Quick Summary: Missing a single dose of your cholesterol pill typically won’t cause immediate harm or symptoms, but it can temporarily reduce the medication’s effectiveness. The general rule: take the missed dose as soon as you remember, unless it’s within 12 hours of your next scheduled dose—in that case, skip it and continue your regular schedule. Never double up on doses, and contact your doctor if you frequently miss doses, as this can increase your cardiovascular risk over time.
Cholesterol medications—particularly statins like atorvastatin, rosuvastatin, and simvastatin—are among the most commonly prescribed drugs worldwide. They work around the clock to reduce low-density lipoprotein (LDL) cholesterol and lower the risk of heart attack, stroke, and other cardiovascular events.
But life gets busy. Alarm clocks get ignored, routines get disrupted, and medication bottles get left behind on countertops.
So what actually happens when that daily dose gets skipped? Here’s everything worth knowing about missing cholesterol medication, based on medical guidance and research data.
Why Cholesterol Pills Matter for Heart Health
Cholesterol-lowering medications serve a critical function in managing atherosclerotic cardiovascular disease (ASCVD). According to medical research, statin therapy has been shown to bring about 23% reduction in major coronary events, 22% reduction in vascular events, and 10% lower mortality in cardiovascular disease management.
These medicines don’t just lower cholesterol numbers on a lab report. They stabilize arterial plaques, reduce inflammation in blood vessel walls, and prevent the formation of dangerous clots.
The catch? They only work when taken consistently.
Research examining 54,872 acute myocardial infarction patients in Sweden found that low statin treatment adherence during the year following a heart attack was associated with increased second-year mortality risk. Translation: skipping doses has measurable consequences.
What Happens Immediately After Missing One Dose
Here’s the thing though—one missed pill isn’t a cardiovascular catastrophe.
Most statins have relatively long half-lives, meaning they stick around in the system for a while. Atorvastatin has active metabolites that remain active for 20 to 30 hours, accounting for roughly 70% of the drug’s effectiveness.
So even 24 hours after the last dose, significant enzyme inhibition continues happening in the liver.
No Immediate Symptoms
Don’t expect to feel anything different after skipping a single dose. Cholesterol medications work silently—there’s no sensation when they’re working, and none when they’re absent.
Cholesterol levels don’t spike overnight. Blood lipid concentrations change gradually, over days and weeks, not hours.
Temporary Reduction in Protection
What does change is the degree of cardiovascular protection. That continuous enzyme blockade gets temporarily weakened. The anti-inflammatory effects diminish slightly. Plaque stabilization loses a bit of momentum.
Real talk: one missed dose won’t undo months of treatment. But it does create a small gap in the protective shield these medicines provide.
What To Do When a Dose Gets Missed
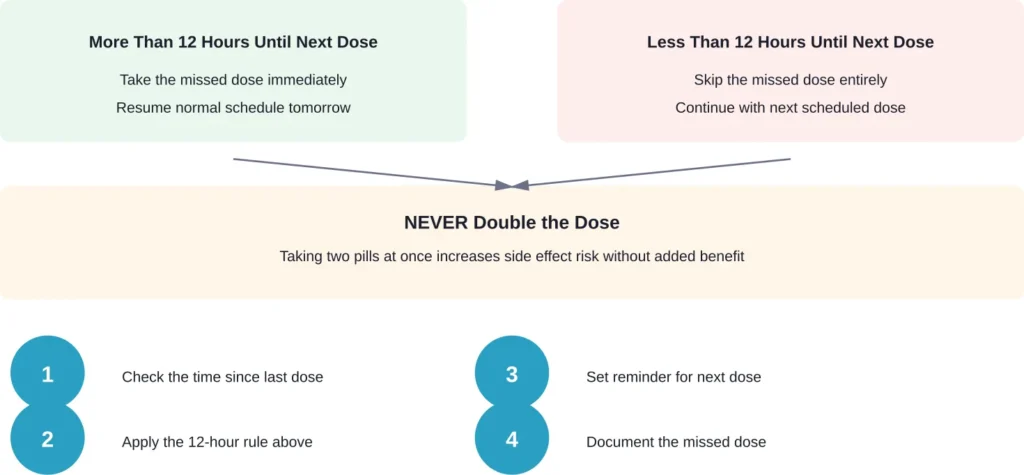
According to MedlinePlus guidance on atorvastatin and other statins, the protocol depends on timing.
| Time When Remembered | Action to Take | Next Scheduled Dose |
|---|---|---|
| Same evening (within 6 hours) | Take immediately | Continue normal schedule tomorrow |
| Next morning (8-10 hours later) | Take immediately | Take tomorrow’s dose at usual time |
| Next afternoon (14+ hours later) | Skip the missed dose | Take next dose at regular time |
| Two days later | Skip both missed doses | Resume normal schedule immediately |
The 12-hour rule exists because doubling up creates unnecessary risk. Taking two statin doses close together increases the likelihood of side effects—particularly muscle pain, liver enzyme elevation, and digestive upset—without providing additional cardiovascular benefit.
Common Mistakes After Missing a Cholesterol Pill
Several patterns show up repeatedly in discussions about missed doses.
Taking a Double Dose
This tops the list. The logic seems sound—compensate for the gap by catching up. But statins don’t work that way. Cholesterol reduction happens through consistent enzyme inhibition, not through peak blood levels.
Doubling the dose just floods the system unnecessarily.
Skipping the Next Regular Dose
Some people miss Monday’s pill, remember on Tuesday, then skip Tuesday’s dose out of confusion or concern. Now two doses have been missed instead of one.
The goal is always to get back on the regular schedule as quickly as possible.
Changing the Dosing Time Permanently
Missing a morning dose and taking it at night doesn’t mean switching permanently to nighttime dosing. Consistency matters more than the specific hour—but once a routine is established, stick with it.
Not Documenting the Miss
Occasional misses happen. Frequent misses indicate a problem. Without tracking, it’s impossible to know which category applies.
Long-Term Consequences of Frequently Missing Doses
Now, this is where it gets serious.
One missed pill? Minimal impact. Missing doses regularly? That’s a different story entirely.
Research published in the American Journal of Preventive Cardiology examined statin adherence challenges in Asian populations and found that nonadherence to statin medications is associated with increased risk of cardiovascular disease. This poses a significant challenge to lipid management in patients at risk for atherosclerotic cardiovascular disease.
Reduced LDL Cholesterol Control
Cholesterol levels start drifting upward when medication adherence drops. The liver’s cholesterol production machinery, which statins normally keep suppressed, begins ramping back up.
Studies show that patients with poor adherence often fail to achieve their LDL cholesterol targets, even when prescribed adequate doses.
Increased Cardiovascular Event Risk
The Swedish study mentioned earlier found measurable mortality differences based on adherence patterns. Patients who maintained consistent statin use after acute myocardial infarction had better survival rates than those with sporadic adherence.
According to research, approximately 11.5% of participants reported not taking their stroke prevention medications as prescribed 90 days after stroke. According to research published December 2024, Mexican American women were three times more likely to report not taking cholesterol-lowering medications as prescribed than Mexican American men.
Wasted Healthcare Resources
Poor medication adherence leads to preventable hospitalizations, emergency department visits, and additional interventions. Administrative claims data analysis reveals significant gaps between prescribed therapy and actual medication use.
When To Contact a Doctor About Missed Doses
Not every missed pill requires a phone call to the healthcare provider. But certain situations do warrant medical consultation.
Missing Multiple Doses in a Week
If doses are getting missed two or three times weekly, something needs to change. Maybe the dosing schedule doesn’t fit the daily routine. Maybe side effects are causing intentional skipping. Maybe the prescription ran out.
Whatever the reason, the doctor needs to know.
Uncertainty About Dosing Instructions
When there’s genuine confusion about what to do after missing a dose—especially if multiple doses were missed—clarification beats guessing.
New or Worsening Symptoms
Muscle pain, unexplained fatigue, dark urine, or yellowing skin can indicate serious statin side effects. These require immediate medical attention regardless of adherence patterns.
Intentional Discontinuation
Some patients stop taking statins deliberately due to concerns about side effects, online misinformation, or perceived lack of benefit. This decision should involve medical guidance, not just abrupt cessation.
Why Cholesterol Medication Adherence Remains Challenging
Statin adherence rates hover disappointingly low across populations. Research examining administrative claims data reveals significant gaps between prescribed medications and actual patient use.
Asymptomatic Condition
High cholesterol produces no symptoms. Patients feel perfectly fine before treatment and typically feel the same during treatment. This lack of noticeable benefit makes the daily pill feel unnecessary.
Side Effect Concerns
Muscle aches, digestive issues, and fatigue—whether truly caused by statins or coincidentally occurring—prompt many people to skip doses or quit entirely.
Complex Medication Regimens
Many patients taking cholesterol medications also manage blood pressure pills, diabetes medications, and other therapies. Juggling multiple prescriptions increases the likelihood of errors.
Cost and Access Barriers
Generic statins are generally affordable, but insurance coverage gaps, high deductibles, and pharmacy access issues create real obstacles for some patients.
Misinformation and Fear
Internet forums and social media spread alarming claims about statin dangers, often lacking scientific foundation. These messages influence patient behavior more than many healthcare providers realize.
Practical Strategies To Prevent Missing Doses
Okay, so what actually works for maintaining consistent medication use?
Link to Existing Habits
Taking medication at the same time as another established routine—morning coffee, toothbrushing, dinner—creates automatic triggers. The existing habit reminds you of the new behavior.
Atorvastatin and most modern statins can be taken any time of day, with or without food, making this flexible.
Use Pill Organizers
Weekly pill boxes provide visual confirmation. Empty compartments immediately show missed doses rather than requiring mental calculations.
Set Phone Alarms
Daily medication reminders work, but only if they’re not ignored. Some people need multiple escalating alarms. Others do better with text message reminders from pharmacy apps.
Keep Backup Supplies
Storing a few pills in multiple locations—car glove box, work desk, travel bag—prevents the “left it at home” scenario from causing missed doses.
Automate Refills
Running out of medication is a common adherence barrier. Automatic refill programs and mail-order pharmacies eliminate this gap.
Address Side Effects Properly
Rather than silently skipping doses due to muscle pain or other concerns, discuss alternatives with the prescriber. Different statins, lower doses, or intermittent dosing schedules might work better.
| Strategy | Best For | Effectiveness |
|---|---|---|
| Habit stacking | People with regular routines | High |
| Pill organizers | Multiple medications or memory concerns | High |
| Phone alarms | Variable schedules | Moderate |
| Backup supplies | Frequent travelers | Moderate |
| Auto refills | Everyone | High |
| Family reminders | Patients with support systems | Moderate |
Different Types of Cholesterol Medications and Missed Doses
While statins dominate the cholesterol medication landscape, other drug classes exist with different missed-dose considerations.
Statins (Atorvastatin, Rosuvastatin, Simvastatin)
These work by inhibiting HMG-CoA reductase, the enzyme controlling cholesterol production in the liver. Most have long enough half-lives that occasional missed doses cause minimal immediate impact.
Ezetimibe
This medication blocks cholesterol absorption in the intestines. According to MedlinePlus, if a dose is missed, it should be taken as soon as remembered unless it’s almost time for the next dose.
PCSK9 Inhibitors
These injectable medications are given every two weeks or monthly. Missing an injection creates a more significant gap than missing a daily oral pill, and healthcare providers should be contacted for rescheduling guidance.
Bile Acid Sequestrants (Colestipol, Cholestyramine)
These medications bind bile acids in the intestines. Missing doses affects cholesterol levels but typically produces no immediate symptoms.
Special Populations and Missed Dose Considerations
Post-Heart Attack or Stroke Patients
For people in secondary prevention—those who’ve already experienced a cardiovascular event—medication adherence becomes even more critical. Research data shows that low adherence during the first year after acute myocardial infarction associates with increased second-year mortality.
Missing doses in this population carries higher stakes.
Older Adults
Cognitive changes, complex medication regimens, and physical limitations can make adherence challenging. Pill organizers, caregiver assistance, and simplified dosing schedules help.
Pregnant or Breastfeeding Individuals
Statins are typically discontinued during pregnancy and lactation due to potential fetal risks. Anyone discovering pregnancy while on cholesterol medication should contact their healthcare provider immediately—not about a missed dose, but about whether to continue the medication at all.
Frequently Asked Questions
No, missing a single dose of atorvastatin will not trigger a heart attack. The medication’s active metabolites remain in the system for 20-30 hours, providing extended coverage. However, habitually missing doses over weeks or months does increase cardiovascular risk by allowing cholesterol levels to rise.
Cholesterol levels typically begin rising within 2-4 weeks after discontinuing statin therapy, though individual variation exists. Complete return to pre-treatment levels usually occurs within 4-6 weeks of cessation. One or two missed doses won’t cause significant cholesterol elevation.
If you remember within 12 hours of when the dose should have been taken, take it immediately. If more than 12 hours have passed and your next scheduled dose approaches soon, skip the missed dose and resume the regular schedule. Never double up to compensate.
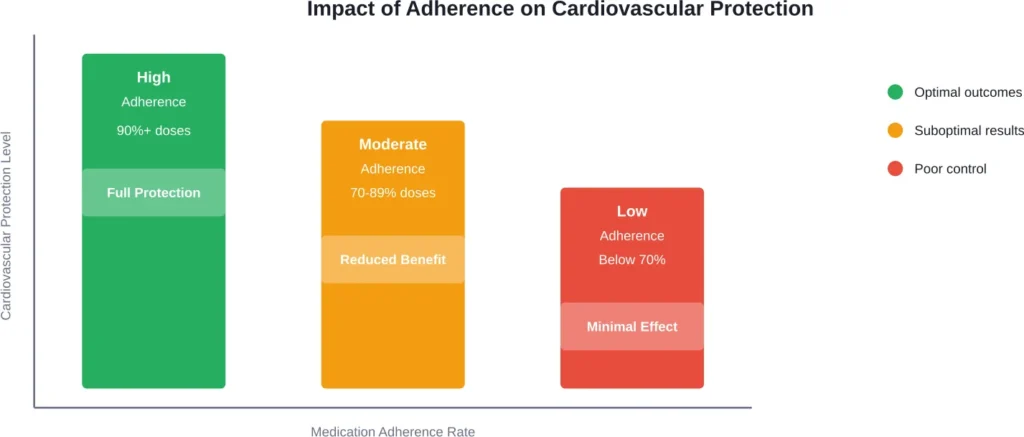
Research suggests that adherence rates above 90% provide optimal cardiovascular protection. Adherence between 70-89% offers reduced benefits, while adherence below 70% produces minimal therapeutic effect. Missing one or two doses monthly typically keeps patients above the 90% threshold.
Generally yes—the 12-hour rule applies to most statins including atorvastatin, rosuvastatin, simvastatin, and pravastatin. However, always follow the specific instructions provided with your particular medication, as some formulations may have unique guidance.
Occasional misses (once or twice monthly) don’t necessarily require reporting unless there’s uncertainty about what to do. However, missing doses weekly or having difficulty maintaining consistent use should be discussed so the healthcare provider can address barriers or adjust the treatment plan.
Yes, most modern statins can be taken at any time of day that works best for the patient’s routine. Atorvastatin and rosuvastatin are particularly flexible. Consistency matters more than the specific hour. Discuss timing changes with the healthcare provider to ensure proper transition.
The Bottom Line on Missing Cholesterol Medication
Missing a cholesterol pill happens. Life is unpredictable, routines get disrupted, and nobody maintains perfect medication adherence indefinitely.
The key is perspective. One missed dose creates minimal disruption. The medication’s protective effects continue due to long-acting metabolites. Cholesterol levels don’t spike overnight. Cardiovascular risk doesn’t suddenly jump.
But patterns matter. Frequent missed doses accumulate into genuine therapeutic failure, allowing cholesterol levels to rise and cardiovascular protection to diminish. Research consistently shows that poor statin adherence associates with worse outcomes—higher event rates, more hospitalizations, increased mortality.
The practical approach: take the missed dose if remembered within 12 hours, skip it otherwise, never double up, and get back on schedule immediately. Track patterns to identify whether misses are truly occasional or becoming habitual. Address barriers proactively rather than letting them silently erode treatment effectiveness.
And most importantly—when adherence becomes consistently difficult, talk to the healthcare provider. Solutions exist, from dosing schedule adjustments to alternative medications to addressing side effects properly. Silently struggling helps nobody.
Cholesterol management is a long game measured in years and decades, not individual doses. Missing one pill doesn’t lose the match. But staying in the game requires showing up consistently, day after day, even when the benefits feel invisible.
That consistency is what ultimately protects the heart, stabilizes arterial plaques, and reduces the risk of the cardiovascular events these medications are designed to prevent.
