Quick Summary: Tetanus is a life-threatening bacterial infection that causes severe muscle stiffness and painful spasms, starting with lockjaw and potentially spreading throughout the body. Without treatment, tetanus can be fatal, but it’s highly preventable through vaccination. Recovery requires immediate hospitalization, intensive care, and can take weeks to months even with proper medical intervention.
Stepping on a rusty nail. Getting a deep cut in the garden. Even a minor puncture wound that seems harmless.
Any of these scenarios could introduce Clostridium tetani bacteria into the body—and what happens next isn’t pretty. Tetanus, commonly known as lockjaw, is one of those diseases that sounds like a relic from the past. But it’s still very much a threat, especially for those who skip their vaccine boosters.
According to the CDC, tetanus is an uncommon but very serious disease that requires immediate medical attention. And while deaths from tetanus have declined dramatically—falling by nearly 90% between 1990 and 2019 globally—the disease remains deadly when it strikes. In recent years, about 10% of people with tetanus in the US have died from the disease.
So what actually happens when tetanus takes hold? Here’s the full picture.
How Tetanus Infects the Body
Tetanus doesn’t spread from person to person. Instead, it enters through breaks in the skin—cuts, puncture wounds, burns, or even surgical incisions.
The bacteria live everywhere. Soil, dust, animal feces, and contaminated surfaces all harbor C. tetani spores. These spores are remarkably resilient. According to CDC data, they can survive autoclaving at 249.8°F (121°C) for 10 to 15 minutes and resist most common antiseptics.
Once inside a wound, especially one with dead tissue or poor oxygen flow, the spores activate. They multiply and release tetanospasmin—a potent neurotoxin that causes all the damage.
This toxin travels through nerve pathways to the spinal cord and brainstem, where it blocks signals that normally keep muscles relaxed. The result? Uncontrolled, painful muscle contractions.
The Three Forms of Tetanus
Not all tetanus presents the same way. The CDC identifies three distinct clinical forms:
Generalized Tetanus
This is the most common form, accounting for the vast majority of cases. It starts with jaw stiffness (hence “lockjaw”) and difficulty swallowing.
Within days, muscle spasms spread throughout the body. Facial muscles contract into a disturbing grimace called risus sardonicus. Neck and back muscles stiffen. The spasms become so severe that they can cause bone fractures and muscle tears.
Localized Tetanus
Muscle spasms occur only near the wound site. This form is less common and typically less severe, though it can progress to generalized tetanus.
Cephalic Tetanus
A rare form that affects cranial nerves, usually after head or face wounds. It often progresses to generalized tetanus and carries a poor prognosis.
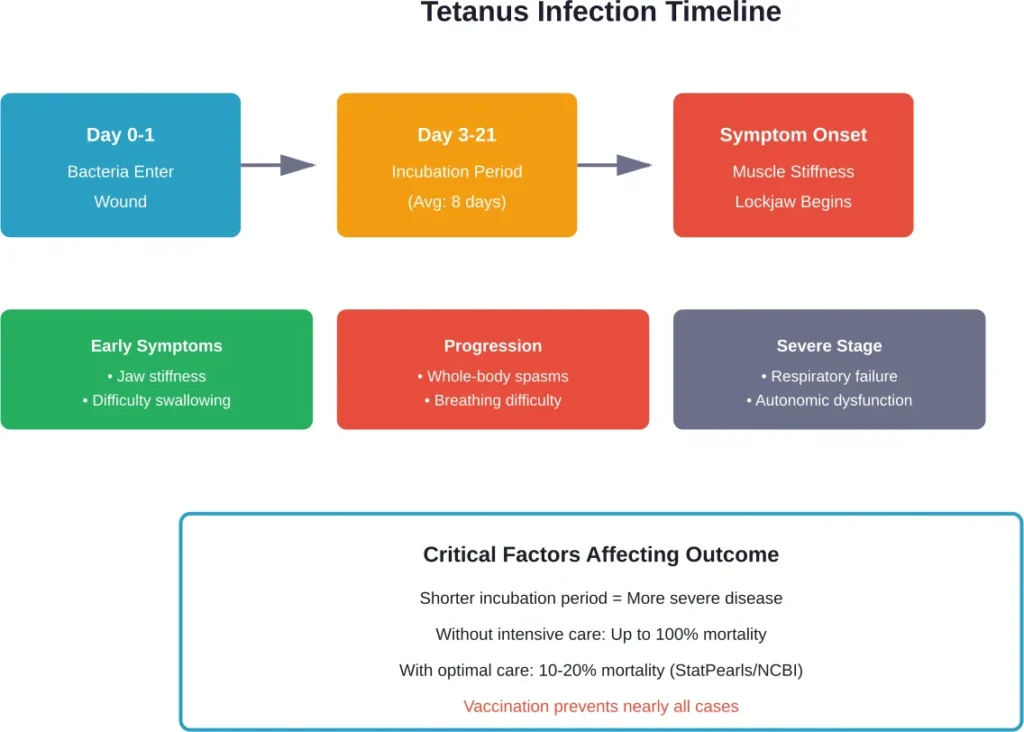
Symptoms: What Getting Tetanus Actually Feels Like
Most cases occur within 14 days of infection, with symptoms typically appearing between 3 and 21 days after exposure (average 8 days).
The first sign is usually jaw muscle stiffness. Opening the mouth becomes difficult, then nearly impossible. This is the “lockjaw” that gives tetanus its common name.
But here’s the thing—it doesn’t stop there.
Stiffness spreads to the neck, making it hard to swallow. Abdominal muscles become rigid. Then the spasms start. These aren’t mild muscle cramps. According to the CDC, tetanus causes severe, painful muscle contractions that can be triggered by minor stimuli—a loud noise, bright light, or even a gentle touch.
Spasms can last minutes and occur repeatedly over weeks. They’re powerful enough to fracture bones or tear muscles. Patients remain fully conscious during these episodes, experiencing every moment of pain.
Additional Symptoms Include:
- Difficulty swallowing and breathing
- Fever and sweating
- Elevated blood pressure and rapid heart rate
- Irritability and restlessness
- Drooling due to inability to swallow
Complications That Make Tetanus Deadly
Tetanus is a medical emergency because of its severe complications. The CDC emphasizes that hospitalization is required, often in an intensive care unit.
| Complication | Description | Risk Level |
|---|---|---|
| Respiratory Failure | Spasms of throat and chest muscles prevent breathing | High – Leading cause of death |
| Aspiration Pneumonia | Inability to swallow causes food/liquid to enter lungs | Moderate to High |
| Autonomic Dysfunction | Blood pressure and heart rate fluctuate dangerously | High – Predicts mortality |
| Bone Fractures | Violent muscle contractions break bones, especially spine | Moderate |
| Pulmonary Embolism | Blood clots from prolonged immobilization | Moderate |
According to medical research, mortality from tetanus is highest among people 70 years of age or older, as well as in cases of dysautonomia (autonomic nervous system dysfunction).
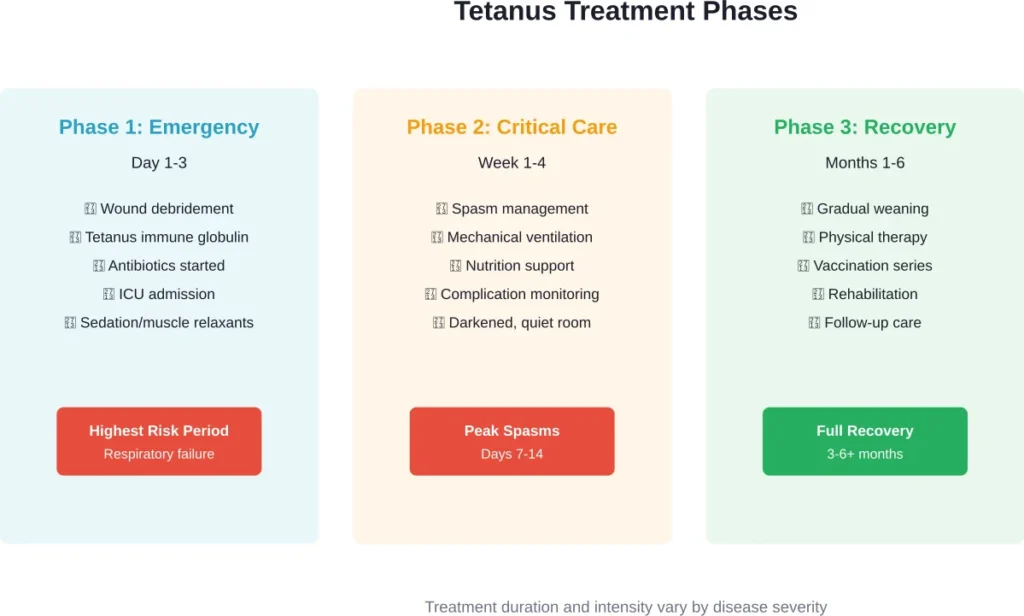
Treatment: The Long Road to Recovery
There’s no cure for tetanus. Once the toxin binds to nerve tissue, treatment focuses on managing symptoms and preventing complications until the body clears the infection.
Immediate Medical Interventions
Treatment begins with wound care—cleaning and removing dead tissue where bacteria are multiplying. Doctors administer tetanus immune globulin (TIG), which neutralizes toxin that hasn’t yet bound to nerves. But it can’t reverse damage already done.
Antibiotics like metronidazole kill active bacteria, but won’t stop toxin already released.
Intensive Care Management
Most patients require weeks in intensive care. Muscle relaxants and sedatives help control spasms. Severe cases need mechanical ventilation because respiratory muscles can’t function.
Patients are kept in quiet, darkened rooms since stimulation triggers spasms. Even routine care—turning the patient, changing bedding—must be done carefully.
According to StatPearls/NCBI, the case-fatality rate without high-quality medical care can approach 100%. With optimal intensive care, mortality ranges from 10% to 20%.
Recovery Timeline
Recovery is slow. Muscle spasms can persist for weeks. Complete recovery often takes months.
And here’s something many don’t realize: surviving tetanus doesn’t provide immunity. The amount of toxin needed to cause disease is too small to trigger an immune response. Patients who recover still need vaccination.
Who’s at Highest Risk
According to CDC guidance, not being up to date with tetanus vaccines is the biggest risk factor for infection.
Adults need a tetanus booster every 10 years. But many skip them.
Certain groups face elevated risk:
- Older adults: According to medical research, mortality from tetanus is highest among people 70 years of age or older
- People with diabetes: Wounds heal more slowly and infections develop more easily
- Injection drug users: Contaminated needles provide direct entry for bacteria
- Agricultural workers: Frequent exposure to soil and animal waste
- Newborns in areas with poor sanitation: In 2018, approximately 25,000 newborns died from neonatal tetanus, a 97% reduction since 1988
Prevention: The Only Reliable Protection
Vaccines are the best way to protect against tetanus, according to the CDC. And they work remarkably well.
The tetanus vaccine is typically given as part of combination vaccines:
| Vaccine Type | Who It’s For | Schedule |
|---|---|---|
| DTaP | Children under 7 | 5 doses: at 2, 4, 6, 15-18 months, and 4-6 years |
| Tdap | Preteens and adults | One dose at age 11-12, then Td boosters every 10 years |
| Td | Adults needing boosters | Every 10 years after Tdap |
Pregnant women should receive Tdap during each pregnancy to protect newborns.
After a dirty wound or burn, doctors may recommend a booster if it’s been more than 5 years since the last dose.
Real Talk: Why Tetanus Still Matters
It’s easy to dismiss tetanus as a rare disease. And in countries with robust vaccination programs, it is uncommon.
But when it occurs, the consequences are devastating. Days in intensive care, weeks of painful spasms, months of recovery—and that’s if patients survive. Without treatment, mortality approaches 100%. Even with optimal care, 10-20% don’t make it.
The bacteria are everywhere. Soil. Dust. Rusty metal, sure—but also clean surfaces contaminated with spores. A minor wound that seems insignificant can become a life-threatening emergency if vaccination status isn’t current.
And here’s what makes tetanus particularly cruel: it’s entirely preventable. Deaths from tetanus fell nearly 90% globally between 1990 and 2019, reflecting the success of vaccination programs.
Frequently Asked Questions
Most cases develop symptoms within 14 days of infection, with symptoms typically appearing between 3 and 21 days after exposure (average 8 days). Shorter incubation periods typically correlate with more severe disease.
According to StatPearls/NCBI, the case-fatality rate without high-quality medical care can approach 100%. Tetanus is a medical emergency that requires immediate hospitalization and intensive care. Without treatment, muscle spasms will eventually affect breathing muscles, leading to respiratory failure and death.
No. The amount of tetanus toxin needed to cause disease is too small to trigger natural immunity. According to the WHO, people who recover from tetanus do not have natural immunity and can be infected again. Vaccination is still necessary after recovery.
Recovery varies by severity but typically takes months. Muscle spasms can persist for weeks. Patients often remain hospitalized for several weeks and require months of rehabilitation and physical therapy before returning to normal activities.
No. While rusty nails are a common example, tetanus bacteria live in soil, dust, and animal feces everywhere. Any wound—clean or dirty, deep or shallow—can introduce bacteria. Puncture wounds, burns, crush injuries, and even minor cuts can cause tetanus if vaccination isn’t current.
According to CDC recommendations, adults should receive a Td or Tdap booster every 10 years. After a severe wound or burn, a booster may be recommended if it’s been more than 5 years since the last dose. Pregnant women should receive Tdap during each pregnancy.
In the United States, about 10% of people with tetanus die from the disease according to CDC data. With optimal intensive care, mortality ranges from 10-20%. Older adults and those with autonomic dysfunction have higher mortality rates.
Conclusion: Prevention Is Everything
What happens if you get tetanus? The honest answer is nothing good.
Severe pain. Weeks in the ICU. Months of recovery. And for some, death—despite every medical intervention available.
But here’s the good news: tetanus is almost entirely preventable. A simple vaccine series, updated every decade, provides reliable protection. It’s one of modern medicine’s clearest success stories.
When was your last tetanus shot? If it’s been more than 10 years—or if you’re not sure—talk to your healthcare provider. A quick booster is vastly preferable to experiencing what happens when tetanus takes hold.
Don’t wait for a rusty nail to make that decision for you.
