Quick Summary: Taking antibiotics too close together can increase the risk of side effects like nausea, diarrhea, and in rare cases, more serious adverse reactions. While occasionally taking doses too close is unlikely to cause serious harm for most people, it disrupts the medication schedule and can affect treatment effectiveness. Maintaining proper spacing between doses helps ensure optimal antibiotic levels in the body while minimizing potential adverse effects and reducing the risk of antibiotic resistance.
Antibiotics have revolutionized modern medicine, saving countless lives by treating bacterial infections. But these powerful medications require precise timing to work effectively and safely.
When someone accidentally takes doses too close together—whether from forgetting a previous dose or misunderstanding the schedule—concerns naturally arise about potential harm. The reality is more nuanced than simple yes-or-no answers.
Understanding what happens when antibiotic doses overlap helps patients make informed decisions and know when medical attention might be necessary.
Why Antibiotic Timing Matters
Antibiotics are designed to maintain specific drug levels in the bloodstream over time. Each medication has a carefully calculated dosing schedule based on how the body absorbs, distributes, and eliminates it.
Taking doses too close together disrupts this balance. Drug levels spike higher than intended, which can overwhelm the body’s ability to process the medication safely.
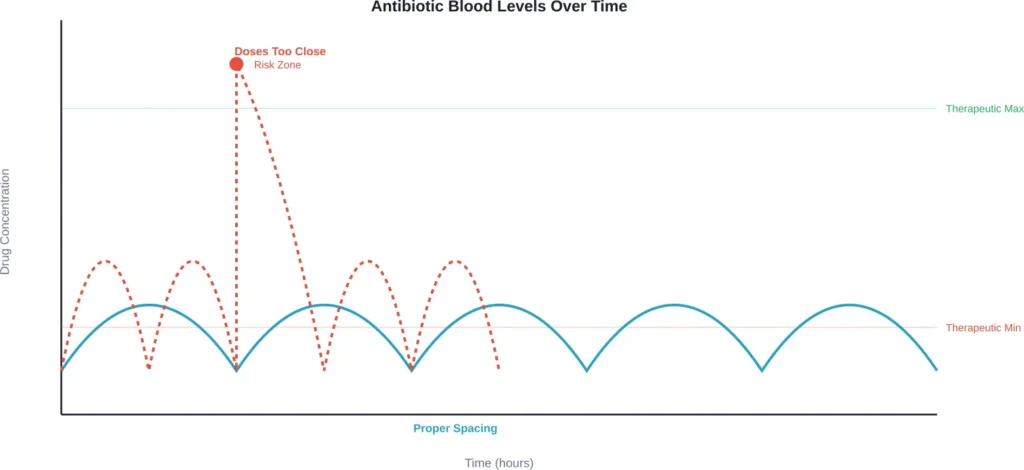
The prescribed spacing—whether every 8 hours, 12 hours, or once daily—isn’t arbitrary. It’s calculated to keep antibiotic concentrations within a therapeutic window: high enough to kill bacteria, but low enough to minimize adverse effects.
How Antibiotics Work in Your System
After swallowing an antibiotic, it travels through the digestive system, gets absorbed into the bloodstream, and circulates throughout the body. The medication targets bacterial cells while the liver and kidneys work to break down and eliminate it.
This elimination process happens at a predictable rate for each drug. When doses are properly spaced, drug levels rise after each dose and fall before the next one, creating a saw-tooth pattern that maintains effectiveness.
But compressing this timeline forces the body to handle higher concentrations before fully processing the previous dose.
Immediate Risks of Taking Doses Too Close Together
The good news? According to medical experts, antibiotic overdoses are rarely dangerous for otherwise healthy individuals. Most instances of taking doses too close together result in mild, temporary discomfort rather than serious medical emergencies.
That said, certain side effects become more likely when drug levels spike unexpectedly.
Common Side Effects
Stomach upset ranks as the most frequent complaint when antibiotics are taken too close together. This includes:
- Nausea and vomiting
- Diarrhea or loose stools
- Abdominal cramping or discomfort
- Loss of appetite
- General digestive distress
These symptoms typically resolve on their own within 24-48 hours as drug levels normalize. They’re uncomfortable but rarely require medical intervention.
Less Common But More Serious Reactions
Research published in medical literature indicates that adverse drug reactions occur in 5–10% of hospital admissions, with serious reactions happening in 0.1–0.3% of cases that may be serious and cause death. While these statistics cover all adverse drug reactions, antibiotics contribute significantly to this burden.
Higher antibiotic concentrations can trigger:
- Allergic reactions ranging from mild rashes to severe anaphylaxis
- Neurotoxic effects including confusion, seizures, or altered mental status (particularly with certain antibiotic classes)
- Liver stress or temporary enzyme elevation
- Kidney function changes, especially with medications like aminoglycosides
According to the CDC’s antibiotic stewardship data, improving how antibiotics are prescribed and used remains critical for patient safety. Proper dosing plays a central role in this effort.
Specific Antibiotic Classes and Their Risks
Not all antibiotics carry the same risk profile when doses overlap. Some medication classes tolerate timing errors better than others.
Beta-Lactams (Penicillins, Cephalosporins)
These common antibiotics generally have wide safety margins. Taking doses too close together rarely causes serious harm, though gastrointestinal upset remains likely.
Allergic reactions represent the primary concern with beta-lactam antibiotics, but timing doesn’t significantly influence allergy risk.
Fluoroquinolones
This class requires more caution. Research on neurotoxic effects of antibiotics shows that fluoroquinolones can cause central nervous system reactions including confusion, agitation, and in rare cases, seizures—particularly at elevated concentrations.
Aminoglycosides
These powerful antibiotics carry heightened risks of kidney damage and hearing loss when levels get too high. Medical literature on aminoglycoside dosing emphasizes the importance of maintaining proper intervals to prevent toxicity.
Fortunately, aminoglycosides are typically administered in hospital settings where dosing is carefully monitored.
Metronidazole
Studies on antimicrobial-induced cognitive side effects note that metronidazole can cause neurological symptoms including peripheral neuropathy and encephalopathy, especially with higher doses or in patients with impaired liver function.
| Antibiotic Class | Common Examples | Risk Level if Taken Too Close | Primary Concerns |
|---|---|---|---|
| Beta-Lactams | Amoxicillin, Cephalexin | Low to Moderate | Stomach upset, diarrhea, allergic reactions |
| Fluoroquinolones | Ciprofloxacin, Levofloxacin | Moderate | Neurological effects, tendon issues |
| Macrolides | Azithromycin, Clarithromycin | Low to Moderate | Heart rhythm changes, liver stress |
| Aminoglycosides | Gentamicin, Tobramycin | High | Kidney damage, hearing loss |
| Metronidazole | Flagyl | Moderate | Neurological symptoms, nausea |
What to Do If You Take Antibiotics Too Close Together
Realizing doses overlapped can be stressful. Here’s what medical professionals recommend:
For Most Cases
If doses were taken just a few hours closer than prescribed, monitor for symptoms but don’t panic. Most people experience no adverse effects or only mild stomach upset.
Skip the next scheduled dose to get back on track, then resume the normal schedule. This prevents further compounding the problem.
Contact a Healthcare Provider If:
- Severe nausea, vomiting, or diarrhea develops
- Signs of allergic reaction appear (rash, itching, swelling, difficulty breathing)
- Neurological symptoms occur (confusion, dizziness, severe headache, vision changes)
- The antibiotic is known to have narrow safety margins
- The person has kidney or liver disease
Poison control centers handle medication questions. If you think someone has taken too much of an antibiotic, use the webPOISONCONTROL® online tool to get help, or call your poison center at 1-800-222-1222.
Emergency Situations
Seek immediate medical attention (call emergency services or go to the emergency department) if someone experiences:
- Rapid heartbeat with chest pain
- Difficulty breathing or swelling of lips, tongue, or throat
- Seizures or loss of consciousness
- Severe abdominal pain
These symptoms, while rare, require prompt evaluation regardless of the antibiotic involved.
The Antibiotic Resistance Connection
Beyond immediate safety concerns, improper antibiotic use contributes to a larger public health crisis. According to the World Health Organization, bacterial antimicrobial resistance was directly responsible for 1.27 million global deaths in 2019 and contributed to 4.95 million deaths.
Taking antibiotics incorrectly—whether doses too close together, skipped doses, or stopping treatment early—can promote bacterial resistance development.
How Resistance Develops
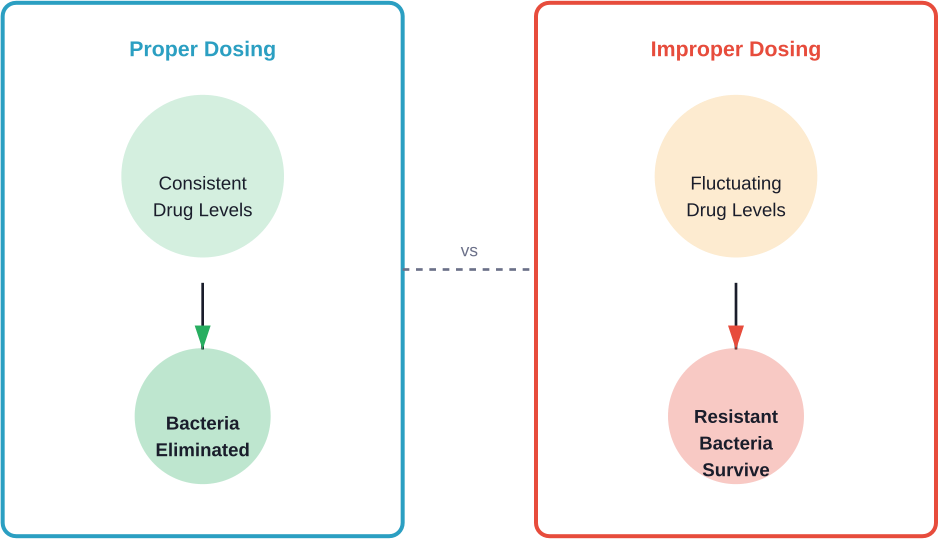
When antibiotic levels fluctuate unpredictably, some bacteria may survive exposure to sub-therapeutic concentrations. These survivors can develop mutations that make them harder to kill.
Maintaining consistent drug levels through proper dosing helps ensure complete bacterial elimination, reducing resistance risk.
The WHO’s AWaRe classification system categorizes antibiotics to promote appropriate use and combat resistance. Understanding proper dosing practices supports these global stewardship efforts.
Prevention Strategies
Avoiding timing mistakes requires simple but effective strategies:
Set Multiple Reminders
Phone alarms work well for maintaining consistent schedules. Set reminders for each dose time, and consider a second alert asking whether the dose was taken.
Use Pill Organizers
Weekly pill boxes with compartments for different times of day provide visual confirmation of whether doses were taken. This simple tool prevents both missed doses and accidental duplicates.
Link to Daily Routines
Associating antibiotic doses with regular activities—meals, bedtime, morning coffee—helps build habits that reduce timing errors.
Write It Down
Keep a medication log noting when each dose is taken. This creates accountability and provides a reference if uncertainty arises.
Clarify Instructions
When picking up prescriptions, ask the pharmacist to explain the dosing schedule clearly. Understand whether “three times daily” means every 8 hours or just during waking hours.
Special Populations at Higher Risk
Certain groups face greater danger from antibiotic dosing errors:
Infants and Young Children
Research indicates that pediatric populations are particularly vulnerable to neurotoxic effects from elevated antibiotic concentrations. Immature liver and kidney function means drugs are eliminated more slowly, and the blood-brain barrier may be more permeable.
Always use precise measuring devices for liquid antibiotics—never household spoons.
Older Adults
Age-related decline in kidney and liver function affects how the body processes medications. Older patients may experience more pronounced effects from dosing errors.
People with Kidney or Liver Disease
These organs eliminate most antibiotics. When they’re not functioning optimally, drugs accumulate more quickly, making timing errors more consequential.
Pregnant Women
Some antibiotics cross the placenta. While most are safe during pregnancy when used correctly, dosing errors introduce unnecessary risks.
Frequently Asked Questions
Generally no. If a dose is missed and it’s close to the next scheduled dose, skip the missed one and continue with the regular schedule. Taking double doses increases side effect risk without significantly improving treatment outcomes. Contact a pharmacist if uncertain about the specific situation.
This depends entirely on the prescribed schedule. “Every 8 hours” means doses should be spaced throughout the day and night. “Three times daily” typically means during waking hours. Follow the specific instructions provided with the prescription, and ask the pharmacist to clarify any confusion.
Common signs include severe nausea, vomiting, diarrhea, and abdominal pain. More serious symptoms can include confusion, dizziness, rapid heartbeat, difficulty breathing, or allergic reactions. While true overdoses are rare, any concerning symptoms after taking too much medication warrant medical evaluation.
A single instance of doses taken too close usually doesn’t compromise treatment effectiveness significantly. However, repeated dosing errors that disrupt the medication schedule can affect how well the antibiotic eliminates bacteria and may contribute to resistance development.
Most common side effects like nausea and diarrhea from taking doses too close together resolve within 24-48 hours as drug levels normalize. More serious reactions may require medical treatment and can last longer depending on the specific reaction and antibiotic involved.
This varies by medication. Some antibiotics should be taken with food to reduce stomach upset, while others need to be taken on an empty stomach for proper absorption. Check the prescription label or ask the pharmacist for specific guidance on the prescribed antibiotic.
Most antibiotics don’t interact dangerously with alcohol, but combining them isn’t recommended. Alcohol can worsen side effects like stomach upset and may slow recovery from infection. Metronidazole and certain other antibiotics can cause severe reactions when combined with alcohol. Avoid alcohol during antibiotic treatment and for 48 hours after finishing the course.
Conclusion
Taking antibiotics too close together typically results in temporary discomfort rather than life-threatening emergencies for most people. Stomach upset and diarrhea represent the most common consequences, while serious reactions remain relatively rare.
That said, proper timing exists for good reasons. Maintaining consistent drug levels optimizes treatment effectiveness while minimizing adverse effects and reducing antibiotic resistance risk.
If doses accidentally overlap, monitor for symptoms and adjust the schedule moving forward. Contact healthcare providers or poison control if concerning reactions develop, especially with high-risk antibiotics or vulnerable populations.
Prevention through careful planning, reminders, and clear understanding of dosing instructions remains the best approach. When in doubt about antibiotic use, consult pharmacists or healthcare providers—they’re equipped to provide guidance tailored to specific medications and circumstances.
Remember: antibiotics are powerful tools that deserve respect. Using them correctly protects both individual health and preserves their effectiveness for future generations.
