Quick Summary: Staying up all night causes immediate cognitive impairment comparable to alcohol intoxication, including reduced reaction time, impaired judgment, and mood disturbances. After 24 hours without sleep, the brain experiences decreased metabolic activity in the prefrontal cortex, affecting attention, memory, and decision-making. While occasional all-nighters won’t cause permanent damage, chronic sleep deprivation increases risk for obesity, diabetes, cardiovascular disease, and mental health disorders.
Everyone has pulled an all-nighter at some point. Whether it’s cramming for an exam, finishing a work deadline, meeting a flight schedule, or binge-watching a series that’s just too good to stop, staying up all night feels manageable in the moment.
But here’s the thing: your body doesn’t treat sleep as optional. According to NIOSH (CDC), sleep is a biological need similar to food and water, essential for proper mental and physical functioning. When you skip an entire night of sleep, the consequences extend far beyond feeling tired the next day.
So what actually happens to your brain and body when you stay awake for 24 hours or longer? Research from the National Institutes of Health reveals a cascade of physiological and cognitive changes that begin within hours and intensify with each passing moment of wakefulness.
What Defines an All-Nighter
An all-nighter typically means staying awake for 24 consecutive hours or more, completely skipping a normal night’s sleep. This differs from simply getting insufficient sleep—you’re not getting reduced hours; you’re getting none.
Most adults need 7 to 8 hours of good-quality sleep every 24 hours to maintain optimal performance. When you lose sleep, you accumulate what sleep researchers call sleep debt. For example, if you lose 2 hours of sleep each night, you’ll have a sleep debt of 14 hours after a week. But an all-nighter creates an immediate, substantial deficit.
People pull all-nighters for various reasons: academic deadlines, work emergencies, shift work requirements, travel across time zones, or social activities. Some do it by choice; others have no alternative. Regardless of the reason, the biological impact remains the same.
The First 24 Hours Without Sleep
Missing 24 hours of sleep won’t cause major long-term health problems for most people, but the immediate effects are substantial and measurable.
Cognitive Impairment Comparable to Intoxication
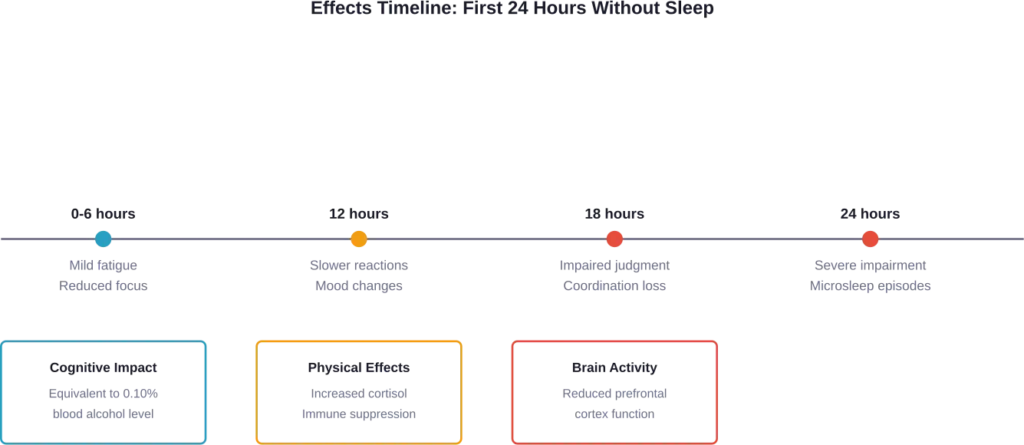
Research shows that staying awake for 24 hours can impair speed and reaction times comparable to alcohol intoxication. Your cognitive performance deteriorates progressively, with noticeable declines in alertness, attention, and executive function.
According to research using PET imaging, 24 hours of sleep deprivation significantly reduces metabolic activity in the prefrontal cortex. This brain region controls decision-making, problem-solving, and impulse control. When it’s compromised, your judgment suffers.
You’ll likely feel tired, exhausted, or simply “off.” Tasks that normally seem straightforward become challenging. Your ability to concentrate diminishes, and you may find yourself reading the same sentence multiple times without comprehension.
Physical Symptoms Begin
Beyond mental fog, physical symptoms emerge relatively quickly. Your coordination suffers, making activities like driving genuinely dangerous. Sleep deprivation-related drowsy driving has been identified as a causal factor in vehicle crashes, with sleep-deprived drivers exhibiting impairment similar to drunk drivers.
Other physical manifestations include increased appetite (particularly for high-calorie foods), slight tremors, and reduced immune function. Your body starts producing stress hormones like cortisol at elevated levels, preparing for what it perceives as an emergency situation.
Mood and Emotional Regulation Decline
Sleep deprivation impairs mood and communication skills significantly. According to NIOSH research on shift workers, sleep-deprived individuals commonly experience irritability, anxiety, and symptoms of depression.
You might view interactions more negatively than you normally would, avoiding communication with difficult colleagues or family members. Confusion, reduced vigor, and fatigue at inappropriate times become increasingly common as the day progresses.
Beyond 24 Hours: The Stages of Sleep Deprivation
The symptoms of sleep deprivation intensify dramatically as you push beyond the 24-hour mark. Sleep researchers have identified distinct stages based on duration of wakefulness.
36-48 Hours: Severe Cognitive Decline
After a day and a half without sleep, cognitive functions deteriorate substantially. Attention span shrinks to near zero for complex tasks. Memory formation becomes severely impaired—you might have conversations you won’t remember later.
Microsleep episodes begin occurring. These are brief moments (lasting fractions of a second to 30 seconds) where your brain essentially shuts down without your conscious awareness. During a microsleep, you’re effectively asleep even though your eyes might be open. This is extraordinarily dangerous during activities like driving.
Emotional regulation becomes increasingly difficult. Irritability intensifies, and stress responses become exaggerated. Small problems feel overwhelming.
72 Hours: Perceptual Distortions and Hallucinations
At the three-day mark without sleep, individuals may experience severe perceptual distortions and an almost uncontrollable urge to sleep. Complex hallucinations and disordered thinking can emerge.
These aren’t necessarily dramatic visual hallucinations like seeing things that aren’t there. More commonly, they involve distortions of actual objects, shadows appearing to move, or misinterpretation of sounds and visual stimuli.
Concentration becomes nearly impossible. Executive function—the ability to plan, organize, and execute tasks—is profoundly compromised.
What Happens to Your Brain During Sleep Deprivation
Understanding the neurological impact of staying awake requires looking at what sleep normally does for brain health.
The Glymphatic System and Waste Removal
Research from the University of Rochester and other institutions has revealed that sleep activates the brain’s waste removal system, called the glymphatic system. During sleep, this system carries fresh cerebrospinal fluid into the brain, mixes it with waste-filled fluid surrounding brain cells, and flushes the mixture out.
This process removes toxic proteins and metabolic waste that accumulate during waking hours. According to studies on sleep depth and brain cleaning, deeper sleep enhances this waste removal process. When you stay up all night, these toxins remain in the brain, potentially contributing to cognitive impairment.
As researchers at Washington University School of Medicine discovered, slow brain waves during sleep are associated with this cleansing process. Without sleep, the buildup of neurotoxic waste may contribute to the cognitive symptoms experienced during sleep deprivation.
Prefrontal Cortex Shutdown
Brain imaging studies demonstrate that the prefrontal cortex—responsible for complex thinking, planning, and impulse control—shows significantly reduced activity after sleep deprivation. This explains why decision-making becomes so impaired.
You might make choices while sleep-deprived that you’d never make when well-rested. Risk assessment becomes skewed, and the ability to inhibit inappropriate responses deteriorates.
Long-Term Health Consequences of Chronic Sleep Loss
While a single all-nighter won’t cause permanent damage for most healthy individuals, patterns of insufficient sleep create serious health risks over time.
Metabolic and Cardiovascular Effects
According to CDC data, sleep deprivation is linked to increased risk of chronic conditions including obesity, Type 2 diabetes, and cardiovascular disease. What you eat, when you eat, how your body processes blood sugar, and sleep quality all contribute to metabolic health.
National data from 2010 showed that over 50% of night shift healthcare workers reported sleeping 6 or fewer hours a day. Studies of healthcare workers on night and rotating shifts indicate they face the highest difficulties with sleep, creating cumulative health risks.
In a study of more than 63,000 nurses, self-identified night owls were 54% more likely to have an unhealthy lifestyle.
Mental Health Impacts
Stanford researchers in a study of more than 70,000 adults found that bedtime significantly affects mental health risk. Those who regularly went to sleep later showed increased rates of depression and anxiety, even when controlling for sleep duration.
The CDC notes that insufficient sleep is linked to increased risk of anxiety and depression. Sleep disruption affects emotional regulation, stress response, and neurotransmitter systems that govern mood.
Immune System Suppression
Sleep deprivation adversely affects immune function. Even a single night without sleep reduces the activity of natural killer cells and other immune components. Over time, chronic insufficient sleep increases susceptibility to infections and may affect recovery from illness.

Recovery From Sleep Deprivation
The good news? Recovery from acute sleep deprivation is possible, though it’s not instantaneous.
After a single all-nighter, most cognitive functions return to normal within 1-2 days of adequate sleep. However, you can’t simply “bank” sleep in advance or completely repay sleep debt with one long sleep session.
Research indicates that chronic sleep restriction requires extended periods of normal sleep to fully recover. If you’ve been sleeping 5-6 hours nightly for weeks, one weekend of sleeping in won’t completely reverse the accumulated deficit.
Some people attempt to use naps to offset sleepiness after an all-nighter. Short naps (20-30 minutes) can provide temporary boosts in alertness and performance, but they don’t replace the restorative functions of a full night’s sleep.
When All-Nighters Might Be Necessary
Sometimes staying up all night isn’t a choice—it’s a requirement. Emergency responders, healthcare workers, military personnel, and others in critical roles occasionally have no alternative.
For those who must pull an all-nighter, certain strategies can minimize harm:
- Stay hydrated throughout the night
- Consume small amounts of caffeine strategically (not after 4 AM if you plan to sleep the next night)
- Keep lights bright to help suppress melatonin
- Move regularly and avoid sitting still for extended periods
- Eat light, healthy snacks rather than heavy meals
- Plan recovery sleep as soon as possible afterward
But here’s the reality: there’s no truly safe way to stay awake for 24+ hours when performing tasks requiring alertness and judgment. The impairment is real and measurable.
The Special Case of Night Owls and Late Sleepers
Being a consistent night owl differs from pulling occasional all-nighters, but the health implications overlap.
Chronotype refers to natural preference for sleep timing. Evening chronotypes (night owls) naturally feel more alert later and prefer sleeping and waking later. This isn’t laziness—it’s biological.
However, research from UCLA Health indicates that being a night owl carries health risks when it conflicts with societal schedules. Night owls often experience “social jet lag,” forced to wake early for work or school despite late bedtimes, creating chronic partial sleep deprivation.
Studies show that night owls face increased risk of cardiovascular problems, metabolic disorders, and mental health issues. The mechanism likely involves circadian rhythm disruption and the chronic sleep restriction many night owls experience.
Shifting to an earlier sleep schedule can help, though it requires patience. Experts recommend moving bedtime earlier by just 15-20 minutes every few days rather than attempting dramatic overnight changes.
Sleep Recommendations by Age
Understanding how much sleep different age groups need provides context for why all-nighters are particularly problematic.
| Age Group | Recommended Sleep Duration | Consequences of Deprivation |
|---|---|---|
| Children 4-12 months | 12-16 hours per 24 hours | Developmental delays, behavioral issues |
| Children 1-2 years | 11-14 hours per 24 hours | Growth problems, cognitive impairment |
| Children 3-5 years | 10-13 hours per 24 hours | Attention problems, emotional dysregulation |
| Children 6-14 years | 9-12 hours per night | Academic difficulties, health risks |
| High school students | 8-10 hours per night | Poor performance, mood disorders |
| Adults | 7-8 hours per night | Chronic disease risk, cognitive decline |
According to CDC data, about one-third of U.S. adults and children (under 14) and three-quarters of high schoolers do not get enough sleep. This widespread sleep deprivation represents a significant public health concern.
Frequently Asked Questions
A single all-nighter won’t kill a healthy person, but extended sleep deprivation can eventually be fatal. Research shows that prolonged total sleep deprivation can lead to death, though this typically requires many days without any sleep. The immediate dangers come from impaired judgment and coordination leading to accidents.
Most people need 1-2 nights of quality sleep to recover from a single all-nighter. Cognitive performance typically returns to baseline within this timeframe. However, some subtle effects on reaction time and complex decision-making may persist slightly longer.
Generally speaking, getting some sleep is better than none. Even 2 hours allows for at least one complete sleep cycle, which provides some restorative benefits. However, waking from deep sleep after only 2 hours can cause severe grogginess. If you have less than 3 hours available before you must wake, some sleep experts suggest staying awake might feel better in the short term, though this remains controversial.
After 48 hours, brain function deteriorates significantly. Cognitive tasks become extremely difficult, microsleep episodes occur frequently, and emotional regulation is severely compromised. Brain imaging shows reduced activity in areas controlling attention, memory, and executive function. Perceptual distortions may begin appearing.
Caffeine can temporarily reduce feelings of sleepiness and improve alertness during sleep deprivation, but it doesn’t reverse the cognitive impairment caused by sleep loss. Strategic caffeine use (small amounts spread throughout the night rather than large doses) works better than consuming massive quantities. Avoid caffeine after 4 AM if you plan to sleep the following night.
Short naps (20-30 minutes) provide temporary improvements in alertness and performance but cannot replace the restorative functions of full nighttime sleep. Longer naps can cause grogginess upon waking. Naps help manage acute sleepiness but don’t eliminate sleep debt or reverse the health impacts of chronic sleep deprivation.
Sleep deprivation triggers stress responses in the body, elevating cortisol and other stress hormones. This can cause nausea, headaches, and general malaise. Additionally, sleep loss impairs immune function, potentially making existing minor illnesses feel worse. Dehydration and poor food choices during all-nighters contribute to feeling unwell.
Conclusion
Staying up all night creates measurable impairment in cognitive function, emotional regulation, and physical coordination. While occasional all-nighters won’t cause permanent damage for most healthy individuals, they’re far from harmless.
The science is clear: sleep isn’t optional luxury. It’s biological necessity. During sleep, your brain clears metabolic waste, consolidates memories, and performs essential maintenance. Without it, performance suffers in ways comparable to intoxication.
If you regularly find yourself pulling all-nighters or consistently getting insufficient sleep, it’s time to prioritize sleep health. The long-term consequences—increased risk for chronic diseases, mental health disorders, and cognitive decline—are too significant to ignore.
Start by establishing consistent sleep and wake times, even on weekends. Create a sleep-friendly environment: dark, quiet, and cool. Limit screen time before bed. If sleep problems persist despite good habits, consult a healthcare provider. According to Institute of Medicine research, about 80 to 90 percent of adults with clinically significant sleep-disordered breathing remain undiagnosed.
Your brain and body will thank you for making sleep a priority rather than an afterthought.
