Quick Summary: Eating or drinking before surgery can lead to pulmonary aspiration—a dangerous condition where stomach contents enter the lungs during anesthesia. Modern fasting guidelines recommend stopping solid foods 6-8 hours before surgery and clear liquids 2 hours before, replacing the outdated ‘nothing after midnight’ rule. Following these evidence-based fasting instructions significantly reduces surgical complications and keeps patients safe.
Preoperative fasting instructions aren’t arbitrary rules designed to make patients uncomfortable. They exist to prevent a potentially fatal complication called pulmonary aspiration. Understanding what happens when these guidelines aren’t followed can mean the difference between a smooth procedure and a medical emergency.
Here’s the thing though—many patients still receive outdated fasting advice that’s unnecessarily restrictive.
The Primary Danger: Pulmonary Aspiration
When anesthesia relaxes the body’s muscles, it also affects the reflexes that normally prevent stomach contents from traveling backward into the esophagus and lungs. If food or liquid sits in the stomach during surgery, it can be regurgitated and aspirated into the lungs.
Pulmonary aspiration occurs when stomach contents enter the respiratory tract. This can cause chemical pneumonitis, bacterial pneumonia, airway obstruction, or even death. The acidic nature of gastric contents damages delicate lung tissue almost immediately.
Pulmonary aspiration during anesthesia can lead to serious respiratory complications including chemical pneumonitis, bacterial pneumonia, and airway obstruction. The risk increases significantly when patients haven’t followed proper fasting guidelines.
But aspiration isn’t just about solid food. Liquids matter too, though current evidence shows clear fluids leave the stomach much faster than previously believed.
Current Fasting Guidelines: Not ‘Nothing After Midnight’
For decades, the medical standard was simple: nothing by mouth after midnight before surgery. This blanket rule has been replaced by more nuanced, evidence-based recommendations from the American Society of Anesthesiologists.
Modern guidelines distinguish between different types of intake:
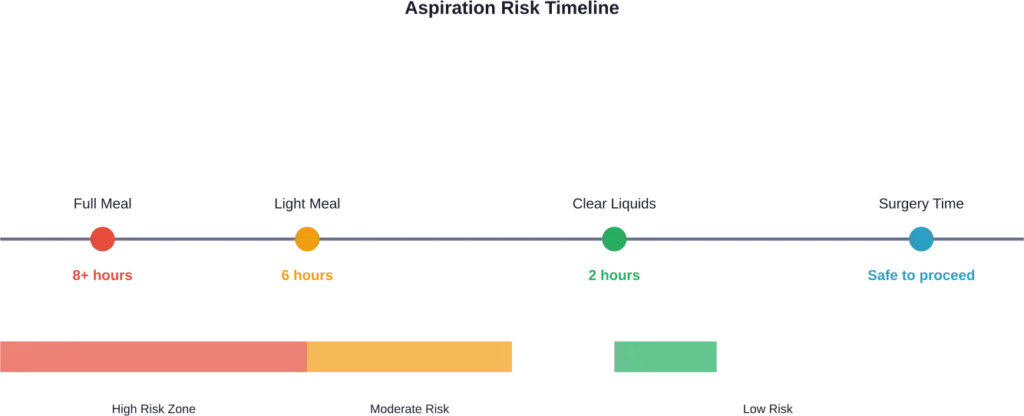
| Food/Drink Type | Recommended Fasting Time | Notes |
|---|---|---|
| Clear liquids | 2 hours | Water, black coffee, clear juice |
| Breast milk | 4 hours | For infants |
| Light meal | 6 hours | Toast, crackers |
| Full meal/fatty foods | 8+ hours | Fried foods, meat |
Research demonstrates that patients drinking clear fluids until two hours before surgery actually had less fluid in their stomachs during the procedure compared to those who fasted from midnight.
Real talk: many surgical patients still fast far longer than necessary. According to the American Society of Anesthesiologists, nearly 80% of infants go without clear liquids for at least twice as long as guidelines recommend before surgery.
What Actually Happens If You Eat Before Surgery
So what happens if someone ignores fasting instructions or accidentally eats something?
The surgical team faces a difficult decision. If food is discovered in the stomach shortly before a scheduled elective procedure, the surgery will likely be postponed. This isn’t a punishment—it’s a safety measure. The risk of aspiration simply becomes too high to proceed safely.
Postponement means rescheduling the operating room, anesthesiology team, and surgical staff. It creates logistical complications and delays necessary treatment. For the patient, it means additional time off work, extended anxiety, and repeating the preparation process.
During emergency procedures where fasting guidelines can’t be followed, anesthesiologists take special precautions. They may use rapid sequence induction techniques, apply cricoid pressure, or choose different anesthesia methods to minimize aspiration risk.
In a study of 321 emergency orthopaedic surgery patients, 18% didn’t meet fasting guidelines. However, anesthesia-related pulmonary complications remained rare when proper precautions were implemented.
Special Considerations That Affect Fasting
GLP-1 Medications (Ozempic, Wegovy, Mounjaro)
Patients taking GLP-1 receptor agonist medications face unique challenges. These drugs slow gastric emptying significantly—food can remain in the stomach much longer than normal.
The American Society of Anesthesiologists issued guidance on GLP-1 receptor agonists. For medications like semaglutide, which has a half-life of approximately 1 week, standard fasting periods may not be sufficient. Some anesthesiologists recommend consuming only clear liquids for 24 hours before surgery for patients on these medications.
Diabetes Management
Diabetic patients face a balancing act. Fasting can affect blood sugar levels, but eating before surgery remains dangerous. Generally speaking, diabetic patients should consult their surgical team about medication adjustments during the fasting period.
Insulin and oral diabetes medications often need dosage modifications when normal eating patterns are disrupted. The care team will provide specific instructions tailored to individual medication regimens.
Emergency Surgery
Emergency procedures can’t wait for proper fasting time. In these cases, anesthesiologists assume the stomach is full regardless of when the patient last ate. They use modified techniques designed specifically for high-risk situations.
Why Shorter Fasting Periods Are Better
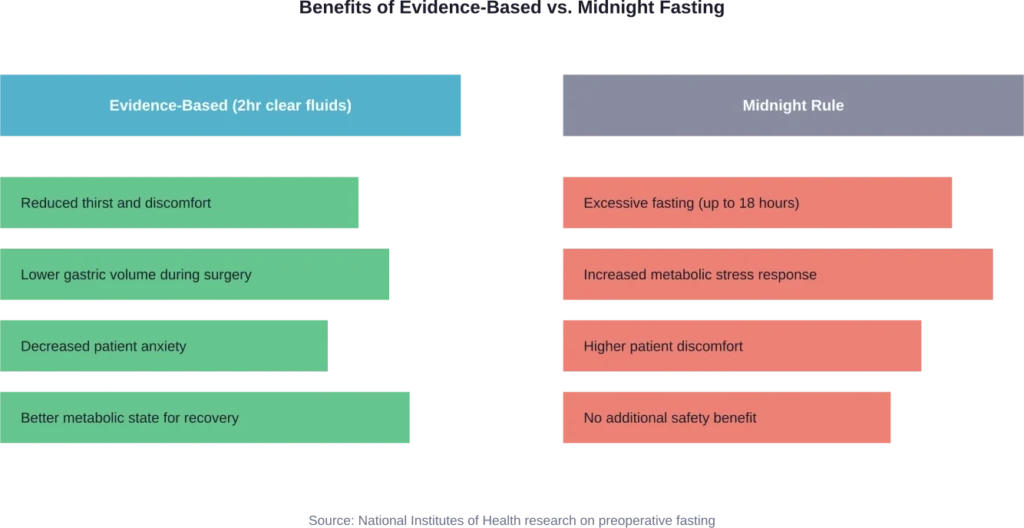
Extended fasting doesn’t just cause discomfort—it can actually harm recovery. Prolonged preoperative fasting exacerbates the body’s metabolic stress response to surgery.
Research shows that allowing clear liquids until two hours before surgery reduces patient thirst, hunger, and anxiety without increasing complications. Evidence from multiple studies demonstrates that shortened fluid fasting doesn’t result in increased risk of aspiration, regurgitation, or related complications compared to the midnight cutoff.
Enhanced Recovery After Surgery (ERAS) protocols now incorporate evidence-based fasting guidelines as a core component. These protocols focus on optimizing every aspect of perioperative care, and appropriate—not excessive—fasting plays a crucial role.
What to Do If You Accidentally Eat or Drink
Mistakes happen. Someone might forget the instructions, take a reflexive sip of water, or pop a piece of gum without thinking.
The most important step: tell the surgical team immediately. Don’t hide it out of embarrassment or fear of judgment. Medical professionals need accurate information to keep patients safe.
The care team will assess what was consumed, how much, and when. For a small sip of water three hours before surgery, they’ll likely proceed as planned. For a full breakfast an hour before, they’ll almost certainly reschedule.
Honesty prevents complications. The surgical team can’t protect patients from risks they don’t know exist.
Frequently Asked Questions
Yes, brushing teeth is typically allowed, but don’t swallow water. Spit thoroughly and use minimal water. Some facilities recommend avoiding toothpaste that might trigger swallowing reflexes.
Clear liquids include water, black coffee, tea without milk, clear juice (apple, white grape), and clear broth. Avoid anything with pulp, cream, or that’s opaque. When in doubt, ask the surgical team.
Most medications can be taken with a small sip of water even during the fasting period, but always confirm with the surgical team. Some medications—particularly diabetes drugs and blood thinners—may need adjustment or temporary discontinuation.
Chewing gum stimulates gastric acid production and saliva, which can be swallowed. Stop chewing gum at the same time solid food is restricted—typically 6-8 hours before surgery.
Not always, but it depends on the procedure and whether sedation will be used. Pure local anesthesia without sedation typically doesn’t require fasting, but procedures using conscious sedation or that might convert to general anesthesia do require it.
If the delay is significant, the anesthesia team may allow clear liquids to prevent excessive fasting. Always ask the care team before consuming anything—don’t assume extended delays change the fasting requirements.
Children follow similar principles but with age-adjusted timing. Infants can typically have breast milk 4 hours before surgery, while clear liquids are allowed 2 hours before for all ages. The American Society of Anesthesiologists provides specific pediatric guidelines.
The Bottom Line on Preoperative Fasting
Eating or drinking before surgery creates real, potentially life-threatening risks. Pulmonary aspiration can cause severe lung damage, pneumonia, or death. Following evidence-based fasting guidelines protects patients while avoiding unnecessarily prolonged fasting.
Modern recommendations allow clear liquids until 2 hours before surgery and solid foods 6-8 hours before—a significant improvement over the outdated midnight rule. These guidelines balance safety with patient comfort and optimal metabolic preparation for surgery.
Always follow the specific instructions provided by the surgical team, disclose all medications including GLP-1 drugs, and immediately report any accidental food or drink consumption. Preoperative fasting isn’t about making patients uncomfortable—it’s about ensuring everyone wakes up safely after their procedure.
