Quick Summary: When you die, your heart stops pumping blood, your brain ceases electrical activity, and your organs shut down sequentially. According to the CDC, approximately 3 million deaths occur annually in the U.S., with heart disease and cancer as leading causes. The dying process involves recognizable physical stages including reduced appetite, breathing changes, and decreased consciousness in the final hours and days.
Death remains one of humanity’s most universal experiences, yet many people don’t understand what actually happens during the process. The biological reality of dying involves a series of predictable physical changes as the body’s systems gradually shut down.
According to the CDC’s most recent mortality data from 2024, approximately 3,072,666 deaths occurred in the United States, representing a death rate of 903.4 deaths per 100,000 population. Life expectancy has reached 79.0 years overall, with females averaging 81.4 years and males 76.5 years.
But what exactly happens during those final moments and the hours leading up to them?
The Leading Causes of Death
Understanding what kills most people provides context for the dying process itself. The CDC tracks the top causes of death annually, revealing patterns in how Americans die.
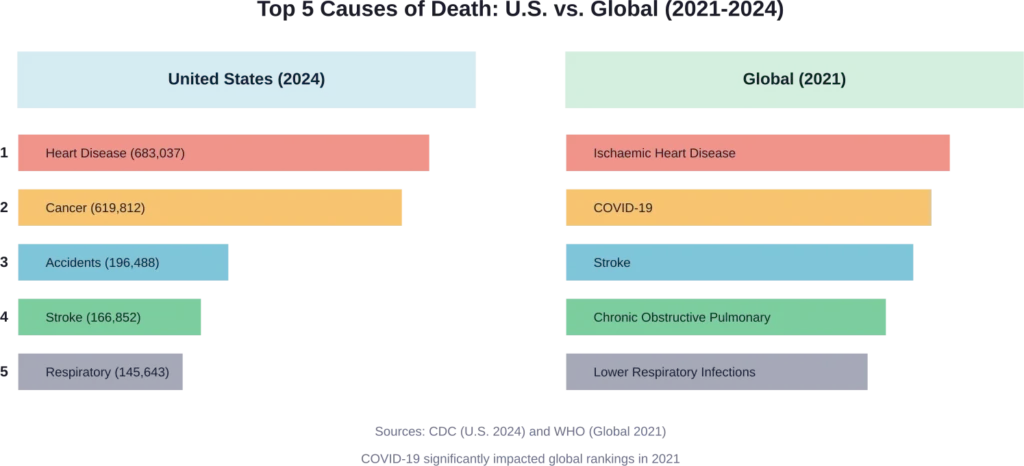
Heart disease remains the number one killer, accounting for 683,037 deaths in 2024. Cancer follows closely behind with 619,812 deaths. Accidents or unintentional injuries claimed 196,488 lives, while stroke accounted for 166,852 deaths.
Globally, the World Health Organization reports that in 2021, the top 10 causes of death accounted for 39 million deaths—57% of the total 68 million deaths worldwide. COVID-19 emerged as the second leading cause globally, directly responsible for 8.8 million deaths in 2021.
| Cause of Death | U.S. Deaths (2024) |
|---|---|
| Heart disease | 683,037 |
| Cancer | 619,812 |
| Accidents | 196,488 |
| Stroke | 166,852 |
| Chronic lower respiratory diseases | 145,643 |
| Alzheimer’s disease | 116,022 |
| Diabetes | 94,445 |
The manner in which death occurs varies dramatically depending on the cause. Sudden cardiac arrest differs significantly from the gradual decline seen in terminal cancer or Alzheimer’s disease.
The Physical Process of Dying
Death marks the moment when vital organs stop working to keep the body alive. But it’s not an instantaneous switch—dying is a process with recognizable stages.
Like giving birth, dying follows a bodily progression with identifiable patterns. Medical professionals who work in hospice and palliative care become familiar with these signs.
Changes in the Last Days
Several days before death, the body begins showing clear signs of decline. Energy levels drop significantly as the body conserves resources for essential functions.
Appetite decreases or disappears entirely. The digestive system requires substantial energy, and as death approaches, the body redirects that energy elsewhere. Many people stop wanting to eat or drink in their final days.
Sleep patterns change dramatically. Dying individuals often sleep most of the day and night, waking only briefly. This drowsiness results from the body’s metabolic changes and the brain’s reduced activity.
Social withdrawal becomes common. Even people who were previously engaged may lose interest in conversation, visitors, or activities they once enjoyed. This isn’t depression—it’s a natural part of the dying process.
Changes in the Last Hours
The final hours bring more pronounced physical changes. Breathing patterns shift noticeably, becoming irregular with pauses between breaths.
This irregular breathing pattern sometimes includes what medical professionals call Cheyne-Stokes respiration—a cycle of shallow breaths followed by deep breaths, then a pause before the pattern repeats.
Body temperature regulation fails. Hands and feet may become cool to the touch as blood circulation decreases. The body prioritizes blood flow to vital organs, reducing circulation to the extremities.
Skin color changes as circulation slows. A bluish or purplish tint may appear on the lips, fingernails, or skin—a condition called cyanosis caused by reduced oxygen in the blood.
Consciousness decreases significantly. Most people become unresponsive in their final hours, though hearing may persist even when they can’t respond. Medical evidence suggests hearing persists even after someone becomes unresponsive.
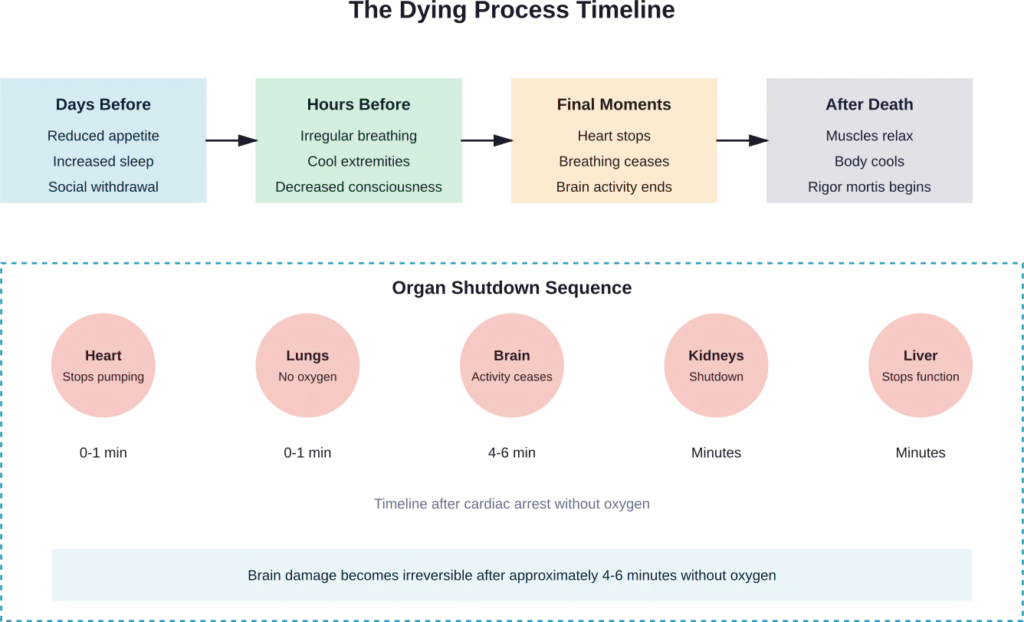
The Moment of Death
Death occurs when the heart stops beating and breathing ceases permanently. Without blood circulation, the brain receives no oxygen and begins to die within minutes.
The heart may stop for several reasons—cardiac arrest, respiratory failure, massive blood loss, or the cumulative effect of disease. Regardless of the trigger, the result is the same: no blood flow means no oxygen delivery to tissues.
Brain cells are extremely sensitive to oxygen deprivation. After about 4-6 minutes without oxygen, brain damage becomes irreversible. Complete brain death follows shortly after if circulation isn’t restored.
Here’s the thing though—different parts of the brain die at different rates. The cerebral cortex, responsible for consciousness and thought, goes first. The brainstem, which controls automatic functions like breathing, may persist slightly longer.
What Determines Legal Death
Medical and legal definitions of death have evolved significantly. Traditionally, death was declared when heartbeat and breathing stopped—called cardiac death.
Modern medicine now recognizes brain death as another criterion. Someone whose brain has completely and irreversibly ceased functioning is legally dead, even if machines maintain heartbeat and breathing.
According to CMS guidelines for hospice care, terminal status is determined when a patient has a life expectancy of six months or less if the disease runs its normal course. Lab testing isn’t required to establish hospice eligibility, though certain markers can indicate disease progression.
Physical Changes After Death
Once death occurs, the body undergoes a series of predictable changes. These post-mortem processes happen in every case, regardless of how death occurred.
Immediately after death, muscles relax completely. This includes sphincters, which may release bladder and bowel contents. The jaw relaxes, eyes may remain partially open, and the body becomes completely limp.
Body temperature begins dropping at a rate of approximately 1.5 degrees Fahrenheit per hour until it reaches room temperature. This cooling process, called algor mortis, helps forensic specialists estimate time of death.
Within 2-6 hours, rigor mortis begins. Chemical changes in muscles cause them to stiffen, starting with the eyelids and jaw, then spreading to larger muscles. This stiffness peaks around 12 hours after death and gradually dissipates over the next 1-3 days.
Blood settles to the lowest points of the body due to gravity, creating purplish discoloration called livor mortis. If someone dies lying on their back, this discoloration appears along the back and buttocks.
What Dying Feels Like
While we can’t know subjective experiences after death, medical professionals have insights into what the dying process feels like based on patient reports and those who’ve been resuscitated.
Many people nearing death report feeling peaceful rather than frightened. Pain management through hospice and palliative care helps minimize physical suffering in the final days.
Drowsiness and reduced consciousness mean most people aren’t fully aware during their final hours. This natural sedation protects individuals from distress.
Does dying hurt? That depends entirely on the cause and circumstances. Sudden death from cardiac arrest may involve brief chest pain. Terminal cancer patients with proper palliative care often experience peaceful deaths with minimal discomfort.
According to hospice workers and medical research, the dying process itself—the actual transition from life to death—appears to be gentle in most cases when symptoms are properly managed.
Terminal Illness and Hospice Care
For individuals with terminal illnesses, hospice care provides comprehensive support focused on comfort rather than cure. Medicare Part A covers hospice benefits for eligible patients.
According to CMS, hospice provides holistic care for terminally ill patients and their families, shifting focus to palliative care for pain relief and symptom management. Patients qualify when their physician certifies a life expectancy of six months or less.
Hospice services include:
- Pain and symptom management
- Medical equipment and supplies
- Medications related to terminal diagnosis
- Nursing care and physician services
- Counseling and spiritual support
- Respite care for family caregivers
For hospice-related medications, patients owe a coinsurance payment of 5% of the drug cost during routine home care or continuous home care.
The Hospice Quality Reporting Program tracks outcomes using data from the Hospice Outcomes and Patient Evaluation (HOPE) assessment, Medicare claims, and patient satisfaction surveys.
Age and Life Expectancy
Death rates and life expectancy vary significantly by age and sex. The CDC’s 2024 data shows life expectancy at birth reached 79.0 years for both sexes combined—81.4 years for females and 76.5 years for males.
But wait. Life expectancy for someone who’s already reached 65 differs from life expectancy at birth. Those who reach 65 can expect an additional 19.7 years on average—20.8 years for females and 18.4 years for males.
| Category | 2023 | 2024 |
|---|---|---|
| Life expectancy (both sexes) | 78.4 years | 79.0 years |
| Life expectancy (females) | 81.1 years | 81.4 years |
| Life expectancy (males) | 75.8 years | 76.5 years |
| At age 65 (both sexes) | 19.5 years | 19.7 years |
Infant mortality remains a critical concern, with 5.52 deaths per 1,000 live births according to the most recent CDC data.
Global Perspectives on Death
Death patterns differ worldwide based on healthcare access, disease prevalence, and socioeconomic factors. The WHO tracks global mortality to identify trends and inform public health policy.
Globally, the top causes of death in 2021 were:
- Ischaemic heart disease
- COVID-19
- Stroke
- Chronic obstructive pulmonary disease
- Lower respiratory infections
- Trachea, bronchus, and lung cancers
- Alzheimer’s disease and other dementias
- Diabetes mellitus
- Kidney diseases
- Tuberculosis
COVID-19’s emergence as the second leading cause globally in 2021 dramatically shifted mortality patterns. The pandemic was directly responsible for 8.8 million deaths that year, pushing other leading causes down in ranking.
Gender differences in mortality are significant. Annual global deaths among women are approximately 13% lower than for men. However, women collectively spend about 26% more years living with disability.
The greatest increase in female deaths over the past two decades has been from Alzheimer’s disease and other dementias, which nearly tripled between 2000 and 2021.
Sudden vs. Expected Death
The dying experience differs dramatically between sudden unexpected death and anticipated death from terminal illness.
Sudden death from accidents, cardiac arrest, or stroke gives individuals no time to prepare. There’s no gradual decline, no final conversations, no opportunity to say goodbye. For the person dying, awareness may be minimal or absent.
Expected death from conditions like cancer or Alzheimer’s disease follows a more predictable trajectory. Families have time to prepare, patients can access hospice care, and the dying process unfolds in stages over days or weeks.
Neither is inherently better or worse—they’re simply different experiences. Sudden death spares individuals from prolonged suffering. Expected death allows time for closure and preparation.
Medical Interventions and End-of-Life Decisions
Modern medicine can sometimes delay death through aggressive interventions. These decisions raise complex ethical questions about quality of life versus quantity of life.
Cardiopulmonary resuscitation can restart the heart after cardiac arrest. Mechanical ventilation can breathe for someone whose lungs have failed. Feeding tubes can provide nutrition when someone can’t eat.
But these interventions don’t always restore quality of life. Someone may survive with severe brain damage or remain dependent on machines indefinitely.
That’s why advance directives and living wills matter. These legal documents specify what interventions someone wants—or doesn’t want—if they become unable to communicate their wishes.
The do-not-resuscitate order tells medical staff not to perform CPR if the heart stops. This choice allows natural death without aggressive intervention.
Frequently Asked Questions
The dying process varies dramatically by cause. Sudden cardiac arrest or traumatic injury can cause death within minutes. Terminal illnesses typically involve gradual decline over weeks or months, with the most recognizable dying signs appearing in the final days and hours before death.
Pain during death depends on the cause and available medical care. Modern hospice and palliative care effectively manage pain for most terminal illnesses. The actual moment of death—when the heart stops and consciousness fades—generally isn’t described as painful by those who’ve been resuscitated. Proper symptom management makes peaceful deaths possible in most cases.
Early signs of dying include significantly decreased appetite and fluid intake, increased sleeping or drowsiness, social withdrawal, and reduced interest in previously enjoyed activities. These changes typically appear days or weeks before death as the body begins shutting down non-essential functions.
Medical evidence suggests hearing persists even after someone becomes unresponsive. Healthcare workers and hospice staff generally believe hearing is the last sense to fade. Many dying individuals who appear unconscious may still hear voices, music, and conversation around them.
Immediately after death, all muscles relax completely, the heart stops pumping blood, and breathing ceases permanently. Body temperature begins dropping at roughly 1.5 degrees Fahrenheit per hour. Within 2-6 hours, rigor mortis causes muscles to stiffen, starting with small muscles and spreading to larger ones.
Brain death occurs when the brain completely and irreversibly stops functioning, including the brainstem that controls automatic functions like breathing. Someone who is brain dead is legally deceased, even if machines maintain heartbeat and circulation. Brain damage becomes irreversible after approximately 4-6 minutes without oxygen.
Physicians determine death by confirming the permanent cessation of heartbeat, breathing, and brain function. Traditional criteria include no pulse, no breathing, no response to stimuli, and fixed dilated pupils. In hospital settings, doctors may use additional tests like electrocardiogram showing no heart activity or electroencephalogram showing no brain waves.
Conclusion
Death remains inevitable, but understanding the process removes some of its mystery. The biological reality involves predictable physical changes as organ systems shut down sequentially.
According to the CDC, over 3 million Americans die annually, with heart disease and cancer as the leading causes. Life expectancy has reached 79 years overall, though significant variation exists by sex, age, and other factors.
The dying process typically follows recognizable stages, particularly in terminal illness. Days before death bring reduced appetite and increased sleep. Hours before death involve irregular breathing and decreased consciousness. The moment of death occurs when the heart stops and brain activity ceases.
Modern hospice care has transformed the dying experience for many, emphasizing comfort and dignity rather than aggressive life-prolonging interventions. Proper symptom management allows most people to die peacefully without severe pain.
Understanding what happens when you die doesn’t make death easy, but it can reduce fear of the unknown. Whether sudden or expected, death represents a natural biological process—the final stage of life that everyone eventually experiences.
Talk to your healthcare provider about advance directives and end-of-life preferences. Having these conversations now ensures your wishes are known and respected when the time comes.
