Quick Summary: Not eating for a week triggers a cascade of metabolic changes as the body shifts from glucose to fat-based energy. While survival is possible with water, severe risks emerge including muscle wasting, electrolyte imbalances, immune suppression, and potentially fatal refeeding syndrome upon resuming food. Medical complications affect the heart, brain, bones, and vital organs.
The human body isn’t designed to run on empty. Yet circumstances ranging from medical conditions to intentional fasting can lead to extended periods without food. Understanding what happens during a week-long fast reveals just how adaptable—and vulnerable—our bodies really are.
Research from the National Institutes of Health shows that food deprivation creates metabolic disturbances affecting every major organ system. But the timeline matters.
How Long Can Humans Actually Survive Without Food?
According to expert analysis of survival cases, adults without underlying health conditions can survive between 8 and 21 days without food, provided they have access to water. The variation depends on factors like body composition, hydration status, and environmental conditions.
Records from survival situations show considerable individual differences. A daylong fast might leave someone irritable and low on energy, but the body adjusts during longer deprivation periods.
Water intake dramatically affects survival time. Without both food and water, survival time drops to just days. With adequate hydration, the body can sustain basic functions much longer by metabolizing stored energy reserves.
The Metabolic Shift: What Happens in Your Body
Here’s the thing though—your body doesn’t just shut down when food stops coming. It pivots.
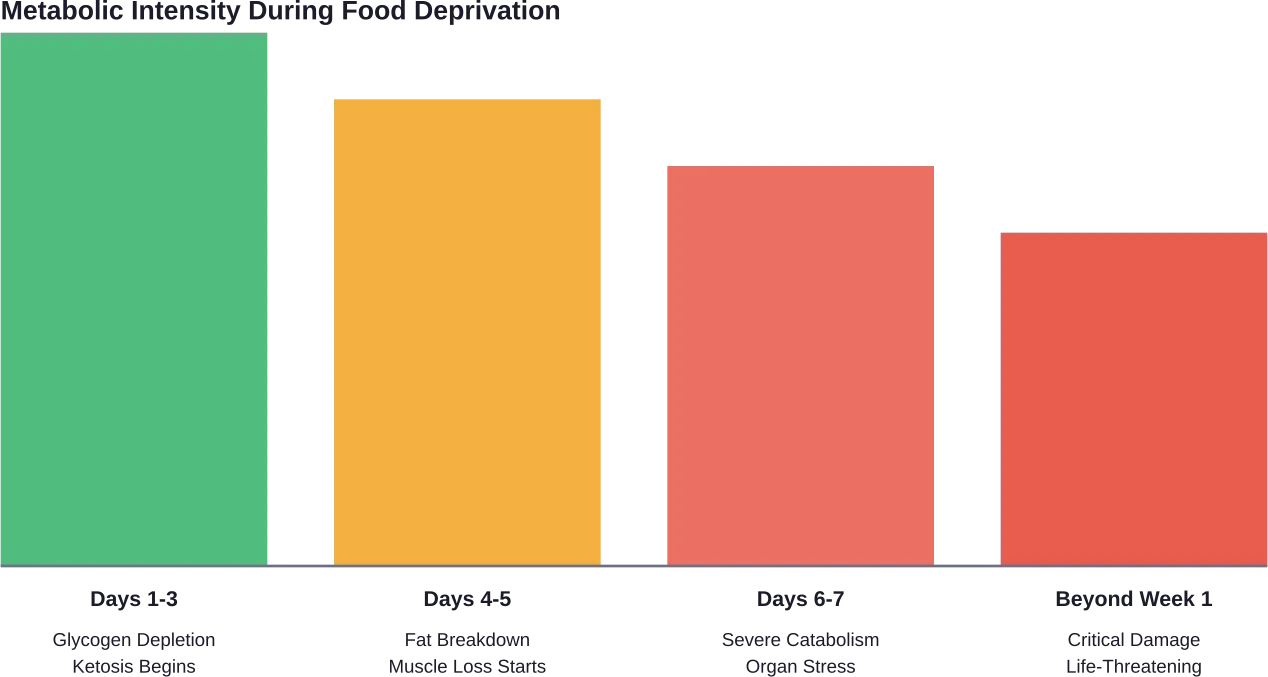
Days 1-3: Glucose Depletion and Ketosis
During the first 24-72 hours, the body burns through glycogen stores in the liver and muscles. Once these glucose reserves deplete, metabolism shifts to ketosis—a state where the body breaks down fat into ketones for fuel.
This transition causes the familiar “brain fog” and fatigue many experience during early fasting. The brain normally runs on glucose, so adapting to ketones takes time.
Days 4-7: Fat and Protein Catabolism
By day four, fat breakdown accelerates. But here’s where it gets concerning: the body also starts breaking down muscle protein for amino acids needed to maintain critical functions.
Research on starvation shows that this protein catabolism affects more than just skeletal muscle. Organ tissues, including the heart, can experience degradation during extended starvation.
Physical Effects and Medical Complications
A week without food doesn’t just trigger hunger pangs. The body experiences measurable physiological changes across multiple systems.
Cardiovascular Stress
The heart muscle itself can weaken during starvation. Electrolyte imbalances—particularly drops in potassium, magnesium, and phosphate—create dangerous cardiac arrhythmias.
Blood pressure often drops as the body conserves energy, leading to dizziness and fainting risk.
Immune System Suppression
According to research on malnutrition and immune function, nutritional deprivation increases infection risk and deteriorates overall health status.
White blood cell production declines, antibody response weakens, and the body’s ability to fight pathogens diminishes significantly.
Bone Density Loss
Research from the International Journal of Endocrinology provides evidence that starvation adversely affects bone quality. Research indicates that nearly 805 million people globally suffer from malnutrition, with documented impacts on skeletal health.
Even short-term food deprivation can trigger mechanisms that impair osteoblast maintenance and calcium regulation.
Neurological and Psychological Changes
Food restriction produces profound psychological effects beyond physical hunger. Studies on starvation show detrimental cognitive and behavioral consequences in both children and adults.
Concentration suffers. Mood becomes unstable. Decision-making capacity declines. These aren’t just subjective experiences—they reflect measurable changes in brain chemistry and function.
| Body System | Effects After 7 Days | Severity Level |
|---|---|---|
| Metabolic | Ketosis, protein catabolism, reduced metabolic rate | Moderate to High |
| Cardiovascular | Electrolyte imbalances, arrhythmia risk, low blood pressure | High |
| Immune | Suppressed white blood cells, reduced antibody production | High |
| Muscular | Muscle wasting, weakness, reduced strength | Moderate to High |
| Skeletal | Bone density reduction, calcium dysregulation | Moderate |
| Neurological | Cognitive impairment, mood instability, confusion | Moderate |
| Digestive | Reduced enzyme production, altered gut function | Moderate |
The Refeeding Syndrome Danger
Now, this is where it gets critical. Surviving a week without food is one thing. Eating again safely is another.
Refeeding syndrome represents one of the most serious medical complications following starvation. According to the National Institute for Health Care and Excellence guidelines cited in StatPearls, this condition results from aggressive nutritional rehabilitation after prolonged fasting.
When food is reintroduced too quickly, fluid and electrolyte shifts can cause life-threatening complications. Hypophosphatemia—dangerously low phosphate levels—is the hallmark sign, but magnesium, potassium, and thiamine deficiencies also occur.
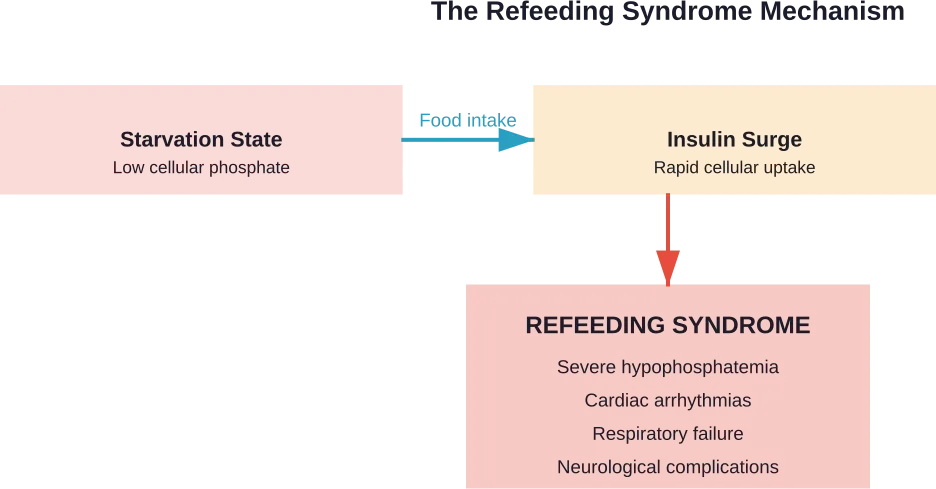
Why Refeeding Is Dangerous
During starvation, cells become depleted of phosphate and other electrolytes. When carbohydrates are suddenly reintroduced, insulin surges and cells rapidly uptake phosphate from the bloodstream. This creates a severe deficit that affects:
- Cardiac function—potentially causing fatal arrhythmias
- Respiratory muscles—leading to breathing difficulties
- Neurological function—causing confusion, seizures, or coma
- Blood cell production—resulting in anemia and immune dysfunction
Medical supervision during refeeding is essential for anyone who has gone without food for more than 5-7 days. Calories must be reintroduced gradually, often starting at just 20% of normal intake.
Who Is at Highest Risk?
Not everyone faces the same danger level from a week without food. Certain populations are particularly vulnerable.
According to NICE guidelines on refeeding syndrome, high-risk factors include:
- Low body mass index
- Unintentional weight loss exceeding 10-15% within 3-6 months
- History of alcohol abuse
- Chronic medical conditions affecting nutrition
- Eating disorders like anorexia nervosa
Children are especially susceptible. Research shows that approximately 45% of deaths in children under five can be correlated with malnutrition.
Intermittent Fasting vs. Starvation
But wait. What about intentional fasting for health benefits?
There’s a crucial distinction between controlled intermittent fasting and unintentional starvation. Research on intermittent fasting shows that alternate-day fasting or time-restricted eating typically involves much shorter fasting windows—16 to 24 hours, not seven consecutive days.
In one study cited in research on intermittent fasting, overweight adults with moderate asthma consumed only 20% of their normal calorie intake on alternate days. Participants who adhered to this pattern lost 8% of their initial weight. Importantly, they still consumed some nutrition regularly and remained under medical observation.
A full week without any food represents an entirely different physiological challenge with substantially higher risks.
Long-Term Consequences
Even after resuming normal eating, the effects of a week-long fast don’t immediately disappear.
Digestive function changes during food deprivation. Research indicates that food deprivation can impact digestive enzyme production and digestive function. The gut needs time to restore normal function.
Metabolic rate often remains suppressed for weeks or months following significant starvation periods. This adaptation, while protective during the fast, can complicate weight management afterward.
Psychological effects may persist as well. Food restriction creates lasting behavioral and cognitive changes that can affect eating patterns long after physical recovery.
When Medical Attention Is Critical
Anyone experiencing extended food deprivation should seek medical evaluation before resuming normal eating. Signs requiring immediate medical attention include:
- Severe weakness or inability to stand
- Irregular heartbeat or chest pain
- Confusion, disorientation, or difficulty concentrating
- Edema (swelling) in extremities
- Difficulty breathing
- Loss of consciousness
Healthcare providers can monitor electrolyte levels, implement safe refeeding protocols, and address complications before they become life-threatening.
Frequently Asked Questions
Death directly from a week without food is unlikely in otherwise healthy adults with adequate water intake. However, serious medical complications can develop, including severe electrolyte imbalances and cardiac stress. The greatest mortality risk often comes during the refeeding period when electrolyte shifts can cause fatal arrhythmias if not properly managed.
Weight loss varies considerably based on starting weight, body composition, and activity level. Initial losses of 1-2 pounds per day are common as the body depletes glycogen and associated water. After that, fat and muscle loss continues at roughly 0.5-1 pound daily. Total weight loss might range from 5-12 pounds, though much of the initial drop is water weight that returns upon refeeding.
Metabolic rate decreases during extended fasting as the body attempts to conserve energy. This adaptive response can reduce metabolic rate by 20-30% or more. The slowdown affects not just calorie burning but also body temperature regulation, hormone production, and cellular repair processes. Metabolic suppression may persist for weeks after resuming normal eating.
Nearly every organ system experiences impact. The heart faces stress from electrolyte imbalances and reduced cardiac muscle mass. The brain experiences cognitive changes from altered fuel sources. Kidneys work harder to maintain fluid balance. The liver depletes glycogen stores and shifts to ketone production. Bones lose density, muscles atrophy, and the immune system weakens. The digestive system reduces enzyme production and gut motility.
Seven-day water fasts carry substantial medical risks and should only be undertaken under direct medical supervision. Even with adequate hydration, the risks of severe electrolyte imbalances, cardiac complications, and dangerous refeeding syndrome remain high. People with underlying health conditions, low body weight, or nutritional deficiencies face elevated danger. Medical monitoring with regular blood work is essential if such a fast is medically indicated.
Extended starvation can produce lasting effects depending on individual circumstances. Bone density loss may be permanent or take years to restore. Cardiac muscle damage might result in ongoing heart function issues. Neurological changes can persist. However, most otherwise healthy individuals who receive proper refeeding care can achieve full recovery, though the timeline varies from weeks to months depending on the severity of depletion.
Refeeding must be gradual and carefully controlled. Medical protocols typically start with small amounts of easily digestible foods—broths, diluted juices, and simple carbohydrates. Caloric intake often begins at just 10-20% of normal needs, increasing slowly over 7-10 days. Phosphate, thiamine, and other electrolyte supplementation is usually necessary. Protein should be reintroduced cautiously. Medical supervision during this process prevents refeeding syndrome and allows monitoring of cardiac and metabolic function.
The Bottom Line
The human body demonstrates remarkable resilience during food deprivation. Metabolic adaptations allow survival for much longer than a week when water is available. But survival and health are different things.
Seven days without food triggers protein catabolism, immune suppression, organ stress, and electrolyte disturbances that create substantial medical risks. The refeeding period poses additional danger when not properly managed.
If medical conditions, eating disorders, or circumstances have resulted in extended food deprivation, professional medical guidance isn’t optional—it’s lifesaving. The physiological changes are too complex and the risks too serious for self-management.
Understanding what happens when the body goes without food reveals both human adaptability and vulnerability. That knowledge can inform safer approaches to fasting, better recognition of malnutrition risks, and appropriate medical intervention when needed.
