Quick Summary: Stopping Farxiga (dapagliflozin) doesn’t cause withdrawal symptoms, but your underlying condition—Type 2 diabetes, heart failure, or chronic kidney disease—may worsen without it. Blood sugar levels can rise within days, and the medication’s protective cardiovascular and kidney benefits will gradually diminish. Always consult your healthcare provider before discontinuing Farxiga to discuss alternatives and ensure safe management of your condition.
Farxiga (dapagliflozin) has become a cornerstone treatment for millions managing Type 2 diabetes, heart failure, and chronic kidney disease. But what happens when someone stops taking it?
Unlike some medications that trigger uncomfortable withdrawal symptoms, Farxiga doesn’t work that way. The real concern isn’t what your body goes through when the drug leaves—it’s what happens to the conditions Farxiga was controlling.
Here’s the thing though—Farxiga isn’t just managing symptoms. According to clinical trials including the DAPA-CKD study, this medication actively reduces the risk of serious complications. When it’s removed from the equation, those protective benefits disappear.
Understanding How Farxiga Works in Your Body
Farxiga belongs to a class of medications called SGLT2 inhibitors. These drugs work differently than traditional diabetes medications.
Instead of forcing your pancreas to produce more insulin or making your cells more sensitive to it, Farxiga targets your kidneys. It blocks a protein called sodium-glucose cotransporter-2, which normally reabsorbs glucose back into your bloodstream.
By inhibiting this protein, Farxiga causes your kidneys to flush excess glucose out through urine. This lowers blood sugar levels naturally. The medication also reduces fluid retention and blood pressure, which explains why it helps with heart failure and kidney disease beyond just diabetes management.
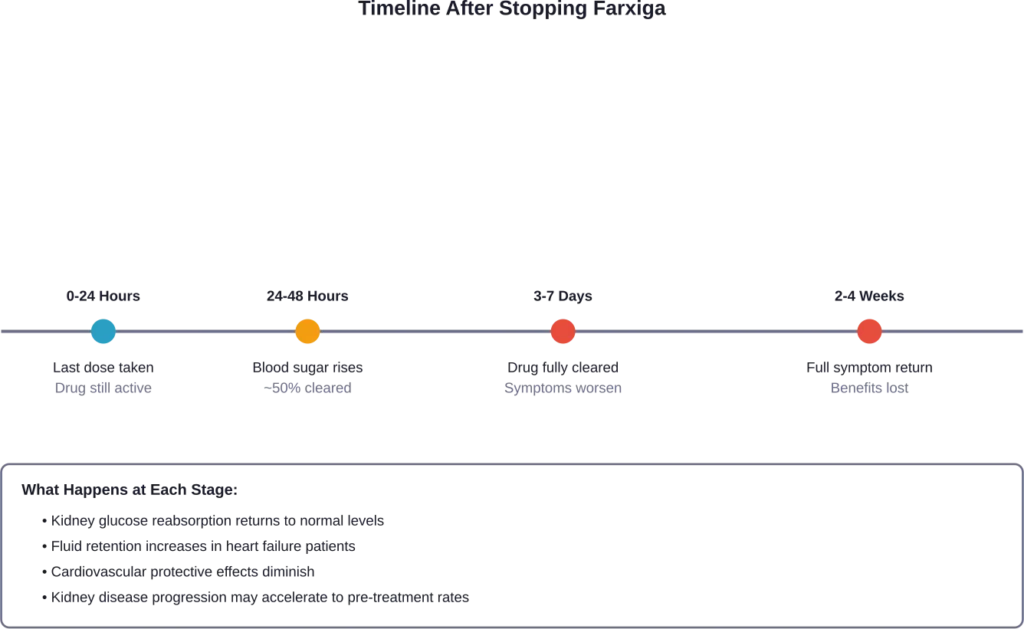
The drug has an elimination half-life of approximately 13 hours. That means every 13 hours, about half of the medication leaves your system. Within roughly three days after your last dose, Farxiga is essentially cleared from your body.
But the effects on your condition? Those change on a different timeline.
What Happens When You Stop Taking Farxiga
The absence of withdrawal symptoms doesn’t mean stopping is without consequences. Your body won’t rebel against the lack of medication, but your underlying condition will.
Blood Sugar Changes (Type 2 Diabetes)
For people taking Farxiga for Type 2 diabetes, blood glucose levels typically begin rising within 24 to 48 hours after discontinuation.
Clinical studies show that dapagliflozin effectively lowers HbA1c by approximately 0.66% compared to placebo, with canagliflozin showing approximately 0.91%. When the medication stops, this benefit reverses. Blood sugar control deteriorates gradually as glucose reabsorption in the kidneys returns to previous patterns.
Some patients notice symptoms of hyperglycemia returning—increased thirst, frequent urination, fatigue, and blurred vision. These signs indicate blood sugar levels are climbing back to pre-treatment ranges.
Heart Failure Progression
The cardiovascular benefits of Farxiga are well-documented. The DELIVER Phase III trial demonstrated that Farxiga significantly reduces the risk of cardiovascular death or worsening heart failure in patients with preserved ejection fraction.
When discontinued, the medication’s protective effects on the heart gradually diminish. Fluid retention may increase as the kidneys resume normal sodium and water reabsorption. This can lead to weight gain, swelling in the legs and ankles, and increased shortness of breath.
Heart failure symptoms that were previously controlled—like difficulty breathing during activities or while lying down—may return or worsen within days to weeks.
Kidney Function Decline
Among patients with chronic kidney disease, regardless of the presence or absence of diabetes, the DAPA-CKD trial showed that the risk of a sustained decline in estimated glomerular filtration rate (eGFR) of at least 50%, end-stage kidney disease, or death from renal or cardiovascular causes was significantly lower with dapagliflozin than with placebo.
Stopping Farxiga removes this protective layer. The medication’s ability to slow chronic decline of eGFR disappears. While kidney function won’t collapse overnight, the progressive deterioration that Farxiga was slowing may accelerate back to its natural course.
Protein in the urine (proteinuria) may also increase after discontinuation, as research shows dapagliflozin reduces proteinuria in non-diabetic patients with chronic kidney disease.
Can You Stop Taking Farxiga Suddenly?
Technically, yes. Farxiga can be stopped abruptly without causing physical withdrawal symptoms or dangerous rebound effects.
But should you? That’s a different question entirely.
Stopping suddenly means losing the medication’s benefits all at once. Your blood sugar, heart function, and kidney protection don’t taper off—they simply revert to their unmedicated state as the drug clears your system.
Medical guidelines don’t require a gradual taper for Farxiga like they do for some other medications. However, abrupt discontinuation should only happen under medical supervision, particularly if you’re experiencing side effects or have been advised to stop due to other health changes.
The safest approach involves working with healthcare providers to either transition to an alternative medication or implement other management strategies before discontinuing Farxiga.
When Should You Consider Stopping Farxiga?
Not everyone stays on Farxiga indefinitely. Several legitimate reasons exist for discontinuation.
Serious Side Effects
According to official prescribing information, Farxiga carries risks of serious side effects that may warrant stopping the medication:
- Ketoacidosis: A dangerous buildup of acids in the blood that can occur even with normal blood sugar levels
- Serious urinary tract infections: Including kidney infections (pyelonephritis) that may lead to hospitalization
- Genital mycotic infections: According to official prescribing information, female genital mycotic infections occur in approximately 8.4% of female patients taking FARXIGA 5 mg and 10 mg doses combined (compared to 6.9% with placebo and 1.5% with control)
- Low blood pressure: Particularly problematic for patients already on blood pressure medications
- Acute kidney injury: Sudden worsening of kidney function
If any of these occur, healthcare providers may recommend discontinuing Farxiga immediately.
Medical Conditions That Require Stopping
Certain medical situations require temporary or permanent discontinuation:
- Scheduled surgery or medical procedures
- Severe illness, dehydration, or prolonged fasting
- Declining kidney function below safe thresholds
- Pregnancy (Farxiga is not recommended during pregnancy)
Cost and Access Issues
Real talk: medication costs matter. Some patients discontinue Farxiga due to affordability concerns.
Community discussions reveal that pricing can be a barrier. While the official Farxiga website mentions a savings card that may reduce costs to $0 per month for eligible patients, not everyone qualifies for such programs.
| Reason for Stopping | Timeline for Discontinuation | Alternative Needed? |
|---|---|---|
| Serious side effects (ketoacidosis, severe infection) | Immediate | Yes—different medication class |
| Scheduled surgery | 3-4 days before procedure | Temporary—may resume after |
| Acute kidney injury | Immediate | Yes—after kidney function stabilizes |
| Cost/affordability | After discussing with provider | Yes—lower-cost alternative |
| Pregnancy | Immediate upon confirmation | Yes—pregnancy-safe options |
Alternatives to Farxiga
If discontinuing Farxiga becomes necessary, several alternatives exist depending on your primary condition.
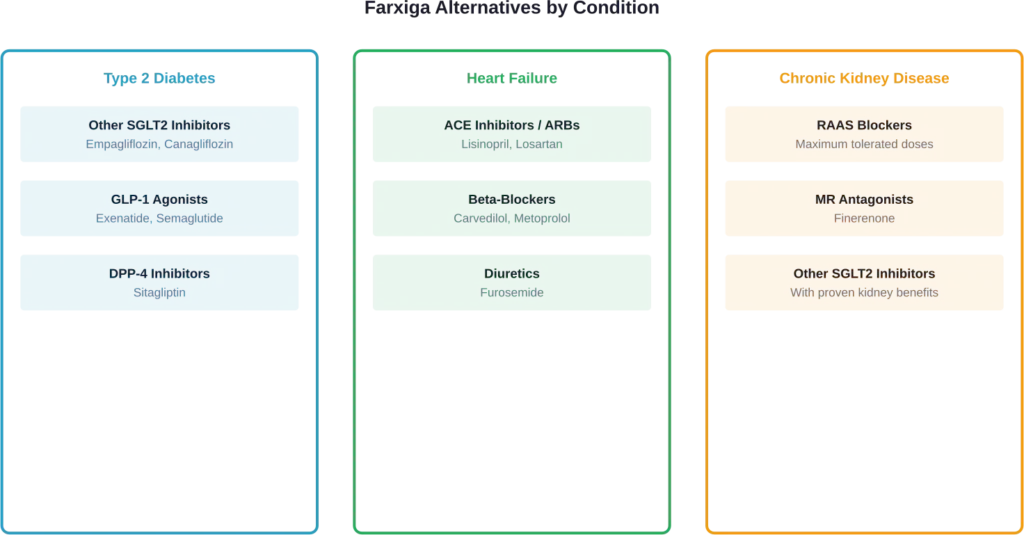
For Type 2 Diabetes
Other SGLT2 inhibitors offer similar mechanisms of action:
- Canagliflozin (Invokana): Lowers HbA1c by approximately 0.91% compared to placebo, with similar cardiovascular benefits
- Empagliflozin (Jardiance): Shows significant reduction in all-cause mortality after three years in clinical trials
Different medication classes include sulfonylureas like glipizide and glyburide, which help the pancreas produce more insulin, or DPP-4 inhibitors that work through different pathways.
For Heart Failure
Heart failure management often involves multiple medications. Alternatives or additions might include:
- ACE inhibitors or ARBs (angiotensin receptor blockers)
- Beta-blockers
- Mineralocorticoid receptor antagonists like finerenone, which shows promise in diabetic kidney disease
- Diuretics for fluid management
For Chronic Kidney Disease
Kidney disease management focuses on slowing progression and managing complications:
- Renin-angiotensin-aldosterone system (RAAS) blockers at maximum tolerated doses
- Other SGLT2 inhibitors with proven kidney benefits
- Blood pressure control medications
- Dietary modifications and protein restriction
How to Safely Stop Taking Farxiga
The safest discontinuation strategy starts with a conversation, not a decision.
Step 1: Consult Your Healthcare Provider
Before stopping Farxiga, schedule an appointment to discuss your concerns. Whether it’s side effects, cost issues, or other reasons, your provider needs to know.
They’ll evaluate your current health status, assess why you’re taking Farxiga, and determine whether stopping is appropriate or if adjustments might address your concerns.
Step 2: Develop a Transition Plan
If discontinuation is warranted, work with your provider to create a plan that might include:
- Starting an alternative medication before stopping Farxiga
- Increasing doses of other medications you’re already taking
- Implementing lifestyle modifications to compensate for the loss of Farxiga’s benefits
- Scheduling follow-up appointments to monitor your condition
Step 3: Monitor Your Symptoms
After stopping Farxiga, pay close attention to changes in your body. Track:
- Blood glucose levels (if diabetic)—check more frequently for the first week
- Weight changes (sudden gains may indicate fluid retention)
- Breathing difficulty or reduced exercise tolerance (heart failure patients)
- Swelling in legs, ankles, or feet
- Changes in urination frequency or appearance
Step 4: Have a Backup Plan
Know the warning signs that require immediate medical attention and when to contact your healthcare provider versus when to seek emergency care.
When to Call Your Healthcare Provider
Contact your doctor if you experience any of these changes after stopping Farxiga:
- Blood sugar levels consistently above your target range
- Weight gain of more than 2-3 pounds in a day or 5 pounds in a week
- Increased shortness of breath or difficulty breathing
- New or worsening swelling in extremities
- Decreased urine output or changes in urine color
- Persistent fatigue or weakness
Seek immediate emergency care for:
- Severe difficulty breathing or chest pain
- Confusion or extreme drowsiness
- Signs of ketoacidosis (nausea, vomiting, abdominal pain, fruity-smelling breath)
- Symptoms of severe dehydration
Real Patient Experiences
Some patients report subjective experiences of feeling unwell when missing doses or stopping the medication, as noted in patient communities. Others describe a return of previous symptoms—increased thirst, frequent urination, and fatigue—within days of discontinuation.
One pattern that emerges from these discussions: the experience varies significantly based on the underlying condition being treated and how well-controlled it was before starting Farxiga.
Patients with well-managed diabetes who stop Farxiga might see gradual changes over weeks. Those with advanced heart failure or kidney disease often notice symptom changes much more quickly.
The Bottom Line on Stopping Farxiga
Farxiga doesn’t cause withdrawal symptoms when discontinued. Your body won’t go through physical dependence or rebound effects like it might with some other medications.
But that doesn’t make stopping consequence-free. The conditions Farxiga treats—Type 2 diabetes, heart failure, and chronic kidney disease—are progressive. Without the medication’s protective effects, these conditions continue their natural course.
Clinical trials like DAPA-CKD demonstrate real benefits: reduced risk of kidney failure, cardiovascular death, and disease progression. When Farxiga stops, so do these benefits.
If you’re considering discontinuing Farxiga, whether due to side effects, cost concerns, or other reasons, the decision deserves careful consideration with your healthcare provider. Alternatives exist, and strategies can be developed to maintain your health without this particular medication.
The key is never stopping abruptly without medical guidance and always having a transition plan in place.
Frequently Asked Questions
No, Farxiga does not cause physical withdrawal symptoms when discontinued. Unlike medications that create dependence, stopping Farxiga won’t trigger uncomfortable rebound effects. However, the underlying condition it was treating—whether diabetes, heart failure, or kidney disease—will lose the medication’s protective benefits, and symptoms of the original condition may return or worsen.
Farxiga has an elimination half-life of approximately 13 hours. This means the medication is essentially cleared from your body within about three days after your last dose. However, the therapeutic effects on blood sugar, fluid balance, and cardiovascular protection begin changing within 24-48 hours as the drug concentration decreases.
Blood sugar levels typically begin rising within 24 to 48 hours after discontinuing Farxiga, though the increase is usually gradual rather than sudden. The exact timeline and severity depend on your overall diabetes management, including diet, exercise, and any other medications you’re taking. Clinical studies show dapagliflozin lowers HbA1c by approximately 0.66% compared to placebo, with canagliflozin showing approximately 0.91%, and these benefits reverse once the medication stops.
Farxiga can be stopped abruptly without requiring a gradual taper. The medication doesn’t need to be slowly reduced like some other drugs. However, stopping should only be done under medical supervision to ensure proper monitoring and transition to alternative treatments if necessary. Your healthcare provider may want to start an alternative medication before discontinuing Farxiga.
The most common reasons for discontinuing Farxiga include serious side effects (such as ketoacidosis, severe urinary tract infections, or genital yeast infections), cost and affordability concerns, medical situations requiring temporary cessation (like surgery or acute illness), declining kidney function below safe thresholds, and pregnancy. According to official prescribing information, female genital mycotic infections occur in approximately 8.4% of female patients taking FARXIGA 5 mg and 10 mg doses combined (compared to 6.9% with placebo and 1.5% with control).
Yes, discontinuing Farxiga removes its protective benefits for both heart failure and chronic kidney disease. The DELIVER Phase III trial showed Farxiga significantly reduces cardiovascular death or worsening heart failure, while the DAPA-CKD trial demonstrated reduced risk of sustained eGFR decline of at least 50%, end-stage kidney disease, or death from renal or cardiovascular causes. When stopped, these protective effects gradually disappear, and disease progression may return to pre-treatment rates.
If cost is preventing you from continuing Farxiga, discuss options with your healthcare provider before stopping. The official Farxiga website mentions a savings card program that may reduce costs to $0 per month for eligible patients. Additionally, your provider can explore alternative medications that may be more affordable, including other SGLT2 inhibitors or different medication classes that treat your condition. Never stop the medication without first exploring these alternatives and developing a transition plan.
Moving Forward
Managing chronic conditions like Type 2 diabetes, heart failure, and kidney disease is a long-term commitment. Medications like Farxiga play an important role, but they’re just one part of comprehensive care.
If Farxiga isn’t working for you—whether due to side effects, effectiveness concerns, or practical barriers—solutions exist. The healthcare system offers multiple medication options, support programs, and management strategies.
What matters most is maintaining open communication with your healthcare team and making informed decisions about your treatment. Never let concerns about a medication go unaddressed, and never make changes to your treatment plan without professional guidance.
Your health deserves that level of attention and care.
