Quick Summary: Missing a birth control pill can reduce contraceptive effectiveness, but the steps you need to take depend on the type of pill, how many you missed, and when in the pack it happened. For combination pills, missing one pill typically requires taking it as soon as you remember and continuing normally, while missing two or more may require backup contraception for seven days. Progestin-only pills have a stricter timeframe and may require emergency contraception if taken more than three hours late.
Almost everyone who takes birth control pills misses a dose at some point. Life happens. You forget. The pill pack gets buried in your bag. Your routine gets disrupted.
But what actually happens when you miss that pill? And more importantly, what should you do next?
The answer isn’t one-size-fits-all. It depends on which type of pill you’re taking, how many you missed, and where you are in your pill pack. According to CDC research on combined hormonal contraceptives, approximately seven out of 100 CHC users become pregnant in the first year with typical use (about 7%)—and missed pills contribute significantly to that statistic.
Here’s everything you need to know about navigating missed birth control pills.
Understanding Different Types of Birth Control Pills
Not all birth control pills work the same way. The guidance for missed pills differs dramatically based on what type you’re taking.
Combination Pills
Combination pills contain both estrogen and progestin. These are the most common type of oral contraceptive in the United States. They come in various formulations, typically with 21 active pills and 7 inactive pills (or 24 active and 4 inactive).
Combination pills contain varying hormone doses. The specific hormonal composition affects how quickly follicular activity resumes when pills are missed.
Progestin-Only Pills (Mini Pills)
Progestin-only pills contain no estrogen—just progestin. According to the CDC, three formulations are currently available in the United States: norethindrone, norgestrel, and drospirenone (DRSP).
These pills work differently and have stricter timing requirements than combination pills. The window for taking them on time is much narrower.
What Happens in Your Body When You Miss a Pill
When you miss a birth control pill, your hormone levels drop. This can trigger several physiological responses.
Birth control pills work primarily by preventing ovulation—they keep your ovaries from releasing an egg. They also thicken cervical mucus and thin the uterine lining.
But here’s the thing: these effects require consistent hormone levels. When you miss a pill, those levels drop, and your body may start trying to ovulate.
A systematic review published by the CDC examined what happens during extended hormone-free intervals. Researchers found wide variability in follicular development when women extended the pill-free interval to 8-14 days. While the overall risk of ovulation remained relatively low, some women did ovulate—though cycles were usually abnormal with low progesterone levels and poor cervical mucus quality.
Translation? Your body doesn’t immediately spring back to full fertility after one missed pill. But it can start heading in that direction.
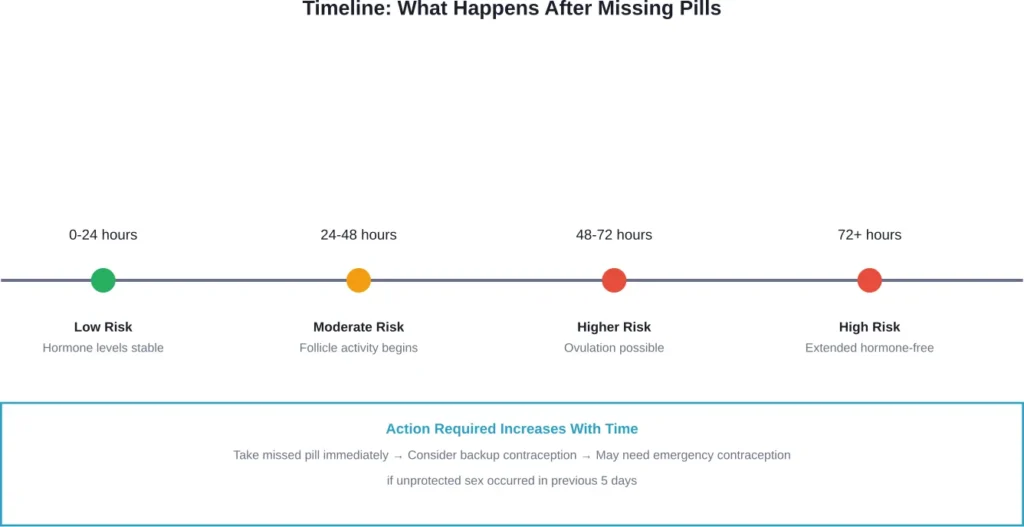
What to Do If You Miss One Combination Pill
Missing a single combination pill is the most common scenario. And it’s also the easiest to handle.
Take the missed pill as soon as you remember, even if that means taking two pills in one day. Then continue taking the rest of your pack on schedule.
Research indicates that missing pills at certain times in the cycle carries lower ovulation risk than missing pills adjacent to the hormone-free interval.
Do you need backup contraception? Generally not, if you’ve only missed one pill and you take it within 24 hours. But if you had unprotected sex in the days before missing the pill, sperm can survive in your reproductive tract for up to five days.
That’s where timing matters.
What to Do If You Miss Two or More Combination Pills
Missing multiple pills increases your pregnancy risk significantly. Here’s what you need to do.
Take the most recent missed pill immediately, even if it means taking two pills on the same day. Skip the other missed pills—don’t try to catch up by taking three or four at once.
Then use backup contraception (like condoms) for the next seven days.
When Emergency Contraception Becomes Necessary
If you had unprotected sex during the seven days before you missed pills, consider emergency contraception. According to the World Health Organization, emergency contraceptive pills can prevent up to over 95% of pregnancies when taken within five days after intercourse.
The copper IUD is even more effective as emergency contraception, but it requires a medical appointment for insertion.
Special Consideration: Missing Pills in Week One
Missing pills during the first week of your pack is particularly risky. You’re just coming off your hormone-free interval, so your ovaries are already more active.
If you miss two or more pills in week one and had unprotected sex, emergency contraception is strongly recommended.
What to Do If You Miss a Progestin-Only Pill
Progestin-only pills operate on a much stricter schedule. The CDC guidelines specify different timeframes depending on which formulation you’re taking.
For norethindrone and norgestrel pills, you have a three-hour window. If you’re more than three hours late, take the missed pill immediately, continue your pack, and use backup contraception for 48 hours.
For drospirenone (DRSP) pills, the window is 24 hours. If you’re more than 24 hours late, the same rules apply: take the pill, continue the pack, use backup contraception for 48 hours.
Why the difference? DRSP has a longer half-life in your body compared to other progestin formulations.
If you had unprotected sex in the days before missing your progestin-only pill, consider emergency contraception—especially with norethindrone or norgestrel, which have that narrow three-hour window.
| Pill Type | Grace Period | Action If Late | Backup Needed |
|---|---|---|---|
| Combination pill | 24 hours | Take missed pill immediately | No (for 1 pill) |
| Combination pill (2+ missed) | N/A | Take most recent pill, skip others | Yes (7 days) |
| Norethindrone/Norgestrel | 3 hours | Take missed pill immediately | Yes (48 hours) |
| Drospirenone (DRSP) | 24 hours | Take missed pill immediately | Yes (48 hours) |
Side Effects You Might Experience After Missing Pills
Missing birth control pills can trigger some noticeable side effects as your hormone levels fluctuate.
Breakthrough Bleeding
This is the most common side effect. You might experience spotting or light bleeding between periods when you miss pills. It happens because the drop in hormones allows the uterine lining to shed slightly.
Breakthrough bleeding doesn’t mean your birth control has failed. It’s just your body responding to the hormone disruption.
Cramping and Bloating
Some women experience mild cramping or bloating after missing pills. Again, this relates to hormone fluctuations.
Nausea
When you take two pills at once to catch up, nausea can occur. Taking pills with food usually helps minimize this.
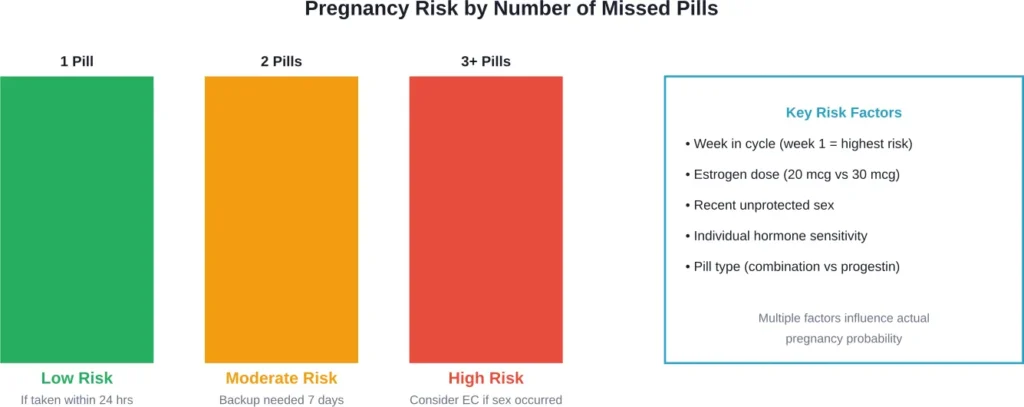
Can You Get Pregnant From Missing One Pill?
The short answer? It’s unlikely, but possible.
Pregnancy risk from a single missed pill depends on multiple factors: where you are in your cycle, your individual hormone sensitivity, and whether you had unprotected sex around the time you missed the pill.
Research shows that typical use effectiveness of birth control pills (accounting for missed pills and other real-world issues) is about 93%, compared to 99% with perfect use. That 6-percentage-point gap reflects the reality that adherence matters.
A study published in the Journal of Medical Internet Research analyzing internet search patterns found that concerns about missed oral contraceptive doses are extremely common—highlighting how widespread this issue is and how much anxiety it causes.
So yes, pregnancy from one missed pill can happen. But if you follow the catch-up instructions and use backup contraception when recommended, your risk remains very low.
When to Take a Pregnancy Test
If you missed pills and had unprotected sex, you might be wondering when to test for pregnancy.
Wait at least 12-14 days after unprotected sex, or until at least the first day of a missed period, before taking a pregnancy test for most reliable results. Testing earlier often produces false negatives because pregnancy hormones haven’t built up to detectable levels yet.
Also watch for your next period. If it doesn’t arrive within a week of when you expect it, take a test.
How to Prevent Missing Pills in the Future
Real talk: the best way to handle missed pills is not to miss them in the first place. Easier said than done, right?
But there are practical strategies that actually work.
Set a Daily Alarm
Choose a time that fits your routine—ideally connected to something you do every day at the same time. Morning coffee? Brushing teeth before bed? Anchor your pill-taking to an existing habit.
Use Apps
Numerous birth control reminder apps exist. Many send notifications and track your pill-taking pattern.
Keep Pills Visible
Out of sight means out of mind. Keep your pill pack somewhere you’ll see it daily, not buried in a drawer.
Consider Long-Acting Contraception
If you consistently struggle with daily pills, talk to your healthcare provider about alternatives. IUDs and implants don’t require daily attention. According to ACOG, use of long-acting reversible contraception (LARC) increased from 2.4% in 2002 to 11.6% in 2012, the most recent year for which data are available from the National Survey of Family Growth, partly because they eliminate adherence issues.
Special Situations and Considerations
Some scenarios create additional complications when dealing with missed pills.
Vomiting or Diarrhea
Severe vomiting within two hours of taking a pill, or severe diarrhea, can prevent proper absorption. Treat this the same as a missed pill.
Time Zone Changes
Traveling across time zones? Take your pill at the usual time in your home time zone, then gradually shift to local time by an hour or two each day if needed.
Medication Interactions
Certain medications can interfere with birth control effectiveness. Rifampin (an antibiotic) is the most well-known, but some anticonvulsants and herbal supplements like St. John’s Wort can also interact.
Always tell healthcare providers you’re on birth control when they prescribe new medications.
The Anxiety Factor: Managing Stress Around Missed Pills
Missing a birth control pill can trigger significant anxiety. The fear of unintended pregnancy is real and valid.
Research on real-world contraceptive concerns shows that anxiety around missed doses is one of the top reasons women search for birth control information online.
If you’re feeling anxious, take concrete action: follow the appropriate steps for your pill type, use backup contraception if needed, and consider emergency contraception if the situation warrants it.
Then give yourself permission to move on. Dwelling on what happened doesn’t change the outcome—taking the right steps does.
If you find yourself constantly anxious about missing pills, that’s valuable information. It might mean daily pills aren’t the right contraceptive method for your lifestyle.
When to Contact Your Healthcare Provider
Most missed pill situations don’t require immediately calling your doctor. But certain circumstances do warrant professional guidance.
Contact your healthcare provider if:
- You missed multiple pills and aren’t sure how to proceed
- You experience severe side effects after missing pills
- You think you might be pregnant
- You’re taking medications that might interact with birth control
- You consistently struggle to remember pills and want to discuss alternative contraception
- You miss a period after missing pills
Many providers also offer advice through patient portals or nurse hotlines, which can be faster than scheduling an appointment.
Understanding Your Specific Pill Instructions
Here’s something important: not all birth control pills have identical instructions for missed doses.
The guidance in this article reflects general CDC recommendations and research findings. But your specific pill brand may have particular instructions in the package insert.
Different progestin-only pill formulations have different missed pill protocols.
Always check your pill package insert or consult your pharmacist for brand-specific guidance. When in doubt, follow the most conservative approach: assume you need backup contraception and consider emergency contraception if you had recent unprotected sex.
| Scenario | Required Action | Backup Contraception | Emergency Contraception |
|---|---|---|---|
| 1 combination pill, <24 hours late | Take immediately, continue pack | Not needed | Usually not needed |
| 2+ combination pills missed | Take most recent, skip others | 7 days | Consider if recent sex |
| Progestin-only (>3 hrs late) | Take immediately, continue pack | 48 hours | Consider if recent sex |
| Missed start of new pack (48+ hrs) | Start pack immediately | 7 days | Yes, if recent sex |
| Vomiting within 2 hours of pill | Take another pill | As above if can’t keep down | Depends on timing |
Frequently Asked Questions
For combination pills, you have about 24 hours before effectiveness drops. For progestin-only pills with norethindrone or norgestrel, you only have three hours. Drospirenone progestin-only pills give you 24 hours. Taking a pill even a few hours late doesn’t immediately make it “missed,” but the closer you stick to your scheduled time, the more effective your contraception remains.
Yes, pregnancy is possible but unlikely if you take the missed pill within 24 hours. Sperm can survive in your reproductive tract for up to five days, so sex before missing the pill still carries risk. The risk is highest if you missed a pill in the first week of your pack. Take the missed pill immediately and monitor for your next period. If you’re very concerned, emergency contraception is an option within five days of intercourse.
Yes. According to CDC guidelines, missing two or more combination pills requires backup contraception (like condoms) for seven days after you resume taking pills correctly. For progestin-only pills, you need backup contraception for 48 hours after taking a late pill. This gives your hormone levels time to re-stabilize and restore full contraceptive protection.
Taking two pills in one day to catch up after missing one is safe and recommended. You might experience mild nausea, but this is temporary. Taking pills with food can minimize nausea. Don’t try to take more than two pills in one day—if you missed multiple pills, take only the most recent missed pill and skip the others.
Emergency contraception pills can prevent up to over 95% of pregnancies when taken within five days after unprotected intercourse, according to the World Health Organization. Effectiveness is highest when taken as soon as possible—ideally within 24 hours. The copper IUD, when inserted within five days, is more than 99% effective as emergency contraception and also provides ongoing contraception.
Yes, breakthrough bleeding or spotting is very common after missing pills. The sudden drop in hormone levels can cause the uterine lining to shed partially. This bleeding doesn’t mean your birth control has failed or that you’re pregnant—it’s simply your body responding to hormone fluctuations. The bleeding usually stops once you resume taking pills regularly.
Yes, continue taking your pills even after missing several. Don’t stop mid-pack. Take the most recent missed pill, skip any others, and continue with the rest of your pack on schedule. Use backup contraception for seven days. Stopping your pills entirely would only increase pregnancy risk. If you’re near the end of your pack and missed pills in the last week, consult your package insert or healthcare provider for specific guidance.
Making Informed Decisions About Your Contraception
Missing a birth control pill happens. It doesn’t make you careless or irresponsible. It makes you human.
What matters is knowing how to respond appropriately based on your specific situation. Combination pills and progestin-only pills require different approaches. One missed pill needs different action than three missed pills. The week of your cycle matters.
The research is clear: missed pills do increase pregnancy risk, but following the proper catch-up protocols significantly reduces that risk. According to CDC systematic reviews, even extended hormone-free intervals show relatively low ovulation rates when pills are resumed correctly, though individual responses vary.
If you find yourself frequently missing pills, don’t just push through and hope for the best. Talk to your healthcare provider about whether daily pills are the right contraceptive choice for your life. Long-acting reversible contraception like IUDs and implants eliminate the adherence challenge entirely. There’s no shame in choosing a method that fits your lifestyle better.
The goal isn’t perfect pill-taking—it’s effective pregnancy prevention that works with your real life, not against it.
Keep your pill package insert handy. Set that daily alarm. And if you do miss a pill, refer back to this guide to know exactly what steps to take next. You’ve got this.
