Quick Summary: Having too much calcium in your blood, called hypercalcemia, can cause kidney stones, bone weakness, heart rhythm problems, and neurological symptoms. This condition is usually caused by overactive parathyroid glands or certain cancers, not dietary calcium intake. Treatment depends on severity and may include hydration, medications, or surgery to address the underlying cause.
Calcium keeps bones strong and helps muscles contract. But when blood calcium levels climb too high, the body faces serious problems.
Most people worry about getting too much calcium from supplements or diet. Here’s the thing though—hypercalcemia rarely comes from what you eat. The real culprits are usually medical conditions affecting how the body regulates calcium.
According to research, high-dose calcium supplements do not typically cause hypercalcemia in healthy adults. Research supported by the NIH-funded Vitamin D and Omega-3 Trial (VITAL) examined vitamin D supplementation at doses of at least 1,000 IU don’t typically cause hypercalcemia in healthy adults. The body tightly controls calcium levels through complex hormonal systems.
Understanding Hypercalcemia and Calcium Levels
Hypercalcemia means elevated calcium in the bloodstream. The condition gets classified by severity based on serum calcium measurements.
Normal serum calcium levels are typically around 8.5-10.5 mg/dL, though reference ranges may vary by laboratory. According to StatPearls, hypercalcemia is categorized as:
| Severity Level | Calcium Range (mg/dL) | Clinical Significance |
|---|---|---|
| Mild | Just above normal but <12 | Often asymptomatic, may not require immediate treatment |
| Moderate | 12 to 14 | Symptoms typically present, treatment usually needed |
| Severe | Above 14 | Medical emergency requiring urgent intervention |
Research from a prospective study published in Endocrine Connections found that hypercalcemia affects only 0.19% of emergency department patients. But that doesn’t make it any less serious when it occurs.
Approximately 40% to 45% of serum calcium binds to albumin. This means calcium levels can fluctuate based on protein levels in the blood, which is why doctors often measure ionized (free) calcium for accurate assessment.
What Causes Too Much Calcium in Blood
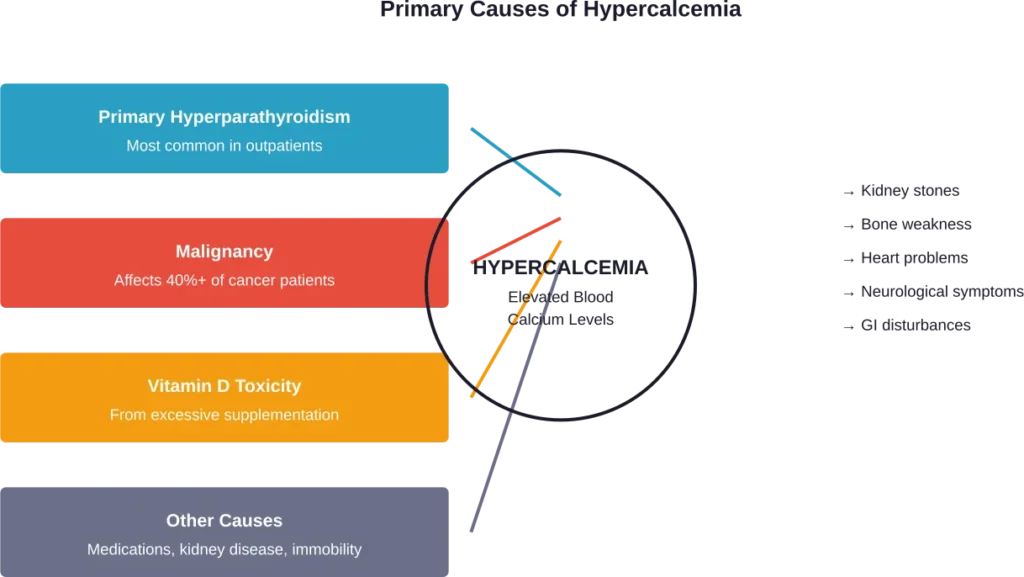
Two conditions account for the vast majority of hypercalcemia cases: primary hyperparathyroidism and malignancy.
Primary Hyperparathyroidism
The four tiny parathyroid glands sit behind the thyroid. They produce parathyroid hormone (PTH), which regulates calcium levels.
When these glands become overactive—usually due to a benign tumor—they pump out too much PTH. This pulls calcium from bones into the bloodstream.
A case report published in Cureus described a 75-year-old woman with undiagnosed primary hyperparathyroidism who developed severe complications including seizures. After diagnosis, treatment with fluid therapy and zoledronic acid resolved her symptoms.
Cancer-Related Hypercalcemia
According to research in Cells, hypercalcemia affects over 40% of cancer patients at some point during their illness. Both solid tumors and blood cancers can trigger elevated calcium levels.
Cancers cause hypercalcemia through two main mechanisms: releasing substances that mimic PTH or directly destroying bone tissue through metastases.
Other Causes
Less common causes include:
- Excessive vitamin D intake (vitamin D toxicity)
- Certain medications, particularly thiazide diuretics
- Prolonged immobilization
- Chronic kidney disease
- Granulomatous diseases like sarcoidosis
The National Kidney Foundation notes that kidney disease creates mineral and bone disorders that can affect calcium regulation as kidney function declines.
Symptoms and Warning Signs
Mild hypercalcemia often produces no symptoms. As levels rise, symptoms emerge across multiple body systems.
The medical community sometimes describes hypercalcemia symptoms with the phrase “stones, bones, groans, and psychiatric overtones.”
Kidney and Urinary Symptoms
Excessive calcium gets filtered through kidneys, leading to:
- Kidney stones (calcium deposits)
- Increased urination
- Excessive thirst
- Kidney damage or failure in severe cases
The National Kidney Foundation identifies calcium kidney stones as the most common type. High blood calcium contributes significantly to stone formation.
Bone and Muscle Effects
When parathyroid problems cause hypercalcemia, calcium leaches from bones into blood. This creates:
- Bone pain and tenderness
- Increased fracture risk
- Muscle weakness
- Joint aches
Neurological and Psychiatric Symptoms
The case report in Cureus documented generalized tonic-clonic seizures as a complication of severe hypercalcemia. Other neurological manifestations include:
- Confusion and disorientation
- Memory problems
- Depression
- Fatigue and lethargy
- In extreme cases, coma
Gastrointestinal Issues
High calcium affects the digestive system, causing:
- Nausea and vomiting
- Constipation
- Abdominal pain
- Loss of appetite
Cardiovascular Complications
Calcium affects heart function. Elevated levels can trigger:
- Irregular heart rhythms (arrhythmias)
- High blood pressure
- In severe cases, cardiac arrest
Research from the Atherosclerosis Risk in Communities Study examined calcium-phosphate levels and cardiovascular disease connections in community-dwelling adults.
Diagnosis and Testing
Doctors diagnose hypercalcemia through blood tests measuring total and ionized calcium levels. Because albumin affects calcium readings, healthcare providers often calculate albumin-adjusted calcium.
Once hypercalcemia is confirmed, additional tests identify the cause:
- Parathyroid hormone (PTH) levels
- Vitamin D levels
- Kidney function tests
- Bone density scans
- Imaging studies to check for tumors
Treatment Options and Management
Treatment depends on severity and underlying cause. Mild cases may require only monitoring.
Immediate Management
For moderate to severe hypercalcemia, initial treatment focuses on lowering calcium levels:
- Hydration: Intravenous fluids help kidneys flush excess calcium
- Bisphosphonates: Medications like zoledronic acid prevent bone calcium release
- Calcitonin: Hormone that rapidly lowers calcium (short-term effect)
- Diuretics: Certain types increase calcium excretion
Treating Underlying Causes
Long-term management addresses root causes:
Primary Hyperparathyroidism: Surgery to remove overactive parathyroid glands often cures the condition permanently. Parathyroid surgery has high success rates when performed by experienced surgeons.
Cancer-Related Hypercalcemia: Treatment targets the underlying malignancy. Research indicates malignancy-related hypercalcemia significantly impacts prognosis and requires comprehensive palliative care planning.
Medication-Induced: Discontinuing or adjusting problematic medications resolves many cases.
Vitamin D Toxicity: Stopping supplements and limiting dietary vitamin D allows levels to normalize gradually.
Can Dietary Calcium Cause Hypercalcemia?
Real talk: dietary calcium almost never causes hypercalcemia in people with normal parathyroid and kidney function.
Harvard Health notes that concerns about calcium supplements focus on other issues—like kidney stone risk and poor micronutrient absorption—not hypercalcemia itself.
The body tightly regulates calcium absorption from food. When intake increases, absorption efficiency decreases. Excess dietary calcium simply passes through the digestive system.
That said, the National Kidney Foundation recommends aiming for about 2,300 mg of sodium per day and getting adequate calcium from food sources rather than excessive supplementation.
Prevention and Risk Reduction
While some causes of hypercalcemia can’t be prevented, certain strategies reduce risk:
- Avoid excessive calcium and vitamin D supplementation without medical guidance
- Stay hydrated, especially during illness or hot weather
- Maintain regular physical activity (immobilization increases calcium release from bones)
- Monitor calcium levels if at risk due to cancer or kidney disease
- Follow up on abnormal blood work promptly
For people with chronic kidney disease, the National Kidney Foundation emphasizes that almost everyone with kidney disease develops some mineral or bone disorder. Regular monitoring becomes essential.
Prognosis and Long-Term Outlook
The prognosis for hypercalcemia varies dramatically based on the underlying cause.
Primary hyperparathyroidism treated with surgery typically has excellent outcomes. Most patients experience complete resolution of symptoms and normal calcium levels afterward.
Cancer-related hypercalcemia carries a more serious prognosis. Studies on survival outcomes indicate it serves as a significant predictor of unfavorable outcomes in cancer patients.
Early detection and treatment prevent complications. Left untreated, severe hypercalcemia can cause permanent kidney damage, severe bone loss, and life-threatening cardiac events.
Frequently Asked Questions
No. Dietary calcium from milk or other foods rarely causes hypercalcemia in healthy individuals. The body regulates calcium absorption efficiently, and excess dietary calcium is excreted rather than absorbed.
According to medical literature, calcium levels above 14 mg/dL are considered severe hypercalcemia requiring urgent treatment. Levels between 12-14 mg/dL are moderate and typically need medical intervention. However, even mildly elevated levels warrant investigation to identify the underlying cause.
Mild to moderate hypercalcemia often responds to treatment within 24-48 hours with intravenous hydration and medications. Severe cases may take several days. Long-term correction depends on addressing the underlying cause, which may require surgery or cancer treatment.
Severe hypercalcemia (above 14 mg/dL) with symptoms is a medical emergency. A prospective study found that while immediately life-threatening complications are relatively rare, severe cases can cause cardiac arrhythmias, altered mental status, or coma requiring urgent intervention.
Yes, if left untreated. Chronic hypercalcemia can cause irreversible kidney damage, severe bone loss, and cardiovascular complications. Early detection and treatment prevent most permanent complications.
Consult your healthcare provider before stopping any supplements. In most cases, hypercalcemia isn’t caused by dietary supplements, so stopping them may not resolve the issue. Medical evaluation to identify the underlying cause is essential.
Hypercalcemia means too much calcium in the blood, while hypocalcemia means too little. Both conditions cause serious health problems but have opposite causes and require different treatments. Symptoms also differ—hypocalcemia typically causes muscle spasms and tingling, while hypercalcemia causes the symptoms described in this article.
Conclusion
Too much calcium in the blood isn’t about drinking too much milk or taking reasonable supplements. Hypercalcemia typically signals an underlying medical condition requiring diagnosis and treatment.
The condition affects multiple body systems—from kidneys and bones to heart and brain. Early recognition of symptoms allows timely intervention before complications develop.
If experiencing unexplained fatigue, increased thirst, frequent urination, bone pain, or confusion, blood calcium testing should be part of the diagnostic workup. With proper treatment targeting the root cause, most people with hypercalcemia can achieve normal calcium levels and prevent long-term complications.
Don’t ignore persistent symptoms or abnormal lab results. Contact a healthcare provider for proper evaluation and personalized treatment recommendations.
