B Failed
The only definitive way to know whether Plan B worked is through a pregnancy test. But pregnancy tests won’t be accurate immediately after taking emergency contraception.
Most home pregnancy tests detect the hormone hCG (human chorionic gonadotropin), which only appears after implantation occurs—typically 6-12 days after fertilization.
For the most accurate results, wait at least 3 weeks after unprotected sex before testing. Testing too early can result in false negatives.
Signs that Plan B may not have worked include:
- A missed period (more than a week late)
- Unusual spotting or bleeding patterns
- Early pregnancy symptoms (nausea, breast tenderness, fatigue)
- Cramping that feels different from normal period cramps
But here’s where it gets tricky: Plan B itself can cause side effects that mimic early pregnancy or disrupt normal cycles. Nausea, breast tenderness, irregular bleeding, and delayed periods are all common after taking levonorgestrel.
So symptoms alone aren’t reliable indicators.
If a period is more than a week late after taking Plan B, take a pregnancy test. If the test is positive or uncertainty remains, consult a healthcare provider for confirmation and to discuss options.
Common Misconceptions About Plan B
Misinformation about emergency contraception circulates widely. Let’s clear up some persistent myths.
Myth: Plan B is an abortion pill
Plan B does not terminate an existing pregnancy. It works by preventing pregnancy from occurring in the first place. If implantation has already happened, Plan B has no effect.
The abortion pill (mifepristone and misoprostol) is a completely different medication used to end an established pregnancy.
Myth: Taking Plan B multiple times causes infertility
There’s no evidence that repeated use of Plan B causes long-term fertility problems. Fertility returns quickly after taking the medication—there’s no delay or lasting impact on the ability to conceive in the future.
That said, Plan B isn’t intended as regular contraception. It’s less effective than ongoing birth control methods and causes more side effects.
Myth: Plan B works at any point in the cycle
As we’ve established, Plan B’s effectiveness depends heavily on cycle timing. It won’t prevent pregnancy if ovulation has already occurred.
Myth: Plan B protects against future intercourse
Plan B only works for sex that happened before taking the pill. It doesn’t provide any protection for intercourse that occurs afterward. If unprotected sex happens again after taking Plan B, another dose may be needed, or alternative contraception should be used.
Who Should Not Take Plan B
While Plan B is generally safe for most people, certain situations warrant caution or alternative options.
Plan B may be less effective for individuals:
- Weighing over 165-175 pounds (ella or copper IUD may be better options)
- Who have already ovulated (copper IUD is the only effective emergency contraception at this point)
- Taking certain medications that interfere with levonorgestrel (some anticonvulsants, St. John’s Wort, certain HIV medications)
Plan B is not recommended if:
- Pregnancy has already been confirmed (it won’t harm an existing pregnancy but won’t be effective either)
- There’s an allergy to levonorgestrel or other ingredients
Plan B doesn’t protect against sexually transmitted infections. If there’s concern about STI exposure, testing and appropriate treatment should be sought regardless of pregnancy prevention measures.
Side Effects and What to Expect
Most people tolerate Plan B well, but side effects can occur. Common ones include:
- Nausea and vomiting
- Fatigue
- Headache
- Dizziness
- Breast tenderness
- Irregular bleeding or spotting
- Changes to the next period (earlier, later, heavier, or lighter than usual)
These side effects typically resolve within a few days. If vomiting occurs within two hours of taking Plan B, the dose may not have been fully absorbed, and another dose may be needed.
Period changes are particularly common. The next period might arrive a few days early or up to a week late. The flow might be heavier or lighter than normal. This is a temporary disruption, and cycles typically return to normal afterward.
The Bigger Picture: Regular Contraception
Emergency contraception fills a critical gap when regular birth control fails or isn’t used. But it’s not a substitute for ongoing contraception.
For those who are sexually active and want to prevent pregnancy, regular contraception is more effective, more reliable, and easier on the body than repeated use of emergency contraception.
Options include:
- Combined oral contraceptives (the pill)
- Progestin-only pills (the mini-pill)
- Contraceptive patch
- Vaginal ring
- Injectable contraception (Depo-Provera)
- Implant (Nexplanon)
- IUDs (hormonal or copper)
- Barrier methods (condoms, diaphragm)
- Fertility awareness methods
Each method has different effectiveness rates, benefits, and considerations. According to the World Health Organization, IUDs are among the most effective reversible contraception, with fewer than 1 pregnancy per 100 women in the first year of use.
With typical use, only 4 to 7 pregnancies occur in 100 women using the pill per year, while perfect use brings that down to less than 1 per 100.
The right contraception depends on individual health, lifestyle, preferences, and medical history. A healthcare provider can help navigate the options.
Frequently Asked Questions
Plan B can be taken at any point in the cycle, but it won’t be effective if ovulation has already occurred. The medication works by preventing or delaying ovulation, so once the egg has been released, Plan B cannot prevent pregnancy. If ovulation has likely occurred, a copper IUD is the only emergency contraception option that remains effective.
Signs of ovulation include clear, stretchy cervical mucus, mild cramping on one side, slight temperature increase, and increased libido. Ovulation predictor kits detect the LH surge that occurs 24-36 hours before ovulation. For most people with regular cycles, ovulation occurs around day 14, but this varies. Without tracking, it’s difficult to know for certain whether ovulation has occurred.
Plan B’s effectiveness depends on timing. When taken within 24 hours of unprotected sex and before ovulation, effectiveness reaches up to 95%. Between 24-48 hours, it drops to approximately 85%. Between 48-72 hours, effectiveness is only around 61%. Overall effectiveness is often cited as 87%, but this assumes the pill is taken before ovulation occurs.
Research suggests Plan B may be less effective for individuals weighing over 165-175 pounds. The medication concentration may not be sufficient to effectively delay ovulation at higher body weights. Ella or a copper IUD are recommended as more reliable emergency contraception options for those in this weight range.
Plan B can be taken more than once, even within the same menstrual cycle, though it’s not ideal. Repeated use can cause more significant cycle disruptions and side effects. It’s less effective than regular contraception and should only be used for emergencies. If emergency contraception is needed frequently, it’s worth exploring ongoing birth control options.
Plan B can delay ovulation by approximately 5-7 days. This is typically long enough for sperm to die off, as sperm can survive in the reproductive tract for up to 5 days. However, if ovulation is delayed rather than prevented entirely, pregnancy could still occur from intercourse that happens after taking Plan B.
Wait at least 3 weeks after unprotected sex before taking a pregnancy test for the most accurate results. Testing earlier can result in false negatives because the pregnancy hormone hCG may not be detectable yet. If a period is more than a week late after taking Plan B, take a pregnancy test or consult a healthcare provider.
Final Thoughts
Understanding how Plan B works—and when it doesn’t—is essential for making informed decisions about emergency contraception. The medication is a valuable tool when used appropriately, but its effectiveness hinges on timing relative to ovulation.
If ovulation has already occurred, Plan B won’t prevent pregnancy. In that situation, a copper IUD is the only effective emergency contraception option.
For anyone who finds themselves needing emergency contraception repeatedly, it’s worth having a conversation with a healthcare provider about more reliable, ongoing contraception methods. Emergency contraception serves a purpose, but regular birth control offers better protection with fewer disruptions.
When in doubt about whether emergency contraception worked, wait the appropriate time and take a pregnancy test. And remember: emergency contraception doesn’t protect against STIs. If there’s any concern about exposure, get tested.
Knowledge is power when it comes to reproductive health. Understanding the science behind emergency contraception helps navigate these situations with confidence and clarity.
