Quick Summary: Taking too much biotin is generally considered safe because it’s a water-soluble vitamin that the body excretes through urine. However, high doses—particularly 15-30 mg or more daily—can cause serious lab test interference, leading to falsely abnormal results for thyroid, heart, and hormone tests. The FDA warns that biotin can mask serious conditions or create false alarms, potentially resulting in misdiagnosis or inappropriate treatment.
Biotin supplements are everywhere. Walk into any pharmacy, and you’ll find bottles promising stronger hair, healthier nails, and glowing skin. Many people pop these supplements daily without a second thought, assuming more is always better.
But here’s the thing—biotin isn’t as harmless as it seems when taken in high doses. While the vitamin itself won’t poison you, it can wreak havoc on medical testing, potentially leading to dangerous misdiagnoses.
So what actually happens when biotin intake goes beyond recommended levels? The answer is more complex than most supplement labels suggest.
Understanding Biotin and Normal Intake Levels
Biotin, also known as vitamin B7, is a water-soluble vitamin that serves as a cofactor for five carboxylases in the body. According to the National Institutes of Health, these enzymes play critical roles in breaking down fats, carbohydrates, and amino acids for energy production and fatty acid synthesis.
The recommended daily intake is modest. For most adults, adequate intake sits at just 30 micrograms (mcg) per day. Pregnant individuals need slightly more at 30 mcg, while those who are breastfeeding require 35 mcg daily.
Natural dietary sources provide plenty of biotin without supplementation. Chicken liver contains approximately 1,872 ng/g of biotin when fried, while beef liver offers around 416 ng/g. Eggs are another rich source—a whole cooked egg contains about 214 ng/g, with the yolk providing 272 ng/g.
| Food Source | Biotin Content |
|---|---|
| Chicken liver (fried) | 1,872 ng/g |
| Beef liver (fried) | 416 ng/g |
| Egg yolk (cooked) | 272 ng/g |
| Whole egg (cooked) | 214 ng/g |
| Egg white (cooked) | 58 ng/g |
| Cheddar cheese | 14 ng/g |
Most people eating a balanced diet don’t need supplements. Yet biotin supplements often contain doses that dwarf these recommendations—sometimes by hundreds or even thousands of times.
What Qualifies as “Too Much” Biotin?
Supplement dosages vary wildly. A basic B-complex vitamin typically contains 30 mcg—matching the daily recommendation perfectly. That’s 100% of the daily value and poses no concerns.
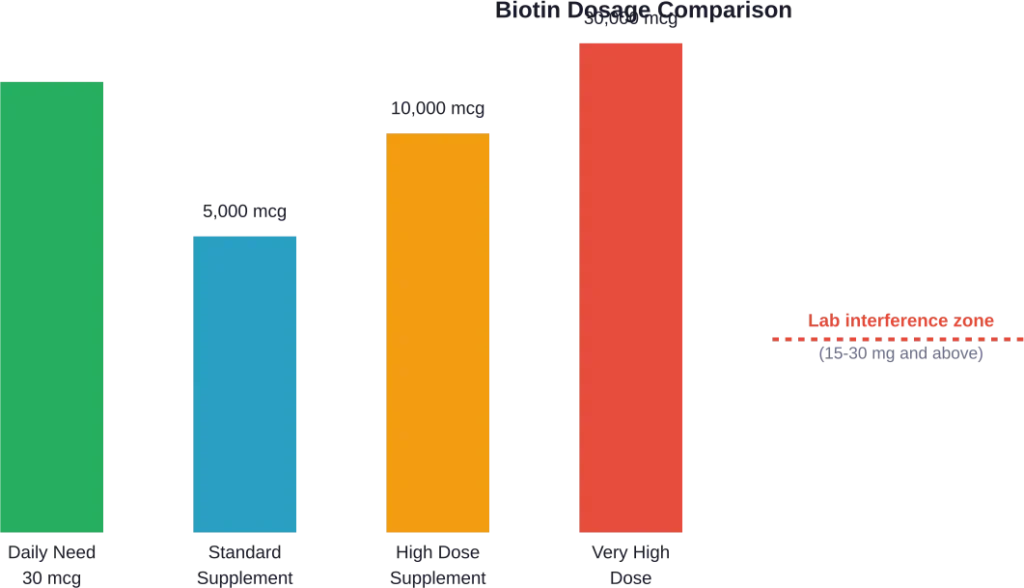
But look closer at hair, skin, and nail supplements. Many contain 5,000 to 10,000 mcg (5-10 mg) per serving. Some formulations push even higher—up to 30 mg daily.
Research published in medical journals shows that doses exceeding 15-30 mg daily can produce blood concentrations above 30 ng/mL. At these levels, significant interference with laboratory immunoassays becomes likely.
Here’s where it gets concerning. According to studies in biotin research, doses that exceed normal dietary intake by 600 times remain nearly 100% bioavailable. The body absorbs these massive doses efficiently, leading to dramatically elevated blood levels that persist for days.
The Serious Risk: Laboratory Test Interference
The most dangerous consequence of excessive biotin isn’t direct toxicity. It’s interference with medical testing.
Many modern laboratory tests use biotin-streptavidin technology. This testing method relies on the incredibly strong bond between biotin and a protein called streptavidin. When biotin levels in blood are abnormally high, this bond gets disrupted, producing false results.
The FDA has issued multiple warnings about this interference. According to their safety communications, biotin can significantly affect lab tests and cause incorrect results that often go undetected by healthcare providers.
Tests Most Affected by Biotin
Thyroid function tests are particularly vulnerable. High biotin levels can make thyroid hormone levels appear falsely elevated or suppressed, potentially leading to unnecessary treatment changes or missed diagnoses of actual thyroid disease.
Cardiac troponin tests—used to diagnose heart attacks—can show falsely low results when biotin interferes. This represents a life-threatening scenario where a real heart attack might be missed because biotin masked the elevated troponin markers.
Hormone tests, vitamin D levels, and reproductive health panels can all produce inaccurate results. Research published in medical journals demonstrates that healthy volunteers taking 15-30 mg daily can show biotin concentrations exceeding 30 ng/mL, creating significant interference across multiple immunoassay platforms.
Real talk: healthcare providers don’t always know patients are taking biotin supplements. And lab personnel might not catch the interference unless they’re specifically looking for it.
How Long Does Biotin Interference Last?
For many laboratories dealing with biotin interference, the standard recommendation is straightforward—patients should abstain from biotin for at least 48 hours before specimen collection.
But that assumes patients know to stop taking it. The problem? Most people don’t realize their hair supplement could affect their heart disease test results.
Direct Side Effects of High-Dose Biotin
Beyond lab interference, direct adverse effects from biotin remain relatively rare. As a water-soluble vitamin, excess biotin typically gets excreted through urine rather than accumulating to toxic levels.
Research indicates biotin is generally well-tolerated at high doses, though specific safety thresholds for extended periods have not been definitively established. No serious adverse effects have been consistently documented at these levels.
That said, some individuals report minor reactions. Skin rashes occasionally appear, though these are uncommon. Digestive upset occurs in some cases, particularly when starting high doses abruptly.
One documented concern involves allergic reactions. Medical literature has reported cases of hypersensitivity to biotin supplementation, though these remain exceptional rather than typical.
| Effect Type | Frequency | Severity |
|---|---|---|
| Lab test interference | Common at high doses | Potentially serious |
| Skin rash | Rare | Mild |
| Digestive upset | Uncommon | Mild |
| Allergic reactions | Very rare | Moderate |
| Direct toxicity | Not established | None documented |
Who Should Be Most Concerned?
Certain individuals face heightened risks from high-dose biotin supplements.
Anyone with existing heart conditions needs to exercise particular caution. If cardiac monitoring depends on troponin tests, biotin interference could delay critical diagnoses. The FDA specifically highlights this risk in their safety communications.
Individuals with thyroid disease should discuss biotin supplementation with healthcare providers. Falsely altered thyroid test results might prompt unnecessary medication adjustments or mask deteriorating thyroid function.
Pregnant individuals represent another concern. While biotin deficiency during pregnancy is legitimate, excessive supplementation hasn’t been adequately studied for safety. The recommended adequate intake during pregnancy is just 30 mcg—far below typical supplement doses.
People scheduled for medical testing face immediate risks. Many don’t realize that stopping biotin 48 hours before testing is necessary, particularly for thyroid panels, cardiac markers, or hormone assays.
When Biotin Supplementation Actually Makes Sense
True biotin deficiency is quite rare. Most people consuming a varied diet get adequate amounts from food sources.
Specific conditions warrant supplementation. Biotinidase deficiency, a rare genetic disorder, prevents proper biotin recycling in the body. According to medical literature, these patients require lifelong supplementation.
Certain medications can deplete biotin levels. Long-term anticonvulsant therapy sometimes leads to deficiency. Individuals on extended antibiotic courses might experience reduced biotin production from intestinal bacteria.
But what about hair, skin, and nails? The evidence here is thin. Research indicates that biotin supplementation helps hair conditions primarily in individuals who are actually deficient. For those with normal biotin levels, supplementation doesn’t produce the dramatic improvements marketing claims suggest.

What to Do If You’re Taking High-Dose Biotin
First, check supplement labels carefully. Many people don’t realize their multivitamin or beauty supplement contains megadoses of biotin. Look for amounts listed in milligrams rather than micrograms—that’s usually a red flag.
Inform all healthcare providers about biotin supplementation. This includes primary care doctors, specialists, and importantly, laboratory personnel. When scheduling any blood work, mention biotin use specifically.
For scheduled medical tests, stop biotin at least 48 hours beforehand. For very high doses (above 10 mg daily), consider stopping 72 hours or more before testing. Healthcare providers can offer specific guidance based on the particular tests ordered.
Consider whether supplementation is actually necessary. If hair, skin, or nail concerns prompted biotin use, consult a dermatologist. They can determine whether biotin deficiency truly exists or if other underlying issues need attention.
For those who genuinely need biotin supplementation, work with healthcare providers to find the minimum effective dose. More isn’t always better, particularly when it comes to interfering with critical medical diagnostics.
Frequently Asked Questions
Direct biotin overdose causing toxicity hasn’t been documented in medical literature. As a water-soluble vitamin, excess biotin is excreted through urine rather than accumulating to dangerous levels. However, high doses can cause serious problems with laboratory test accuracy, potentially leading to misdiagnosis or inappropriate treatment.
The adequate intake for adults is just 30 mcg daily. Supplements containing 5,000-10,000 mcg (5-10 mg) or more exceed recommended amounts by hundreds of times. Doses of 15-30 mg and above create significant risk for laboratory test interference, according to research published in medical journals.
Biotin clears from the body relatively quickly, but timing varies with dose. Medical recommendations suggest stopping biotin at least 48 hours before laboratory testing. For very high doses, 72 hours or more may be necessary to prevent test interference. Water-soluble vitamins like biotin don’t accumulate long-term in tissues.
Yes, biotin can significantly interfere with thyroid function tests including TSH, T3, and T4 measurements. According to the FDA and published research, this interference can make thyroid hormone levels appear falsely elevated or suppressed, potentially leading to incorrect diagnoses or unnecessary treatment changes.
Direct symptoms from excess biotin are rare. Some individuals report skin rashes or digestive upset, though these aren’t common. The primary concern isn’t physical symptoms but rather the hidden risk—inaccurate medical test results that might go unnoticed by both patients and healthcare providers.
Most evidence suggests biotin supplements primarily benefit individuals with actual deficiency. For those with normal biotin levels, supplementation hasn’t been shown to significantly improve hair, skin, or nail health. Given the risks of test interference, supplementation without confirmed deficiency may not be advisable.
Yes, this represents one of the most serious risks. Biotin can cause falsely low results on cardiac troponin tests used to diagnose heart attacks. The FDA has specifically warned about this interference, which could potentially delay or prevent detection of actual cardiac events.
Final Thoughts on Biotin Safety
Biotin supplements aren’t the harmless beauty boosters marketing suggests. While direct toxicity remains unlikely due to biotin’s water-soluble nature, the interference with medical testing creates real and potentially serious consequences.
The majority of people don’t need biotin supplementation at all. Dietary sources provide adequate amounts for normal bodily functions. Hair, skin, and nail supplements containing megadoses offer questionable benefits for those without deficiency while introducing unnecessary medical risks.
Anyone taking biotin supplements—especially at doses exceeding 1,000 mcg—should inform healthcare providers and laboratory personnel before any blood testing. Better yet, discuss with a healthcare provider whether supplementation is truly necessary in the first place.
The bottom line? More biotin doesn’t equal better health. In fact, it might just interfere with the tests needed to actually monitor that health. Before reaching for that hair supplement, consider whether the modest beauty claims are worth the hidden medical risks.
Looking for healthier alternatives to improve hair and nail health? Consider addressing nutrition holistically, managing stress, and consulting dermatologists about evidence-based treatments rather than relying on supplements with questionable efficacy and documented test interference risks.
