Quick Summary: Taking too much insulin causes hypoglycemia (dangerously low blood sugar), with symptoms ranging from shakiness and confusion to seizures, coma, or death in severe cases. Immediate treatment involves consuming 15-20 grams of fast-acting carbohydrates, rechecking blood sugar after 15 minutes, and seeking emergency medical help if symptoms worsen or consciousness is lost.
Insulin overdose represents one of the most serious complications people with diabetes face. The CDC identifies diabetes agents, including insulin, as almost one in seven (or 14%) of emergency department visits for adverse drug events, making them a significant category among medication-related emergencies.
According to the CDC, adverse drug events are a serious public health threat. For adults managing diabetes, medication errors increase significantly as treatment regimens become more complex.
An insulin overdose occurs when someone takes more insulin than their body needs, causing blood sugar levels to drop dangerously low. This condition—called hypoglycemia—can escalate from mild shakiness to life-threatening emergencies within minutes.
Understanding what happens during an insulin overdose, recognizing the warning signs, and knowing exactly what to do can literally save lives.
What Actually Happens During an Insulin Overdose
When excess insulin enters the bloodstream, it forces too much glucose out of the blood and into cells. Blood sugar drops rapidly.
The brain depends entirely on glucose for fuel. When blood sugar falls below normal levels, the brain essentially starts running out of gas. That’s when symptoms begin.
But here’s the thing—the body doesn’t give up without a fight. The adrenal glands release stress hormones like epinephrine (adrenaline) to try raising blood sugar back up. This emergency response causes many of the early warning signs: sweating, shaking, and rapid heartbeat.
If blood sugar continues dropping despite these defense mechanisms, brain function deteriorates progressively. Confusion sets in, followed by coordination problems, then altered consciousness.
In documented cases of severe insulin poisoning, patients have remained in comas for extended periods. Research published through the NIH describes a case where a 27-year-old paramedical healthcare worker who intentionally overdosed on insulin remained comatose for 90 hours and required 470 grams of dextrose infusion before regaining consciousness. The patient also developed bradycardia (slow heart rate) and dangerously low blood pressure requiring ionotropic support.
Symptoms of Insulin Overdose: What to Watch For
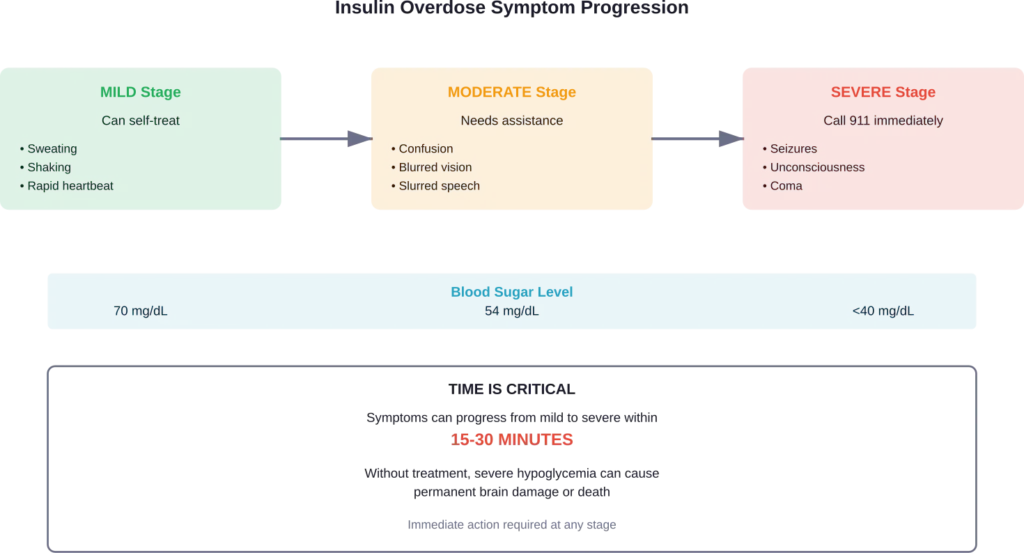
Symptoms progress through stages as blood sugar drops lower.
Early Warning Signs (Mild Hypoglycemia)
These appear first, when blood sugar drops but the brain still functions normally:
- Sweating (often profuse, even in cool environments)
- Shakiness or trembling
- Rapid or irregular heartbeat
- Anxiety or nervousness
- Hunger pangs
- Irritability or mood changes
- Pale skin
- Tingling around the mouth
At this stage, the person remains fully conscious and can treat themselves.
Moderate Symptoms (Progressing Hypoglycemia)
As blood sugar drops further, brain function begins to suffer:
- Confusion or difficulty concentrating
- Dizziness or lightheadedness
- Blurred or double vision
- Slurred speech
- Weakness or fatigue
- Headache
- Difficulty with coordination
People at this stage may struggle to help themselves and need assistance.
Severe Symptoms (Critical Hypoglycemia)
When blood sugar reaches dangerously low levels, symptoms become life-threatening:
- Seizures or convulsions
- Loss of consciousness or coma
- Inability to wake the person
- Unresponsiveness
- Abnormal breathing patterns
According to Poison Control, for young children exposed to diabetes medications, even one pill can cause blood sugar to drop dangerously low, causing seizures, coma, or death. There is no safe dose of diabetes pills for children who don’t have diabetes.
Emergency Treatment: What to Do Right Now
Speed matters. Brain cells begin dying when deprived of glucose for too long.
For Mild to Moderate Symptoms (Person Is Conscious)
Follow the 15-15 rule, as recommended by the CDC and diabetes organizations:
Step 1: Consume 15-20 grams of fast-acting carbohydrates immediately. The CDC specifically recommends glucose tablets or high-glucose foods.
Foods containing 15-20 grams of fast-acting carbohydrates include:
- 4 glucose tablets
- 4 ounces (1/2 cup) of fruit juice
- 4 ounces of regular soda (not diet)
- 1 tablespoon of honey
- 1 tablespoon of sugar dissolved in water
- Hard candies (check packaging for amount)
Step 2: Rest and get off your feet. Avoid physical activity, which burns glucose.
Step 3: Recheck blood sugar after 15 minutes using a glucose meter.
Step 4: If blood sugar remains low after 15 minutes, take another 15-20 grams of fast-acting carbohydrates.
Step 5: Once blood sugar returns to normal (above 70 mg/dL), eat a small snack containing protein and complex carbohydrates to prevent another drop.
For Severe Symptoms (Unconscious, Seizing, or Unable to Swallow)
Real talk: This is a medical emergency. The person cannot safely swallow, so oral sugar won’t work and could cause choking.
Call 911 immediately. Tell the dispatcher it’s an insulin overdose with loss of consciousness.
If a glucagon emergency kit is available and someone present knows how to administer it, use it right away. Glucagon is a hormone that signals the liver to release stored glucose into the bloodstream.
Do not try to force food or liquid into an unconscious person’s mouth. That’s a choking hazard.
Position the person on their side (recovery position) to keep airways clear if vomiting occurs.
Stay with the person until emergency medical services arrive. Monitor breathing and be prepared to start CPR if needed.
| Situation | Action Required | Timeline |
|---|---|---|
| Mild symptoms, person alert | 15-20g fast carbs, recheck in 15 min | Should improve within 15 minutes |
| Moderate symptoms, confused but conscious | Assist with fast carbs, monitor closely | Recheck every 15 minutes |
| Severe symptoms, unconscious or seizing | Call 911, administer glucagon if available | Emergency medical care needed immediately |
| Symptoms don’t improve after treatment | Call 911 or go to emergency room | Do not delay |
Common Causes: How Insulin Overdoses Happen
Accidental insulin overdoses happen more often than many people realize.
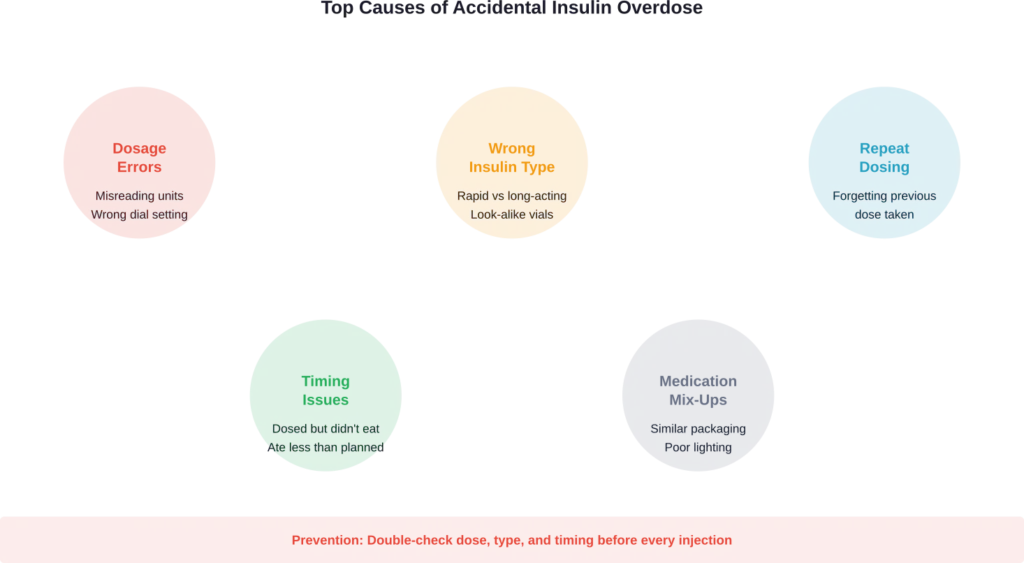
Dosage Calculation Errors
Mixing up units is dangerously easy. Taking 50 units instead of 5 units represents a tenfold overdose. With insulin pens and syringes, a misread dial or syringe marking can have serious consequences.
Taking the Wrong Type of Insulin
People managing diabetes often use multiple insulin types: long-acting background insulin and rapid-acting mealtime insulin. Taking rapid-acting insulin instead of long-acting—or vice versa—creates dangerous blood sugar swings.
Taking a dose of rapid-acting insulin when meaning to take long-acting can cause a sudden, severe drop in blood sugar within 15-30 minutes.
Repeat Dosing (Forgetting Previous Dose)
According to Poison Control, medication confusion is a common cause of calls to poison centers, particularly among older adults. Taking insulin twice because someone forgot they’d already taken their dose doubles the amount in the system.
Incorrect Timing
Taking mealtime insulin but then not eating—or eating much less than planned—leaves excess insulin with insufficient carbohydrates to match it.
Medication Mix-Ups
In healthcare settings, administering insulin intended for one patient to another patient, or selecting the wrong concentration, has resulted in serious adverse events.
The CDC tracks these medication errors as part of their adverse drug event surveillance, noting that insulin and other diabetes agents are among the most problematic categories.
Prevention Strategies That Actually Work
Preventing insulin overdose requires systematic habits, not just good intentions.
Check the Label Every Single Time
According to Poison Control, many medication errors happen because people don’t verify what they’re taking. Check the medication name, concentration, and dose before drawing up or dialing insulin—even if it’s the same insulin taken for years.
If glasses are needed for reading, wear them. Turn on adequate lighting. These simple steps prevent devastating errors.
Use a Medication Tracking System
Keep a written log, use a smartphone app, or maintain a chart showing when each insulin dose was taken. This prevents repeat dosing errors.
Some insulin pens have memory functions that display when the last dose was given. Use this feature.
Store Insulin Types Separately
Keep rapid-acting and long-acting insulins in different areas of the refrigerator or medicine cabinet. Physical separation reduces the chance of grabbing the wrong type.
Match Insulin to Food
For mealtime insulin, establish a routine: draw up or dial the dose, then immediately eat. Don’t dose mealtime insulin and then wait, hoping to eat later. Plans change, delays happen, and blood sugar crashes.
Educate Everyone in the Household
Family members, roommates, or caregivers should know:
- What insulin is being used and when
- Signs of low blood sugar
- Where glucose tablets or juice are kept
- How to use a glucagon emergency kit
- When to call 911
For Children: Strict Medication Security
Poison Control emphasizes that for young children, there is no safe dose of diabetes medications. Even one pill can cause dangerous hypoglycemia leading to seizures, coma, or death.
Store all diabetes medications in original containers, in locked cabinets or areas completely inaccessible to children. Never leave insulin, pills, or supplies where children can reach them.
Long-Term Health Risks From Repeated Overdoses
Even when successfully treated, repeated episodes of severe hypoglycemia carry consequences.
Research on persistent insulin-induced hypoglycemia has identified toxicological effects beyond the immediate crisis. The brain adapts to repeated low blood sugar episodes, which can reduce the intensity of warning symptoms over time—a dangerous condition called hypoglycemia unawareness.
When warning symptoms diminish, people may not recognize they’re becoming hypoglycemic until they’ve reached severe, dangerous levels requiring emergency assistance.
Repeated severe hypoglycemia has also been associated with increased cardiovascular events and may contribute to cognitive impairment over time.
When Medical Intervention Is Absolutely Necessary
Some situations require professional medical care, not home treatment:
- The person is unconscious or cannot be awakened
- Seizures occur
- Blood sugar doesn’t respond to treatment after two rounds of fast-acting carbohydrates
- The person is confused, combative, or unable to cooperate with treatment
- There’s uncertainty about how much insulin was taken
- The overdose was intentional (suicide attempt)
In hospital settings, treatment for severe insulin overdose can extend for many hours. The case documented in NIH research required continuous dextrose infusion for 90 hours along with cardiovascular support.
Medical teams can provide continuous IV glucose, monitor vital signs, and manage complications like bradycardia, hypotension, or cerebral edema that can accompany severe insulin poisoning.
FAQs About Insulin Overdose
Any amount of insulin that causes blood sugar to drop below normal levels (typically below 70 mg/dL) technically represents too much for that situation. The specific units that constitute an overdose vary dramatically based on individual factors like body weight, insulin sensitivity, food intake, and activity level. What’s normal for one person could be an overdose for another.
Yes, severe hypoglycemia from insulin overdose can cause permanent brain damage if blood sugar remains critically low for extended periods. Brain cells require constant glucose and can die when deprived of it. However, when treated promptly, most people recover fully without lasting effects.
Mild symptoms typically resolve within 15-30 minutes after consuming fast-acting carbohydrates. Severe overdoses, particularly with long-acting insulin, may require treatment for many hours or even days. The NIH-documented case required 90 hours of continuous treatment before the patient regained consciousness.
Insulin overdose causes hypoglycemic coma (too little blood sugar). Diabetic coma can also result from hyperglycemia (too much blood sugar) in uncontrolled diabetes. They’re opposite problems requiring opposite treatments—which is why checking blood sugar before treatment is critical when possible.
Yes, 4 ounces of orange juice or other fruit juice contains approximately 15 grams of fast-acting carbohydrates and is specifically recommended by the CDC for treating low blood sugar. The sugar in juice enters the bloodstream quickly. However, juice won’t help if the person is unconscious or unable to swallow safely.
It depends. For mild overdoses that responded quickly to treatment and involved rapid-acting insulin, hospital care may not be necessary. However, overdoses involving long-acting insulin, situations where the exact amount taken is unknown, or any case where symptoms recur should receive medical evaluation. When in doubt, call a poison control center at 1-800-222-1222 for expert guidance.
Yes. Research published through PubMed documents fatal outcomes from insulin overdose. Severe hypoglycemia that goes untreated can cause death through various mechanisms including seizures, cardiovascular collapse, or irreversible brain damage. This is why recognizing symptoms and seeking immediate treatment is critical.
Bottom Line: Respect Insulin’s Power
Insulin is life-saving medication for millions of people with diabetes. But its power to lower blood sugar also makes it potentially dangerous when dosing errors occur.
The key takeaways: Know the warning signs of low blood sugar. Keep fast-acting carbohydrates immediately accessible. Check labels and doses every single time. And never hesitate to call for emergency help when symptoms are severe.
According to the CDC, adverse drug events from diabetes medications represent a serious and preventable public health threat. Most insulin overdoses are accidental and avoidable through careful medication management practices.
If managing diabetes feels overwhelming, or if hypoglycemia episodes happen frequently, talk with a healthcare provider about adjusting the treatment plan. Modern diabetes management offers many options to reduce the risk of dangerous blood sugar swings while maintaining good glucose control.
Store emergency contact numbers—including poison control at 1-800-222-1222—where they’re immediately accessible. Make sure glucagon kits are available, unexpired, and that household members know how to use them.
Taking insulin requires attention and respect for what it does. With proper precautions, tracking systems, and emergency preparedness, the risks of overdose can be minimized while still achieving the blood sugar control that keeps people with diabetes healthy.
