Quick Summary: Rabies is a fatal viral disease that attacks the nervous system. Once symptoms appear, death typically occurs within days. However, rabies is entirely preventable through immediate post-exposure treatment and vaccination before symptoms develop.
Rabies stands as one of the deadliest viruses known to humanity. According to the CDC, this viral disease is fatal if people don’t receive medical care before symptoms start. But what actually happens when the rabies virus enters the body?
The reality is stark. Once clinical signs appear, rabies is nearly always fatal. The World Health Organization reports that rabies causes tens of thousands of deaths annually, with 40% being children under 15. Dog bites and scratches cause 99% of human rabies cases.
Here’s the thing though—rabies is entirely preventable. Around 100,000 Americans are vaccinated against rabies following a potential exposure each year. Understanding what happens if you contract rabies explains why immediate treatment is absolutely critical.
How Rabies Virus Enters and Travels Through the Body
The rabies virus (RABV) is transmitted through the saliva of infected animals. According to the CDC, transmission occurs through bites or scratches from infected mammals, contaminating open skin or mucous membranes. In rare cases, organ transplantation has transmitted the virus.
Once the virus enters the body, it doesn’t immediately spread through the bloodstream like many other viruses. Instead, rabies employs a more insidious strategy.
The virus replicates at the wound site, then travels along peripheral nerves toward the central nervous system. This neural pathway is what makes rabies so deadly—and also why there’s a window for treatment before symptoms appear.
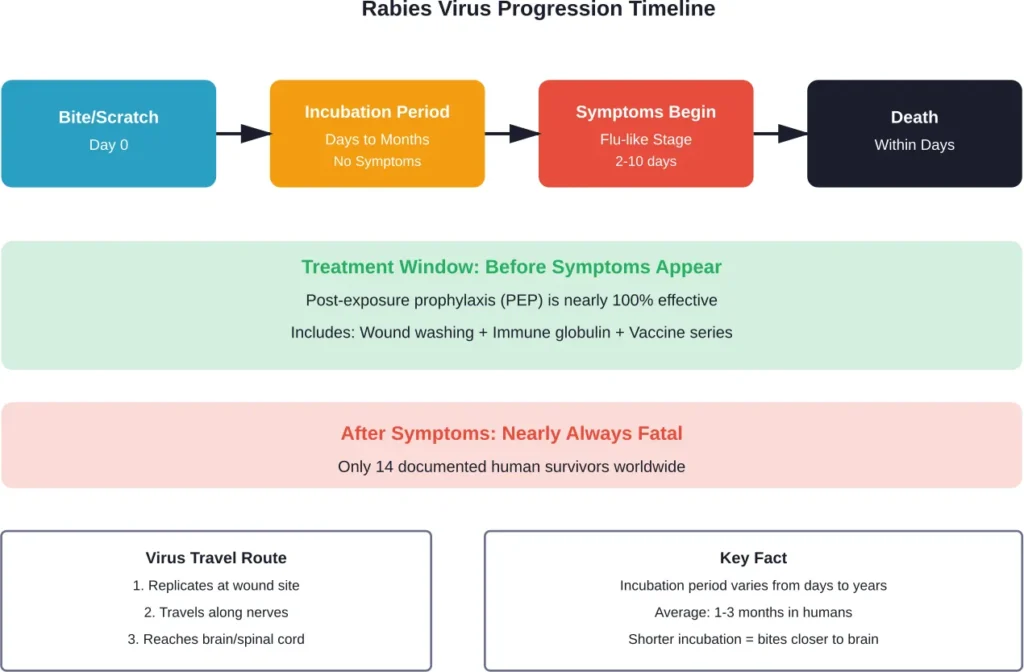
The Incubation Period: Silent and Unpredictable
Following an incubation period ranging from a few days to a few years, rabies presents with symptoms. According to the StatPearls medical database, the average incubation period is 1-3 months, though this varies considerably.
Several factors influence incubation length:
- Location of the bite (closer to the brain means shorter incubation)
- Severity of the wound
- Amount of virus introduced
- Viral strain involved
During this period, infected individuals feel completely normal. No symptoms appear. No warning signs emerge. The virus silently travels toward the brain.
This is the critical window where post-exposure prophylaxis (PEP) works. According to the CDC, rabies can be prevented before and after exposure through vaccines and immune globulin. Once symptoms begin, treatment options become extremely limited.
Stage One: Early Symptoms That Mimic Common Illnesses
The first symptoms of rabies are frustratingly nonspecific. According to the CDC, these may include:
- Flu-like illness including weakness or discomfort
- Fever or headache
- Discomfort, prickling, or itching sensation at the bite site
Additional early signs documented by medical researchers include:
- Sore throat
- Stiff muscles
- Loss of appetite
- Nausea
- Depression
Real talk: these symptoms could indicate dozens of different conditions. That’s precisely what makes rabies so dangerous in this stage. Many people don’t connect these vague symptoms to an animal bite that occurred weeks or months earlier.
Pain, itching, or tingling at the bite site is the most distinctive early symptom. This occurs as the virus reaches nerve endings. But even this symptom isn’t universal.
This early stage typically lasts 2-10 days. Medical intervention is still possible during this window, though effectiveness decreases as neurological symptoms progress.
Stage Two: Neurological Symptoms and Two Clinical Forms
Usually, severe disease appears within 2 weeks of the first symptoms, according to the CDC. Once rabies virus reaches the brain and spinal cord, it causes acute encephalitis—inflammation of the brain.
The World Health Organization identifies two distinct clinical forms:
Furious Rabies (80% of Human Cases)
This is the “classic” rabies that most people are familiar with. Symptoms include:
- Hyperactivity and agitation
- Hallucinations
- Hydrophobia (fear of water)
- Aerophobia (fear of drafts or fresh air)
- Difficulty swallowing
- Excessive salivation
- Confusion and disorientation
- Bizarre behavior
Hydrophobia deserves special attention. It’s not actually a fear of water itself. Attempting to drink triggers painful spasms of the throat muscles. Patients become terrified of drinking because of the excruciating pain it causes. Even seeing water can trigger anxiety and spasms.
Paralytic Rabies (20% of Human Cases)
According to the WHO, paralytic rabies runs a less dramatic and usually longer course than furious rabies. This form features:
- Gradual muscle paralysis, starting at the bite site
- Slow progression to coma
- Less obvious symptoms initially
- Often misdiagnosed as other conditions
The paralytic form is particularly dangerous because it’s frequently unrecognized. Medical professionals may not immediately suspect rabies, delaying proper precautions and public health interventions.

Stage Three: Coma and Death
Both forms of rabies progress to coma. According to the WHO, death occurs after a few days due to cardio-respiratory arrest.
From symptom onset to death typically takes 2-10 days, though paralytic rabies may last slightly longer. Medical research documents that death typically occurs within 2 to 3 days of coma onset.
The neurological damage is catastrophic. The virus destroys neurons throughout the brain and spinal cord. Multiple organ systems fail. The autonomic nervous system—which controls breathing, heart rate, and other vital functions—ceases to function properly.
Treatment at this stage focuses on comfort care. According to the CDC, once symptoms begin, treatment typically focuses on minimizing the patient’s pain and suffering. In resource-poor countries, many individuals die at home.
Can Anyone Survive Rabies After Symptoms Appear?
The short answer? Extraordinarily rarely.
Medical literature documents only approximately 14 documented human survivors worldwide who developed symptoms. That’s out of tens of thousands of annual deaths. The survival rate is effectively zero.
The so-called “Milwaukee Protocol”—an experimental treatment involving induced coma and antiviral medications—has been attempted numerous times with minimal success. Most patients who receive this protocol still die. The few survivors often suffer severe, permanent neurological damage.
This underscores a critical point: rabies prevention must happen before symptoms appear. Waiting for symptoms is waiting for death.
Post-Exposure Prophylaxis: The Life-Saving Treatment
Here’s where the story becomes hopeful. According to the CDC, rabies post-exposure prophylaxis includes wound washing, human rabies immune globulin, and a four-dose series of vaccines.
PEP is nearly 100% effective when administered promptly and correctly. This treatment has saved countless lives.
The PEP Protocol
| Treatment Component | Purpose | Timing |
|---|---|---|
| Immediate wound washing | Remove virus from wound site | As soon as possible after exposure |
| Human rabies immune globulin (HRIG) | Provides immediate antibodies | Day 0 (first visit) |
| Rabies vaccine dose 1 | Stimulate immune response | Day 0 |
| Rabies vaccine dose 2 | Boost immunity | Day 3 |
| Rabies vaccine dose 3 | Further boost immunity | Day 7 |
| Rabies vaccine dose 4 | Complete immunization | Day 14 |
According to the CDC, patients should wash the wound right away with soap and water, using a 10% povidone-iodine solution if available. This simple step significantly reduces viral load at the exposure site.
Immune globulin provides immediate passive immunity—borrowed antibodies that attack the virus while the body develops its own response. The vaccine series teaches the immune system to recognize and destroy rabies virus.
Side Effects of Treatment
The CDC notes that approximately 6% of people experience mild reactions. Common side effects include:
- Pain, itching, or swelling at injection site
- Headache
- Nausea
- Muscle aches
- Dizziness
- Abdominal pain
These mild reactions are infinitely preferable to rabies infection. Serious side effects are rare.
Who Needs Pre-Exposure Prophylaxis
Some people face elevated rabies risk due to their occupation or travel plans. According to the CDC, certain people should receive pre-exposure prophylaxis (PrEP).
PrEP candidates include:
- Veterinarians and veterinary staff
- Animal control officers
- Wildlife rehabilitators
- Laboratory workers handling rabies virus
- Travelers to rabies-endemic areas with limited access to medical care
- People living in areas with endemic dog rabies
PrEP consists of a two-dose vaccine series. It doesn’t eliminate the need for PEP after an exposure, but it simplifies treatment. Those who received PrEP don’t need immune globulin and require fewer vaccine doses.
Animals That Commonly Carry Rabies
According to the CDC, the animals most frequently found with rabies in the United States are bats, skunks, raccoons, and foxes. Dog bites represent less than 10% of all animal rabies recorded in the U.S. and Europe, where domestic animal rabies was largely controlled during the 1940-50s.
Globally, the picture differs dramatically. The WHO reports that dog bites and scratches cause 99% of human rabies cases worldwide, particularly in Asia and Africa.
| Region | Primary Rabies Reservoir | Human Risk Level |
|---|---|---|
| United States | Bats, raccoons, skunks, foxes | Low (domestic animals controlled) |
| Europe | Wildlife (bats, foxes) | Low (domestic animals controlled) |
| Asia | Dogs | High (endemic dog rabies) |
| Africa | Dogs | High (endemic dog rabies) |
| Latin America | Dogs, bats | Moderate to High |
Bat exposure requires special consideration. Bat bites may be nearly invisible. People who wake up to find a bat in their room should seek medical evaluation, even without an obvious bite. Bat teeth are small enough that bites can occur without the person realizing it.
When to Seek Medical Care Immediately
According to the WHO, if a person is bitten or scratched by a potentially rabid animal, they should immediately and always seek PEP care.
Seek immediate medical attention if:
- Any wild animal bites or scratches occurred
- A bat touched the skin or was in the room with a sleeping person
- An unprovoked domestic animal attack happened
- A stray dog or cat bite occurred, especially in rabies-endemic areas
- Any animal bite broke the skin
- Saliva from a potentially rabid animal contacted mucous membranes or open wounds
Don’t wait to see if symptoms develop. Don’t wait to see if the animal can be tested. According to the CDC, contact the health department immediately for a risk assessment to determine eligibility for post-exposure prophylaxis.
Time is critical. The virus is traveling toward the brain. Every hour counts.
Frequently Asked Questions
The incubation period for rabies typically ranges from 1-3 months but can vary from a few days to several years in rare cases. The virus is not truly “dormant” during this time—it’s actively traveling along nerves toward the brain, but no symptoms appear. The incubation length depends on factors including bite location, severity, and viral load.
No. Rabies is nearly always fatal once clinical symptoms develop. Only approximately 14 documented human survivors worldwide have survived symptomatic rabies, and most survivors suffered severe permanent neurological damage. Once symptoms begin, treatment focuses on comfort care rather than cure. This is why prevention before symptoms appear is absolutely critical.
The first symptoms are often nonspecific and flu-like: fever, headache, weakness, nausea, and general discomfort. The most distinctive early symptom is pain, tingling, or itching at the bite site, which occurs as the virus reaches nerve endings. These initial symptoms typically last 2-10 days before progressing to severe neurological symptoms.
Post-exposure prophylaxis (PEP) is nearly 100% effective when administered promptly and correctly. The treatment includes wound washing, immune globulin, and a four-dose vaccine series. Effectiveness depends on receiving treatment before symptoms appear and following the complete protocol. Delays in treatment or incomplete vaccination reduce effectiveness.
Yes. Rabies virus is present in the saliva of infected animals. If an animal’s saliva contacts broken skin—even a minor scratch that doesn’t bleed significantly—transmission is possible. Scratches that break the skin surface require medical evaluation and potential PEP, according to CDC guidelines.
Hydrophobia (fear of water) develops because the virus affects the throat muscles and swallowing reflex. Attempting to drink triggers extremely painful spasms of the throat and respiratory muscles. Patients develop anxiety and fear around drinking because of the excruciating pain it causes. Eventually, even seeing or thinking about water can trigger spasms and panic.
Some countries are categorized as rabies virus-free, though some of these are endemic for related viruses like Australian bat lyssavirus. Antarctica is the only continent completely free of rabies. Island nations with strict quarantine policies, such as Japan, Australia, and the United Kingdom, have eliminated terrestrial rabies, though bat-related lyssaviruses may still be present in some regions.
The Bottom Line: Prevention Is Everything
What happens if someone contracts rabies without treatment is a progression toward certain death. The virus methodically destroys the nervous system, causing either furious or paralytic rabies, then coma, then death within days of symptom onset.
But here’s the critical takeaway: this outcome is entirely preventable.
Rabies represents a unique situation in infectious disease. It’s nearly 100% fatal once symptoms appear, yet nearly 100% preventable with prompt treatment. The vaccines and immune globulin that prevent rabies death have been available for decades.
If an animal bite or scratch occurs—particularly from wildlife or an unknown animal—seek medical evaluation immediately. Contact the local health department for risk assessment. Don’t wait. Don’t assume the animal was healthy. Don’t gamble with the virus that has claimed countless lives throughout human history.
According to the CDC’s clinical guidelines, rabies is fatal if it’s untreated before symptoms start. That single sentence contains both the terror and the hope of this disease. The terror: once symptoms begin, death is virtually inevitable. The hope: treatment before symptoms provides near-certain survival.
For travelers to rabies-endemic areas, consider pre-exposure vaccination. For those who work with animals, PrEP is essential protection. For everyone: understand that rabies remains a serious public health threat in over 150 countries and territories worldwide.
The rabies virus has killed humans for millennia. Modern medicine has provided the tools to prevent every single death. Using those tools requires only one thing: seeking treatment immediately after potential exposure, before the virus reaches the brain and symptoms begin.
That window of opportunity is the difference between life and certain death.
