Quick Summary: Vitamin B12 is water-soluble and excess amounts typically leave the body through urine, making toxicity extremely rare from supplements alone. However, very high blood levels have been associated with serious underlying conditions like liver disease, kidney dysfunction, and certain cancers. While direct toxicity from supplements is uncommon, persistently elevated B12 levels warrant medical investigation to identify potential health concerns.
Vitamin B12 is essential for producing red blood cells, supporting nerve function, and creating DNA. Nearly 20% of people over 60 have B12 deficiency, which drives many people to supplements.
But can the pendulum swing too far in the other direction?
The question of B12 excess matters more than most people realize. While this water-soluble vitamin has long been considered safe at high doses, emerging research suggests that very high blood levels might signal something more concerning than just taking too many pills.
Understanding B12 and How the Body Processes It
Vitamin B12, also called cobalamin because it contains the mineral cobalt, plays crucial roles in protein metabolism and nervous system health. According to the NIH, the body stores B12 in the liver—sometimes several years’ worth.
Here’s the thing though: B12 is water-soluble. That means after the body uses what it needs, leftover amounts typically leave through urine. This built-in safety mechanism makes B12 fundamentally different from fat-soluble vitamins like A or D, which accumulate in tissues and can reach toxic levels.
The recommended dietary allowance varies by age and circumstance. Adults need about 2.4 micrograms daily, while pregnant women require slightly more. Food sources include poultry, meat, fish, and dairy products.
But absorption isn’t straightforward. The vitamin needs intrinsic factor—a protein produced in the stomach—to be absorbed in the terminal ileum (the last part of the small intestine). This process requires calcium from the pancreas. Only about 1% of B12 absorbs through passive diffusion without this complex mechanism.
Can You Actually Overdose on B12 Supplements?
Real talk: true B12 toxicity from supplements is exceptionally rare.
The NIH notes that no tolerable upper intake level has been established for B12 because the body excretes excess amounts efficiently. Most studies haven’t found adverse effects from high-dose supplementation in healthy individuals.
Research documented cases of high-dose B12 administration for severe pernicious anemia treatment. While such doses are astronomically higher than the RDA, the clinical consequences focused on specific toxicity symptoms rather than widespread harm.
Many B12 supplements contain 500 to 5,000 micrograms per dose—far exceeding daily needs. Yet serious side effects remain uncommon.
That said, some people have reported symptoms with excessive supplementation. According to a case report published in the Journal of Chiropractic Care, one patient experienced paresthesias (tingling sensations) and muscle spasms throughout the body correlated with hypercobalaminemia—abnormally high B12 blood levels.
When High B12 Levels Become a Warning Sign
Now, this is where it gets interesting.
Elevated B12 blood levels often aren’t caused by supplements at all. According to research in PubMed, high serum cobalamin may signal serious, even life-threatening conditions.
A 2020 study published in JAMA Network Open (Association of Plasma Concentration of Vitamin B12 With All-Cause Mortality in the General Population in the Netherlands by JL Flores-Guerrero et al) found that very high blood levels of B12 were associated with increased risk of all-cause mortality.
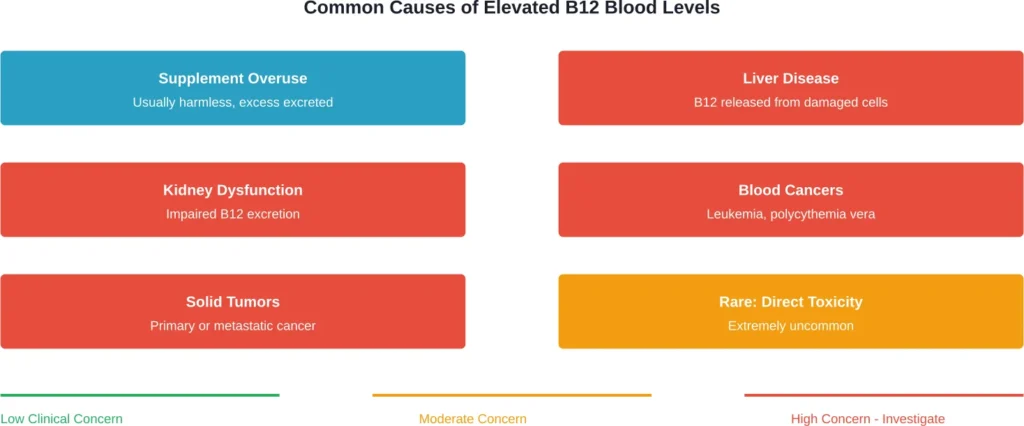
Conditions associated with elevated B12 include:
- Liver disease (cirrhosis, hepatitis, hepatocellular carcinoma)
- Kidney dysfunction
- Chronic myelogenous leukemia
- Promyelocytic leukemia
- Polycythemia vera
- Hypereosinophilic syndrome
- Solid tumors (primary or metastatic)
The liver stores most of the body’s B12. When liver cells are damaged or destroyed, they release their B12 stores into the bloodstream, creating falsely elevated readings. Similarly, kidney disease prevents proper B12 excretion.
According to research on hypervitaminosis B12, this biological abnormality is frequently underestimated in clinical practice. High B12 shouldn’t be dismissed as harmless—it often warrants investigation for underlying disease.
Symptoms and Side Effects of Excess B12
What does too much B12 actually feel like?
For most people taking standard supplements, nothing at all. The body handles the excess without issue.
However, rare cases have documented specific symptoms:
- Skin reactions (acne, rosacea-like symptoms)
- Numbness or tingling (paresthesias)
- Muscle twitches or spasms
- Anxiety or restlessness
- Headaches
- Dizziness
A dermatology review published in PubMed noted that altered cobalamin levels can lead to skin manifestations, indicating either deficiency or excess. The relationship between B12 and skin health is complex.
One case report documented peripheral neuropathy and muscle twitches as clinical manifestations of hypercobalaminemia. But wait—these are also classic B12 deficiency symptoms. The overlap makes diagnosis tricky without blood testing.
The short answer? Symptoms from supplements alone are uncommon. When they occur, stopping supplementation typically resolves the issue quickly since B12 leaves the body through urine.
How Much B12 Is Too Much?
According to CDC data analyzing NHANES 2007–2018 surveys, folic acid intakes from various sources were documented, with median usual folic acid intakes varying by intake source. For B12 specifically? No upper limit exists because toxicity is so rare.
That doesn’t mean unlimited supplementation makes sense. Tufts University researchers studying B vitamins note that while these nutrients support crucial biological functions, their role in human health is challenging to tease out—including how they might contribute both positively and negatively.
According to the Linus Pauling Institute at Oregon State University, B12 can be absorbed through passive diffusion, but this process is very inefficient—only about 1% succeeds this way. Even massive doses don’t guarantee proportional absorption.
| B12 Dose | Typical Source | Safety Profile |
|---|---|---|
| 2.4 mcg/day | Recommended dietary allowance (RDA) | Optimal for most adults |
| 25-100 mcg/day | Standard multivitamin | Safe, well-tolerated |
| 500-1,000 mcg/day | B12-specific supplement | Safe for most people |
| 1,000-5,000 mcg/day | High-dose therapeutic supplement | Generally safe, rarely necessary |
| 1,000+ mcg injection | Medical treatment for deficiency | Safe under medical supervision |
Who Should Be Cautious About B12 Supplements?
Certain groups face different considerations with B12 supplementation.
People with kidney disease should consult healthcare providers before high-dose B12. Impaired kidney function affects B12 excretion, potentially leading to accumulation.
Those with Leber’s disease—a rare hereditary eye condition—should avoid cyanocobalamin (the most common supplement form). This form can worsen optic nerve damage. Methylcobalamin or hydroxocobalamin are safer alternatives.
According to the CDC, breastfeeding mothers need adequate B12 because infants require it for brain development and red blood cell production. Deficiency can cause serious problems, but excessive supplementation beyond recommended amounts isn’t beneficial for either mother or infant.
People undergoing certain medical treatments should also exercise caution. The CDC notes that unsafe injection practices—reusing needles or syringes—pose serious risks. Always follow proper administration guidelines for injectable B12.
The Bigger Picture: B12 Deficiency Versus Excess
Look, the reality is that B12 deficiency represents a far more common and serious problem than excess.
Conditions causing deficiency include:
- Total or partial gastrectomy (reduces intrinsic factor production)
- Small intestine bacterial overgrowth (bacteria consume B12)
- Pernicious anemia (autoimmune destruction of intrinsic factor)
- Ileal resection or disease (removes absorption site)
- Strict vegan diet without supplementation
- Chronic stomach inflammation
According to StatPearls, B12 deficiency can cause megaloblastic anemia and serious neurological damage if untreated. The nervous system consequences can be irreversible.
This context matters because fear of taking too much B12 might prevent people who genuinely need supplementation from getting adequate amounts.

What to Do If Your B12 Levels Are High
Discovered elevated B12 on bloodwork? Don’t panic, but don’t ignore it either.
First, review all supplements and medications. Many multivitamins, B-complex supplements, and energy drinks contain B12. If intake is excessive from supplements, reducing or stopping them should normalize levels within weeks to months.
Second, work with a healthcare provider to investigate potential underlying causes. According to research on hypervitaminosis B12, elevated levels can indicate:
- Liver function problems (check liver enzymes, imaging)
- Kidney disease (assess creatinine, GFR)
- Hematological disorders (complete blood count, peripheral smear)
- Malignancies (age-appropriate cancer screening)
Third, retest after an appropriate interval. A single elevated reading doesn’t necessarily indicate a problem. Persistently high levels despite stopping supplements require thorough evaluation.
Some healthcare providers dismiss high B12 as harmless because it’s water-soluble. While true that direct toxicity is rare, research suggests this dismissive attitude might miss serious underlying conditions.
Frequently Asked Questions
For most people, B12 supplements are safe even at doses far exceeding the RDA. The body excretes excess through urine. However, very high blood levels may indicate underlying health problems requiring investigation rather than supplement toxicity.
Direct symptoms from supplement excess are rare but may include skin reactions, tingling, muscle twitches, headaches, or anxiety. More commonly, elevated B12 levels are symptomless and discovered incidentally on bloodwork, potentially signaling liver disease, kidney problems, or malignancy.
No official upper limit exists for B12 because toxicity is extremely rare. The RDA is 2.4 micrograms daily for adults. Supplements often contain 500-5,000 micrograms. While generally safe, amounts exceeding 1,000 micrograms daily are rarely necessary unless treating diagnosed deficiency under medical supervision.
If blood tests show elevated B12 and supplements are the likely cause, reducing or stopping them is reasonable. However, consult a healthcare provider first—high B12 often indicates underlying disease rather than supplement overuse, requiring medical investigation before assuming supplements are the problem.
Research, including a 2020 study published in JAMA Network Open (Association of Plasma Concentration of Vitamin B12 With All-Cause Mortality in the General Population in the Netherlands by JL Flores-Guerrero et al), found very high B12 blood levels associated with increased all-cause mortality risk. This likely reflects underlying conditions causing the elevation rather than B12 itself being harmful. High B12 can signal liver disease, kidney dysfunction, or cancer.
Supplements typically contain cyanocobalamin, while food provides various forms including methylcobalamin. The body converts both to active forms. Absorption differs—food B12 requires intrinsic factor and complex digestive processes, while high-dose supplements can absorb through passive diffusion, making supplementation effective for deficiency.
Most people eating animal products get adequate B12 from diet alone. However, nearly 20% of people over 60 have deficiency due to decreased stomach acid, intrinsic factor problems, or medications. Vegans, those with digestive issues, and people on certain medications often benefit from supplementation regardless of diet.
The Bottom Line on B12 Excess
Here’s what matters most: true B12 toxicity from supplements is extraordinarily rare. The water-soluble nature of this vitamin provides built-in protection against overdose.
But that doesn’t mean elevated B12 levels are meaningless. According to authoritative research from the NIH and published medical literature, very high blood levels warrant investigation for underlying conditions—liver disease, kidney problems, blood disorders, and malignancies.
For most people taking standard B12 supplements, there’s little concern. The body efficiently handles excess through urinary excretion. Doses of 500-1,000 micrograms daily are well-tolerated and safe.
The real danger isn’t taking too much B12—it’s either avoiding supplementation when genuinely needed (leading to deficiency) or ignoring elevated blood levels that might signal serious disease.
If you’re concerned about B12 status, the solution is straightforward: get tested, review supplement intake with a healthcare provider, and investigate persistently high levels to rule out underlying conditions. Balance matters more than arbitrary limits.
