Quick Summary: Mixing Lexapro (escitalopram) and alcohol is not recommended by the FDA due to increased risks of sedation, impaired judgment, worsened depression, and enhanced side effects. Both substances affect serotonin levels and central nervous system function, creating unpredictable interactions that can undermine treatment effectiveness and safety.
Lexapro is one of the most commonly prescribed antidepressants in the United States, used to treat major depressive disorder and anxiety. But when it comes to mixing this medication with alcohol, the answer isn’t as simple as a yes or no.
The FDA recommends avoiding alcohol while taking Lexapro. But what actually happens in your body when these two substances combine? And are there situations where an occasional drink might be acceptable?
This guide breaks down the science, the risks, and what healthcare providers actually tell their patients about drinking on Lexapro.
Understanding Lexapro and How It Works
Lexapro, known generically as escitalopram, belongs to a class of medications called selective serotonin reuptake inhibitors (SSRIs). These drugs work by increasing serotonin levels in the brain, a neurotransmitter that regulates mood, anxiety, and emotional stability.
When someone takes Lexapro, the medication blocks the reabsorption of serotonin in brain cells. This allows more serotonin to remain available in the neural pathways, which gradually improves symptoms of depression and anxiety over several weeks.
The medication is typically prescribed at doses ranging from 10mg to 20mg daily. It reaches steady levels in the body after about a week of consistent use, though full therapeutic effects often take 4-6 weeks to develop.
How Alcohol Affects Your Brain Chemistry
Alcohol functions as a central nervous system depressant. It enhances the effects of GABA, an inhibitory neurotransmitter, while simultaneously affecting serotonin, dopamine, and other neurochemical systems.
Here’s where the problem begins: alcohol also influences serotonin levels. When combined with Lexapro, which is already manipulating serotonin pathways, the interaction becomes unpredictable.
Alcohol can counteract the therapeutic benefits of antidepressants. While Lexapro works to stabilize mood, alcohol disrupts this process by depressing neural activity and potentially worsening depression and anxiety symptoms.
The Dangerous Interaction Between Lexapro and Alcohol
When Lexapro and alcohol combine in the system, several concerning interactions occur simultaneously.
Enhanced Central Nervous System Depression
Both substances depress central nervous system function. When taken together, this sedative effect amplifies significantly beyond what either substance produces alone.
This combination can lead to dangerous levels of drowsiness, confusion, and coordination problems that persist well beyond typical alcohol recovery time. The enhanced sedative effects may impair the ability to drive, work, or make sound decisions for up to 24 hours.
Serotonin System Disruption
The serotonin interaction creates a complex problem. While rare, combining alcohol with SSRIs can theoretically increase the risk of serotonin syndrome, a potentially life-threatening condition caused by excessive serotonin activity.
More commonly, alcohol interferes with Lexapro’s therapeutic mechanism, reducing the medication’s effectiveness in treating depression and anxiety.
Impaired Judgment and Cognitive Function
Lexapro alone can occasionally cause dizziness or drowsiness, especially during the initial weeks of treatment. Alcohol magnifies these effects considerably.
Patients report experiencing confusion, difficulty concentrating, and significantly impaired decision-making ability when mixing these substances. Individual sensitivity to both alcohol and medication can vary greatly, making it impossible to predict exactly how any one person will react.
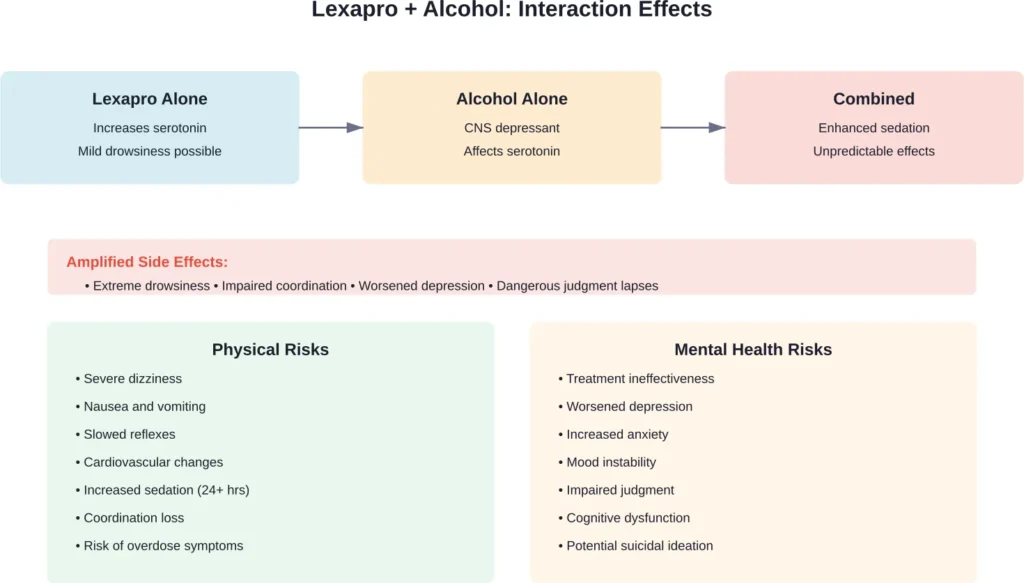
Common Side Effects of Mixing Lexapro and Alcohol
Research and clinical reports identify several common side effects when these substances are combined:
| Side Effect Category | Symptoms | Severity Level |
|---|---|---|
| Cognitive Impairment | Confusion, difficulty concentrating, memory problems, slowed thinking | Moderate to High |
| Physical Coordination | Dizziness, loss of balance, slowed reflexes, motor skill impairment | Moderate to High |
| Sedation | Extreme drowsiness, fatigue, difficulty staying awake | High |
| Mood Changes | Worsened depression, increased anxiety, mood swings, irritability | High |
| Gastrointestinal | Nausea, vomiting, stomach discomfort | Moderate |
| Cardiovascular | Changes in blood pressure, irregular heartbeat | Moderate |
The severity and combination of symptoms varies significantly between individuals. Factors like body weight, metabolism, dosage, alcohol amount, and individual sensitivity all play a role.
Why Alcohol Undermines Mental Health Treatment
According to research on co-occurring alcohol use disorder and major depressive disorder, the bidirectional relationship between alcohol use and depression complicates diagnosis and treatment outcomes significantly.
Alcohol is inherently a depressant. While it may provide temporary mood elevation or anxiety relief, it disrupts the neurochemical balance that antidepressants work to establish.
Treatment Effectiveness Concerns
Studies examining psychiatric inpatients with alcohol use disorder found that antidepressants were among the most frequently prescribed medications (31.2% of cases), according to a pharmacovigilance program analyzing 10,332 patients treated between 2000 and 2016. However, concurrent alcohol use can substantially reduce the therapeutic benefits of these medications.
When someone drinks while taking Lexapro, they’re essentially working against their treatment. The medication tries to stabilize serotonin levels and improve mood, while alcohol disrupts these same systems.
Over time, this pattern can lead to treatment resistance, where the antidepressant becomes less effective even when alcohol consumption stops.
The Cycle of Depression and Drinking
Many people with depression turn to alcohol for temporary relief. But this creates a destructive cycle: depression leads to drinking, drinking worsens depression, worsening depression increases drinking.
Research on integrated management of co-occurring alcohol use disorder and depression emphasizes that concurrent disorders require specialized treatment approaches. Treating depression alone without addressing problematic drinking patterns often leads to poor outcomes.
How Long After Taking Lexapro Can You Drink?
This question doesn’t have a straightforward answer, and that frustrates many patients.
Lexapro has a half-life of approximately 27-32 hours (verified in MedlinePlus sources). This means it takes about 27-32 hours for half the drug to leave the system. But that doesn’t mean the other half disappears quickly.
Generally speaking, it takes about 5-6 half-lives for a medication to be mostly eliminated from the body. For Lexapro, that’s roughly 6-7 days after the last dose.
But here’s the thing: healthcare providers don’t typically recommend timing alcohol consumption around Lexapro doses for several reasons.
First, Lexapro works best when taken consistently at the same time daily. Missing doses or timing them irregularly to accommodate drinking undermines the entire treatment.
Second, the therapeutic benefits of SSRIs depend on maintaining steady levels in the system. Strategic dose timing defeats this purpose.
Third, if someone is thinking about their drinking schedule in relation to medication, that pattern might indicate a problematic relationship with alcohol worth discussing with a healthcare provider.
Individual Risk Factors That Matter
Not everyone responds to the Lexapro-alcohol combination identically. Several factors influence individual risk levels.
Dosage Considerations
Higher Lexapro doses (15-20mg) typically carry greater interaction risks than lower doses (5-10mg). The more medication present in the system, the more pronounced the interaction with alcohol becomes.
Treatment Phase
Early treatment phases, particularly the first 4-6 weeks, represent a critical period. The body is still adjusting to the medication, and adding alcohol to this adjustment period increases risks substantially.
During this time, patients are more susceptible to side effects and less able to predict how their body will respond to various substances.
Personal Health Factors
Liver function, body weight, metabolism speed, age, and other medications all influence how both Lexapro and alcohol are processed. Older adults typically experience more pronounced effects from both substances.
Anyone with liver or kidney problems faces additional risks, as these organs are responsible for metabolizing both the medication and alcohol.
Drinking Patterns
There’s a difference between having one glass of wine with dinner occasionally and regular heavy drinking. Binge drinking episodes carry significantly higher risks than moderate, infrequent alcohol consumption.
That said, even moderate drinking can be problematic for some individuals, particularly those with histories of depression, anxiety, or substance use concerns.

What Healthcare Providers Actually Recommend
The official medical guidance is clear: avoid alcohol while taking Lexapro.
But real-world conversations between doctors and patients often involve more nuanced discussions. Some healthcare providers acknowledge that complete abstinence may not be realistic for all patients, particularly those with stable, long-term treatment.
In these cases, providers might discuss harm reduction strategies: limiting alcohol to very occasional, single servings; avoiding drinking during treatment initiation or dose changes; monitoring for any symptom changes; and maintaining open communication about drinking patterns.
However, this isn’t a blanket permission. Providers make these individualized recommendations based on specific patient circumstances, treatment history, and risk assessment.
Signs You Need Immediate Medical Attention
Certain symptoms after mixing Lexapro and alcohol require immediate medical evaluation:
- Severe confusion or disorientation
- Difficulty breathing or rapid heartbeat
- Loss of consciousness or extreme sedation
- Seizures or convulsions
- Severe agitation or restlessness
- High fever, excessive sweating, or tremors (possible serotonin syndrome)
- Suicidal thoughts or self-harm urges
- Uncontrollable vomiting
These symptoms may indicate serious complications including overdose, serotonin syndrome, or severe interaction effects. Don’t wait to see if symptoms improve—seek emergency care immediately.
The Reality of Social Drinking Pressure
One of the most challenging aspects of avoiding alcohol on Lexapro isn’t physical—it’s social.
Drinking culture pervades many social situations, from work events to family gatherings. Declining drinks repeatedly can feel uncomfortable, especially when treatment for depression or anxiety isn’t something a person wants to disclose publicly.
Some strategies that help:
Order non-alcoholic drinks that look like cocktails. Nobody needs to know that’s tonic water with lime instead of a gin and tonic.
Have a prepared, simple explanation: “I’m not drinking tonight” or “I’m taking a break from alcohol” usually suffices without inviting intrusive questions.
Remind yourself that prioritizing mental health treatment over social expectations isn’t selfish—it’s necessary.
Consider whether the friendship or social situation genuinely requires alcohol. If so, that might be worth examining more closely.
Addressing Common Myths About Safe Mixing
Several myths circulate about supposedly safe ways to mix Lexapro and alcohol. Real talk: most are dangerous misconceptions.
Myth: Waiting a Few Hours After Your Dose Makes It Safe
False. Lexapro remains active in the system for days, not hours. Timing drinking around daily doses doesn’t eliminate interaction risks.
Myth: Drinking Only Beer or Wine Is Safer Than Liquor
The type of alcohol doesn’t matter—the issue is the ethanol content and its interaction with the medication. A standard beer, glass of wine, and shot of liquor all contain roughly equivalent amounts of alcohol.
Myth: If You Don’t Feel Side Effects, It’s Fine
Some of the most concerning effects—like reduced medication effectiveness and worsening depression—aren’t immediately noticeable. Just because someone doesn’t experience acute drowsiness doesn’t mean the combination is harmless.
Myth: Everyone on SSRIs Drinks Sometimes
Community discussions on health forums suggest many people do drink occasionally while on antidepressants. But prevalence doesn’t equal safety. Individual experiences vary dramatically, and what didn’t cause problems for one person might be dangerous for another.
When Drinking Patterns Indicate Bigger Problems
Research examining concurrent alcohol use disorder and major depressive disorder highlights how frequently these conditions co-occur and complicate each other.
If the thought of giving up alcohol while taking Lexapro feels impossible, that reaction itself may be significant. Difficulty abstaining from alcohol, even temporarily for health reasons, can indicate problematic drinking patterns.
Warning signs that alcohol use might require professional attention include:
- Drinking daily or feeling unable to skip drinking
- Continuing to drink despite knowing the medical risks
- Increasing alcohol amounts to achieve the same effects
- Using alcohol to cope with depression or anxiety symptoms
- Experiencing withdrawal symptoms when not drinking
- Prioritizing drinking over health, relationships, or responsibilities
According to research on pharmacotherapy for alcohol use disorder, integrated treatment addressing both conditions simultaneously produces better outcomes than treating either condition alone.
Alternative Coping Strategies
For many people, alcohol serves as a social lubricant or stress management tool. Finding alternatives becomes important when alcohol is no longer compatible with treatment.
Exercise provides natural mood elevation through endorphin release and complements antidepressant therapy. Even moderate activity like walking shows measurable benefits for depression and anxiety.
Mindfulness practices, meditation, and breathing exercises offer stress reduction without substance use. Many find these techniques enhance the benefits of medication rather than working against it.
Social connection through non-drinking activities—hobby groups, sports, volunteer work, or creative pursuits—provides the community benefits of social drinking without the risks.
Therapy, particularly cognitive behavioral therapy, addresses underlying patterns that medication alone doesn’t resolve. The combination of therapy and medication typically produces better outcomes than either approach alone.
Having Honest Conversations With Your Doctor
Many patients hesitate to discuss alcohol use honestly with healthcare providers, fearing judgment or lecture. But accurate information is essential for safe, effective treatment.
Healthcare providers need to know actual drinking patterns—not idealized versions—to make appropriate recommendations. A doctor who knows a patient occasionally has 2-3 drinks can provide more relevant guidance than one operating on the assumption of complete abstinence.
Questions to discuss with healthcare providers include:
- Given my specific situation, what are my actual risks with alcohol?
- Are there warning signs I should watch for?
- How will we know if alcohol is interfering with my treatment?
- If I do choose to drink occasionally, what precautions should I take?
- Should we consider alternative medications if alcohol avoidance isn’t realistic?
Some people find that certain SSRIs or other antidepressant classes have fewer alcohol interactions, though all carry some risk. These decisions require medical guidance based on individual health profiles.
Frequently Asked Questions
The FDA recommends avoiding alcohol entirely while taking Lexapro. While some individuals may tolerate a single drink without obvious adverse effects, the interaction risks still exist. Individual responses vary significantly based on dosage, metabolism, treatment phase, and personal health factors. Anyone considering occasional alcohol consumption should discuss their specific situation with their prescribing healthcare provider first.
Lexapro has a half-life of approximately 27-32 hours. It takes roughly 6-7 days for the medication to be mostly eliminated from the body after the last dose. However, this doesn’t mean drinking becomes safe after missing a dose or two, as consistent medication levels are essential for therapeutic effectiveness.
If someone accidentally consumes alcohol while taking Lexapro, they should monitor for enhanced sedation, dizziness, confusion, or mood changes. Drinking plenty of water, avoiding additional alcohol, and resting in a safe environment are important. If severe symptoms develop—including extreme drowsiness, difficulty breathing, or unusual behavior—seek immediate medical attention. Contact the prescribing healthcare provider to report the incident and discuss any concerns.
Yes, alcohol can reduce Lexapro’s therapeutic effectiveness. Alcohol disrupts the same neurotransmitter systems that the medication works to stabilize, particularly serotonin pathways. Regular alcohol consumption while taking antidepressants can lead to worsened depression symptoms, increased anxiety, and reduced treatment outcomes. This effect may not be immediately obvious but can undermine long-term mental health improvement.
No. The interaction concern involves ethanol (alcohol) itself, not the specific beverage type. A standard serving of beer, wine, or liquor contains approximately the same amount of alcohol and poses equivalent interaction risks with Lexapro. The myth that beer or wine is safer than spirits has no scientific basis regarding medication interactions.
Long-term, stable treatment doesn’t eliminate interaction risks, though some healthcare providers may offer more nuanced guidance for patients who have been stable on consistent doses for extended periods. The interaction between alcohol and Lexapro exists regardless of treatment duration. However, individual risk assessments may differ for someone stable on 10mg for three years versus someone who started 20mg last month. These decisions require individualized medical consultation.
Serotonin syndrome is rare but potentially serious. Warning signs include high fever, excessive sweating, rapid heartbeat, severe agitation or restlessness, confusion, dilated pupils, muscle rigidity or twitching, tremors, and coordination problems. Severe cases may involve seizures or loss of consciousness. While serotonin syndrome more commonly occurs when combining multiple serotonergic medications, the theoretical risk exists with alcohol combinations. Any suspected symptoms require immediate emergency medical evaluation.
The Bottom Line on Lexapro and Alcohol
The evidence is clear: mixing Lexapro and alcohol creates multiple risks that outweigh any perceived benefits.
These substances interact in ways that enhance sedation, impair cognitive function, worsen mental health symptoms, and potentially reduce treatment effectiveness. Individual sensitivity varies, making reactions unpredictable.
The FDA and healthcare providers recommend avoiding alcohol while taking Lexapro. For those who struggle with this recommendation, honest conversations with medical providers about drinking patterns, treatment alternatives, and potential alcohol use concerns are essential.
Mental health treatment works best when supported by lifestyle choices that complement rather than undermine therapeutic goals. For most people taking Lexapro, that means avoiding alcohol or severely limiting consumption in consultation with healthcare providers.
If drinking feels impossible to reduce or eliminate, that pattern itself warrants professional evaluation. According to recent research on concurrent disorders, integrated treatment addressing both depression and alcohol use produces better outcomes than treating either condition in isolation.
Taking Lexapro represents a commitment to mental health improvement. Protecting that investment by avoiding interactions that compromise treatment effectiveness is part of that commitment.
If you’re struggling with depression, anxiety, or questions about medication interactions, consult with a healthcare provider who can provide personalized guidance based on your specific health situation and treatment goals.