Quick Summary: A tick bite typically causes minor skin reactions, but some ticks transmit serious diseases like Lyme disease. Most bites are painless, and ticks must be attached for 24-36 hours to spread infection. Proper removal within this timeframe and monitoring for symptoms like rashes or fever are critical for preventing complications.
Most people don’t even realize when a tick bites them. These small arachnids attach painlessly to skin, feeding on blood for hours or even days before being noticed. But here’s what matters: some ticks carry bacteria and viruses that cause serious infections.
Understanding what happens during and after a tick bite can help prevent complications. The response varies dramatically based on whether the tick carries disease and how quickly it’s removed.
The Immediate Bite: What Actually Happens
When a tick finds exposed skin, it doesn’t just bite immediately. According to Harvard Health, ticks wander the body for 30 minutes to an hour before inserting their feeding parts into the skin. They prefer warm, moist areas like the scalp, armpits, groin, and behind the knees.
The bite itself is painless. Ticks burrow their feeding parts into the skin, secreting compounds that prevent blood clotting and numb the area. Only these feeding parts penetrate—the tick’s body remains visible on the surface.
Most tick bites cause minimal immediate symptoms. A small red bump may appear at the bite site, similar to a mosquito bite. Sometimes there’s slight swelling or irritation, but severe reactions are rare.
Disease Transmission: The Real Danger
The serious concern isn’t the bite itself—it’s what the tick might be carrying. According to the CDC, blacklegged ticks (also called deer ticks) spread Lyme disease bacteria to humans. Lyme disease represents the leading cause of tickborne illness in the United States.
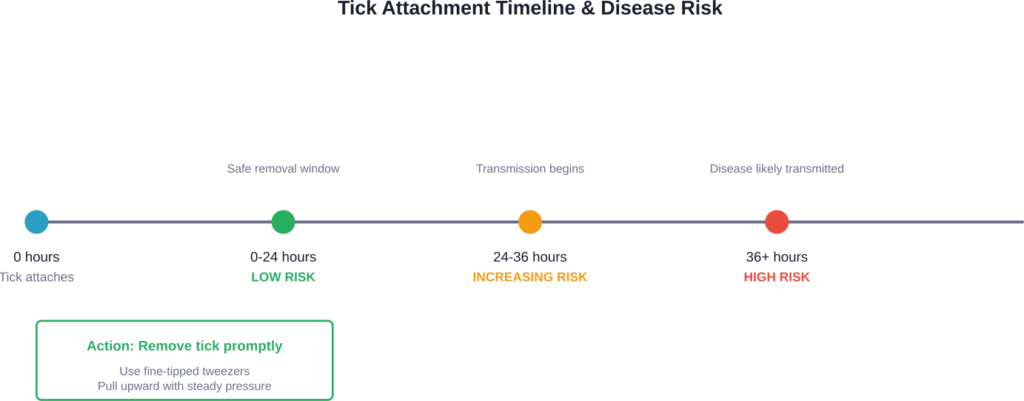
But transmission isn’t instant. Research from Cornell Health shows that infected deer ticks must remain attached for at least 24 to 36 hours to transmit Lyme disease. This timeframe provides a critical window for prevention.
Here’s the thing though—not all ticks carry disease. Even in high-risk areas, only a fraction of ticks are infected. According to InformedHealth.org (NCBI), in TBE high-risk areas in Germany, only about 0.1 to 5% of ticks carry the tick-borne encephalitis virus.
Symptoms: What to Watch For
According to the CDC, typical Lyme disease symptoms include fever, headache, fatigue, and a characteristic skin rash called erythema migrans. This rash often appears as a circular red area expanding outward from the bite site—sometimes described as a “bull’s-eye” pattern.
Early signs typically develop 3 to 30 days after the bite. Not everyone develops the rash, though. Some people only experience flu-like symptoms.
Early Stage Symptoms
The initial phase produces relatively mild symptoms that many people dismiss as a common cold or flu. Fever and chills appear frequently. Headaches and muscle aches are common complaints.
The erythema migrans rash remains the most distinctive early indicator. It expands gradually over several days, sometimes reaching 12 inches (30 cm) or more across.
Later Stage Complications
If left untreated, infection spreads beyond the bite site. According to the CDC, Lyme disease can spread to joints, the heart, and the nervous system. Symptoms become progressively severe.
Joint pain and swelling—particularly in the knees—affects many untreated patients. Facial paralysis can occur. Some people develop irregular heartbeat or neurological problems.
Real talk: early treatment prevents these complications. Antibiotics work effectively when started during the early infection stage.
| Symptom Category | Timing After Bite | Common Signs |
|---|---|---|
| Immediate Reaction | 0-2 days | Small red bump, mild swelling, slight irritation |
| Early Localized | 3-30 days | Expanding rash, fever, headache, fatigue |
| Early Disseminated | Days to weeks | Multiple rashes, facial paralysis, heart palpitations |
| Late Disseminated | Months to years | Severe joint pain, neurological symptoms, chronic arthritis |
Other Tick-Borne Diseases Beyond Lyme
Lyme disease gets the most attention, but ticks transmit numerous other pathogens. Rocky Mountain spotted fever causes severe illness with fever, headache, and distinctive spotted rash. Tick-borne encephalitis (TBE) represents another serious viral infection.
According to WHO, TBE causes viral infections of the central nervous system with symptoms including fever, headache, stiff neck, drowsiness, and confusion. For the European form, the case-fatality rate is approximately 1-5%; for the Asian form, approximately 20%.
Tick paralysis presents another risk. According to the University of Illinois, this condition causes impaired muscle control and paralysis starting in the feet and legs, moving upward. Symptoms typically develop after the tick has been attached for 3 to 7 days but subside within 24 hours of removing the tick.
Stanford Medicine data shows tick-borne diseases overall increased about 25% from 2011 to 2019. Warmer climates, booming deer and rodent populations, and suburban expansion contribute to this rise.
Proper Tick Removal: The Critical First Step
Removal technique matters enormously. According to Cornell Health, improper removal methods can actually increase the chances of disease transmission.
Never use nail polish, petroleum jelly, or heat to remove ticks. These folk remedies don’t work and may cause the tick to regurgitate into the wound, increasing infection risk.
The correct method requires fine-tipped tweezers. Grasp the tick as close to the skin’s surface as possible. Pull upward with steady, even pressure—don’t twist or jerk, which can break off mouthparts in the skin.
After removal, clean the bite area thoroughly with rubbing alcohol or soap and water. Dispose of the live tick by submersing it in alcohol, placing it in a sealed bag, or flushing it down the toilet.

When to Seek Medical Care
Not every tick bite requires a doctor visit. But certain situations demand prompt medical attention.
Seek care immediately if a rash develops at the bite site, especially if it expands over several days. Fever, headache, or flu-like symptoms appearing within 30 days of a bite warrant evaluation.
According to the CDC, prompt medical care is essential if symptoms appear after spending time in areas known for Lyme disease. The Northeast, mid-Atlantic, and upper-Midwest regions of the United States show the highest Lyme disease rates.
Some healthcare providers may prescribe preventive antibiotics after high-risk tick bites in certain situations.
Prevention Strategies That Actually Work
According to the CDC, the best way to protect against Lyme disease is preventing tick bites altogether. Several evidence-based strategies reduce exposure risk.
Use EPA-registered insect repellents containing DEET, picaridin, IR3535, oil of lemon eucalyptus (OLE), para-menthane-diol (PMD), or 2-undecanone. These compounds effectively repel ticks when applied to exposed skin.
Wear long-sleeved shirts and pants when hiking or walking through wooded areas. Tuck pant legs into socks and shirts into pants—this looks dorky but works. Light-colored clothing makes ticks easier to spot.
Treat clothing and gear with products containing 0.5% permethrin. This insecticide kills ticks on contact and remains effective through multiple washings.
After outdoor activities, conduct thorough tick checks. Examine the entire body, paying special attention to hidden areas: scalp, behind ears, armpits, groin, behind knees, and between toes. Shower within two hours of coming indoors—this helps wash off unattached ticks.
| Prevention Strategy | Effectiveness | Best Use Case |
|---|---|---|
| DEET repellent (20-30%) | High | Exposed skin during outdoor activities |
| Permethrin-treated clothing | Very High | Hiking, camping, yard work in tick areas |
| Long sleeves and pants | Moderate-High | Walking through tall grass or woods |
| Daily tick checks | Essential | After any outdoor exposure |
| Shower within 2 hours | Moderate | Removes unattached ticks |
Geographic Risk Areas
Tick distribution isn’t uniform. According to the CDC, Lyme disease is most common in the Northeast, mid-Atlantic, and upper-Midwest regions of the United States. These areas harbor large populations of blacklegged ticks.
But wait. Tick ranges are expanding. Climate change and environmental factors allow ticks to survive in previously unsuitable areas. What was once a low-risk region may now harbor established tick populations.
Other tick-borne diseases show different geographic patterns. Rocky Mountain spotted fever occurs throughout the United States but concentrates in specific regions. Tick-borne encephalitis remains primarily a European and Asian concern, though awareness is growing.
Frequently Asked Questions
According to research from Cornell Health and the CDC, an infected blacklegged tick must remain attached for at least 24 to 36 hours to transmit Lyme disease bacteria. This timeframe provides a critical window for safe tick removal before infection occurs. Prompt removal within 24 hours significantly reduces transmission risk.
Most tick bites appear as small red bumps similar to mosquito bites. The area may show slight swelling or irritation. The characteristic Lyme disease rash—erythema migrans—develops 3 to 30 days after the bite and expands outward in a circular pattern, sometimes with a clear center resembling a bull’s-eye. Not all Lyme cases produce this rash.
No, tick bites are painless. According to Harvard Health, ticks secrete compounds that numb the bite area while preventing blood clotting. This allows them to feed undetected for hours or days. Most people discover ticks during visual checks rather than feeling the bite itself.
Saving the tick can be helpful for identification purposes, particularly if symptoms develop later. Place it in a sealed container with rubbing alcohol and note the date of removal. Some healthcare providers or health departments offer tick identification services. However, immediate testing of the tick itself isn’t typically recommended—monitoring for symptoms remains more practical.
No. Only certain tick species transmit Lyme disease—primarily blacklegged ticks in the United States. Even among these species, not all individual ticks are infected. Infection rates vary by geographic region and tick population.
An ordinary tick bite creates a small red bump that appears within hours and typically resolves in a few days. The Lyme disease rash—erythema migrans—appears 3 to 30 days after the bite, expands gradually over days, and often reaches 6-12 inches in diameter. The expanding circular pattern with possible central clearing distinguishes it from a simple bite reaction.
According to the CDC, seek medical care if any rash develops at the bite site, especially if it expands. Also consult a healthcare provider if fever, headache, fatigue, or flu-like symptoms appear within 30 days of a tick bite. Immediate care is particularly important for bites occurring in high-risk Lyme disease areas like the Northeast, mid-Atlantic, or upper-Midwest United States.
The Bottom Line
Tick bites range from completely harmless to potentially serious depending on whether the tick carries disease. The good news? Most complications are preventable through prompt tick removal and awareness of warning signs.
Understanding the 24-36 hour transmission window empowers effective prevention. Daily tick checks after outdoor activities, proper removal techniques, and monitoring for symptoms create multiple layers of protection.
Don’t panic if you find a tick—but don’t ignore it either. Remove it properly, clean the area thoroughly, and watch for symptoms over the following weeks. When in doubt, consult a healthcare provider. Early detection and treatment of tick-borne diseases produce excellent outcomes.
Stay vigilant during peak tick season (late spring through early summer), use proven repellents, and enjoy the outdoors with confidence.
