Quick Summary: Taking metformin without diabetes can lead to dangerously low blood sugar (hypoglycemia), gastrointestinal distress, and vitamin B12 deficiency. While research explores metformin’s potential benefits for non-diabetic conditions like PCOS and cancer prevention, unnecessary use carries risks that outweigh speculative benefits. Always consult healthcare providers before taking any prescription medication.
Metformin stands as the most prescribed medication for type 2 diabetes worldwide. Since the FDA approved it in 1994, it’s become the first-line treatment recommended by the American Diabetes Association for managing high blood sugar.
But here’s the thing—some people take metformin without having diabetes at all.
Whether obtained through off-label prescription, leftover medication, or other means, using metformin when the body doesn’t need it creates a specific set of risks. The medication works by lowering blood glucose levels, which sounds harmless enough. But when those levels are already normal, things can go sideways fast.
How Metformin Works in the Body
Understanding what happens when someone takes metformin unnecessarily requires knowing what the drug actually does.
Metformin operates through three primary mechanisms. It reduces glucose production in the liver, decreases glucose absorption in the intestines, and improves insulin sensitivity in muscle tissue. These actions combine to lower blood sugar levels—which is exactly what people with type 2 diabetes need.
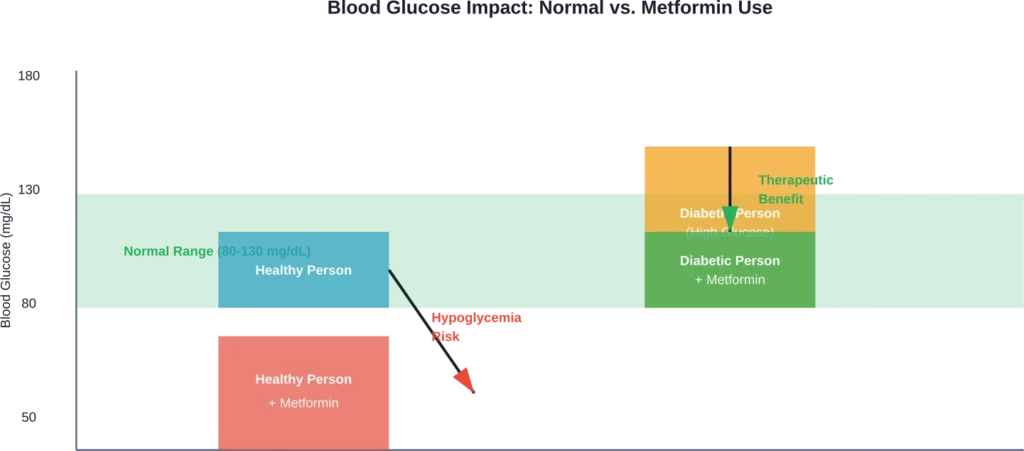
For someone without diabetes, these same mechanisms become problematic. The body’s glucose regulation system is already functioning properly. Introducing metformin disrupts this balance.
The medication doesn’t know whether blood sugar is high or normal. It just does its job: pushing glucose levels down.
The Primary Risk: Hypoglycemia
When metformin lowers already-normal blood sugar, hypoglycemia occurs. This condition means blood glucose drops below healthy levels—typically under 70 mg/dL.
Hypoglycemia isn’t just uncomfortable. It’s dangerous.
Early symptoms include shakiness, sweating, rapid heartbeat, dizziness, hunger, irritability, and confusion. As blood sugar continues dropping, symptoms escalate to blurred vision, weakness, difficulty concentrating, and headaches.
Severe hypoglycemia can cause seizures, loss of consciousness, and in extreme cases, death. The brain depends on glucose for fuel. Starve it of that fuel, and serious neurological consequences follow.
For people with diabetes taking metformin as prescribed, healthcare providers monitor blood glucose levels and adjust dosing accordingly. Someone taking metformin without medical supervision lacks this safety net.
Gastrointestinal Distress and Digestive Disruption
Digestive problems represent the most common metformin side effects, with approximately 20-30% of individuals reporting gastrointestinal upset during the initial two to four weeks of treatment.
Metformin-associated gastrointestinal symptoms can significantly impact quality of life.
Common digestive complaints include:
- Diarrhea (often severe and persistent)
- Nausea and vomiting
- Abdominal cramping and bloating
- Loss of appetite
- Metallic taste in the mouth
- Gas and flatulence
Metformin affects the digestive system through multiple pathways. It modifies glucose and bile salt uptake in the intestines. In the colon, it acts locally by altering the gut microbiome and increasing glucose delivery to intestinal cells.
For someone with diabetes, these side effects are often considered acceptable trade-offs for better blood sugar control. Medical supervision helps manage symptoms through dosage adjustments or extended-release formulations.
But someone taking metformin without diabetes experiences all the discomfort with none of the therapeutic benefit. There’s no blood sugar problem to solve—just days or weeks of digestive misery.
Vitamin B12 Deficiency: The Silent Complication
Long-term metformin use interferes with vitamin B12 absorption. This isn’t speculation—it’s a well-documented effect that healthcare providers monitor in diabetic patients.
Metformin affects vitamin B12 uptake in the digestive system, reducing the body’s ability to absorb this essential nutrient from food. Over months and years, this can lead to B12 deficiency.
Vitamin B12 deficiency develops slowly, making it easy to miss. Early symptoms include fatigue, weakness, constipation, and loss of appetite. As deficiency worsens, neurological symptoms emerge: numbness and tingling in hands and feet, difficulty walking, memory problems, and mood changes.
Severe B12 deficiency causes irreversible nerve damage.
People with diabetes taking metformin under medical supervision typically receive regular B12 level monitoring. Someone taking the medication without proper oversight won’t have this protection. The deficiency develops silently until symptoms become obvious—and potentially permanent.
Lactic Acidosis: Rare but Life-Threatening
Lactic acidosis represents the most serious potential complication of metformin use. Though rare, it’s life-threatening when it occurs.
The condition happens when lactic acid builds up in the bloodstream faster than the body can clear it. Symptoms include muscle pain, difficulty breathing, stomach pain, dizziness, and feeling extremely weak or tired.
Metformin has no direct toxic effect on the kidneys. However, the medication is cleared through renal filtration. Very high circulating drug levels combined with impaired kidney function create conditions for lactic acidosis to develop.
Someone taking metformin without medical need might not know about underlying kidney issues, dehydration, or other risk factors. Doctors screen for these conditions before prescribing metformin precisely to prevent lactic acidosis.
Taking the medication without this screening is playing Russian roulette with metabolic function.
When Metformin Is Actually Prescribed for Non-Diabetic Conditions
Now, metformin does have legitimate off-label uses for people without diabetes. Understanding these helps clarify the difference between medically supervised use and taking the drug unnecessarily.
Metformin is currently the only antidiabetic medication for prediabetes recommended by the American Diabetes Association (ADA). It’s also prescribed off-label for polycystic ovary syndrome (PCOS), gestational diabetes management, and weight gain associated with antipsychotic medications.
Research explores other potential applications. Studies have investigated metformin’s effects on cancer prevention, cardiovascular disease in non-diabetic patients, and even anti-aging properties.
According to research published in medical journals, metformin has been studied for conditions ranging from HIV treatment-related side effects to autosomal dominant polycystic kidney disease in non-diabetic patients.
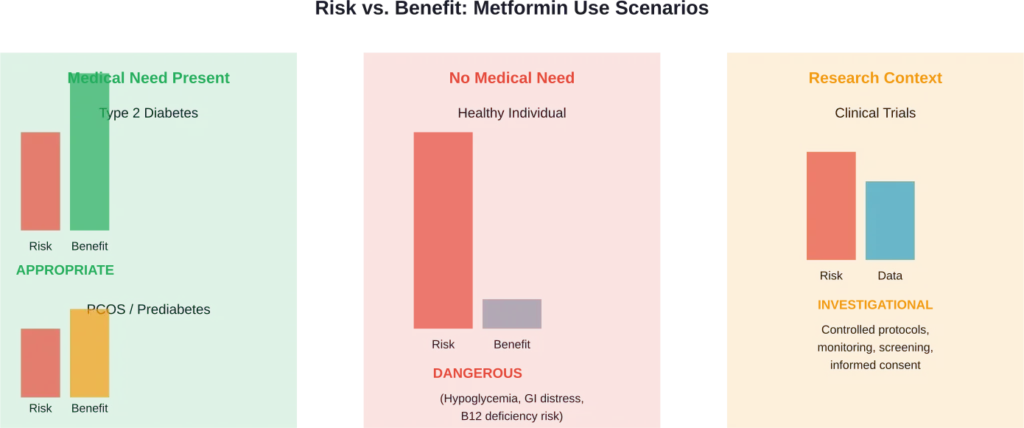
But here’s the crucial difference: all these applications involve medical supervision, specific diagnostic criteria, and careful risk-benefit analysis.
A doctor prescribing metformin for PCOS monitors the patient’s response, checks for side effects, and adjusts treatment as needed. Someone taking metformin on their own lacks this framework entirely.
| Condition | Evidence Level | Typical Supervision |
|---|---|---|
| Type 2 Diabetes | FDA-approved, first-line | Regular A1C monitoring, kidney function tests |
| Prediabetes Prevention | ADA-recommended | Glucose monitoring, lifestyle counseling |
| PCOS | Off-label, well-studied | Hormone levels, ovulation tracking |
| Gestational Diabetes | Off-label use | Intensive prenatal monitoring |
| Cancer Prevention | Research stage only | Clinical trial protocols |
| Unauthorized Self-Use | No evidence base | None—major safety concern |
The False Promise of Metformin for Weight Loss
One reason people consider taking metformin without diabetes is weight loss. The medication sometimes causes modest weight reduction, particularly in people with insulin resistance.
But metformin isn’t a weight loss drug.
Any weight loss typically results from the gastrointestinal side effects—nausea, diarrhea, and reduced appetite. Losing weight because medication makes eating unpleasant isn’t a sustainable or healthy strategy.
For people without diabetes or insulin resistance, metformin’s effect on weight is minimal to nonexistent. The risks—hypoglycemia, digestive distress, B12 deficiency—far outweigh any potential weight changes.
Real talk: if someone wants to lose weight, dozens of safer, more effective approaches exist. Taking a prescription medication designed for a condition they don’t have isn’t one of them.
Drug Interactions and Compounding Risks
Metformin interacts with numerous other medications and substances. These interactions can amplify side effects or create new problems.
Alcohol consumption while taking metformin increases lactic acidosis risk. Certain blood pressure medications, corticosteroids, and diuretics can interact with metformin in ways that affect blood sugar or kidney function.
Contrast dye used in medical imaging poses specific risks. Guidelines recommend temporarily discontinuing metformin before procedures involving iodinated contrast medium to prevent contrast-induced acute kidney injury and subsequent lactic acidosis.
Someone taking metformin without a prescription might not inform healthcare providers during emergency situations or before medical procedures. This information gap creates serious safety risks.
What Research Actually Says About Metformin in Healthy Individuals
Scientific investigation into metformin’s effects beyond diabetes continues. Some findings look promising—on paper.
Metformin was found to reduce the levels of plasminogen activator inhibitor-1 and Von Willibrand factor from the unhealthy endothelium in patients with no underlying diabetes mellitus. Research suggests potential protective effects against certain cancers. Some data indicates possible benefits for depression prevention in specific populations.
Sound exciting? Sure.
But these studies involve controlled research settings, specific patient populations, and careful monitoring. They’re exploring possibilities, not endorsing casual metformin use in healthy people.
The GLINT feasibility trial examined metformin’s effects on cardiovascular disease and cancer in people with non-diabetic hyperglycemia and high cardiovascular risk. Even in this carefully selected population with elevated (though not diabetic) glucose levels, researchers needed extensive protocols to ensure safety.
Taking metformin based on preliminary research while ignoring established risks represents a fundamental misunderstanding of how medical evidence works.
Legal and Ethical Considerations
Metformin is a prescription medication. Taking it without a prescription is illegal in most jurisdictions.
Beyond legality, using someone else’s prescription medication or obtaining metformin through unauthorized channels bypasses critical safety mechanisms. Prescriptions exist for a reason—they ensure appropriate diagnosis, dosing, and monitoring.
Healthcare providers weigh individual patient factors before prescribing any medication. Age, kidney function, other medications, medical history, and specific health conditions all influence whether metformin is appropriate and at what dose.
Skipping this process isn’t a harmless shortcut. It’s eliminating safeguards designed to prevent exactly the complications this article describes.
What to Do If You’ve Taken Metformin Without Needing It
If someone has taken metformin without a medical need, stopping requires caution and medical guidance.
For people with diabetes, suddenly stopping metformin causes blood sugar to rise. But for someone without diabetes who’s been taking it unnecessarily, stopping eliminates the risk of hypoglycemia and other side effects.
That said, consulting a healthcare provider is essential. They can:
- Assess for any complications that developed during use
- Check vitamin B12 levels if use was prolonged
- Monitor for withdrawal effects or blood sugar changes
- Address underlying concerns that led to taking the medication
- Provide appropriate alternatives if there was a legitimate health goal
Honesty with healthcare providers is crucial. They’re not there to judge—they’re there to help. Explaining the situation allows them to provide appropriate care.
The Bottom Line on Unnecessary Metformin Use
Metformin is an effective, well-studied medication for type 2 diabetes and certain other conditions when prescribed and monitored appropriately.
Taking it without medical need creates risks without corresponding benefits. Hypoglycemia can be dangerous. Gastrointestinal side effects significantly impact quality of life. B12 deficiency causes potentially permanent neurological damage. Lactic acidosis, though rare, can be fatal.
The speculative potential benefits currently under research don’t justify these concrete, immediate risks. Research investigations happen in controlled settings for good reason—researchers understand the risks and implement protocols to manage them.
If concerns exist about prediabetes, PCOS, weight management, or other health issues, legitimate pathways exist. Schedule an appointment with a healthcare provider. Discuss symptoms and concerns. Get appropriate testing and diagnosis.
If metformin is truly appropriate, a doctor can prescribe it with proper monitoring. If it’s not appropriate, they can suggest safer, more effective alternatives.
Taking prescription medication without medical supervision isn’t biohacking or being proactive about health. It’s unnecessary risk-taking that can cause serious harm.
Frequently Asked Questions
Yes, metformin can cause hypoglycemia in people with normal blood sugar levels. The medication works by lowering glucose regardless of whether levels are already normal, potentially dropping them into dangerous territory. Symptoms include shakiness, confusion, rapid heartbeat, and in severe cases, loss of consciousness.
Metformin is not a weight loss medication. Any weight reduction typically comes from gastrointestinal side effects like nausea and diarrhea rather than actual metabolic changes. For people without diabetes or insulin resistance, weight loss effects are minimal and don’t justify the medication’s risks.
The most common side effects include severe diarrhea, nausea, vomiting, abdominal cramping, bloating, and loss of appetite. These digestive issues occur in 20-30% of metformin users and can significantly impact daily life. Unlike people with diabetes who benefit from blood sugar control, healthy individuals experience these side effects without any therapeutic advantage.
Vitamin B12 deficiency from metformin develops over months to years of use. The medication interferes with B12 absorption in the digestive system. Early symptoms include fatigue and weakness, progressing to neurological issues like numbness, tingling, and memory problems if deficiency continues. People taking metformin without medical supervision won’t receive the B12 monitoring that prescribed patients get.
While metformin has no direct toxic effect on healthy kidneys, it poses risks even with normal kidney function. The medication is cleared through the kidneys, and factors like dehydration or undiscovered kidney issues can lead to drug accumulation and potentially lactic acidosis. Doctors screen kidney function before prescribing metformin—a safety step that’s skipped when taking it without supervision.
While stopping metformin eliminates the risks for someone who doesn’t need it, consultation with a healthcare provider is important. They can check for complications that developed during use, assess vitamin B12 levels if use was prolonged, and ensure no other health issues need addressing. Honesty with providers allows them to give appropriate care without judgment.
Yes, doctors prescribe metformin off-label for conditions like polycystic ovary syndrome (PCOS), prediabetes prevention in high-risk patients, and gestational diabetes management. The American Diabetes Association recommends it as the only medication for certain prediabetic patients. However, these uses all involve proper diagnosis, medical supervision, and monitoring—completely different from taking metformin without medical need.
Making Informed Health Decisions
The healthcare landscape is full of information, misinformation, and everything in between. Social media influencers promote medications for unapproved uses. Online communities share anecdotal experiences that sound compelling but lack scientific rigor.
Critical thinking matters.
Metformin’s legitimate medical applications don’t translate to “everyone should take it.” The medication addresses specific physiological problems. Without those problems, it creates new ones instead of solving anything.
Healthcare decisions should be informed by evidence, individualized to specific circumstances, and made in partnership with qualified professionals. That’s not medical gatekeeping—it’s recognizing that medications are powerful tools that require appropriate application.
If health concerns exist, professional evaluation is the answer. Not self-prescribing. Not using someone else’s medication. Not ordering drugs from questionable online sources.
The body deserves better than that. And so do you.
Speak with a healthcare provider about any health concerns. Get proper testing and diagnosis. Make informed decisions based on individual circumstances rather than general trends or internet advice.
That’s how real health improvement happens—safely, effectively, and sustainably.
