Quick Summary: Taking too much Azo (phenazopyridine) can cause serious health complications including methemoglobinemia (a blood disorder causing oxygen deprivation), acute kidney failure, severe skin discoloration, and potential liver damage. Medical research documents cases of life-threatening hypoxia and organ failure from overdoses, requiring emergency treatment with methylene blue and sometimes dialysis.
Azo—the bright orange pill many reach for during urinary tract infections—seems harmless enough sitting on drugstore shelves. It’s available over the counter, marketed for quick relief from burning and urgency.
But here’s the thing: phenazopyridine isn’t as benign as its easy accessibility suggests.
When people take more than the recommended dose, whether accidentally or intentionally, the consequences can escalate from uncomfortable to genuinely dangerous. Medical literature contains multiple documented cases of overdoses resulting in emergency room visits, organ damage, and even life-threatening conditions.
Understanding what happens when someone exceeds the safe dosage of this urinary analgesic matters—especially since it’s so readily available without a prescription.
Understanding Phenazopyridine and How It Works
Phenazopyridine is an azo dye that functions as a urinary tract analgesic. According to the NIH’s StatPearls database, the FDA approved this medication to alleviate symptoms of dysuria, burning sensations, urgency, frequency, and pain linked to lower urinary tract infections.
The drug works by providing a local anesthetic effect on the urinary tract mucosa. It doesn’t cure infections—that’s what antibiotics do—but it can make the wait for antibiotic treatment more bearable.
After oral administration, approximately 41% to 65% of the medication is eliminated unchanged by the kidneys. This is crucial information because it explains why the medication poses particular risks to kidney function when taken excessively.
Typical adult dosing involves 100 to 200 mg taken 3 times daily after meals for healthy adults. Over-the-counter formulations are available as 95mg or 99.5mg tablets. Maximum strength formulations exist, but regardless of the version, exceeding recommended doses triggers a cascade of potential complications.
The Dangerous Reality of Methemoglobinemia
The most serious acute risk from phenazopyridine overdose is methemoglobinemia—a blood disorder where hemoglobin’s iron oxidizes from ferrous (Fe2+) to ferric (Fe3+) state.
Sound technical? Here’s what actually happens: this oxidation increases oxygen affinity so much that hemoglobin molecules bind oxygen more tightly and can’t release it effectively to tissues. The result is tissue hypoxia despite normal oxygen saturation readings on standard pulse oximeters.
Medical research published in Clinical Practice documented an 89-year-old female who presented with severe hypoxia, shortness of breath, headache, nausea, and dizziness caused by phenazopyridine-induced methemoglobinemia. Her methemoglobin level reached 21.5%.
Another case report from Cureus described a 31-year-old patient presenting to the emergency department with cyanosis of the hands and mouth. These aren’t isolated incidents—the medical literature contains numerous similar cases across all age groups.
Recognizable Symptoms of Methemoglobinemia
When methemoglobin levels climb too high, patients develop characteristic symptoms:
- Blue-gray skin discoloration (cyanosis), especially around lips, mouth, and fingertips
- Severe headaches and dizziness
- Shortness of breath and rapid breathing
- Confusion and altered mental status
- Rapid heart rate
- Nausea and vomiting
The University of Pittsburgh Medical Center documented a 14-year-old female who ingested 15 Pyridium tablets in a suicide attempt, presenting with vomiting and significant cyanosis. Treatment required methylene blue administration—the specific antidote given intravenously at 1-2 mg/kg over five minutes.
Methylene blue works by reducing methemoglobin back to hemoglobin through cofactor activity. Without this intervention, severe methemoglobinemia can progress to seizures, coma, and death.
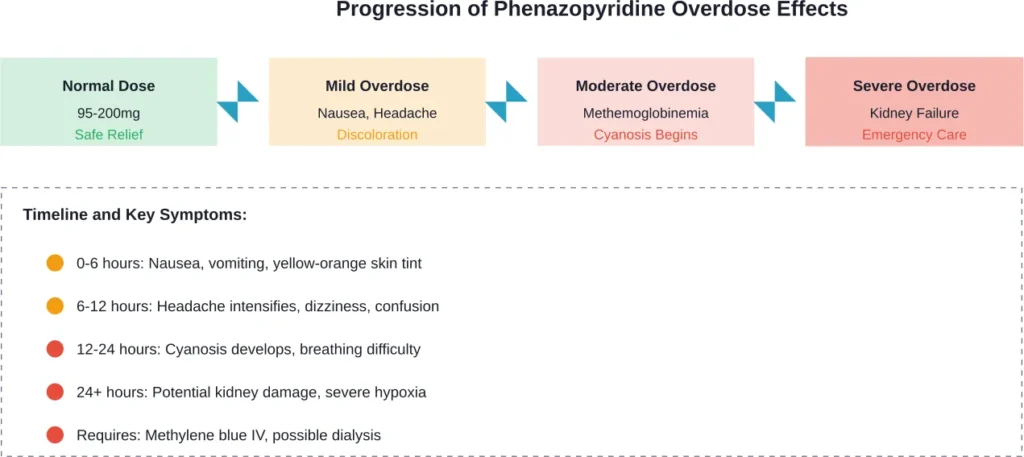
Acute Kidney Failure From Phenazopyridine Toxicity
Beyond methemoglobinemia, excessive phenazopyridine consumption poses direct nephrotoxic risks. Medical literature documents cases of acute renal failure following phenazopyridine overdoses, particularly concerning given that approximately 41% to 65% of the medication is eliminated unchanged by the kidneys.
Medical literature documents cases where acute renal failure followed phenazopyridine overdoses, with some cases showing reversibility and others resulting in persistent kidney impairment. Treatment sometimes required peritoneal dialysis to manage kidney shutdown.
Medical literature documents cases where phenazopyridine overdose caused methemoglobinemia, muscle damage (rhabdomyolysis), and severe acute renal failure, with some patients remaining oliguric despite methemoglobin level reversal within 24 hours. Oliguria—producing minimal urine—indicates serious kidney impairment.
The mechanism involves direct toxic effects on renal tubules combined with potential muscle breakdown products overwhelming kidney filtration capacity.
Who Faces Higher Kidney Risk?
Certain individuals face amplified kidney damage risk from phenazopyridine:
- Those with preexisting kidney disease or reduced renal function
- Elderly patients with age-related kidney decline
- People taking other nephrotoxic medications concurrently
- Individuals who are dehydrated during overdose
Medical literature specifically notes that phenazopyridine has been associated with acute renal failure especially in patients with preexisting kidney disease. This makes dosage adherence critically important for vulnerable populations.
Additional Serious Complications From Overdose
Methemoglobinemia and kidney failure represent the most documented severe outcomes, but phenazopyridine overdose triggers other concerning effects.
Hepatotoxicity and Liver Damage
Research indicates phenazopyridine can cause hepatitis and liver dysfunction. The medication undergoes hepatic metabolism, and excessive amounts strain liver processing capacity.
Yellow skin discoloration sometimes attributed to the drug’s dye properties may actually signal liver involvement in some overdose cases.
Hemolytic Anemia
Phenazopyridine has been associated with hemolytic anemia—the premature destruction of red blood cells. This compounds the oxygen delivery problems already created by methemoglobinemia.
When red blood cells break down faster than the body replaces them, patients experience fatigue, weakness, pale skin, and shortness of breath that persists even after methemoglobin levels normalize.
Severe Skin Reactions
Beyond the expected orange-red urine discoloration and yellowish skin tint from normal therapeutic use, overdoses can produce more dramatic skin changes. Documented cases describe patients presenting with pronounced yellow discoloration that alarmed both patients and medical staff.
Neurological Effects
Case reports document seizures, coma, and altered mental status in severe overdose scenarios. Medical case reports document pediatric phenazopyridine overdoses presenting with serious neurological symptoms alongside methemoglobinemia.
The neurological symptoms likely result from tissue hypoxia affecting brain function, though direct neurotoxic effects may also contribute.
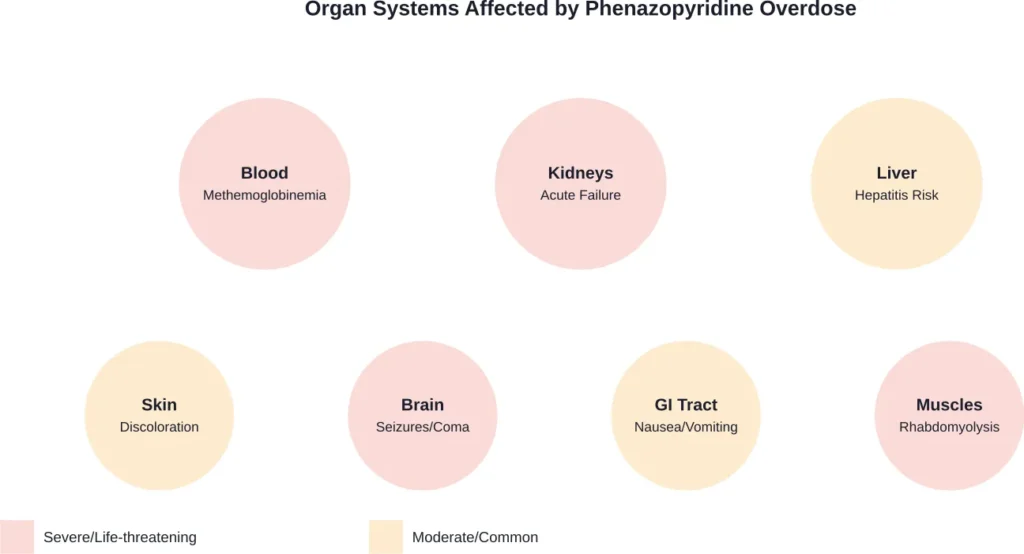
Emergency Treatment for Phenazopyridine Overdose
Medical intervention for phenazopyridine overdose follows established toxicology protocols. According to documented treatment approaches, initial management includes:
| Treatment Method | Purpose | Timing |
|---|---|---|
| Induced emesis or gastric lavage | Remove unabsorbed drug | If patient presents within 1-2 hours |
| Activated charcoal | Bind remaining drug in GI tract | Early presentation |
| Methylene blue IV (1-2 mg/kg) | Reverse methemoglobinemia | When methemoglobin levels elevated |
| Peritoneal dialysis or hemodialysis | Support kidney function, remove toxins | Acute renal failure cases |
| Exchange transfusion | Replace affected blood | Severe refractory cases |
The specific antidote—methylene blue—works by reducing methemoglobin back to functional hemoglobin. Administration typically occurs over five minutes intravenously.
In documented cases, patients showed rapid improvement following methylene blue treatment. The 89-year-old woman with 21.5% methemoglobin levels experienced significant symptom relief after receiving this antidote.
Supportive care includes oxygen supplementation, intravenous fluids, and monitoring of vital signs and laboratory values. Kidney function tests, complete blood counts, and methemoglobin levels require serial monitoring.
Safe Usage Guidelines and Maximum Dosage
Understanding proper dosing helps prevent the complications described above. Standard phenazopyridine dosing for adults involves taking the medication after meals to reduce stomach upset.
Dosage forms typically include 95mg, 99.5mg, or 200mg tablets. Maximum strength over-the-counter formulations contain higher concentrations per tablet.
The medication should not be used for more than two days without medical supervision. This short-term limit exists because phenazopyridine only masks symptoms—it doesn’t treat underlying infections.
If symptoms persist beyond two days, the infection likely requires antibiotic treatment rather than continued analgesic use.
Critical Safety Points
Never exceed the dosage listed on the product label. Taking extra tablets because symptoms feel unbearable won’t provide additional relief—phenazopyridine has a ceiling effect for pain relief but no ceiling for toxicity.
Avoid taking phenazopyridine if kidney disease or reduced kidney function exists. The drug’s renal elimination pathway makes it particularly risky for those with compromised kidney health.
Don’t combine multiple products containing phenazopyridine without realizing it. Some combination urinary products contain this ingredient alongside other medications.
Environmental and Long-Term Exposure Concerns
Research using zebrafish models has explored phenazopyridine’s environmental impact. The Harvard/zebrafish study notes that ’40─50 % of this drug gets eliminated in its native form’ and contributes to pharmaceutical burden in the environment.
Zebrafish exposed to sublethal doses showed developmental toxicity including cardiotoxicity, delayed hatching, absent swim bladders, reduced blood cell populations, and defective vascularization. Investigation revealed elevated reactive oxygen species signals and downregulated antioxidant response genes.
While these findings apply to environmental science and aquatic organisms, they underscore the drug’s biological activity and potential for oxidative stress—mechanisms relevant to human toxicity as well.
Frequently Asked Questions
Any amount exceeding the labeled dosage constitutes potential overdose. Standard adult doses range from 100 to 200 mg taken 3 times daily after meals for a maximum of two days. Taking more tablets than directed, using it longer than two days, or combining multiple phenazopyridine-containing products can lead to toxic accumulation.
Initial overdose symptoms typically include nausea, vomiting, and stomach pain. Headache and dizziness often follow within hours. As toxicity progresses, more serious signs develop including yellowing of skin beyond normal medication effects, confusion, blue-gray discoloration of lips and fingertips (cyanosis), and difficulty breathing.
Severe phenazopyridine overdoses can cause lasting organ damage. Documented cases show some patients developed acute kidney failure requiring dialysis, and while many cases resolved, preexisting kidney disease combined with overdose can result in permanent renal impairment. Severe methemoglobinemia and associated tissue hypoxia may potentially cause brain damage if not treated promptly.
Contact poison control immediately at 1-800-222-1222 or seek emergency medical care. Don’t wait for symptoms to develop. If the overdose occurred within the past hour, medical providers may administer activated charcoal. Monitor for signs of cyanosis, breathing difficulty, severe headache, or altered mental status, which require immediate emergency department evaluation.
Not always. Methylene blue specifically treats methemoglobinemia when levels become clinically significant. Medical providers measure methemoglobin levels through blood tests and administer methylene blue when these levels reach concerning thresholds or when patients show symptoms of tissue hypoxia like cyanosis and respiratory distress. Mild overdoses might only require supportive care and monitoring.
Phenazopyridine use in children requires medical supervision and proper weight-based dosing. Pediatric overdoses documented in medical literature show children face the same risks as adults—methemoglobinemia, kidney damage, and neurological effects. Medical case reports document pediatric phenazopyridine overdoses presenting with serious neurological symptoms alongside methemoglobinemia. Keep all medications out of children’s reach, and seek immediate emergency care if pediatric ingestion occurs.
Absolutely. Medical research specifically notes that phenazopyridine-associated acute renal failure occurs especially in patients with preexisting kidney disease. Since 41-65% of the drug exits unchanged through kidneys, impaired renal function means slower elimination, higher accumulation, and increased toxicity risk. People with any degree of kidney impairment should avoid phenazopyridine unless specifically directed by a physician who can adjust dosing appropriately.
Conclusion: Respect the Dosage Limits
Phenazopyridine’s easy over-the-counter availability creates a false sense of safety. The documented medical cases of methemoglobinemia, acute kidney failure, and life-threatening complications prove otherwise.
The medication serves a legitimate purpose—providing temporary relief while antibiotics work. But exceeding recommended doses transforms a helpful analgesic into a potentially dangerous toxin.
If urinary tract symptoms persist beyond two days or worsen despite taking Azo as directed, that’s a signal to seek medical evaluation rather than increase the dose. Actual treatment requires addressing the underlying infection, not masking worsening symptoms with more medication.
Take phenazopyridine exactly as labeled. And if overdose occurs—whether accidental or intentional—contact poison control or emergency services immediately. The serious complications are treatable when caught early, but delayed intervention can result in lasting organ damage.
