Quick Summary: Taking ibuprofen daily for a year poses significant health risks including gastrointestinal damage, kidney dysfunction, cardiovascular complications, and potential liver injury. Medical evidence shows that long-term NSAID use beyond 10 consecutive days without physician supervision can lead to stomach ulcers, increased stroke risk, and organ damage. Safe ibuprofen use requires limiting intake to 1,200 mg daily for no more than 10 days unless medically supervised.
Ibuprofen sits in medicine cabinets worldwide as one of the most trusted over-the-counter painkillers. It’s affordable, accessible, and effective for everything from headaches to arthritis pain.
But here’s the thing—what starts as occasional use can quickly become a daily habit. And that’s where serious problems begin.
Taking ibuprofen every single day for an entire year fundamentally changes the equation from safe pain relief to potentially dangerous medication overuse. The consequences affect multiple organ systems, with some damage becoming irreversible.
Understanding Ibuprofen and NSAIDs
Ibuprofen belongs to a class of medications called nonsteroidal anti-inflammatory drugs (NSAIDs). These drugs work by inhibiting cyclooxygenase (COX) enzymes—specifically COX-1 and COX-2—which convert arachidonic acid into prostaglandins, prostacyclin, and thromboxane.
That biochemistry matters because prostaglandins don’t just cause pain and inflammation. They also protect your stomach lining, regulate kidney function, and help control blood clotting.
When you block prostaglandin production daily for months on end, you’re not just stopping pain signals. You’re removing critical protective mechanisms throughout your body.
According to research published in the National Institutes of Health database, NSAIDs undergo extensive hepatic metabolism primarily through cytochrome P450 2C9 enzymes and are eliminated via renal excretion. This metabolic pathway means your liver and kidneys bear the processing burden every single time you swallow that pill.
What Defines Safe Ibuprofen Use
Before examining what happens during a year of daily use, it’s important to understand what medical professionals actually consider safe.
Unless otherwise directed by a physician, teens and adults should take no more than 200 to 400 milligrams every four to six hours as needed. That’s one or two regular-strength tablets or one extra-strength tablet.
The maximum daily limit sits at 1,200 mg in a 24-hour period for over-the-counter use.
And here’s the critical part: this dosing should not continue for more than 10 consecutive days without medical supervision.
That 10-day threshold exists for good reason. Short-term use allows your body to recover between episodes of NSAID exposure. Long-term daily use denies your organs that recovery window.
Gastrointestinal Damage: The First System to Suffer
Your digestive system takes the most immediate and visible hit from chronic ibuprofen use.
Prostaglandins protect your stomach lining by stimulating mucus and bicarbonate secretion. When ibuprofen blocks these protective prostaglandins day after day, your stomach becomes vulnerable to its own acid.
Research examining adverse reactions to NSAIDs found that gastrointestinal complications remain among the most common serious side effects. The proportion of pediatric ibuprofen packages purchased without a prescription rose from 28% in 2008 to 70% in 2015, with pediatric use growing by over 60% from 2020 to 2024—suggesting increasing consumption without corresponding medical oversight.
Here’s what develops during months of continuous use:
- Gastritis and inflammation of the stomach lining
- Peptic ulcers in the stomach and duodenum
- Gastrointestinal bleeding that can occur without warning
- Increased risk of perforation in severe cases
The stomach bleeding risk is particularly concerning because it can happen suddenly, without preceding symptoms. Discussions in chronic pain communities describe experiences of discovering blood in stool or vomit after months of daily NSAID use—often the first indication that serious damage has occurred.
Real talk: stomach ulcers from NSAIDs aren’t just uncomfortable. They can be life-threatening if bleeding becomes severe or perforation occurs.
Kidney Function Deterioration
Your kidneys rely on prostaglandins to maintain proper blood flow and filtration. Chronic NSAID use disrupts this delicate balance.
During the first few months of daily ibuprofen use, you might not notice anything wrong. But your kidneys are compensating, working harder to maintain function despite reduced prostaglandin support.
By the six-month mark of continuous use, measurable changes often appear. Glomerular filtration rate may decline. Fluid retention can develop. Blood pressure may increase.
According to NIH research on NSAID toxicity, these medications are generally contraindicated in patients with significant hepatic or renal impairment precisely because the drugs undergo renal excretion through glomerular filtration and tubular secretion.
But wait—if you start with healthy kidneys and then damage them with daily ibuprofen, you’ve created a dangerous cycle. Your compromised kidneys now struggle to clear the very medication that’s harming them.
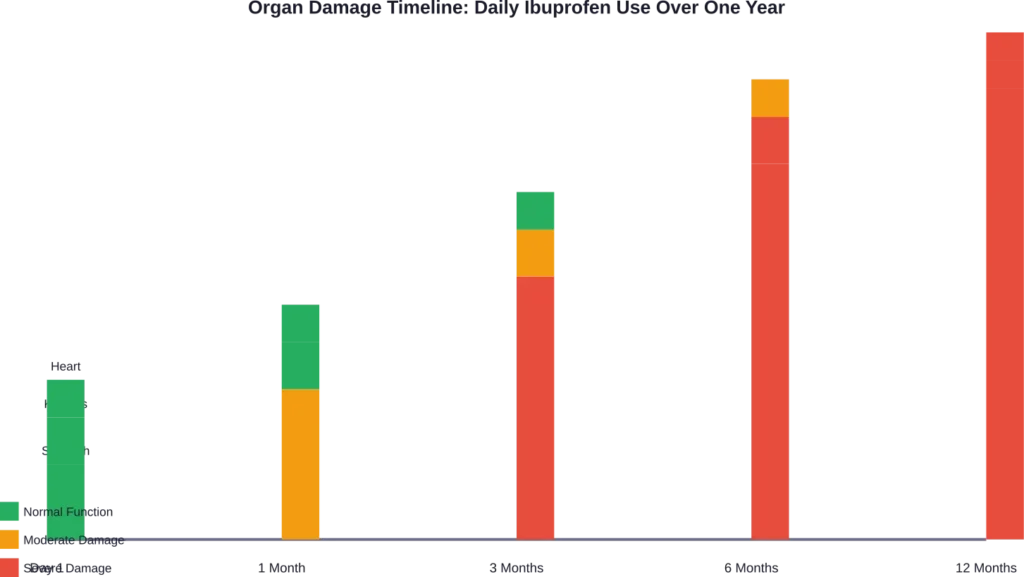
Long-term consequences of kidney damage include:
- Chronic kidney disease that may progress even after stopping ibuprofen
- Acute kidney injury requiring hospitalization
- Electrolyte imbalances affecting heart rhythm
- Increased blood pressure adding cardiovascular stress
Cardiovascular Complications
This is where the risks get genuinely frightening.
Research from the University of California, Davis examined cardiovascular effects of ibuprofen. Professor Aldrin Gomes and 36 current and former students published findings noting that one study found ibuprofen tripled the risk of stroke, while other studies found increased stroke risk ranging from 10% to 50%. This risk begins within the first few weeks of regular, daily use.
The cardiovascular dangers emerge from multiple mechanisms. NSAIDs can increase blood pressure. They affect blood clotting factors. They may accelerate atherosclerosis in susceptible individuals.
After months of daily use, these effects compound. A 2025 pharmacovigilance analysis of EudraVigilance reports examined 58,911 total cases reported for ibuprofen. Of these, 13.9% contained nervous system disorders and 10.7% entailed psychiatric disorders—but cardiovascular events represented a significant portion of serious adverse events.
The FDA warns that NSAIDs can cause stroke, heart attack, heart failure, and stomach bleeding. These aren’t theoretical risks appearing in fine print. They’re documented outcomes from real patients taking these medications long-term.
So what actually happens to your cardiovascular system during a year of daily ibuprofen?
| Cardiovascular Effect | Timeline | Severity Risk |
|---|---|---|
| Blood pressure elevation | 2-4 weeks | Moderate |
| Fluid retention | 1-2 months | Moderate |
| Increased clotting tendency | 2-3 months | High |
| Heart attack risk elevation | 3-6 months | High |
| Stroke risk elevation | 3-6 months | High |
| Heart failure exacerbation | 6-12 months | Very High |
For individuals with pre-existing cardiovascular conditions, the timeline accelerates and the severity magnifies.
Liver Injury Potential
While less common than gastrointestinal or kidney problems, liver damage from chronic ibuprofen use does occur.
According to NIH’s LiverTox database, ibuprofen is considered among the safest NSAIDs and is generally well tolerated. However, it can nevertheless rarely cause clinically apparent and serious acute liver injury, particularly when given in high therapeutic doses.
The liver processes every dose of ibuprofen you take through cytochrome P450 enzymes. During short-term use, this presents no problem. But daily processing for months creates sustained metabolic stress.
Side effects may include headache, dizziness, somnolence, dyspepsia, nausea, abdominal discomfort, heartburn, and diarrhea. Rare but potentially serious adverse events include hepatotoxicity.
Liver damage typically manifests as elevated liver enzymes detected in blood tests. In severe cases, it can progress to hepatitis or even liver failure requiring transplantation.
Neuropsychiatric Effects
Here’s something most people don’t expect: chronic NSAID use can affect your nervous system and mental health.
Recent pharmacovigilance research analyzing real-world adverse event reports found that from total cases reported for ibuprofen, 13.9% contained nervous system disorders and 10.7% entailed psychiatric disorders.
These effects include:
- Persistent headaches (ironically, from the medication meant to treat them)
- Dizziness and vertigo
- Cognitive changes including difficulty concentrating
- Mood alterations including depression and anxiety
- Sleep disturbances
The mechanisms aren’t fully understood, but prostaglandin modulation affects neurotransmitter systems. When you alter prostaglandin signaling every single day for a year, neurological consequences can emerge.
Additional Risks and Complications
Beyond the major organ systems, year-long daily ibuprofen use creates other problems.
Fertility concerns affect both men and women. Research indicates NSAIDs may cause temporary infertility in some individuals through effects on reproductive hormone signaling.
Fetal toxicity represents a serious concern for pregnant women. In September 2025, the FDA initiated a label change process for acetaminophen to reflect evidence suggesting that use during pregnancy may be associated with increased risk of neurological conditions such as autism and ADHD in children—and NSAIDs carry their own pregnancy warnings, particularly in the third trimester.
Hypersensitivity reactions can develop even in people who previously tolerated ibuprofen well. Chronic exposure sometimes triggers allergic responses ranging from rash to serious conditions like Stevens-Johnson syndrome.
Peripheral edema—swelling in the legs, ankles, and feet—commonly develops from fluid retention caused by prostaglandin disruption in the kidneys.
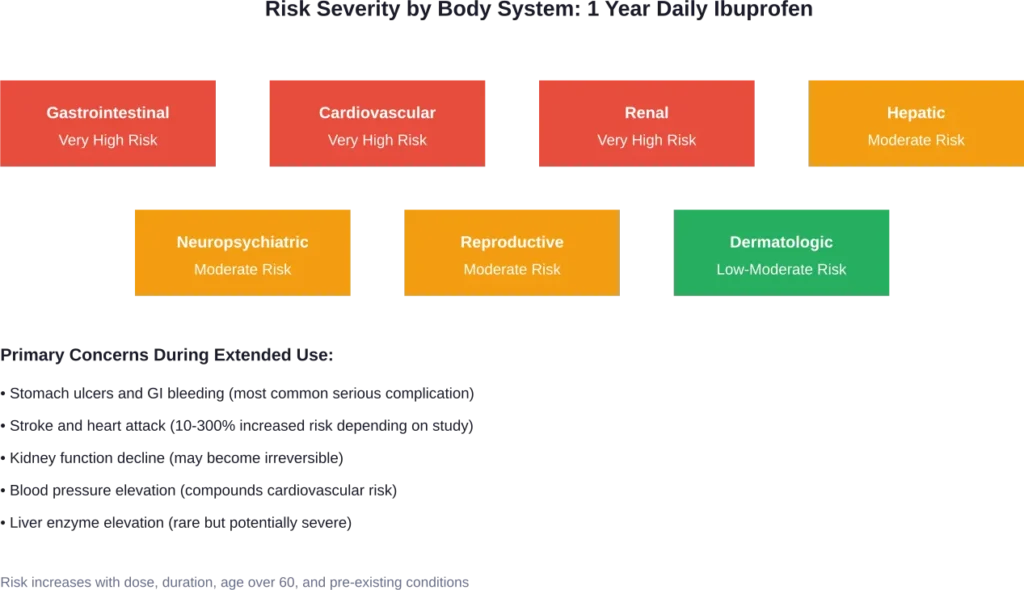
Who Faces the Greatest Danger
Not everyone experiences the same risk level from chronic ibuprofen use. Certain factors dramatically increase vulnerability.
Age matters significantly. Adults over 60 face substantially higher risks of complications, particularly gastrointestinal bleeding and cardiovascular events.
Pre-existing conditions amplify danger:
- Kidney disease patients face accelerated decline
- Heart disease patients experience elevated heart attack and stroke risk
- Stomach ulcer history predicts likely recurrence
- Liver disease patients cannot safely metabolize chronic NSAIDs
- Hypertension worsens under NSAID influence
Concurrent medications create additional hazards. Combining ibuprofen with blood thinners, certain antidepressants, corticosteroids, or other NSAIDs multiplies bleeding risk and other complications.
Alcohol consumption while taking daily ibuprofen significantly increases stomach bleeding risk.
What Medical Professionals Recommend Instead
So if chronic ibuprofen use causes this much damage, what should people with ongoing pain do instead?
Medical professionals emphasize that no one should take ibuprofen daily for extended periods without physician supervision and monitoring. That supervision includes regular blood tests checking kidney function, liver enzymes, and blood counts.
For chronic pain management, safer approaches include:
Physical therapy and exercise address underlying mechanical problems without medication. Targeted strengthening and flexibility work often reduces pain more effectively than pills.
Topical NSAIDs deliver medication directly to painful areas with minimal systemic absorption. These formulations provide relief without subjecting your entire body to NSAID exposure.
Acetaminophen offers an alternative for pain relief, though it carries its own risks with chronic use. The FDA initiated label changes in September 2025 regarding potential neurological risks during pregnancy, and liver toxicity remains a concern with high doses.
Prescription medications including COX-2 selective inhibitors may provide anti-inflammatory benefits with reduced gastrointestinal risk, though cardiovascular concerns persist.
Non-pharmacological interventions including heat therapy, cold therapy, massage, acupuncture, and cognitive behavioral therapy help many people manage chronic pain without medication risks.
Recognizing Warning Signs
If you’ve been taking ibuprofen daily for months, certain symptoms demand immediate medical attention.
Stop the medication and seek care if you experience:
- Black, tarry stools or blood in stool (indicating gastrointestinal bleeding)
- Vomiting blood or material that looks like coffee grounds
- Severe abdominal pain
- Chest pain or pressure
- Sudden severe headache or vision changes
- Weakness on one side of the body or slurred speech (stroke symptoms)
- Significant swelling in legs, ankles, or feet
- Decreased urination or dark urine
- Yellowing of skin or eyes (jaundice)
- Unexplained fatigue or weakness
The FDA operates MedWatch, a program for reporting serious reactions to medical products. Healthcare professionals and patients can report adverse events, product quality problems, and medication errors.
The Reality Check
Look, ibuprofen is genuinely useful medication. For short-term use—a few days for a headache, a week for dental pain, 10 days for a sports injury—it’s generally safe and effective.
But a year of daily use? That’s a completely different scenario.
Your body isn’t designed to have prostaglandin synthesis blocked every single day for months. The protective mechanisms that prostaglandins provide throughout your digestive, cardiovascular, and urinary systems exist for good reasons.
Discussion among chronic pain patients reveal a common pattern: what starts as temporary relief becomes long-term use, with gradually increasing doses sometimes needed for the same effect. By the time serious complications emerge, significant organ damage may have already occurred.
A large population-based study utilizing enrollment data from the Tabari cohort found that NSAID usage prevalence reached 14.7%, with consumption increasing with age. The study assessed NSAID use based on self-reported consumption for at least 30 days, identifying demographic, behavioral, and clinical risk factors.
That said, the real prevalence of year-long continuous use likely exceeds reported figures, since many people don’t consider over-the-counter medications worth mentioning to physicians.
Frequently Asked Questions
Some damage reverses after stopping ibuprofen, while other effects may be permanent. Stomach lining typically heals within weeks to months after discontinuation. Kidney function may partially recover if damage hasn’t progressed to chronic kidney disease, though some decline may persist. Cardiovascular risks decrease after stopping, but any permanent vascular changes remain. Early detection and cessation offer the best chance for recovery.
Medical guidelines recommend not exceeding 10 consecutive days of ibuprofen use without physician supervision. Beyond this threshold, risks of serious complications increase significantly. Any use extending beyond several weeks should involve medical oversight with regular monitoring of kidney function, liver enzymes, and blood pressure. Year-long daily use without medical supervision poses unacceptably high risks.
Early kidney damage often produces no noticeable symptoms. The first detectable signs typically appear in blood tests showing elevated creatinine and reduced glomerular filtration rate. Later symptoms may include decreased urination, dark or foamy urine, fatigue, nausea, swelling in legs and ankles, shortness of breath, and confusion. By the time symptoms appear, significant damage has usually occurred.
Lower doses reduce but don’t eliminate risks from chronic use. While taking 200 mg daily poses less immediate danger than 1,200 mg daily, both exposure patterns create cumulative organ stress over months. The duration of use matters as much as the dose. Even low-dose daily ibuprofen for a year can cause gastrointestinal damage, kidney dysfunction, and cardiovascular complications.
Youth and good baseline health reduce but don’t prevent risks from chronic NSAID use. Younger individuals generally tolerate ibuprofen better than older adults, but daily use for a year still damages stomach lining, stresses kidneys, and increases cardiovascular risks. Starting with healthy organs doesn’t provide immunity to medication side effects—it just means you have more reserve before dysfunction becomes clinically apparent.
Ibuprofen doesn’t cause physical dependence or withdrawal symptoms like opioids do. You can stop abruptly without tapering. However, the underlying pain condition will return to its baseline level without medication. Some people experience rebound pain temporarily. After stopping, damaged organs begin healing, though recovery timelines vary—stomach lining heals fastest, kidney function recovery depends on damage extent, and cardiovascular risk gradually decreases.
No oral medication is entirely safe for daily use over a full year without risks. However, certain approaches offer better safety profiles than chronic ibuprofen: topical NSAIDs provide localized relief with minimal systemic absorption; physical therapy and exercise address root causes; some prescription medications under physician monitoring may be appropriate; non-pharmacological treatments including heat, cold, and behavioral approaches avoid medication risks entirely. The safest approach combines multiple modalities rather than relying on any single medication daily.
Final Thoughts
Taking ibuprofen every day for a year transforms a safe, effective medication into a source of potentially serious harm.
The evidence is clear. Your stomach lining will sustain damage. Your kidneys will experience functional decline. Your cardiovascular risk will increase. Your liver may show signs of stress. And in some cases, these effects become irreversible.
None of this means ibuprofen is a bad medication. It means chronic daily use for months or years represents misuse of a drug designed for short-term symptom relief.
If you’re currently taking ibuprofen daily, talk with a healthcare provider about safer alternatives for managing your pain. If you’ve been doing so for months already, request blood tests to check kidney and liver function before permanent damage occurs.
Your pain is real and deserves effective management. But that management shouldn’t come at the cost of your kidneys, stomach, heart, and liver.
Better options exist. You just need to look beyond that familiar bottle in your medicine cabinet.
